Abstract
Introduction
Recent studies have raised the question of whether last year medical students and first year residents show an adequate attitude toward their patient’s pain as reflected by prescribed pain medication. Underuse of analgetics could be demonstrated in several studies even after a correct diagnosis of pain was made and has led to the term “oligoanalgesia.” Our study was aimed at evaluating the potential of improving student attitudes toward pain by changing the curriculum during the last year of medical education.
Methods
The study was designed as a prospective, randomized controlled, blinded cohort study. A recent change by law (2002) in the official curriculum (“Approbationsordnung”) made it possible to compare two groups of last year medical students who were trained in different curricula during a 1-year transitional period. One group received special training on various aspects of pain and analgesic therapy (new curriculum), while the other group followed the conventional curriculum (old curriculum) without further special training. Both students and examiners were blinded toward the study target. Measurement parameters were a clinical experiment with standardized patients (OSCE) and a key features test.
Results
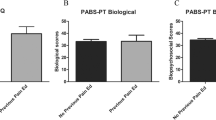
The study shows a considerable improvement of attitude toward pain in those students undergoing the new curriculum. This group demonstrated better OSCE results and significant improvement in key features tasks, and also outperformed the old curriculum group in the choice of analgesia.
Discussion
Our results confirm the importance of humanistic attitudes in future doctors in addition to the traditional implementation of knowledge and skills. Changes in the medical curriculum can positively influence these attitudes.


Similar content being viewed by others

References
Dandavino M, Snell L, Wiseman J. Why medical students should learn how to teach. Med Teach. 2007;6:558–5.
Ger LP, Lee MC, Wong CS, Chao SS, Wang JJ, Ho ST. The effect of education and clinical practice on knowledge enlightenment to and attitudes toward the use of analgesics for cancer pain among physicians and medical students. Acta Anaesthesiol Sin. 2003;41:105–14.
Hanna MN, Donnelly MB, Montgomery CL, Sloan PA. Perioperative pain management education: a short structured regional anesthesia course compared with traditional teaching among medical students. Reg Anesth Pain Med. 2005;30:523–8.
Lown BA, Chou CL, Clark WD, Haidet P, White MK, Krupat E, Pelletier S, Weissmann P, Anderson MB. Caring attitudes in medical education: perceptions of deans and curriculum leaders. J Gen Intern Med 2007;22:1514–22.
Moore GT, Block SD, Style CB, Mitchell R. The influence of the New Pathway curriculum on Harvard medical students. Acad Med. 1994;69:983–9.
Ostgathe C, Voltz R, Nauck F, Klaschik E. Undergraduate training in palliative medicine in Germany: what effect does a curriculum without compulsory palliative care have on medical students’ knowledge, skills and attitudes? Palliat Med. 2007;21:155–6.
Perleth M. Basic medical competence: a neglected educational goal in medical education? Med Klin (Munich) 1998;93:381-7. Review. German.
Satterfield JM, Hughes E. Emotion skills training for medical students: a systematic review. Med Educ. 2007;41:935–41.
Tsimtsiou Z, Kerasidou O, Efstathiou N, Papaharitou S, Hatzimouratidis K, Hatzichristou D. Medical students’ attitudes toward patient-centred care: a longitudinal survey. Med Educ. 2007;41:146–53.
Deladisma AM, Cohen M, Stevens A, Wagner P, Lok B, Bernard T, Oxendine C, Schumacher L, Johnsen K, Dickerson R, Raij A, Wells R, Duerson M, Harper JG, Lind DS. Association for Surgical Education. Do medical students respond empathetically to a virtual patient? Am J Surg. 2007;193:756–60.
Leila NM, Pirkko H, Eeva P, Eija K, Reino P. Training medical students to manage a chronic pain patient: both knowledge and communication skills are needed. Eur J Pain. 2006;10:167–70.
Brainard AH, Brislen HC. Learning professionalism: a view from the trenches. Acad Med. 2007;82:1010–4.
Fernando N, McAdam T, Cleland J, Yule S, McKenzie H, Youngson G. How can we prepare medical students for theatre-based learning? Med Educ 2007;41:968–74.
O’Brien B, Cooke M, Irby DM. Perceptions and attributions of third-year student struggles in clerkships: do students and clerkship directors agree? Acad Med 2007;82:970–8.
Swick HM, Szenas P, Danoff D, Whitcomb ME. Teaching professionalism in undergraduate medical education. JAMA. 1999;282:830–2.
Niemi-Murola L, Nieminen JT, Kalso E, Pöyhiä R. Medical undergraduate students’ beliefs and attitudes toward pain: how do they mature? Eur J Pain 2007;11:700-6.
Meekin SA, Klein JE, Fleischman AR, Fins JJ. Development of a palliative education assessment tool for medical student education. Acad Med 2000;75:986–92.
Elliott TE, Murray DM, Elliott BA, Braun B, Oken MM, Johnson KM, Post-White J, Lichtblau L. Physician knowledge and attitudes about cancer pain management: a survey from the Minnesota cancer pain project. J Pain Symptom Manage. 1995;10:494–504.
Rupp T, Delaney KA. Inadequate analgesia in emergency medicine. Ann Emerg Med. 2004;43:494–503. Review.
Raftery KA, Smith-Coggins R, Chen AH. Gender-associated differences in emergency department pain management. Ann Emerg Med 1995;26:414-21.
Heins A, Grammas M, Heins JK, Costello MW, Huang K, Mishra S. Determinants of variation in analgesic and opioid prescribing practice in an emergency department. J Opioid Manag. 2006;2:335–40.
Bijur PE, Bérard A, Esses D, Nestor J, Schechter C, Gallagher EJ. Lack of influence of patient self-report of pain intensity on administration of opioids for suspected long-bone fractures. J Pain. 2006;7:438–44.
Decosterd I, Hugli O, Tamchès E, Blanc C, Mouhsine E, Givel JC, Yersin B, Buclin T. Oligoanalgesia in the emergency department: short-term beneficial effects of an education program on acute pain. Ann Emerg Med. 2007;50:462–71.
Fosnocht DE, Swanson ER, Barton ED. Changing attitudes about pain and pain control in emergency medicine. Emerg Med Clin North Am. 2005;23:297–306.
Brown JC, Klein EJ, Lewis CW, Johnston BD, Cummings P. Emergency department analgesia for fracture pain. Ann Emerg Med. 2003;42:197–205.
McEachin CC, McDermott JT, Swor R. Few emergency medical services patients with lower-extremity fractures receive prehospital analgesia. Prehosp Emerg Care. 2002;6:406–10.
Neighbor ML, Honner S, Kohn MA. Factors affecting emergency department opioid administration to severely injured patients. Acad Emerg Med. 2004;11:1290–6.
Hatala R, Norman GR. Adapting the Key Features Examination for a clinical clerkship. Med Educ. 2002;36:160–5.
Watmough S, Garden A, Taylor D. Does a new integrated PBL curriculum with specific communication skills classes produce Pre Registration House Officers (PRHOs) with improved communication skills? Med Teach. 2006;28:264–9.
Norman G, Bordage G, Page G, Keane D. How specific is case specific? Med Educ 2006;40:618–23.
Hanna MN, Donnelly MB, Montgomery CL, Sloan PA. Perioperative pain management education: a short structured regional anaesthesia course compared with traditional teaching among medical students. Reg Anaesth Pain Med. 2005;30:523–8.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schreiner, U., Haefner, A., Gologan, R. et al. Effective teaching modifies medical student attitudes toward pain symptoms. Eur J Trauma Emerg Surg 37, 655–659 (2011). https://doi.org/10.1007/s00068-011-0111-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-011-0111-8