Abstract
Purpose
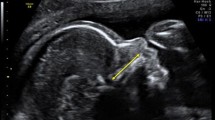
Our study was designed to investigate premaxillary–maxillary suture growth in fetuses from the first trimester of pregnancy using the B‑ultrasound technique in order to determine the suture fusion time.
Methods
We selected 169 healthy Han singleton pregnancies as subjects. All subjects received routine pregnancy tests and were divided into three groups based on the gestational age of the fetus: group 1, the 11th gestational week; group 2, the 12th gestational week; and group 3, the 13th gestational week. Fetal biometric measurements were recorded during consecutive prenatal ultrasonographic examinations. These measurements included nuchal translucency thickness, crown–rump length, and premaxillary–maxillary length. Intergroup comparisons were performed using analysis of variance (ANOVA).
Results
The premaxillary–maxillary suture grows gradually and its measured length at the 11th, 12th and 13th week was 0.54 cm, 0.65 cm, and 0.74 cm, respectively. We observed a significant linear correlation between the premaxillary–maxillary length and the week of gestation in the first trimester. The growth rate of the maxilla at the 11th, the 12th and the 13th week are significantly different with a descending order of growth rates being week 12, week 11 and week 13, with the 12th week rate being the most rapid.
Conclusion
The premaxillary and maxillary growth at 11 and 12 gestational weeks in the first trimester steadily accelerated, peaking at the 12th week. The rate of growth slows down after week 12 which may be associated with the fusion of the premaxillary–maxillary suture.
Zusammenfassung
Ziel
Die vorliegende Studie wurde durchgeführt, um die Entwicklung der Sutur zwischen Prämaxilla und Maxilla bei Föten im ersten Schwangerschaftsdrittel mittels B‑Ultraschalltechnik zu untersuchen und den Zeitpunkt der Suturverknöcherung zu bestimmen.
Methode
An der Studie nahmen 169 gesunde Schwangere (Mehrlingsgebärende ausgeschlossen) teil. Alle Teilnehmerinnen wurden regelmäßig routinemäßig untersucht und wurden in drei Gruppen eingeteilt, basierend auf dem Gestationsalter des Fötus: Gruppe 1: 11. Schwangerschaftswoche (SSW); Gruppe 2: 12. SSW, und Gruppe 3: 13. SSW. Die biometrische Vermessung der Föten wurde während der konsekutiven pränatalen Ultraschalluntersuchungen durchgeführt. Diese Messungen enthielten Nackentransparenzmessung, Schädel-Steiß-Länge und Länge der Prämaxilla-Maxilla. Vergleiche zwischen den Gruppen wurden mittels Varianzanalyse (ANOVA) durchgeführt.
Ergebnisse
Die Sutur Prämaxilla-Maxilla entwickelte sich kontinuierlich, wobei ihre Länge in der 11., 12. und 13. SSW 0,54 cm, 0,65 cm und 0.74 cm beträgt. Wir konnten eine signifikante lineare Korrelation zwischen Prämaxilla-Maxilla-Länge und der SSW im ersten Schwangerschaftsdrittel beobachten. Das maxilläre Wachstum in der 11., 12. und 13. SSW unterscheidet sich signifikant, wobei die Wachstumsrate in der 12. SSW am höchsten ist, gefolgt von der 11. und 13. SSW.
Schlussfolgerung
Das Wachstum der Prämaxilla und Maxilla nahm in der 11. und 12. SSW stetig zu, und wies einen Wachstumsgipfel in der 12. SSW auf. Die Wachstumsrate verlangsamte sich nach der 12. SSW, was sich möglicherweise auf die Verknöcherung der Sutur Prämaxilla-Maxilla zurückführen lässt.



Similar content being viewed by others
References
AlSarheed M (2015) A comparative study of oral health amongst trisomy 21 children living in Riyadh, Saudi Arabia: Part 1 caries, malocclusion, trauma. Saudi Dent J 27:220–223. https://doi.org/10.1016/j.sdentj.2015.03.003
Barteczko K, Jacob M (2004) A re-evaluation of the premaxillary bone in humans. Anat Embryol (berl) 207:417–437. https://doi.org/10.1007/s00429-003-0366-x
Behrents RG, Harris EF (1991) The premaxillary-maxillary suture and orthodontic mechanotherapy. Am J Orthod Dentofacial Orthop 99:1–6. https://doi.org/10.1016/s0889-5406(05)81673-7
Cicero S, Curcio P, Rembouskos G et al (2004) Maxillary length at 11–14 weeks of gestation in fetuses with trisomy 21. Ultrasound Obstet Gynecol 24:19–22. https://doi.org/10.1002/uog.1077
Gu LL (2012) Study on new technique of prenatal ultrasound screening and diagnosis of maxillofacial structural malformations in first-trimester. Southern medical university, Guangdong (Master’s thesis)
Holton NE, Franciscus RG, Nieves MA et al (2010) Sutural growth restriction and modern human facial evolution: an experimental study in a pig model. J Anat 216:48–61. https://doi.org/10.1111/j.1469-7580.2009.01162.x
Ishii M, Sun J, Ting MC et al (2015) The development of the calvarial bones and sutures and the pathophysiology of craniosynostosis. Curr Top Dev Biol 115:131–156. https://doi.org/10.1016/bs.ctdb.2015.07.004
Karki S, Joshi KS, Tamrakar SR et al (2013) Nuchal translucency in normal fetus and its variation with increasing crown rump length (CRL) and gestational age. Kathmandu Univ Med J 11:282–286. https://doi.org/10.3126/kumj.v11i4.12522
Lauridsen H, Hansen BF, Reintoft I et al (2005) Short hard palate in prenatal trisomy 21. Orthod Craniofac Res 8:91–95. https://doi.org/10.1111/j.1601-6343.2005.00318.x
Li ZH, Hong Y, Qin LL et al (2016) The value of nuchal translucency thickness in the fetal chromosome abnormality screening. J Pract Med 32:402–405
Liao D (2015) Correlation of fetal nuchal translucency sonography and abnormal fetal development. Chin J Fam Plann 23:239–241
Mak KL (1969) An analysis of treated orthodontic patients in Hong Kong. Dent Mag Oral Top 86:258–259
Markov D, Jacquemyn Y, Leroy Y (2003) Bilateral cleft lip and palate associated with increased nuchal translucency and maternal cocaine abuse at 14 weeks of gestation. Clin Exp Obstet Gynecol 30:109–110
Maureille B, Bar D (1999) The premaxilla in Neandertal and early modern children: ontogeny and morphology. J Hum Evol 37:137–152. https://doi.org/10.1006/jhev.1999.0312
Mooney MP, Siegel MI (1986) Developmental relationship between premaxillary-maxillary suture patency and anterior nasal spine morphology. Cleft Palate J 23:101–107
Mooney MP, Siegel MI (1991) Premaxillary-maxillary suture fusion and anterior nasal tubercle morphology in the chimpanzee. Am J Phys Anthropol 85:451–456. https://doi.org/10.1002/ajpa.1330850408
Nicolaides KH, Azar G, Byrne D et al (1992) Fetal nuchal translucency: ultrasound screening for chromosomal defects in first trimester of Pregnaney. BMJ 304:867–869. https://doi.org/10.1136/bmj.304.6831.867
Ruan WH, Winger JN, Yu JC et al (2008) Induced premaxillary suture fusion: class III malocclusion model. J Dent Res 87:856–860. https://doi.org/10.1177/154405910808700901
Shyu IL, Yang MJ, Wang HI et al (2014) Fetal maxillary and mandibular length in normal pregnancies from 11 weeks’ to 13+6 weeks’ gestation: a Taiwanese study. Taiwan J Obstet Gynecol 53:53–56. https://doi.org/10.1016/j.tjog.2012.05.003
Singh GD (1999) Morphologic determinants in the etiology of class III malocclusions: a review. Clin Anat 12:382–405. https://doi.org/10.1002/(SICI)1098-2353(1999)12:5<382::AID-CA9>3.0.CO;2-0
Stojanović Z, Nikolić P, Nikodijević A (2013) Cephalometric assessment of maxillary length in Serbian children with skeletal class III. Vojnosanit Pregl 70:645–652. https://doi.org/10.2298/vsp110224042s
Szuhanek C, Gâdea PE, Sişu AM et al (2011) Cephalometric investigation of Class III dentoalveolar malocclusion. Rom J Morphol Embryol 52:1343–1346
Tan CY, Qi H, Zhang AQ et al (2012) The evaluation of nuchal translucency abnormality in 115 cases. Chin J Prac Gynecol Obstet 28:56–58
Trevizan M, Consolaro A (2017) Premaxilla: an independent bone that can base therapeutics for middle third growth! Dental Press J Orthod 22:21–26. https://doi.org/10.1590/2177-6709.22.2.021-026.oin
Wu BH, Kou XX, Zhang C et al (2017) Stretch force guides finger-like pattern of bone formation in suture. PLoS ONE 12:e177159. https://doi.org/10.1371/journal.pone.0177159
Xue F, Wong RW, Rabie AB (2010) Genes, genetics, and Class III malocclusion. Orthod Craniofac Res 13:69–74. https://doi.org/10.1111/j.1601-6343.2010.01485.x
Zhang WJ, Fang JX (2000) Embryonic development for the jaws. J Linyi Med Coll 22:161–162
Zhang WJ, Ma YZ, Meng QL et al (1999) Observation of primary ossification center of fetal cranium viscerale. J Linyi Med Coll 21:5–6
Acknowledgements
This study was funded by the key project of the medical science and technology plan of Zhejiang province (2012ZDA028).
The authors are very grateful to James L. Borke, Professor and Assistant Dean of the College of Dental Medicine, Western University of Health Sciences, Pomona, CA, USA and Raymond Wong, Professor of Pediatric Dentistry from California, San Francisco, CA, USA, for reviewing this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
W.-H. Ruan, W.-Q. Han, M.-l. Huang, K.-l. Huang and L.-l. Jin declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Ruan, Wh., Han, Wq., Huang, Ml. et al. Premaxillary–maxillary suture development in the first trimester. J Orofac Orthop 80, 25–31 (2019). https://doi.org/10.1007/s00056-018-0163-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00056-018-0163-z