Abstract
Objectives
Several public health interventions are not described, not evaluated and not transferred. The objective was to assess the feasibility and acceptability of using a description model making a distinction between interventions’ transferable elements, and those that are more context-specific, to make their evaluation and transferability easier.
Methods
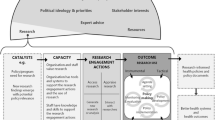
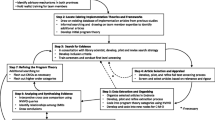
The theoretical distinction between an intervention function and its form in a specific context has been empirically explored. A community-based intervention (named “Ciné-Ma-Santé”) has been described, using a “key function/implementation/context” model. This process has been co-constructed through qualitative research and knowledge exchange process between project leaders and researchers from different disciplines.
Results
The use of the model proves feasible and useful for both project leaders and researchers. Nine key functions were described, as well as their implementation and the features of the intervention context.
Conclusions
Rendering explicit key functions of public health interventions could constitute a useful step to their evaluation and transfer. It enables the formulation of hypotheses regarding the potentially standardizable elements of interventions, and elements that can be modified while maintaining the integrity of the intervention.


Similar content being viewed by others
References
Barnes M, Matka E, Sullivan H (2003) Evidence, understanding and complexity evaluation in non-linear systems. Evaluation 9:265–284
Basson J-C, Haschar-Noé N, Honta M (2013) Toulouse, une «figure urbaine de la santé publique». À propos de l’action publique municipale de lutte contre les inégalités sociales de santé. Rev Épidémiol Santé Publique 61:81–88
Bauman LJ, Stein REK, Ireys HT (1991) Reinventing fidelity: the transfer of social technology among settings. J Community Psychol 19:619–639
Bernier J (2014) La Recherche Partenariale Comme Espace de Soutien à L’innovation. Global Health Promot 21:58–63
Bonell C, Fletcher A, Morton M, Lorenc T, Moore L (2012) Realist randomised controlled trials: a new approach to evaluating complex public health interventions. Soc Sci Med 75:2299–2306
Cargo M, Mercer SL (2008) The value and challenges of participatory research: strengthening its practice. An Rev Public Health 29:325–350
Delpierre C, Kelly-Irving M (2011) To what extent are biological pathways useful when aiming to reduce social inequalities in cancer? Europ J Public Health 21:398–399
Evans R, Scourfield J, Murphy S (2014) Pragmatic, formative process evaluations of complex interventions and why we need more of them. J Epidemiol Community Health. doi:10.1136/jech-2014-204806
Funnell SC, Rogers PJ (2011) Purposeful program theory: effective use of theories of change and logic models. Wiley, New York
Graham ID, Logan J, Harrison MB, Straus SE, Tetroe J, Caswell W, Robinson N (2006) Lost in knowledge translation: time for a map? J Contin Educ Health Prof 26:13–24
Hawe P, Potvin L (2009) What is population health intervention research? Can J Public Health 100(1):8–14
Hawe P, Shiell A, Riley T (2004) Complex interventions: how “out of control” can a randomised controlled trial be? BMJ 328:1561–1563
Hawe P, Shiell A, Riley T (2009) Theorising Interventions as events in systems. Am J Community Psychol 43:267–276
Lang T, Kelly-Irving M, Delpierre C (2009) Inequalities in health: from the epidemiologic model towards intervention. Pathways and accumulations along the life course. Rev Epidémiol Santé Publique 57:429–435
Lang T, Bidault E, Villeval M, Alias F, Gandouet B, Servat M, Théis I, Breton E, Haschar-Noé N, Grosclaude P (2015) A health equity impact assessment umbrella program (AAPRISS) to tackle social inequalities in health: program description. Global Health Promot. pii:1757975914568127 (Epub ahead of print)
Lapalme J, Bisset S, Potvin L (2013) Role of context in evaluating neighbourhood interventions promoting positive youth development: a narrative systematic review. Int J Public Health 59:31–42
Mackenzie M, O’Donnell C, Halliday E, Sridharan S, Platt S (2010) Do health improvement programmes fit with MRC guidance on evaluating complex interventions? BMJ (Clin Res Ed.) 340:c185
Marchal B, van Belle S, van Olmen J, Hoerée T, Kegels G (2012) Is realist evaluation keeping its promise? A review of published empirical studies in the field of health systems research. Evaluation 18:192–212
Masuda JR, Zupancic T, Crighton E, Muhajarine N, Phipps E (2014) Equity-focused knowledge translation: a framework for “reasonable action” on health inequities. Int J Public Health 59:457–464
Michie S, Fixsen D, Grimshaw JM, Eccles MP (2009) Specifying and reporting complex behaviour change interventions: the need for a scientific method. Implement Sci 4:40
Patton MQ (1997) Utilization-focused evaluation: the new century text, 3rd edn. Sage, Thousand Oaks
Patton MQ, LaBossière F (2012) L’évaluation axée sur l’utilisation. In: Ridde V, Dagenais C (eds) Approches et pratiques en évaluation de programmes, 2nd edn. Presses de l’Université de Montréal, Montréal, pp 145–160
Pawson R, Tilley N (1997) Realistic evaluation. Sage, London
Pearson TA, Lewis C, Wall S, Jenkins PL, Nafziger A, Weinehall L (2001) Dissecting the “black box” of community intervention: background and rationale. Scand J Public Health 29:5–12
Potvin L, McQueen DD (2009) Practical dilemnas for health promotion evaluation. In: Potvin L, McQueen DD (eds) Health promotion evaluation practices in the Americas—values and research. Springer, New York, pp 25–45
Potvin L, Bilodeau A, Gendron S (2008) Trois Défis Pour L’évaluation En Promotion de La Santé. Promot Educ 15:17–21
Rychetnik L, Frommer M, Hawe P, Shiell A (2002) Criteria for evaluating evidence on public health interventions. J Epidemiol Community Health 56:119–127
Shiell A, Hawe P, Gold L (2008) Complex interventions or complex systems? Implications for health economic evaluation. BMJ 336:1281–1283
Shoveller J, Viehbeck S, Di Ruggiero E, Greyson D, Thomson K, Knight R (2015) A critical examination of representations of context within research on population health interventions. Crit Public Health. doi:10.1080/09581596.2015.1117577
Van Daele T, Van Audenhove C, Hermans D, Van Den Bergh O, Van Den Broucke S (2012) Empowerment implementation: enhancing fidelity and adaptation in a psycho-educational intervention. Health Promot Int 29:212–222
Villeval M, Ginsbourger T, Bidault E, Alias F, Delpierre C, Gaborit E, Kelly-Irving M, Manuello P, Grosclaude P, Lang T (2014) L’interdisciplinarité en action: les «mots-pièges» d’une recherche interdisciplinaire. Santé Publique 26:155–163
Villeval M, Bidault E, Gaborit E, Grosclaude P, Haschar-Noé N, Lang T (2015) Un programme de recherche interventionnelle (AAPRISS) visant à réduire les inégalités sociales de santé: méthodes et validation. Can J Public Health 106:e434–e441
Wang S, Moss JR, Hiller JE (2006) Applicability and transferability of interventions in evidence-based public health. Health Promot Int 21:76–83
Whitehead M (2007) A typology of actions to tackle social inequalities in health. J Epidemiol Community Health 61:473–478
WHO (1998) Health promotion evaluation: recommendation to policy-makers. Report of the WHO European Working Group on Health Promotion Evaluation. World Health Organisation Europe, Copenhagen. doi:10.1111/j.1365-2214.2004.00453.x/full
Woodward A, Kawachi I (2000) Why reduce health inequalities? J Epidemiol Community Health 54:923–929
Acknowledgments
This work was supported by the Institut National du Cancer (INCA N° 2011-009), the Agence Nationale de la Recherche (ANR-11-INEG-0003 “EVALISS”), the Agence Régionale de Santé Midi-Pyrénées (ARS), and the Fondation ARC pour la recherche sur le cancer for the PhD student MV (File n°DOC20140601025). We would like to thank the AAPRISS Scientific Committee: Franco Berrino, Pierre Blaise, Pierre Chauvin, Hercberg Serge, France Lert, Louise Potvin, and Alfred Spira.
The AAPRISS group: B Almudever, L Birelichie, E Breton, A Bulle, F Cayla, C Delpierre, P Ducournau, E Gaborit, B Gandouet, T Ginsbourger, E Godeau, A Guichard, N Haschar-Noé, M Kelly-Irving, A Lacouture, C Martin, A Mayère, P Manuello, I Poirot-Mazère, E Salaméro, M Servat, F Sicot, F Sordes-Ader, I Theis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
For the AAPRISS group see “Acknowledgments”.
Rights and permissions
About this article
Cite this article
Villeval, M., Bidault, E., Shoveller, J. et al. Enabling the transferability of complex interventions: exploring the combination of an intervention’s key functions and implementation. Int J Public Health 61, 1031–1038 (2016). https://doi.org/10.1007/s00038-016-0809-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00038-016-0809-9