Abstract
Purpose
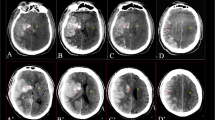
CT hyperattenuation arising from iodinated contrast has a different temporal evolution than that arising due to hemorrhage. This paper presents a method for optimal discrimination between hemorrhage and iodinated contrast in a postintervention CT in stroke patients.
Methods
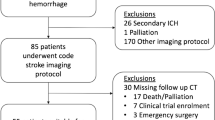
We analyzed the brain computed tomography (CT) scans of consecutive patients with intraparenchymal hyperattenuation due to hemorrhage (n= 41), those due to iodinated contrast alone (n= 24), and those due to contrast mixed with hemorrhage after reperfusion therapy (n= 14) in stroke patients. The difference between the maximum enhancement in hyperattenuation in the affected area and the corresponding contralateral area, dubbed Relative Maximum Enhancement (RME), was tracked over time. We fitted regression models to the RME changes due to hemorrhage and contrast to describe their temporal decay, and then derived the optimal discriminant curve that distinguishes the two. A computer algorithm coregistered the baseline and follow-up CT scans and performed pixel-by-pixel comparison to determine hemorrhage and iodinated contrast based on the RME changes with respect to the discriminant curve.
Results
For both hemorrhage (k= − 0.004, R 2 = 0.7) and iodinated contrast (k= − 0.064, R 2 = 0.9), the temporal evolution of RMEs were best fitted by exponential decay curves, with respective half-lives of 192.3 and 10.7 h. An exponential decay model (k= − 0.026) for optimal discrimination of hemorrhage vs. contrast was fitted. The computer algorithm implementing this model was successful in predicting the presence of hemorrhage in a hyperdense lesion with sensitivity = 93 % and specificity = 91 %.
Conclusion
Intraparenchymal hemorrhage and contrast have markedly different decay half-lives that can be used to assess hemorrhage in a hyperdense lesion on a CT scan after intra-arterial therapy.



Similar content being viewed by others
References
Abou-Chebl A. Intra-arterial therapy for acute ischemic stroke. Neurotherapeutics. 2011;8(3):400–13.
Jayaraman MV, Haas RA, Ahn SH. Intra-arterial therapy for acute stroke: trials and tribulations. Med Health R I. 2011;94(12):357–9.
Smith WS, Sung G, Saver J, et al. Mechanical thrombectomy for acute ischemic stroke: final results of the Multi MERCI trial. Stroke. 2008;39(4):1205–12.
Investigators IMSS. Combined intravenous and intra-arterial recanalization for acute ischemic stroke: the Interventional Management of Stroke Study. Stroke. 2004;35(4):904–11.
Khatri P, Wechsler LR, Broderick JP. Intracranial hemorrhage associated with revascularization therapies. Stroke. 2007;38(2):431–40.
Berger C, Fiorelli M, Steiner T, et al. Hemorrhagic transformation of ischemic brain tissue: asymptomatic or symptomatic? Stroke. 2001;32(6):1330–5.
Paciaroni M, Agnelli G, Corea F, et al. Early hemorrhagic transformation of brain infarction: rate, predictive factors, and influence on clinical outcome: results of a prospective multicenter study. Stroke. 2008;39(8):2249–56.
Yoon W, Seo JJ, Kim JK, Cho KH, Park JG, Kang HK. Contrast enhancement and contrast extravasation on computed tomography after intra-arterial thrombolysis in patients with acute ischemic stroke. Stroke. 2004;35(4):876–81.
Mericle RA, Lopes DK, Fronckowiak MD, Wakhloo AK, Guterman LR, Hopkins LN. A grading scale to predict outcomes after intra-arterial thrombolysis for stroke complicated by contrast extravasation. Neurosurgery. 2000;46(6):1307–14; discussion 14–5.
Yokogami K, Nakano S, Ohta H, Goya T, Wakisaka S. Prediction of hemorrhagic complications after thrombolytic therapy for middle cerebral artery occlusion: value of pre- and post-therapeutic computed tomographic findings and angiographic occlusive site. Neurosurgery. 1996;39(6):1102–7.
Taussky P, Tawk RG, Daugherty WP, Hanel RA. Medical therapy for ischemic stroke: review of intravenous and intra-arterial treatment options. World Neurosurg. 2011;76(6 Suppl):9–15.
Higashida R, Furlan A, Roberts H, et al. Trial design and reporting standards for intraarterial cerebral thrombolysis for acute ischemic stroke. J Vasc Interv Radiol. 2003;14(9 Pt 2):493–4.
Parrilla G, Garcia-Villalba B, Espinosa de Rueda M, et al. Hemorrhage/contrast staining areas after mechanical intra-arterial thrombectomy in acute ischemic stroke: imaging findings and clinical significance. AJNR Am J Neuroradiol. 2012;33(9):1791–6.
Darkhabani Z, Nguyen T, Lazzaro MA, et al. Complications of endovascular therapy for acute ischemic stroke and proposed management approach. Neurology. 2012;79(13 Suppl 1):192–8.
Gupta R, Phan CM, Leidecker C, et al. Evaluation of dual-energy CT for differentiating intracerebral hemorrhage from iodinated contrast material staining. Radiology. 2010;257(1):205–11.
Phan CM, Yoo AJ, Hirsch JA, Nogueira RG, Gupta R. Differentiation of hemorrhage from iodinated contrast in different intracranial compartments using dual-energy head CT. AJNR Am J Neuroradiol. 2012;33(6):1088–94.
Ferda J, Novak M, Mirka H, et al. The assessment of intracranial bleeding with virtual unenhanced imaging by means of dual-energy CT angiography. Eur Radiol. 2009;19(10):2518–22.
Bradley WG, Jr. MR appearance of hemorrhage in the brain. Radiology. 1993;189(1):15–26.
Nakano S, Iseda T, Kawano H, Yoneyama T, Ikeda T, Wakisaka S. Parenchymal hyperdensity on computed tomography after intra-arterial reperfusion therapy for acute middle cerebral artery occlusion: incidence and clinical significance. Stroke. 2001;32(9):2042–8.
Nakano S, Iseda T, Yoneyama T, Wakisaka S. Early CT signs in patients with acute middle cerebral artery occlusion: incidence of contrast staining and haemorrhagic transformations after intra-arterial reperfusion therapy. Clin Radiol. 2006;61(2):156–62.
del Zoppo GJ, von Kummer R, Hamann GF. Ischaemic damage of brain microvessels: inherent risks for thrombolytic treatment in stroke. J Neurol Neurosurg Psychiatry. 1998;65(1):1–9.
Mokin M, Kan P, Kass-Hout T, et al. Intracerebral hemorrhage secondary to intravenous and endovascular intraarterial revascularization therapies in acute ischemic stroke: an update on risk factors, predictors, and management. Neurosurg Focus. 2012;32(4):E2.
Siddiqui FM, Bekker SV, Qureshi AI. Neuroimaging of hemorrhage and vascular defects. Neurotherapeutics. 2011;8(1):28–38.
Kidwell CS, Wintermark M. Imaging of intracranial haemorrhage. Lancet Neurol. 2008;7(3):256–67.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Khalilzadeh, O., Sabel, B., Sung, Y. et al. Temporal Evolution of Intraparenchymal Hyperdensity After Intra-arterial Therapy in Patients with Ischemic Stroke: Optimal Discrimination Between Hemorrhage and Iodinated Contrast. Clin Neuroradiol 24, 365–371 (2014). https://doi.org/10.1007/s00062-013-0268-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-013-0268-0