Abstract
Background
Increasing numbers needed to treat within the first hours after ischemic stroke onset indicate a strong time dependency of the viability of brain tissue. However, this time dependency is not reflected in recent randomized controlled trials of endovascular stroke treatment. This study evaluates whether and to which extent a time dependency exists in patients with embolic carotid T or M1 occlusions within the first 6 h of stroke onset.
Methods
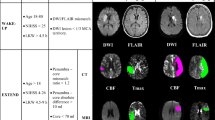
Patient data were retrieved from the Freiburg stroke data bank. Time from onset to acquisition of the diffusion weighted images (DWIs) varied between 49 and 357 min. Ischemic lesions were semiautomatically segmented on apparent diffusion coefficient maps with a threshold of 600 × 10 − 6 mm2/s. Occlusion location and thrombus length were determined with magnetic resonance angiography, T2*, and more recently susceptibility weighted image (SWI) sequences. A hyperintense vessel sign in FLAIR images as a possible surrogate for collaterals was also identified.
Results
A total of 155 patients with occlusions of the carotid T (n = 26), proximal M1 segment (n = 44), and distal M1 segment (n = 85) of the middle cerebral artery between 2011 and 2015 were included. Infarct volumes varied from 0.3 to 180.2 mL. Infarct size did not correlate with stroke onset to DWI times. Infarct volumes also did not associate with different locations of vessel occlusion, thrombus length, presence of the hyperintense vessel sign and initial infarct growth.
Conclusion
We found no significant time dependency of the viability of brain tissue with embolic carotid T or M1 occlusions between 1 and 6 h after stroke onset. The early infarction volume is thus probably determined in the hyperacute phase by the quality of leptomeningeal collaterals and comparatively stable in this time period.



Similar content being viewed by others
References
Lees KR, Bluhmki E, Kummer R von, Brott TG, Toni D, Grotta JC, et al. Time to treatment with intravenous alteplase and outcome in stroke: an updated pooled analysis of ECASS, ATLANTIS, NINDS, and EPITHET trials. Lancet. 2010;375:1695–703.
Wardlaw JM, Murray V, Berge E, del Zoppo GJ. Thrombolysis for acute ischaemic stroke. Cochrane Database Syst Rev. 2014;7:CD000213.
Saver JL, Gornbein J, Grotta J, Liebeskind D, Lutsep H, Schwamm L, et al. Number needed to treat to benefit and to harm for intravenous tissue plasminogen activator therapy in the 3- to 4.5-hour window: joint outcome table analysis of the ECASS 3 trial. Stroke. 2009;40:2433–7.
Saver JL. Time is brain-quantified. Stroke. 2006;37:263–6.
Berkhemer OA, Fransen PSS, Beumer D, van den Berg LA, Lucie A, Lingsma HF, Yoo AJ, et al. A randomized trial of intraarterial treatment for acute ischemic stroke. N Engl J Med. 2015;372:11–20.
Saver JL, Goyal M, Bonafe A, Diener H, Levy EI, Pereira VM, et al. Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. N Engl J Med. 2015;372:2285–95.
Goyal M, Demchuk AM, Menon BK, Eesa M, Rempel JL, Thornton J, et al. Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med. 2015;372:1019–30.
Yushkevich PA, Piven J, Hazlett HC, Smith RG, Ho S, Gee JC, Gerig G. User-guided 3D active contour segmentation of anatomical structures: significantly improved efficiency and reliability. Neuroimage. 2006;31:1116–28.
Naggara O, Raymond J, Domingo Ayllon M, Al-Shareef F, Touzé E, Chenoufi M, et al. T2* “susceptibility vessel sign” demonstrates clot location and length in acute ischemic stroke. PLoS One. 2013;8:e76727.
Christoforidis GA, Mohammad Y, Kehagias D, Avutu B, Slivka AP. Angiographic assessment of pial collaterals as a prognostic indicator following intra-arterial thrombolysis for acute ischemic stroke. AJNR Am J Neuroradiol. 2005;26:1789–97.
Hakimelahi R, Vachha BA, Copen WA, Papini GDE, He J, Higazi MM, et al. Time and diffusion lesion size in major anterior circulation ischemic strokes. Stroke. 2014;45:2936–41.
Fisher M, Albers GW. Advanced imaging to extend the therapeutic time window of acute ischemic stroke. Ann Neurol. 2013;73:4–9.
Cheng-Ching E, Frontera JA, Man S, Aoki J, Tateishi Y, Hui FK, et al. Degree of collaterals and not time is the determining factor of core infarct volume within 6 hours of stroke onset. AJNR Am J Neuroradiol. 2015;36:1272–6.
Fiehler J, Kucinski T, Knudsen K, Rosenkranz M, Thomalla G, Weiller C, et al. Are there time-dependent differences in diffusion and perfusion within the first 6 hours after stroke onset? Stroke. 2004;35:2099–104.
Neumann-Haefelin T, Kastrup A, Crespigny A de, Yenari MA, Ringer T, Sun GH, Moseley ME. Serial MRI after transient focal cerebral ischemia in rats: dynamics of tissue injury, blood-brain barrier damage, and edema formation. Stroke. 2000;31:1965–72; discussion 1972–3.
Jung S, Gilgen M, Slotboom J, El-Koussy M, Zubler C, Kiefer C, et al. Factors that determine penumbral tissue loss in acute ischaemic stroke. Brain. 2013;136:3554–60.
Bang OY, Saver JL, Buck BH, Alger JR, Starkman S, Ovbiagele B, et al. Impact of collateral flow on tissue fate in acute ischaemic stroke. J Neurol Neurosurg Psychiatr. 2008;79:625–9.
Lansberg MG, Cereda CW, Mlynash M, Mishra NK, Inoue M, Kemp S, et al. Response to endovascular reperfusion is not time-dependent in patients with salvageable tissue. Neurology. 2015;85:708–14.
Finitsis S, Kemmling A, Havemeister S, Thomalla G, Fiehler J, Brekenfeld C. Stability of ischemic core volume during the initial hours of acute large vessel ischemic stroke in a subgroup of mechanically revascularized patients. Neuroradiology. 2014;56:325–32.
Pfaff J, Pham M, Herweh C, Wolf M, Ringleb PA, Schönenberger S, et al. Clinical outcome after mechanical thrombectomy in non-elderly patients with acute ischemic stroke in the anterior circulation: primary admission versus patients referred from remote hospitals. Clin Neuroradiol. 2015. doi:10.1007/s00062-015-0463-2.
Nelles M, Greschus S, Möhlenbruch M, Simon B, Wüllner U, Urbach H. Patient selection for mechanical thrombectomy. Clin Neuroradiol. 2014;24:239–44.
Bardutzky J, Shen Q, Bouley J, Sotak CH, Duong TQ, Fisher M. Perfusion and diffusion imaging in acute focal cerebral ischemia: temporal vs. spatial resolution. Brain Res. 2005;1043:155–62.
Pierpaoli C, Alger JR, Righini A, Mattiello J, Dickerson R, Des Pres D, et al. High temporal resolution diffusion MRI of global cerebral ischemia and reperfusion. J Cereb Blood Flow Metab. 1996;16:892–905.
Yoo AJ, Verduzco LA, Schaefer PW, Hirsch JA, Rabinov JD, González RG. MRI-based selection for intra-arterial stroke therapy: value of pretreatment diffusion-weighted imaging lesion volume in selecting patients with acute stroke who will benefit from early recanalization. Stroke. 2009;40:2046–54.
van den Wijngaard IR, Boiten J, Holswilder G, Algra A, Dippel DWJ, Velthuis BK, et al. Impact of collateral status evaluated by dynamic computed tomographic angiography on clinical outcome in patients with ischemic stroke. Stroke. 2015. doi:10.1161/STROKEAHA.115.010354.
Beyer SE, Thierfelder KM, Baumgarten L von, Rottenkolber M, Meinel FG, Janssen H, et al. Strategies of collateral blood flow assessment in ischemic stroke: prediction of the follow-up infarct volume in conventional and dynamic CTA. AJNR Am J Neuroradiol. 2015;36:488–94.
Smit EJ, Vonken E, van Seeters T, Dankbaar JW, van der S, Irene C, Kappelle LJ, et al. Timing-invariant imaging of collateral vessels in acute ischemic stroke. Stroke. 2013;44:2194–9.
Gawlitza M, Gragert J, Quäschling U, Hoffmann KT. FLAIR-hyperintense vessel sign, diffusion-perfusion mismatch and infarct growth in acute ischemic stroke without vascular recanalisation therapy. J Neuroradiol. 2014;41:227–33.
Riedel CH, Zimmermann P, Jensen-Kondering U, Stingele R, Deuschl G, Jansen O. The importance of size: successful recanalization by intravenous thrombolysis in acute anterior stroke depends on thrombus length. Stroke. 2011;42:1775–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
This article is dedicated to Professor Dr. László Solymosi in honor of his 65th birthday.
Rights and permissions
About this article
Cite this article
Maurer, C.J., Egger, K., Dempfle, AK. et al. Facing the Time Window in Acute Ischemic Stroke: The Infarct Core. Clin Neuroradiol 26, 153–158 (2016). https://doi.org/10.1007/s00062-016-0501-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-016-0501-8