Abstract
Background
Transcatheter aortic valve implantation (TAVI) is safe and effective for patients with aortic stenosis (AS) who have a high operative risk. However, there is still debate on the effect of TAVI in AS patients with reduced left ventricular ejection fraction (REF). The objective of the review is to clarify the efficacy of TAVI and the impact of REF on the 30-day and midterm mortality in these patients.
Methods
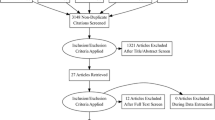
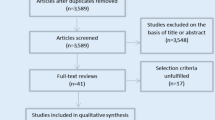
Studies on TAVI were searched in PubMed, Embase, and the Cochrane Library databases and were included in this review following predefined criteria. Data were extracted and pooled risk ratios (RR) were synthesized to explore the relationship between REF and 30-day plus midterm mortality.
Results
Twenty-eight studies comprising 14,099 patients were included in the analysis of the association of REF with the prognosis of patients after TAVI. An average increase in left ventricular ejection fraction of 8–10 % was observed among these patients after TAVI. REF was not related to the 30-day mortality [RR = 1.90, 95 % confidence interval (CI) = 0.80–4.47]; however, it was related to the midterm mortality (RR = 1.49, 95 %CI = 1.14–1.93) of patients undergoing TAVI. Patients with low-flow and low-gradient AS had a higher 30-day mortality (RR = 1.54, 95 %CI = 1.11–2.13) and midterm mortality rate (RR = 1.69, 95 %CI = 1.33–2.14) compared with AS patients without these characteristics. The mortality of TAVI patients was significantly lower than that of those undergoing conservative therapy, and was similar to that of patients undergoing surgical aortic valve replacement.
Conclusion
REF was not associated with 30-day mortality, but it was associated with the midterm mortality of TAVI patients. Patients with REF could benefit from TAVI compared with conservative therapy.
Zusammenfassung
Hintergrund
Die Transkatheter-Aortenklappenimplantation (TAVI) ist sicher und wirksam bei Patienten mit Aortenstenose (AS) und hohem Operationsrisiko. Jedoch ist die Wirksamkeit der TAVI bei AS-Patienten mit verminderter linksventrikulärer Ejektionsfraktion (LVEF) umstritten. Ziel der vorliegenden Übersicht war es, die Wirksamkeit der TAVI und die Auswirkungen einer verminderten LVEF auf die 30-Tage- und mittelfristige Mortalität bei diesen Patienten zu klären,
Methoden
Es wurde nach Studien zur TAVI in den Datenbanken PubMed, Embase und Cochrane Library gesucht. Diese Studien wurden nach vorher festgelegten Kriterien in die Auswertung einbezogen. Die Daten wurden extrahiert und die gepoolten relativen Risiken ermittelt, um die Beziehung zwischen einer verminderten LVEF und der 30-Tage- bzw. der mittelfristigen Mortalität zu untersuchen.
Ergebnisse
Es wurden 28 Studien mit 14.099 Patienten in die Auswertung eingeschlossen, um den Zusammenhang zwischen einer verminderten LVEF und der Prognose von Patienten nach TAVI zu ermitteln. Ein durchschnittlicher Anstieg von 8–10 % des LVEF wurde bei diesen Patienten nach TAVI festgestellt. Eine verminderte LVEF war nicht mit der 30-Tage-Mortalität assoziiert [RR = 1,90; 95 %-Konfidenzintervall (CI): 0,80–4,47], jedoch mit der mittelfristigen Mortalität (RR = 1,49; 95 %-KI: 1,14–1,93) der Patienten, bei denen eine TAVI erfolgte. Patienten mit niedrigem Fluss und niedrigem Gradienten der AS wiesen im Vergleich zu AS-Patienten ohne diese Merkmale eine höhere 30-Tage- (RR = 1,54; 95 %-KI: 1,11–2,13) und mittelfristige Mortalität auf (RR = 1,69; 95 %-KI: 1,33–2,14). Die Mortalität der TAVI-Patienten war deutlich niedriger als bei konservativer Therapie und ähnlich wie bei einer Aortenklappenersatzoperation.
Schlussfolgerung
Eine verminderte LVEF war nicht mit der 30-Tage-Mortalität, aber mit der mittelfristigen Mortalität von TAVI-Patienten assoziiert. Patienten mit verminderter LVEF konnten gegenüber der konservativen Therapie von der TAVI profitieren.





Similar content being viewed by others
References
Smith CR, Leon MB, Mack MJ et al (2011) Transcatheter versus surgical aortic-valve replacement in high-risk patients. N Engl J Med 364(23):2187–2198
Leon MB, Smith CR, Mack M et al (2010) Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med 363(17):1597–1607
Tamburino C, Capodanno D, Ramondo A et al (2011) Incidence and predictors of early and late mortality after transcatheter aortic valve implantation in 663 patients with severe aortic stenosis. Circulation 123(3):299–308
Moat NE, Ludman P, Belder MA de et al (2011) Long-term outcomes after transcatheter aortic valve implantation in high-risk patients with severe aortic stenosis: the U.K. TAVI (United Kingdom Transcatheter Aortic Valve Implantation) registry. J Am Coll Cardiol 58(20):2130–2138
Toggweiler S, Humphries KH, Lee M et al (2013) 5-year outcome after transcatheter aortic valve implantation. J Am Coll Cardiol 61(4):413–419
Zahn R, Gerckens U, Linke A et al (2013) Predictors of one-year mortality after transcatheter aortic valve implantation for severe symptomatic aortic stenosis. Am J Cardiol
Kodali SK, Williams MR, Smith CR et al (2012) Two-year outcomes after transcatheter or surgical aortic-valve replacement. N Engl J Med 366(18):1686–1695
Bleiziffer S, Mazzitelli D, Opitz A et al (2012) Beyond the short-term: clinical outcome and valve performance 2 years after transcatheter aortic valve implantation in 227 patients. J Thorac Cardiovasc Surg 143(2):310–317
Codner P, Assali A, Dvir D et al (2013) Two-year outcomes for patients with severe symptomatic aortic stenosis treated with transcatheter aortic valve implantation. Am J Cardiol
Hakki AH, Kimbiris D, Iskandrian AS et al (1980) Angina pectoris and coronary artery disease in patients with severe aortic valvular disease. Am Heart J 100(4):441–449
Ross J Jr, Braunwald E (1968) Aortic stenosis. Circulation 38(1 Suppl):61–67
Tribouilloy C, Levy F, Rusinaru D et al (2009) Outcome after aortic valve replacement for low-flow/low-gradient aortic stenosis without contractile reserve on dobutamine stress echocardiography. J Am Coll Cardiol 53(20):1865–1873
Nishimura RA, Grantham JA, Connolly HM et al (2002) Low-output, low-gradient aortic stenosis in patients with depressed left ventricular systolic function: the clinical utility of the dobutamine challenge in the catheterization laboratory. Circulation 106(7):809–813
Quere JP, Monin JL, Levy F et al (2006) Influence of preoperative left ventricular contractile reserve on postoperative ejection fraction in low-gradient aortic stenosis. Circulation 113(14):1738–1744
Pereira JJ, Lauer MS, Bashir M et al (2002) Survival after aortic valve replacement for severe aortic stenosis with low transvalvular gradients and severe left ventricular dysfunction. J Am Coll Cardiol 39(8):1356–1363
Levy F, Laurent M, Monin JL et al (2008) Aortic valve replacement for low-flow/low-gradient aortic stenosis operative risk stratification and long-term outcome: a European multicenter study. J Am Coll Cardiol 51(15):1466–1472
Amabile N, Ramadan R, Ghostine S et al (2012) Early and mid-term cardiovascular outcomes following TAVI: Impact of pre-procedural transvalvular gradient. Int J Cardiol
Hayashida K, Morice MC, Chevalier B et al (2012) Sex-related differences in clinical presentation and outcome of transcatheter aortic valve implantation for severe aortic stenosis. J Am Coll Cardiol 59(6):566–571
Houthuizen P, Van Garsse LA, Poels TT et al (2012) Left bundle-branch block induced by transcatheter aortic valve implantation increases risk of death. Circulation 126(6):720–728
Nombela-Franco L, Webb JG, Jaegere PP de et al (2012) Timing, predictive factors, and prognostic value of cerebrovascular events in a large cohort of patients undergoing transcatheter aortic valve implantation. Circulation 126(25):3041–3053
Wenaweser P, Pilgrim T, Roth N et al (2011) Clinical outcome and predictors for adverse events after transcatheter aortic valve implantation with the use of different devices and access routes. Am Heart J 161(6):1114–1124
Stroup DF, Berlin JA, Morton SC et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283(15):2008–2012
Moher D, Liberati A, Tetzlaff J et al (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097
Elm E von, Altman DG, Egger M et al (2007) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 370(9596):1453–1457
Zhang J, Yu KF (1998) What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. JAMA 280(19):1690–1691
Seiffert M, Schnabel R, Conradi L et al (2012) Predictors and outcomes after transcatheter aortic valve implantation using different approaches according to the valve academic research consortium definitions. Catheter Cardiovasc Interv
Amabile N, Azmoun A, Ghostine S et al (2012) Incidence, predictors and prognostic value of serious hemorrhagic complications following transcatheter aortic valve implantation. Int J Cardiol
Elhmidi Y, Bleiziffer S, Piazza N et al (2013) The evolution and prognostic value of N-terminal brain natriuretic peptide in predicting 1-year mortality in patients following transcatheter aortic valve implantation. J Invasive Cardiol 25(1):38–44±30.32
Lauten A, Zahn R, Horack M et al (2012) Transcatheter aortic valve implantation in patients with low-flow, low-gradient aortic stenosis. JACC Cardiovasc Interv 5(5):552–559
Sinning JM, Horack M, Grube E et al (2012) The impact of peripheral arterial disease on early outcome after transcatheter aortic valve implantation: results from the German Transcatheter Aortic Valve Interventions Registry. Am Heart J 164(1):102–110 e101
Rodes-Cabau J, Webb JG, Cheung A et al (2010) Transcatheter aortic valve implantation for the treatment of severe symptomatic aortic stenosis in patients at very high or prohibitive surgical risk: acute and late outcomes of the multicenter Canadian experience. J Am Coll Cardiol 55(11):1080–1090
Stohr R, Dohmen G, Herpertz R et al (2011) Thirty-day outcome after transcatheter aortic valve implantation compared with surgical valve replacement in patients with high-risk aortic stenosis: a matched comparison. Coron Artery Dis 22(8):595–600
Meguro K, Lellouche N, Yamamoto M et al (2013) Prognostic value of QRS duration after transcatheter aortic valve implantation for aortic stenosis using the core valve. Am J Cardiol
Stortecky S, Buellesfeld L, Wenaweser P et al (2013) Atrial fibrillation and aortic stenosis: impact on clinical outcomes among patients undergoing transcatheter aortic valve implantation. Circ Cardiovasc Interv 6(1):77–84
Wendler O, Walther T, Schroefel H et al (2013) Transapical aortic valve implantation: mid-term outcome from the SOURCE registry. Eur J Cardiothorac Surg 43(3):505–511 (discussion 511–502)
Pilgrim T, Wenaweser P, Meuli F et al (2011) Clinical outcome of high-risk patients with severe aortic stenosis and reduced left ventricular ejection fraction undergoing medical treatment or TAVI. PLoS One 6(11):e27556
Munoz-Garcia AJ, Jimenez-Navarro MF, Rodriguez-Bailon I et al (2012) Impact of transcatheter aortic valve implantation with the CoreValve prosthesis in patients with severe aortic stenosis and left ventricular dysfunction. Int J Cardiol 157(1):124–125
Ewe SH, Ajmone Marsan N, Pepi M et al (2010) Impact of left ventricular systolic function on clinical and echocardiographic outcomes following transcatheter aortic valve implantation for severe aortic stenosis. Am Heart J 160(6):1113–1120
Gotzmann M, Rahlmann P, Hehnen T et al (2012) Heart failure in severe aortic valve stenosis: prognostic impact of left ventricular ejection fraction and mean gradient on outcome after transcatheter aortic valve implantation. Eur J Heart Fail 14(10):1155–1162
Fraccaro C, Al-Lamee R, Tarantini G et al (2012) Transcatheter aortic valve implantation in patients with severe left ventricular dysfunction: immediate and mid-term results, a multicenter study. Circ Cardiovasc Interv 5(2):253–260
Boon RM van der, Nuis RJ, Van Mieghem NM et al (2012) Clinical outcome following Transcatheter Aortic Valve Implantation in patients with impaired left ventricular systolic function. Catheter Cardiovasc Interv 79(5):702–710
Unbehaun A, Pasic M, Buz S et al (2012) Transapical aortic valve implantation in patients with severely depressed left ventricular function. J Thorac Cardiovasc Surg 143(6):1356–1363
Erez A, Segev A, Medvedofsky D et al (2014) Factors affecting survival in men versus women following transcatheter aortic valve implantation. Am J Cardiol 113(4):701–705
Barbanti M, Binder RK, Dvir D et al (2014) Prevalence and impact of preoperative moderate/severe tricuspid regurgitation on patients undergoing transcatheter aortic valve replacement. Catheter Cardiovasc Interv
El-Mawardy M, Wubken-Kleinfeld N, Schwarz B et al (2014) Transcatheter aortic valve implantation in patients with severely reduced left ventricular systolic function: a single-center experience. Clin Res Cardiol 103(8):621–630
Elmariah S, Palacios IF, McAndrew T et al (2013) Outcomes of transcatheter and surgical aortic valve replacement in high-risk patients with aortic stenosis and left ventricular dysfunction: results from the Placement of Aortic Transcatheter Valves (PARTNER) trial (cohort A). Circ Cardiovasc Interv 6(6):604–614
Barbash IM, Minha S, Ben-Dor I et al (2014) Relation of preprocedural assessment of myocardial contractility reserve on outcomes of aortic stenosis patients with impaired left ventricular function undergoing transcatheter aortic valve implantation. Am J Cardiol 113(9):1536–1542
Ben-Dor I, Maluenda G, Iyasu GD et al (2012) Comparison of outcome of higher versus lower transvalvular gradients in patients with severe aortic stenosis and low (< 40 %) left ventricular ejection fraction. Am J Cardiol 109(7):1031–1037
Clavel MA, Webb JG, Rodes-Cabau J et al (2010) Comparison between transcatheter and surgical prosthetic valve implantation in patients with severe aortic stenosis and reduced left ventricular ejection fraction. Circulation 122(19):1928–1936
Bauer F, Coutant V, Bernard M et al (2013) Patients with severe aortic stenosis and reduced ejection fraction: earlier recovery of left ventricular systolic function after transcatheter aortic valve implantation compared with surgical valve replacement. Echocardiography
Gotzmann M, Lindstaedt M, Bojara W et al (2012) Clinical outcome of transcatheter aortic valve implantation in patients with low-flow, low gradient aortic stenosis. Catheter Cardiovasc Interv 79(5):693–701
O’Sullivan CJ, Stortecky S, Heg D et al (2013) Clinical outcomes of patients with low-flow, low-gradient, severe aortic stenosis and either preserved or reduced ejection fraction undergoing transcatheter aortic valve implantation. Eur Heart J 34(44):3437–3450
Le Ven F, Freeman M, Webb J et al (2013) Impact of low flow on the outcome of high-risk patients undergoing transcatheter aortic valve replacement. J Am Coll Cardiol 62(9):782–788
Elhmidi Y, Piazza N, Krane M et al (2014) Clinical presentation and outcomes after transcatheter aortic valve implantation in patients with low flow/low gradient severe aortic stenosis. Catheter Cardiovasc Interv 84(2):283–290
Smith N, McAnulty JH, Rahimtoola SH (1978) Severe aortic stenosis with impaired left ventricular function and clinical heart failure: results of valve replacement. Circulation 58(2):255–264
Carabello BA, Green LH, Grossman W et al (1980) Hemodynamic determinants of prognosis of aortic valve replacement in critical aortic stenosis and advanced congestive heart failure. Circulation 62(1):42–48
Ross J Jr (1985) Afterload mismatch in aortic and mitral valve disease: implications for surgical therapy. J Am Coll Cardiol 5(4):811–826
Vaquette B, Corbineau H, Laurent M et al (2005) Valve replacement in patients with critical aortic stenosis and depressed left ventricular function: predictors of operative risk, left ventricular function recovery, and long term outcome. Heart 91(10):1324–1329
Morris JJ, Schaff HV, Mullany CJ et al (1993) Determinants of survival and recovery of left ventricular function after aortic valve replacement. Ann Thorac Surg 56(1):22–29 (discussion 29–30)
Connolly HM, Oh JK, Schaff HV et al (2000) Severe aortic stenosis with low transvalvular gradient and severe left ventricular dysfunction:result of aortic valve replacement in 52 patients. Circulation 101(16):1940–1946
Powell DE, Tunick PA, Rosenzweig BP et al (2000) Aortic valve replacement in patients with aortic stenosis and severe left ventricular dysfunction. Arch Intern Med 160(9):1337–1341
Borz B, Durand E, Godin M et al (2012) Incidence, predictors and impact of bleeding after transcatheter aortic valve implantation using the balloon-expandable Edwards prosthesis. Heart
Monin JL, Quere JP, Monchi M et al (2003) Low-gradient aortic stenosis: operative risk stratification and predictors for long-term outcome: a multicenter study using dobutamine stress hemodynamics. Circulation 108(3):319–324
Compliance with ethical guidelines
Conflict of interest. X. Luo, Z. Zhao, H. Chai, C. Zhang, Y. Liao, Q. Li, Y. Peng, W. Liu, X. Ren, Q. Meng, C. Chen, M. Chen, Y. Feng, and D. Huang state that there are no conflicts of interest. The accompanying manuscript does not include studies on humans or animals.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Luo, X., Zhao, Z., Chai, H. et al. Efficacy of transcatheter aortic valve implantation in patients with aortic stenosis and reduced LVEF. Herz 40 (Suppl 2), 168–180 (2015). https://doi.org/10.1007/s00059-014-4193-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-014-4193-z
Keywords
- Aortic stenosis
- Reduced ejection fraction
- Transcatheter aortic valve implantation
- Conservative treatment
- Mortality