Abstract
Background
The time course of human papillomavirus (HPV) DNA clearance was studied in patients with carcinoma of the cervix during follow-up after primary radical radiotherapy (RT). This study investigated the relationship between timing of HPV clearance and RT effectiveness.
Patients and methods
A total of 71 consecutive patients who were treated for cervical cancer with primary radical radiotherapy and high-dose rate intracavitary brachytherapy with or without chemotherapy were enrolled in the study. Samples for HPV DNA examination were taken before (1) treatment, (2) every brachytherapy, and (3) every follow-up examination. The times when HPV DNA was undetected were analyzed for association with recurrence-free survival.
Results
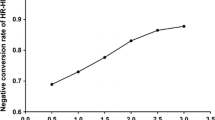
HPV DNA was not detected in 13 patients (18 %) before RT. Of the 58 patients with HPV DNA detected before treatment, HPV DNA was not detected in 34 % during treatment and in 66 % after the treatment. Within 6 months after RT, HPV DNA was detected in 0 % of all patients. The patients were followed up for a median period of 43 months (range 7–70 months). In all, 20 patients were found to develop recurrence. The 3-year cumulative disease-free survival (DFS) rate was 71 ± 5.4 % for all 71 patients. In multivariate analysis, DFS was significantly associated with HPV (detected vs. not detected) with a hazard ratio of 0.07 (95 % confidence interval 0.008–0.6, p = 0.009).
Conclusion
In this study, patients in whom HPV was not detected had the worst prognosis. Six months after RT, HPV DNA was detected in 0 % of the patients. Patients in whom HPV DNA could not be detected before treatment need careful follow-up for recurrence and may be considered for additional, or alternative treatment.
Zusammenfassung
Ziel
Gegenstand der Untersuchung war der Zeitverlauf der Eliminierung von humaner Papillomvirus-(HPV-)DNA bei Patienten mit Zervixkarzinomen während der Nachfolgeuntersuchungen nach einer primären radikalen Strahlentherapie (RT). Diese Studie untersuchte den Zusammenhang zwischen dem Zeitpunkt der HPV-Eliminierung und der RT-Effizienz.
Patienten und Methoden
Insgesamt 71 aufeinanderfolgende Patienten, die mit einer primären RT behandelt wurden, nahmen an der Studie teil. Proben für HPV-DNA-Untersuchungen wurden 1) vor der Behandlung, 2) vor jeder Brachytherapie und 3) vor jeder Nachfolgeuntersuchung genommen. Die Fälle, bei denen keine HPV-DNA entdeckt wurde, wurden auf einen Zusammenhang zu rückfallfreiem Überleben analysiert.
Ergebnisse
Bei 13 Patienten (18 %) konnte keine HPV-DNA vor der RT festgestellt werden. Von den 58 Patienten, bei denen HPV-DNA vor der Behandlung identifiziert wurde, wurde die HPV-DNA bei 34 % nicht während der Behandlung und bei 66 % nicht nach der Behandlung entdeckt. Innerhalb von 6 Monaten nach der RT wurde die HPV-DNA bei keinem Patienten (0 %) festgestellt. Die Patienten wurden für eine durchschnittliche Zeitdauer von 43 Monaten (Spanne 7–70 Monate) weiterbetreut. Bei 20 Patienten trat ein Rückfall ein. Die 3-jährige kumulative krankheitsfreie Überlebensrate (DFS) war 71 ± 5,4 % für alle 71 Patienten. In einer multivariaten Analyse war DFS signifikant mit HPV verbunden (entdeckt vs. nicht entdeckt) mit einer Hazard-Ratio (HR) von 0,07 (95 %-KI 0,008–0,6; p = 0,009).
Schlussfolgerung
In dieser Studie hatten Patienten, bei denen HPV nicht entdeckt wurde, die schlechteste Prognose. Sechs Monate nach der RT wurde HPV-DNA bei 0 % der Patienten entdeckt. Patienten, bei denen vor der Behandlung keine HPV-DNA identifiziert werden konnte, sollten sorgfältig nachbeobachtet werden und für zusätzliche oder alternative Therapien in Erwägung gezogen werden.

Similar content being viewed by others
References
zur Hausen H (1996) A major cause of human cancers. Biochim Biophys Acta 1288:55–78
de Villiers EM, Wagner D, Schneider A et al (1987) Human papillomavirus infections in women with and without abnormal cervical cytology. Lancet 2:703–706
Walboomers JM, Jacobs MV, Manos MM et al (1999) Human papillomavirus is a necessary cause of invasive cervical cancer worldwide. J Pathol 189:12–19
Parkin DM, Bray F (2006) Chapter 2: the burden of HPV-related cancers. Vaccine 24:S11–S25
Nagai Y, Toma T, Moromizato H et al (2004) Persistence of human papillomavirus infection as a predictor for recurrence in carcinoma of the cervix after radiotherapy. Am J Obstet Gynecol 191:1907–1913
Badaracco G, Savarese A, Micheli A, Rizzo C, Paolini F, Carosi M, Cutillo G, Vizza E, Arcangeli G, Venuti A (2010) Persistence of HPV after radio-chemotherapy in locally advanced cervical cancer. Oncol Rep 23:1093–1099
Gravitt PE, Peyton CL, Alessi TQ, Wheeler CM, Coutlee F, Hildesheim A, Schiffman MH, Scott DR, Apple RJ (2000) Improved amplification of genital human papillomaviruses. J Clin Microbiol 38:357–361
Ngelangel C, Munoz N, Bosch FX et al (1998) Causes of cervical cancer in the Philippines: a case control study. J Natl Cancer Inst 90:43–49
Chichareon S, Herrero R, Munoz N et al (1998) Risk factors for cervical cancer in Thailand: a case-control study. J Natl Cancer Inst 90:50–57
Walboomers JMM, Jacobs MV, Manos MM et al (1999) Human papillomavirus is a necessary cause of invasive cervical cancer worldwide. J Pathol 189:12–19
Ishikawa H, Mitsuhashi N, Sakurai H et al (2001) The effects of p53 status and human papillomavirus infection on the clinical outcome of patients with stage IIIB cervical carcinoma treated with radiation therapy alone. Cancer 91:80–89
Harima Y, Sawada S, Nagata K et al (2002) Human papillomavirus (HPV) DNA associated with prognosis of cervical cancer after radiotherapy. Int J Radiat Oncol Biol Phys 52:1345–1351
Bachtiary B, Obermair A, Dreier P et al (2002) Impact of multiple HPV infection on response to treatment and survival in patients receiving radical radiotherapy for cervical cancer. Int J Cancer 102:237–243
Lindel K, Burri P, Studer HU et al (2005) Human papillomavirus status in advanced cervical cancer: predictive and prognostic significance for curative radiation treatment. Int J Gynecol Cancer 15:278–284
Song YJ, Kim JY, Lee SK et al (2011) Persistent human papillomavirus DNA is associated with local recurrence after radiotherapy of uterine cervical cancer. Int J Cancer 15:896–902
Hubbard RA (2003) Human Papillomavirus testing methods. Arch Pathol Lab Med 127:940–945
Wilting SM, Snijderes PJ, Varlaat W et al (2012) Altered micro RNA expression associated with chromosomal changes contributes to cervical carcinogenesis. Oncogene 13:1038
Konya J, Veress G, Hernadi Z et al (1995) Correlation of human papillomavirus 16 and 18 with prognostic factors in invasive cervical neoplasias. J Med Virol 46:1–6
Nakagawa S, Yoshikawa H, Onda T et al (1996) Type of human papillomavirus is related to clinical features of cervical carcinoma. Cancer 78:1935–1941
Lombard I, Vincent-Salomon A, Validire P et al (1998) Human papillomavirus genotype as a major determinant of the course of cervical cancer. J Clin Oncol 16:2613–2619
Im SS, Wilczynski SP, Burger RA, Monk BJ (2003) Early stage cervical cancers containing human papillomavirus type 18 DNA have more nodal metastasis and deeper stromal invasion. Clin Cancer Res 9:4145–4150
Czegledy J, Iosif C, Hansson BG et al (1995) Can a test for E6/E7 transcripts of human papillomavirus type 16 serve as a diagnostic tool for the detection of micrometastasis in cervical cancer? Int J Cancer 64:211–215
Okuma K, Yamashita H, Kobayashi R, Nakagawa K (2015) A study of high-dose-rate intracavitary brachytherapy boost for curative treatment of uterine cervical cancer. J Contemp Brachytherapy 7:128–134
Yoshinaga K, Niikura H, Ogawa Y, Nemoto K, Nagase S, Takano T, Ito K, Yaegashi N (2007) Phase I trial of concurrent chemoradiation with weekly nedaplatin in patients with squamous cell carcinoma of the uterine cervix. Gynecol Oncol 104:36–40
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
K. Okuma, H. Yamashita, T. Yokoyama, K. Nakagawa, and K. Kawana state that there are no conflicts of interest.
All studies on humans described in the present manuscript were carried out with the approval of the responsible ethics committee and in accordance with national law and the Helsinki Declaration of 1975 (in its current, revised form). Informed consent was obtained from all patients included in studies.
Rights and permissions
About this article
Cite this article
Okuma, K., Yamashita, H., Yokoyama, T. et al. Undetected human papillomavirus DNA and uterine cervical carcinoma. Strahlenther Onkol 192, 55–62 (2016). https://doi.org/10.1007/s00066-015-0909-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-015-0909-0