Abstract
Background
This meta-analysis compared the efficacy and safety of culprit-only revascularization (COR) and complete revascularization (CR) in the treatment of patients with acute ST-elevation myocardial infarction (STEMI) and multivessel disease to determine the optimal reperfusion strategy.
Method
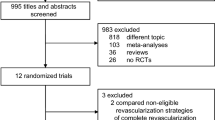
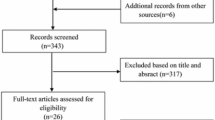
We analyzed published multicenter randomized controlled trials to compare COR and CR in patients with acute STEMI and multivessel disease. The PubMed, Cochrane Library, and Ovid databases were searched, and the meta-analysis was performed using Review Manager 5.3 software.
Results
Eight multicenter randomized controlled trials were selected involving 2870 patients, of whom 1604 underwent COR and 1266 underwent CR. No significant heterogeneity was identified across these selected studies. The CR strategy significantly decreased the incidence of major adverse cardiac events (MACE; odds ratio [OR]: 2.44, 95% CI [95% confidence interval]: 1.96–3.03, p < 0.001), mortality (OR: 1.76, 95% CI: 1.25–2.47, p = 0.001), myocardial infarction (MI, OR: 1.62, 95% CI: 1.12–2.35, p = 0.01), and repeat revascularization (OR: 3.20, 95% CI: 2.41–4.24, p < 0.001) compared with the COR approach. Moreover, no significant difference was identified in the safety indexes, including contrast-induced nephropathy, stroke, and bleeding, between the CR and the COR group (p > 0.05).
Conclusion
The present meta-analysis determined that CR is an efficacious and safe reperfusion strategy in patients with acute STEMI and multivessel disease.
Zusammenfassung
Hintergrund
In der vorliegenden Metaanalyse werden die Wirksamkeit und Sicherheit der alleinigen Revaskularisierung der verursachenden Läsion („culprit-only revascularization“, COR) und die komplette Revaskularisierung („complete revascularization“, CR) in der Therapie von Patienten mit akutem ST-Hebungs-Infarkt (STEMI) und Mehrgefäßerkrankung verglichen, um die optimale Reperfusionsstrategie zu ergründen.
Methode
Die Autoren werteten publizierte randomisierte kontrollierte Multizenterstudien aus, um die COR und CR bei Patienten mit akutem STEMI und Mehrgefäßerkrankung zu vergleichen. Dazu wurden die Datenbanken PubMed, Cochrane Library und Ovid durchsucht und eine Metaanalyse unter Verwendung der Software Review Manager 5.3 erstellt.
Ergebnisse
Es wurden 8 randomisierte kontrollierte Multizenterstudien mit 2870 Patienten ausgewählt, von denen 1604 mit einer COR und 1266 mit einer CR behandelt wurden. Zwischen den ausgewählten Studien wurde keine signifikante Heterogenität festgestellt. Mit der CR-Strategie kam es zu einer signifikanten Abnahme der Inzidenz schwerer unerwünschter kardialer Ereignisse („major adverse cardiac events“, MACE; Odds Ratio [OR]: 2,44; 95%-Konfidenzintervall [95%-KI]: 1,96–3,03; p < 0,001), der Mortalität (OR: 1,76; 95%-KI: 1,25–2,47; p = 0,001), des Myokardinfarkts (MI; OR: 1,62; 95%-KI: 1,12–2,35; p = 0,01) und der wiederholt erforderlichen Revaskularisierung (OR: 3.20, 95%-KI: 2,41–4,24; p < 0,001) im Vergleich zum COR-Ansatz. Außerdem wurde auch kein signifikanter Unterschied bei den für die Sicherheit wichtigen Parametern, einschließlich kontrastmittelinduzierter Nephropathie, Schlaganfall und Blutung, zwischen der CR- und der COR-Gruppe festgestellt (p > 0,05).
Schlussfolgerung
Die vorliegende Metaanalyse ergab, dass die CR eine wirksame und sichere Reperfusionsstrategie bei Patienten mit akutem STEMI und Mehrgefäßerkrankung darstellt.









Similar content being viewed by others
References
Choudhury T, West NE, El-Omar M (2016) ST elevation myocardial infarction. Clin Med 16(3):277
Jolly SS, Cairns JA, Yusuf S et al (2016) Outcomes after thrombus aspiration for ST elevation myocardial infarction: 1‑year follow-up of the prospective randomised TOTAL trial. Lancet 387(10014):127
Park DW, Clare RM, Schulte PJ et al (2014) Extent, location, and clinical significance of non-infarct-related coronary artery disease among patients with ST-elevation myocardial infarction. JAMA 312(19):2019–2027
Keeley EC, Boura JA, Grines CL (2003) Primary angioplasty versus intravenous thrombolytic therapy for acute myocardial infarction: a quantitative review of 23 randomised trials. Acc Curr J Rev 12(2):77–78
Abe D, Sato A, Hoshi T et al (2014) Initial culprit-only versus initial multivessel percutaneous coronary intervention in patients with ST-segment elevation myocardial infarction: results from the Ibaraki Cardiovascular Assessment Study registry. Heart Vessels 29(2):171–177
Corpus RA, House JA, Marso SP et al (2004) Multivessel percutaneous coronary intervention in patients with multivessel disease and acute myocardial infarction. Am Heart J 148(3):493–500
Kim MC, Jeong MH, Park KH et al (2014) Three-year clinical outcomes of staged, ad hoc and culprit-only percutaneous coronary intervention in patients with ST-segment elevation myocardial infarction and multivessel disease. Int J Cardiol 176(2):505–507
Hannan EL, Samadashvili Z, Walford G et al (2010) Culprit vessel percutaneous coronary intervention versus multivessel and staged percutaneous coronary intervention for ST-segment elevation myocardial infarction patients with multivessel disease. Jacc Cardiovasc Interv 3(1):22–31
Navarese EP, De Servi S, Buffon A, Suryapranata H, De Luca G (2011) Clinical impact of simultaneous complete revascularization vs. culprit only primary angioplasty in patients with st-elevation myocardial infarction and multivessel disease: a meta-analysis. J Thromb Thrombolysis 31(2):217–225
Wang CH, Zhang SY, Jin XF (2017) Complete revascularization versus culprit-only revascularization in ST-segment elevation myocardial infarction and multivessel disease patients undergoing primary percutaneous coronary intervention: a meta-analysis and trial sequential analysis. Int J Cardiol 228:844–852
Rasoul S, van Ommen V, Vainer J et al (2015) Multivessel revascularisation versus infarct-related artery only revascularisation during the index primary PCI in STEMI patients with multivessel disease: a meta-analysis. Neth Heart J 23(4):224–231
Nguyen AV, Thanh LV, Kamel MG et al (2017) Optimal percutaneous coronary intervention in patients with ST-elevation myocardial infarction and multivessel disease: an updated, large-scale systematic review and meta-analysis. Int J Cardiol 01(244):67–76
Zhang D, Song X, Lv S et al (2014) Culprit vessel only versus multivessel percutaneous coronary intervention in patients presenting with ST-segment elevation myocardial infarction and multivessel disease. PLoS ONE 9(3):e92316
Dahal K, Rijal J, Panta R, Lee J, Azrin M, Lootens R (2014) Multi-vessel versus culprit-vessel and staged percutaneous coronary intervention in STEMI patients with multivessel disease: a meta-analysis of randomized controlled trials. Cardiovasc Revasc Med 15(8):408–413
Sarathy K, Nagaraja V, Kapur A et al (2015) Target-vessel versus multivessel revascularisation in ST-elevation myocardial infarction: a meta-analysis of randomised trials. Heart Lung Circ 24(4):327–334
Bangalore S, Toklu B, Wetterslev J (2015) Complete versus culprit-only revascularization for ST-segment-elevation myocardial infarction and multivessel disease: a meta-analysis and trial sequential analysis of randomized trials. Circ Cardiovasc Interv 8(4):pii: e2142
El-Hayek GE, Gershlick AH, Hong MK et al (2015) Meta-analysis of randomized controlled trials comparing multivessel versus culprit-only revascularization for patients with ST-segment elevation myocardial infarction and Multivessel disease undergoing primary percutaneous coronary intervention. Am J Cardiol 115(11):1481–1486
Di Mario C, Mara S, Flavio A et al (2004) Single vs multivessel treatment during primary angioplasty: results of the multicentre randomised HEpacoat for cuLPrit or multivessel stenting for Acute Myocardial Infarction (HELP AMI) Study. Int J Cardiovasc Intervent 6(3–4):128–133
Politi L, Sgura F, Rossi R et al (2010) A randomised trial of target-vessel versus multi-vessel revascularisation in ST-elevation myocardial infarction: major adverse cardiac events during long-term follow-up. Heart 96(9):662–667
Wald DS, Morris JK, Wald NJ et al (2013) Randomized trial of preventive angioplasty in myocardial infarction. N Engl J Med 369(12):1115–1123
Hofsten DE, Kelbaek H, Helqvist S et al (2015) The third DANish study of optimal acute treatment of patients with ST-segment elevation myocardial infarction: ischemic postconditioning or deferred stent implantation versus conventional primary angioplasty and complete revascularization versus treatment of culprit lesion only: Rationale and design of the DANAMI 3 trial program. Am Heart J 169(5):613–621
Gershlick AH, Khan JN, Kelly DJ et al (2015) Randomized trial of complete versus lesion-only revascularization in patients undergoing primary percutaneous coronary intervention for STEMI and multivessel disease: the CvLPRIT trial. J Am Coll Cardiol 65(10):963–972
Buffie CG, Pamer EG (2013) Microbiota-mediated colonization resistance against intestinal pathogens. Nat Rev Immunol 13(11):790–801
Hamza M, Elgendy IY (2016) A randomized trial of complete versus culprit-only revascularization during primary percutaneous coronary intervention in diabetic patients with acute ST elevation myocardial infarction and multi vessel disease. J Interv Cardiol 29(3):241–247
Smits PC, Abdel-Wahab M, Neumann FJ et al (2017) Fractional flow reserve-guided multivessel angioplasty in myocardial infarction. N Engl J Med 376(13):1234–1244
Hlinomaz O (2015) Multi vessel coronary disease diagnosed at the time of primary PCI for STEMI: complete revascularization versus conservative strategy: the PRAGUE 13 trial. Presented at: EuroPCR, May 19, 2015, Paris, France
Engstrøm T, Kelbæk H, Helqvist S et al (2015) Complete revascularisation versus treatment of the culprit lesion only in patients with ST-segment elevation myocardial infarction and multivessel disease (DANAMI-3—PRIMULTI): an open-label, randomised controlled trial. Lancet 386(9994):665–671
Stone GW, Maehara A, Lansky AJ et al (2011) A prospective natural-history study of coronary atherosclerosis. N Engl J Med 364(3):226–235
Goldstein JA, Demetriou D, Grines CL, Pica M, Shoukfeh M, O’Neill WW (2000) Multiple complex coronary plaques in patients with acute myocardial infarction. N Engl J Med 343(13):915–922
Marenzi G, Assanelli E, Campodonico J et al (2009) Contrast volume during primary percutaneous coronary intervention and subsequent contrast-induced nephropathy and mortality. Ann Intern Med 150(3):170–177
Ambrose JA, Weinrauch M (1996) Thrombosis in ischemic heart disease. Arch Intern Med 156(13):1382–1394
Heusch G, Kleinbongard P, Bose D et al (2009) Coronary microembolization: from bedside to bench and back to bedside. Circulation 120(18):1822–1836
Hanratty CG, Koyama Y, Rasmussen HH, Nelson GI, Hansen PS, Ward MR (2002) Exaggeration of nonculprit stenosis severity during acute myocardial infarction: implications for immediate multivessel revascularization. J Am Coll Cardiol 40(5):911–916
Elgendy IY, Wen X, Mahmoud A, Bavry AA (2016) Complete versus culprit-only revascularization for patients with multi-vessel disease undergoing primary percutaneous coronary intervention: an updated meta-analysis of randomized trials. Catheter Cardiovasc Interv 88(4):501–505
Levine GN, Bates ER, Blankenship JC et al (2016) 2015 ACC/AHA/SCAI focused update on primary percutaneous coronary intervention for patients with ST-elevation myocardial infarction: an update of the 2011 ACCF/AHA/SCAI guideline for percutaneous coronary intervention and the 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines and the Society for Cardiovascular Angiography and Interventions. Circulation 133(11):1135–1147
Roe MT, Cura FA, Joski PS et al (2001) Initial experience with multivessel percutaneous coronary intervention during mechanical reperfusion for acute myocardial infarction. Am J Cardiol 88(2):170–173, A176
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
G. Fan, Y. Zhang, L. Lin, M. Chen, J. Wei, and J. Diao declare that they have no competing interests.
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
G. Fan, YW. Zhang, L. Lin, M. Cheng, J. Wei and J. Diao contributed equally to the article.
Rights and permissions
About this article
Cite this article
Fan, G., Zhang, Y.W., Lin, L. et al. Optimal reperfusion strategy in patients with acute STEMI and multivessel disease—an updated meta-analysis. Herz 45, 272–279 (2020). https://doi.org/10.1007/s00059-018-4722-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-018-4722-2
Keywords
- ST-segment elevation myocardial infarction
- Percutaneous coronary intervention
- Culprit-only PCI
- Multivessel disease
- Meta-analysis