Abstract
Background
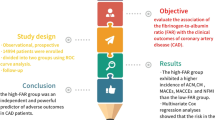
We aimed to investigate the predictive value of the fibrinogen-to-albumin ratio (FAR) regarding the development of major cardiovascular events (MACE) in patients treated with percutaneous coronary intervention (PCI) for acute coronary syndrome (ACS).
Methods
This was a prospective, observational cohort study that included 261 consecutive patients who were treated with PCI. The patients were grouped according to the occurrence of MACE during the follow-up period.
Results
During follow-up, MACE occurred in 68 (26%) patients. The FAR was independently predictive of MACE (HR: 1.017, 95% CI: 1.010–1.024, p < 0.001). In addition, left ventricular ejection fraction (LVEF) and a diagnosis of ST-segment elevation myocardial infarction (STEMI) were independent predictors of MACE. The area under the curve (AUC) of the multivariable model, including LVEF and diagnosis of STEMI, was 0.707 (95% CI: 0.631–0.782, p < 0.001). When the FAR was added to the multivariable model, the AUC was 0.770 (95% CI: 0.702–0.838, z = 2.820, difference p = 0.0048).
Conclusion
The FAR could be used for the prediction of MACE in patients with ACS who have undergone PCI.
Zusammenfassung
Hintergrund
Ziel der vorliegenden Studie war es, den prädiktiven Wert des Fibrinogen-Albumin-Quotienten (FAR) hinsichtlich der Entstehung schwergradiger kardiovaskulärer Ereignisse (MACE) bei Patienten zu untersuchen, die wegen eines akuten Koronarsyndroms (ACS) mit einer perkutanen Koronarintervention (PCI) behandelt worden waren.
Methoden
Es handelt sich dabei um eine prospektive Beobachtungs-Kohortenstudie mit 261 konsekutiven Patienten, bei denen die Therapie mit einer PCI erfolgte. Die Patienten wurden je nach Auftreten von MACE während des Nachbeobachtungszeitraums eingruppiert.
Ergebnisse
So traten MACE während des Nachbeobachtungszeitraums bei 68 (26 %) Patienten auf. Der FAR war in unabhängiger Weise für MACE prädiktiv (Hazard Ratio, HR: 1,017; 95 %-Konfidenzintervall, 95 %-KI: 1,010–1,024; p < 0,001). Außerdem waren die linksventrikuläre Ejektionsfraktion (LVEF) und die Diagnose eines ST-Strecken-Hebungs-Infarkts (STEMI) unabhängige Prädiktoren für MACE. Im multivariablen Modell einschließlich LVEF und STEMI-Diagnose betrug die Fläche unter der Kurve (AUC) 0,707 (95 %-KI: 0,631–0,782; p < 0,001). Unter Berücksichtigung des FAR beim multivariablen Modell lag die AUC bei 0,770 (95 %-KI: 0,702–0,838; z = 2,820; Differenz bei p = 0,0048).
Schlussfolgerung
Der FAR könnte zur Prädiktion von MACE bei Patienten mit ACS eingesetzt werden, bei denen eine PCI durchgeführt wurde.



Similar content being viewed by others
References
Schultz DR, Arnold PI (1990) Properties of four acute phase proteins: C‑reactive protein, serum amyloid A protein, alpha 1‑acid glycoprotein, and fibrinogen. Semin Arthritis Rheum 20(3):129–147
Tabakcı MM, Gerin F, Sunbul M et al (2017) Relation of plasma fibrinogen level with the presence, severity, and complexity of coronary artery disease. Clin Appl Thromb Hemost 23(6):638–644
Danesh J, Lewington S, Thompson SG et al (2005) Plasma fibrinogen level and the risk of major cardiovascular diseases and nonvascular mortality: an individual participant meta-analysis. JAMA 294(14):1799–1809
Ang L, Behnamfar O, Palakodeti S et al (2017) Elevated baseline serum fibrinogen: effect on 2‑year major adverse cardiovascular events following percutaneous coronary intervention. J Am Heart Assoc 6(11). https://doi.org/10.1161/JAHA.117.006580
Kuller LH, Eichner JE, Orchard TJ et al (1991) The relation between serum albumin levels and risk of coronary heart disease in the Multiple Risk Factor Intervention Trial. Am J Epidemiol 134(11):1266–1277
Oduncu V, Erkol A, Karabay CY et al (2013) The prognostic value of serum albumin levels on admission in patients with acute ST segment elevation myocardial infarction undergoing a primary percutaneous coronary intervention. Coron Artery Dis 24(2):88–94
Ertas F, Avci E, Kiris T (2019) The ratio of fibrinogen to albumin as a predictor of contrast-induced nephropathy after carotid angiography. Angiology 70(5):458–464
Kayapinar O, Ozde C, Kaya A (2019) Relationship between the reciprocal change in inflammation-related biomarkers (fibrinogen-to-albumin and hsCRP-to-albumin ratios) and the presence and severity of coronary slow flow. Clin Appl Thromb Hemost 25:1076029619835383
Xiao L, Jia Y, Wang X, Huang H (2019) The impact of preoperative fibrinogen-albumin ratio on mortality in patients with acute ST-segment elevation myocardial infarction undergoing primary percutaneous coronary intervention. Clin Chim Acta 493:8–13
Zhao YP, Ji YY, Wang FY et al (2019) Value of fibrinogen to albumin ratio on predicting spontaneous recanalization of infarct-related artery in patients with acute ST-segment elevation myocardial infarction. Zhonghua Xin Xue Guan Bing Za Zhi 47(2):123–128
Karahan O, Acet H, Ertaş F et al (2016) The relationship between fibrinogen to albumin ratio and severity of coronary artery disease in patients with STEMI. Am J Emerg Med 34(6):1037–1042
TIMI Study Group (1985) The Thrombolysis in Myocardial Infarction (TIMI) trial. Phase I findings. N Engl J Med 312(14):932–936
Amsterdam EA, Wenger NK, Brindis RG et al (2014) 2014 AHA/ACC Guideline for the Management of Patients with Non-ST-Elevation Acute Coronary Syndromes: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 64(24):e139–e228
Levine GN, Bates ER, Blankenship JC et al (2016) 2015 ACC/AHA/SCAI focused update on primary percutaneous coronary intervention for patients with ST-elevation myocardial infarction: an update of the 2011 ACCF/AHA/SCAI guideline for percutaneous coronary intervention and the 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Society for Cardiovascular Angiography and Interventions. Catheter Cardiovasc Interv 87(6):1001–1019
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44(3):837–845
Pencina MJ, D’Agostino RB Sr, Steyerberg EW (2011) Extensions of net reclassification improvement calculations to measure usefulness of new biomarkers. Stat Med 30(1):11–21
Mosesson MW (2005) Fibrinogen and fibrin structure and functions. J Thromb Haemost 3(8):1894–1904
Wilson PA, McNicol GP, Douglas AS (1968) Effect of fibrinogen degradation products on platelet aggregation. J Clin Pathol 21(2):147–153
Song B, Shu Y, Xu YN et al (2015) Plasma fibrinogen lever and risk of coronary heart disease among Chinese population: a systematic review and meta-analysis. Int J Clin Exp Med 8(8):13195–13202
Kurtul A, Yarlioglues M, Murat SN et al (2016) The association of plasma fibrinogen with the extent and complexity of coronary lesions in patients with acute coronary syndrome. Kardiologia Pol 74(4):338–345
Kaptoge S, Di Angelantonio E, Pennells L et al (2012) C‑reactive protein, fibrinogen, and cardiovascular disease prediction. N Engl J Med 367(14):1310–1320
Shi Y, Wu Y, Bian C et al (2010) Predictive value of plasma fibrinogen levels in patients admitted for acute coronary syndrome. Tex Heart Inst J 37(2):178–183
Peters T (1995) All about albumin, biochemistry, genetics, and medical applications. Academic Press, Elsevier
Maalej N, Albrecht R, Loscalzo J et al (1999) The potent platelet inhibitory effects of S‑nitrosated albumin coating of artificial surfaces. J Am Coll Cardiol 33(5):1408–1414
Joles JA, Willekes-Koolschijn N, Koomans HA (1997) Hypoalbuminemia causes high blood viscosity by increasing red cell lysophosphatidylcholine. kidney Int 52(3):761–770
Don BR, Kaysen G (2004) Serum albumin: relationship to inflammation and nutrition. Semin Dial 17(6):432–437
Roche M, Rondeau P, Singh NR et al (2008) The antioxidant properties of serum albumin. Febs Lett 582(13):1783–1787
Gillum RF, Makuc DM (1992) Serum albumin, coronary heart disease, and death. Am Heart J 123(2):507–513
Sinha MK, Roy D, Gaze DC et al (2004) Role of “Ischemia modified albumin”, a new biochemical marker of myocardial ischaemia, in the early diagnosis of acute coronary syndromes. Emerg Med J 21(1):29–34
Peacock F, Morris DL, Anwaruddin S et al (2006) Meta-analysis of ischemia-modified albumin to rule out acute coronary syndromes in the emergency department. Am Heart J 152(2):253–262
González-Pacheco H, Amezcua-Guerra LM, Sandoval J et al (2017) Prognostic Implications of Serum Albumin Levels in Patients With Acute Coronary Syndromes. Am J Cardiol 119(7):951–958
Author information
Authors and Affiliations
Contributions
All authors contributed to: (1) substantial contributions to conception and design, or acquisition of data, or analysis and interpretation of data, (2) drafting the article or revising it critically for important intellectual content, and (3) final approval of the version to be published.
Corresponding author
Ethics declarations
Conflict of interest
M. Çetin, T. Erdoğan, T. Kırış, S. Özer, A.S. Yılmaz, H. Durak, A.Ç. Aykan and Ö. Şatıroğlu declare, that they have no competing interests.
All procedures performed in studies involving human participants or on human tissue were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Çetin, M., Erdoğan, T., Kırış, T. et al. Predictive value of fibrinogen-to-albumin ratio in acute coronary syndrome. Herz 45 (Suppl 1), 145–151 (2020). https://doi.org/10.1007/s00059-019-4840-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-019-4840-5