Abstract
Background
This study aimed to observe the effect and potential mechanism of physiological ischemic training (PIT) in patients with ischemic cardiomyopathy.
Methods
A total of 165 patients with ischemic cardiomyopathy were randomly selected by the convenience sampling method and were divided into the control and experimental groups. The control group received conventional drug treatment, while the experimental group received additional PIT. All patients were followed up for 6 months and renin–angiotensin–aldosterone system (RAS) activity parameters and myocardial remodeling indicators were recorded.
Results
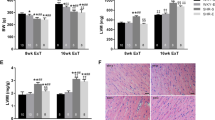
After the 6‑month intervention, cardiac function indicators in the two groups were significantly improved compared with before intervention (all P < 0.01), but the experimental group showed significantly more improvement compared with the control group (all P < 0.01). Similarly, RAS activity parameters and myocardial remodeling indicators of the two groups were significantly reduced after intervention compared with before intervention (all P < 0.01). However, the experimental group showed significantly lower myocardial remodeling indicators than the control group (all P < 0.01). Vascular endothelial growth factor (VEGF) and nitric oxide (NO) concentrations in peripheral blood in the experimental group were significantly increased after intervention compared with before intervention (both P < 0.01).
Conclusions
PIT can be applied in patients with ischemic cardiomyopathy on the basis of the original standardized drug treatment. PIT ameliorates cardiac blood flow reserve by increasing VEGF and NO concentrations in the peripheral blood, as well as by inhibiting the RAS system and myocardial remodeling. This ultimately improves the patient’s cardiac function to a greater extent.
Zusammenfassung
Hintergrund
Ziel dieser Studie war es, die Wirkung und den potenziellen Mechanismus des physiologischen ischämischen Trainings (PIT) bei Patienten mit ischämischer Kardiomyopathie zu beobachten.
Methoden
Insgesamt 165 Patienten mit ischämischer Kardiomyopathie wurden nach dem willkürlichen Stichprobenverfahren nach dem Zufallsprinzip ausgewählt und in die Kontroll- und die Versuchsgruppe aufgeteilt. Die Kontrollgruppe erhielt eine konventionelle medikamentöse Behandlung, während die Versuchsgruppe zusätzlich ein PIT erhielt. Alle Patienten wurden 6 Monate lang nachbeobachtet, und es wurden Aktivitätsparameter des Renin-Angiotensin-Aldosteron-Systems (RAS) sowie Indikatoren des myokardialen Remodelings erfasst.
Ergebnisse
Nach der 6‑monatigen Intervention waren die Herzfunktionsindikatoren in beiden Gruppen im Vergleich zu vor der Intervention signifikant besser (alle p<0,01), aber die Versuchsgruppe zeigte eine signifikant stärkere Verbesserung im Vergleich zur Kontrollgruppe (alle p<0,01). Ebenso waren die RAS-Aktivitätsparameter und die myokardialen Remodeling-Indikatoren der beiden Gruppen nach der Intervention im Vergleich zu vorher signifikant reduziert (alle p<0,01). Die Versuchsgruppe zeigte jedoch signifikant niedrigere myokardiale Remodeling-Indikatoren als die Kontrollgruppe (alle p<0,01). Die Konzentrationen des vaskulären endothelialen Wachstumsfaktors (VEGF) und von Stickstoffmonoxid (NO) im peripheren Blut waren in der Versuchsgruppe nach der Intervention im Vergleich zur vorher signifikant erhöht (beide p<0,01).
Schlussfolgerung
Die PIT kann bei Patienten mit ischämischer Kardiomyopathie auf der Grundlage der ursprünglichen standardisierten medikamentösen Behandlung angewendet werden. Die PIT verbessert die kardiale Durchblutungsreserve durch Erhöhung der VEGF- und NO-Konzentrationen im peripheren Blut sowie durch Hemmung des RAS-Systems und des myokardialen Remodelings. Dies verbessert letztendlich die Herzfunktion des Patienten in höherem Maße.




Similar content being viewed by others
References
Benjamin EJ, Muntner P, Alonso A et al (2019) Heart disease and stroke statistics-2019update: A report from the American Heart Association. Circulation 139(10):e56–e528
Wolfson AM, Fong M, Grazette L et al (2018) Chronic heart failure management and remote haemodynamic monitoring. Heart 104(23):1910–1919
Felker GM, Shaw LK, O’Connor CM (2002) A standardized definition of ischemic cardiomyopathy for use in clinical research. J Am Coll Cardiol 39(2):210–218
Ponikowski P, Voors AA, Anker SD et al (2016) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail 18(8):891–975
Yancy CW, Jessup M, Bozkurt B et al (2017) 2017 ACC/AHA/HFSA focused update of the 2013 ACCF/AHA Guideline for the management of heart failure: A report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines and the heart failure society of America. Circulation 136(6):e137–e161
Lala A, Desai AS (2014) The role of coronary artery disease in heart failure. Heart Fail Clin 10(2):353–365
Rosinberg A, Khan TA, Sellke FW et al (2004) Therapeutic angiogenesis for myocardial ischemia. Expert Rev Cardiovasc Ther 2(2):271–283
Meier P, Hemingway H, Lansky AJ et al (2012) The impact of the coronary collateral circulation on mortality: a meta-analysis. Eur Heart J 33(5):614–621
Lin A, Li J, Zhao Y et al (2011) Effect of physiologic ischemic training on protection of myocardial infarction in rabbits. Am J Phys Med Rehabil 90(2):97–105
Zheng Y, Lu X, Li J et al (2014) Impact of remote physiological ischemic training on vascular endothelial growth factor, endothelial progenitor cells and coronary angiogenesis after myocardial ischemia. Int J Cardiol 177(3):894–901
Shen M, Gao J, Li J et al (2009) Effect of ischaemic exercise training of a normal limb on angiogenesis of a pathological ischaemic limb in rabbits. Clin Sci 117(5):201–208
Doyle B, Metharom P, Caplice NM (2006) Endothelial progenitor cells. Endothelium 13(6):403–410
Xiao M, Lu X, Li J et al (2014) Physiologic ischaemic training induces endothelial progenitor cell mobilization and myocardial angiogenesis via endothelial nitric oxide synthase related pathway in rabbits. J Cardiovasc Med 15(4):280–287
Qureshi AI, Chaudhry SA, Hassan AE et al (2011) Thrombolytic treatment of patients with acute ischemic stroke related to underlying arterial dissection in the United States. Acta Neurol 68(12):1536–1542
Wan C, Li J, Yi L (2011) Enhancement of homing capability of endothelial progenitor cells to ischaemic myocardium through physiological ischaemia training. J Rehabil Med 43(6):550–555
Gao J, Shen M, Guo X et al (2011) Proteomic mechanism of myocardial angiogenesis augmented by remote ischemic training of skeletal muscle in rabbit. Cardiovasc Ther 29(3):199–210
Lin S, Chen Y, Li Y et al (2014) Physical ischaemia induced by isometric exercise facilitated collateral development in the remote ischaemic myocardium of humans. Clin Sci 127(10):581–588
Feng M, Li Z, Wang D et al (2018) MicroRNA-210 aggravates hypoxia-induced injury in cardiomyocyte H9c2 cells by targeting CXCR4. Biomed Pharmacother 102:981–987
Chen W, Ni J, Qiao Z et al (2019) Comparison of the clinical outcomes of two physiological ischemic training methods in patients with coronary heart disease. Open Med 14(1):224–233
McMurray JJ, Packer M, Desai AS et al (2014) Angiotensin-neprilysin inhibition versus enalapril in heart failure. N Engl J Med 371(11):993–1004
Corletto A, Fröhlich H, Täger T et al (2018) Beta blockers and chronic heart failure patients: prognostic impact of a dose targeted beta blocker therapy vs. heart rate targeted strategy. Clin Res Cardiol 107(11):1040–1049
Ruzicka M, Floras JS, McReynolds AJ et al (2013) Do high doses of AT (1)-receptor blockers attenuate central sympathetic outflow in humans with chronic heart failure? Clin Sci 124(9):589–595
McMurray J (2011) CONSENSUS to EMPHASIS: the overwhelming evidence which makes blockade of the renin–angiotensin–aldosterone system the cornerstone of therapy for systolic heart failure. Eur J Heart Fail 13(9):929–936
Acknowledgements
We thank Ellen Knapp, PhD, from Liwen Bianji, Edanz Group China (www.liwenbianji.cn/ac), for editing the English text of a draft of this manuscript.
Funding
This study was supported by the Science and Technology Development Program of Suzhou Ninth People’s Hospital (YUAN201823).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
W. Chen, J. Shen, R. Chen, H. You, F. Ye, J. Zheng, L. Lu, X. Lu, J. Ni, Y. Wu and Z. Qiao declare that they have no competing interests.
All procedures performed in studies involving human participants or on human tissue were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Additional information
Weihai Chen, Jun Shen and Rongrong Chen contributed equally to this work.
Rights and permissions
About this article
Cite this article
Chen, W., Shen, J., Chen, R. et al. Amelioration of ischemic cardiomyopathy in patients using physiological ischemic training. Herz 46 (Suppl 2), 173–179 (2021). https://doi.org/10.1007/s00059-020-04975-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-020-04975-3