Abstract
Purpose
To develop an automated treatment planning approach for whole breast irradiation with simultaneous integrated boost using an automated hybrid VMAT class solution (HVMAT).
Materials and methods
Twenty-five consecutive patients with left breast cancer received 50 Gy (2 Gy/fraction) to the whole breast and an additional simultaneous 10 Gy (2.4 Gy/fraction) to the tumor cavity. Ipsilateral lung, heart, and contralateral breast were contoured as main organs-at-risk. HVMAT plans were inversely optimized by combining two open fields with a VMAT semi-arc beam. Open fields were setup to include the whole breast with a 2 cm flash region and to carry 80% of beams weight. HVMAT plans were compared with three tangential techniques: conventional wedged-field tangential plans (SWF), field-in-field forward planned tangential plans (FiF), and hybrid-IMRT plans (HMRT). Dosimetric differences among the plans were evaluated using Kruskal–Wallis one-way analysis of variance. Dose accuracy was validated using the PTW Octavius-4D phantom together with the 1500 2D-array.
Results
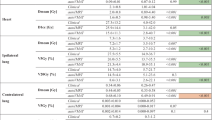
No significant differences were found among the four techniques for both targets coverage. HVMAT plans showed consistently better PTVs dose contrast, conformity, and homogeneity (p < 0.001 for all metrics) and statistically significant reduction of high-dose breast irradiation. V55 and V60 decreased by 30.4, 26.1, and 20.8% (p < 0.05) and 12.3, 9.9, and 6.0% (p < 0.05) for SWF, FIF, and HMRT, respectively. Pretreatment dose verification reported a gamma pass-rate greater than the acceptance threshold of 95% for all HVMAT plans. In addition, HVMAT reduced the time for full planning optimization to about 20 min.
Conclusions
HVMAT plans resulted in superior target dose conformity and homogeneity compared to other tangential techniques. Due to fast planning time HVMAT can be applied for all patients, minimizing the impact on human or departmental resources.






Similar content being viewed by others
References
Fisher B, Anderson S, Bryant J, Margolese RG, Deutsch M, Fisher ER et al (2002) Twenty-year follow-up of a randomised trial comparing total mastectomy, lumpectomy and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med 347:1233–1241. https://doi.org/10.1056/NEJMoa022152
Bartelink H, Horiot JC, Poortmans PM, Struikmans H, Van den Bogaert W, Fourquet A et al (2007) Impact of a higher radiation dose on local control and survival in breast-conserving therapy of early breast cancer: 10-year results of the randomized boost versus no boost EORTC 22881-10882 trial. J Clin Oncol 25(22):3259–3265. https://doi.org/10.1200/JCO.2007.11.4991
Immink JM, Putter H, Bartelink H, Cardoso JS, Cardoso MJ, van der Hulst-Vijgen MH et al (2012) Long-term cosmetic changes after breast-conserving treatment of patients with stage I–II breast cancer and included in the EORTC ‘boost versus no boost’ trial. Ann Oncol 23(10):2591–2598. https://doi.org/10.1093/annonc/mds066
Tortorelli G, Di Murro L, Barbarino R, Cicchetti S, Di Cristino D, Falco MD et al (2013) Standard or hypofractionated radiotherapy in the postoperative treatment of breast cancer: a retrospective analysis of acute skin toxicity and dose inhomogeneities. BMC Cancer 13:230. https://doi.org/10.1186/1471-2407-13-230
Borghero YO, Salehpour M, McNeese MD, Stovall M, Smith SA, Johnson J et al (2007) Multileaf field-in-field forward-planned intensity-modulated dose compensation for whole-breast irradiation is associated with reduced contralateral breast dose: a phantom model comparison. Radiother Oncol 82:324–328. https://doi.org/10.1016/j.radonc.2006.10.011
Buwenge M, Cammelli S, Ammendolia I, Tolento G, Zamagni A, Arcelli A et al (2017) Intensity modulated radiation therapy for breast cancer: current perspectives. Breast Cancer (Dove Med Press) 9:121–126. https://doi.org/10.2147/BCTT.S113025
Guerrero M, Li XA, Earl MA, Sarfaraz M, Kiggundu E (2004) Simultaneous integrated boost for breast cancer using IMRT: a radiobiological and treatment planning study. Int J Radiat Oncol Biol Phys 59(5):1513–1522. https://doi.org/10.1016/j.ijrobp.2004.04.007
Hijal T, Fournier-Bidoz N, Castro-Pena P, Kirova YM, Zefkili S, Bollet MA et al (2010) Simultaneous integrated boost in breast conserving treatment of breast cancer: a dosimetric comparison of helical tomotherapy and three-dimensional conformal radiotherapy. Radiother Oncol 94(3):300–306. https://doi.org/10.1016/j.radonc.2009.12.043
Aly MM, Glatting G, Jahnke L, Wenz F, Abo-Madyan Y (2015) Comparison of breast simultaneous integrated boost (SIB) radiotherapy techniques. Radiat Oncol 10:139. https://doi.org/10.1186/s13014-015-0452-2
Corradini S, Ballhausen H, Weingandt H, Freislederer P, Schönecker S, Niyazi M et al (2018) Left-sided breast cancer and risks of secondary lung cancer and ischemic heart disease: effects of modern radiotherapy techniques. Strahlenther Onkol 194:196–205. https://doi.org/10.1007/s00066-017-1213-y
Badakhshi H, Kaul D, Nadobny J, Wille B, Sehouli J, Budach V (2013) Image-guided volumetric modulated arc therapy for breast cancer: a feasibility study and plan comparison with three-dimensional conformal and intensity-modulated radiotherapy. Br J Radiol 86:20130515. https://doi.org/10.1259/bjr.20130515
Fogliata A, Seppala J, Reggiori G, Lofefalo F, Palumbo V, De Rose F et al (2017) Dosimetric trade-offs in breast treatment with VMAT technique. Br J Radiol 90(1070):20160701. https://doi.org/10.1259/bjr.20160701
Balaji K, Balaji Subramanian S, Sathiya K et al (2020) Hybrid planning techniques for hypofractionated whole-breast irradiation using flattening filter-free beams. Strahlenther Onkol. https://doi.org/10.1007/s00066-019-01555-1
Bahrainy M, Kretschmer M, Jost V, Kasch A, Würschmidt F, Dahle J et al (2016) Treatment of breast cancer with simultaneous integrated boost in hybrid plan technique. Strahlenther Onkol 192(4):333–341. https://doi.org/10.1007/s00066-016-0960-5
Venjakob A, Oertel M, Hering DA, Moustakis C, Haverkamp U, Eich HT (2021) Hybrid volumetric modulated arc therapy for hypofractionated radiotherapy of breast cancer: a treatment planning study. Strahlenther Onkol 197(4):296–307. https://doi.org/10.1007/s00066-020-01696-8
Nelms BE, Robinson G, Markham J, Velasco K, Boyd S, Narayan S et al (2012) Variation in external beam treatment plan quality: an inter-institutional study of planners and planning systems. Pract Radiat Oncol 2:296–305. https://doi.org/10.1016/j.prro.2011.11.012
Zhao X, Kong D, Jozsef G, Chang J, Wong EK, Formenti SC et al (2012) Automated beam placement for breast radiotherapy using a support vector machine based algorithm. Med Phys 39:2536–2543. https://doi.org/10.1118/1.3700736
Mitchell RA, Wai P, Colgan R, Kirby AM, Donovan EM (2017) Improving the efficiency of breast radiotherapy treatment planning using a semiautomated approach. J Appl Clin Med Phys 18:18–24. https://doi.org/10.1002/acm2.12006
Kim H, Kwak J, Jung J, Jeong C, Yoon K, Lee S‑W et al (2018) Automated field-in-field (FIF) plan framework combining scripting application programming interface and user-executed program for breast forward IMRT. Technol Cancer Res Treat 17:1533033818810391. https://doi.org/10.1177/1533033818810391
Cilla S, Ianiro A, Romano C, Deodato F, Macchia G, Buwenge M et al (2020) Template-based automation of treatment planning in advanced radiotherapy: a comprehensive dosimetric and clinical evaluation. Sci Rep 16:423. https://doi.org/10.1038/s41598-019-56966-y
Marrazzo L, Meattini I, Arilli C, Calusi S, Casati M, Talamonti C et al (2019) Auto-planning for VMAT accelerated partial breast irradiation. Radiother Oncol 132:85–92. https://doi.org/10.1016/j.radonc.2018.11.006
Cilla S, Macchia G, Romano C, Morabito VE, Boccardi M, Picardi V et al (2021) Challenges in lung and heart avoidance for post-mastectomy breast cancer radiotherapy: Is automated planning the answer? Med Dosim. https://doi.org/10.1016/j.meddos.2021.03.002
Chen K, Wei J, Ge C, Xia W, Shi Y, Wang H et al (2020) Application of autoplanning in radiotherapy for breast cancer after breast-conserving surgery. Sci Rep 10:10927. https://doi.org/10.1038/s41598-020-68035-w
Cilla S, Digesu C, Macchia G, Deodato F, Sallustio G, Piermattei A et al (2014) Clinical implications of different calculation algorithms in breast radiotherapy: a comparison between pencil beam and collapsed cone convolution. Phys Med 30(4):473–481. https://doi.org/10.1016/j.ejmp.2014.01.002
ICRU (2010) Report 83. Prescribing, recording, and reporting intensity-modulated photon-beam. J ICRU. https://doi.org/10.1093/jicru/10.1.report83
NSABP (2013) NSABP protocol B‑51. mt-cancer.org/Protocols/B51_Protocol.pdf. Accessed 25 Apr 2014 (A randomized phase III clinical trial evaluating post-mastectomy chestwall and regional nodal xrt and post-lumpectomy regional nodal xrt in patients with positive axillary nodes before neoadjuvant chemotherapy who convert to pathologically negative axillary nodes after neoadjuvant chemotherapy)
Gagliardi G, Constine LS, Moiseenko V, Correa C, Pierce LJ, Allen AM et al (2010) Radiation dose-volume effects in the heart. Int J Radiat Oncol Biol Phys 76:77–85. https://doi.org/10.1016/j.ijrobp.2009.04.093
Lee BM, Chang JS, Kim SY, Keum K, Suh CO, Kim YB (2020) Hypofractionated radiotherapy dose scheme and application of new techniques are associated to a lower incidence of radiation pneumonitis in breast cancer patients. Front Oncol 10:124. https://doi.org/10.3389/fonc.2020.00124
Morganti AG, Cilla S, De Gaetano A, Panunzi S, Digesù C, Macchia G et al (2011) Forward planned intensity modulated radiotherapy (IMRT) for whole breast postoperative radiotherapy. Is it useful? When? J Appl Clin Med Phys 12:213e9. https://doi.org/10.1120/jacmp.v12i2.3451
Morganti AG, Cilla S, Valentini V, Digesù C, Macchia G, Deodato F et al (2009) Phase I–II studies on accelerated IMRT in breast carcinoma: technical comparison and acute toxicity in 332 patients. Radiother Oncol 90(1):86e92. https://doi.org/10.1016/j.radonc.2008.10.017
Van’t Riet A, Mak AC, Moerland MA, Elders LH, van der Zee W (1997) A conformation number to quantify the degree of conformality in brachytherapy and external beam irradiation: application to the prostate. Int J Radiat Oncol Biol Phys 37:731–736. https://doi.org/10.1016/s0360-3016(96)00601-3
Cilla S, Deodato F, Digesù C, Macchia G, Picardi V, Ferro M et al (2014) Assessing the feasibility of volumetric-modulated arc therapy using simultaneous integrated boost (SIB-VMAT): an analysis for complex head-neck, high-risk prostate and rectal cancer cases. Med Dosim 39(1):108–116. https://doi.org/10.1016/j.meddos.2013.11.001
Abo-Madyan Y, Aziz MH, Aly MMOM, Schneider F, Sperk E, Clausen S et al (2014) Second cancer risk afer 3D-CRT, IMRT and VMAT for breast cancer. Radiother Oncol 110:471–476. https://doi.org/10.1016/j.radonc.2013.12.002
Macchia G, Cilla S, Buwenge M et al (2020) Intensity-modulated radiotherapy with concomitant boost after breast conserving surgery: a phase I–II trial. Breast Cancer 12:243–249. https://doi.org/10.2147/BCTT.S261587
Vrieling C, Collette L, Fourquet A, Hoogenraad WJ, Horiot JC, Jager JJ et al (1999) The influence of the boost in breast conserving therapy on cosmetic outcome in the EORTC “boost versus no boost” trial. Int J Radiat Oncol Biol Phys 45:677–685. https://doi.org/10.1016/s0360-3016(99)00211-4
Pignol JP, Olivotto I, Rakovitch E, Gardner S, Sixel K, Beckhamet W et al (2008) A multicenter randomized trial of breast intensity-modulated radiation therapy to reduce acute radiation dermatitis. J Clin Oncol 26:2085–2092. https://doi.org/10.1200/JCO.2007.15.2488
Stovall M, Smith SA, Langholz BM, Boice JD Jr, Shore RE, Andersson M et al (2008) Dose to the contralateral breast from radiotherapy and risk of second primary breast cancer in the WECARE study. Int J Radiat Oncol Biol Phys 72:1021–1030. https://doi.org/10.1016/j.ijrobp.2008.02.040
Grantzau T, Thomsen MS, Vaeth M, Overgaard J (2014) Risk of second primary lung cancer in women after radiotherapy for breast cancer. Radiother Oncol 111(3):366–373. https://doi.org/10.1016/j.radonc.2014.05.004
Asakura H, Hashimoto T, Zenda S, Harada H, Hirakawa K, Mizumoto M et al (2010) Analysis of dose-volume histogram parameters for radiation pneumonitis after definitive concurrent chemoradiotherapy for esophageal cancer. Radiother Oncol 95(2):240–244. https://doi.org/10.1016/j.radonc.2010.02.006
Darby SC, Ewertz M, McGale P, Bennet AM, Blom-Goldman U, Brønnum D et al (2013) Risk of ischemic heart disease in women after radiotherapy for breast cancer. N Engl J Med 368:987–998. https://doi.org/10.1056/NEJMoa1209825
Viren T, Heikkila J, Myllyoja K, Koskela K, Lahtinen T, Seppala J (2015) Tangential volumetric modulated arc therapy technique for left-sided breast cancer radiotherapy. Radiat Oncol 10:79. https://doi.org/10.1186/s13014-015-0392-x
van Mourik A, van Kranen S, den Hollander S, Sonke JJ, van Herk M, van Vliet-Vroegindeweij C (2011) Effects of setup errors and shape changes on breast radiotherapy. Int J Radiat Oncol Biol Phys 79:1557–1564. https://doi.org/10.1016/j.ijrobp.2010.07.032
Lizondo M, Latorre-Musoll A, Ribas M, Carrasco P, Espinosa N et al (2019) Pseudo skin flash on VMAT in breast radiotherapy: optimization of virtual bolus thickness and HU values. Phys Med 63:56–62. https://doi.org/10.1016/j.ejmp.2019.05.010
Reitz D, Walter F, Schönecker S, Freislederer P, Pazos M, Niyazi M et al (2020) Stability and reproducibility of 6013 deep inspiration breath-holds in left-sided breast cancer. Radiat Oncol 15(1):121. https://doi.org/10.1186/s13014-020-01572-w
Piroth MD, Baumann R, Budach W, Dunst J, Feyer P et al (2018) Heart toxicity from breast cancer radiotherapy. Strahlenther Onkol 195(1):1–12. https://doi.org/10.1007/s00066-018-1378-z
Fogliata A, Vanetti E, Clivio A, Nicolini G, Winkler P, Cozzi L (2006) The impact of photon dose calculation algorithms on lung tissue under different respiratory phases. Phys Med Biol 51:142138. https://doi.org/10.1088/0031-9155/53/9/011
Funding
The authors received no specific financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Contributions
Concept: SC. Design: SC. Conduct: SC, CR, GM, FD, LS, LI Supervision: MB, LI, VV, AGM. Data acquisition: VEM, CR, LPDV. Statistical analysis: SC, MB. Critical review: VV, AGM. Manuscript drafting, editing: all authors. Revision and final approval: all authors.
Corresponding author
Ethics declarations
Conflict of interest
S. Cilla, C. Romano, G. Macchia, M. Boccardi, L.P. De Vivo, V.E. Morabito, M. Buwenge, L. Strigari, L. Indovina, V. Valentini, F. Deodato and A.G. Morganti declare that they have no competing interests.
Ethical standards
All procedures performed in studies involving human participants or on human tissue were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. The study received approval at the Gemelli Molise Hospital Institutional Review Board. Informed consent: not applicable; patients signed informed consent to the treatment procedure, but the study was retrospective.
Additional information
The two authors Francesco Deodato and Alessio G. Morganti share the seniorship.
Rights and permissions
About this article
Cite this article
Cilla, S., Romano, C., Macchia, G. et al. Automated hybrid volumetric modulated arc therapy (HVMAT) for whole-breast irradiation with simultaneous integrated boost to lumpectomy area. Strahlenther Onkol 198, 254–267 (2022). https://doi.org/10.1007/s00066-021-01873-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-021-01873-3