Abstract
Objectives
To summarize evidence about (1) the costs of limited health literacy (HL) and (2) the cost-effectiveness of interventions to improve limited HL.
Methods
We performed a systematic review searching electronic databases and additional information resources. We included observational studies and interventional studies with HL-outcomes. We included populations at high risk for low HL and patients with (1) diabetes mellitus or (2) hyperlipidemia.
Results
We retrieved 2,340 papers and included 10 studies for analysis. The prevalence of limited HL is considerable (range 34–59%). On the health system level, the additional costs of limited HL range from 3 to 5% of the total health care cost per year. On the patient level, the additional expenditures per year per person with limited HL compared to persons with adequate HL range from US $143 to 7,798. Data on the cost-effectiveness of interventions to improve limited HL are scarce.
Conclusion
The costs of limited HL may be substantial, but few studies were retrieved and the results are heterogeneous.
Zusammenfassung
Fragestellung
Wie hoch sind (1) die Kosten von eingeschränkter Gesundheitskompetenz (GK) und (2) wie ist die Kosten-Effektivität von Interventionen zur Verbesserung der GK?
Methodik
Systematic Review unter Einbezug von elektronischen Datenbanken und zusätzlichen Informationsquellen. Eingeschlossene Studiendesigns: Beobachtungs- und Interventionsstudien mit GK als Outcome. Eingeschlossen waren Personen mit hohem Risiko für eingeschränkte GK oder Patienten mit (i) Diabetes mellitus oder (ii) Hyperlipidämie.
Ergebnisse
Von 2340 gefundenen Studien wurden 10 Studien in die Auswertung eingeschlossen. Die Prävalenz von eingeschränkter GK ist beträchtlich (zwischen 34% und 59%). Bezogen auf das Gesundheitssystem betragen die zusätzlichen Kosten auf Grund eingeschränkter GK zwischen 3 und 5% der jährlichen gesamten Gesundheitskosten. Beim Vergleich von Patienten mit eingeschränkter GK vs. nicht eingeschränkter GK belaufen sich die jährlichen zusätzlichen Kosten pro Person auf 143 bis 7,798 US $. Empirische Daten zur Kosten-Effektivität von Interventionen, die die GK verbessern sollen, sind lückenhaft.
Schlussfolgerung
Die Kosten von eingeschränkter GK sind möglicherweise beträchtlich, allerdings ist die Datenlage bisher spärlich und die Ergebnisse sind heterogen.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Health literacy (HL) has become an increasingly important skill of citizens for health relevant decisions in modern societies. In addition, navigation in modern health care systems gets more and more complex for patients (Kickbusch et al. 2006; Nielsen-Bohlman et al. 2004; Nutbeam 2000).
According to Nutbeam (2000) HL comprises three levels: (1) Basic/functional HL (i.e., sufficient basic reading and writing skills), (2) interactive HL (i.e., ability to extract health relevant information and derive meaning from different forms of communication), (3) critical HL (i.e., more advanced skills to critically analyse health relevant information and to use it for health decisions). Measures of HL cover health-related knowledge, attitudes, motivation, behavioral intentions, personal skills and self efficacy (Nutbeam 2000).
More research has been done to assess the association of limited HL with health/social outcomes (Kondilis et al. 2006). There is convincing evidence that limited HL is more prevalent in specific risk groups (such as low education groups) and is associated with poorer health/social outcomes and specific patterns of health care service use (DeWalt et al. 2004; Rudd et al. 1999).
Little is known, however, about the economic implications of limited HL on the health system. In addition, HL-data have most often been derived from US health care setting and transferability to other countries is unclear.
In this paper, we aim to systematically review the economic implications of limited HL by collecting evidence about the costs of limited HL and the cost-effectiveness of interventions to improve limited HL. Two research questions guided this systematic review: (1) What are the costs associated with limited HL. (2) What is the cost-effectiveness of interventions to improve HL?
Methods
We performed a systematic review in accordance with current guidelines (Drummond et al. 2005; NHS Centre for Reviews and Dissemination 2001). For methodological advice, we conducted a preliminary expert workshop of Swiss and international HL experts.
HL is generated in the society as a whole, i.e., in different societal areas (Kickbusch et al. 2006; Nielsen-Bohlman et al. 2004). HL may be generated in a private context (e.g., via educational learning in the family) or in the public environment (e.g., via health promotion programmes in schools) leading to improved HL in a broader sense. In addition, HL may be generated in the health care system for patients (via traditional patient education or patient self management programmes) leading to improved “Patient Literacy” (Table 1). We applied this concept in our review by grouping retrieved studies to either a “Culture and society” category (such as Personal and community health, Adult education, HL friendly environments) or to the “Health care system” category (such as Patient education, Patient self management).
We applied an existing outcome model for health promotion (Gesundheitsförderung Schweiz 2007; Nutbeam 2000). According to this model, health promotion interventions (e.g., personal development programmes) may lead to (1) improved HL. Improved HL may then lead to (2) improved intermediate health outcomes (e.g., healthy life styles) and, finally, to (3) improved health outcomes (e.g., reduced morbidity or improved health-related quality of life). We applied this outcome model in our review as follows: as the focus was on HL, included studies had to report HL-outcomes (additional intermediate or final outcomes were possible). Studies reporting only about intermediate or final outcomes, without HL-information, were excluded.
Data sources
We systematically searched electronic databases for studies (Medline, Embase, the Cochrane library, PsychInfo, CINHAL; from 1980 through January 2008; no language restriction; see Appendix 1 for search strategy). In addition, we screened databases specialized in economic evaluations (NHS-Economic Evaluation Database) or HL (Harvard School of Public Health [Health Literacy Studies]); National Library of Medicine [Current Bibliographies in Medicine, 2004-1]; Agency for Healthcare Research and Quality [Health Literacy and Cultural competency]. Furthermore, we screened selected books and reference lists, performed Internet searches and contacted experts. All references were stored in an EndNote X.1 database (Thomson/ISI ResearchSoft Berkeley, CA, USA).
To be included, observational studies assessing the costs of limited HL had to report about all of the following items: prevalence of limited HL (as a base for cost calculations); health/social consequences of limited HL (such as service use or morbidity); and costs of limited HL in money terms. Studies assessing the prevalence of HL levels on a population level (without health/social consequences or cost data) were included, as well, to provide information on measurement methods for HL and on the budget impact of results of cost of illness studies.
To be included, interventional studies assessing cost-effectiveness had to report about all of the following items: interventions directed at HL; HL-outcomes (or HL-components such as knowledge, attitudes, or skills; additional intermediate or final outcomes were possible); and costs [i.e., full economic evaluations that jointly compared costs and effects on HL of two or more alternatives (Drummond et al. 2005)].
For interventional studies, we included population groups with limited HL (as measured with established instruments) or groups known to be at high risk for limited HL (such as minority groups, elderly persons, or low education populations) (Rudd et al. 2004). We concentrated on such groups, as HL-interventions are expected to be most likely cost-effective in populations with the biggest need for improvement. In addition, this allows collecting evidence in intervention fields, where future programmes will probably be implemented.
To collect evidence about interventions directed at “Patient Literacy” in the health care system (according to our HL-framework; Table 1), we included patients with two health problems (irrespective of the patients’ HL-level, as it is specifically difficult to navigate and take health decisions in this expert oriented system for almost every patient): (1) Patients with diabetes mellitus and (2) patients with hyperlipidemia with established cardiovascular disease (i.e., secondary prevention indication). Our reasons to concentrate on two selected patient groups were as follows: First, a body of evidence already exists about traditional education programmes (as for hypertension or asthma therapy). To review this amount of literature would not be realistic for practical reasons. Second, the two selected health problems are of particular relevance due to their economic impact in the health care system. If interventions, directed at limited HL of such persons, were cost-effective, this might have relevant impact.
We excluded studies if interventions were directed at the general population (i.e., not targeting specific risk groups) or at patient groups with main health problems other than diabetes mellitus or hyperlipidemia (such as asthma). We included studies from developed countries (USA, Canada, Europe, Australia, New Zealand). We excluded reports from developing countries (with focus on poor basic Literacy skills), grey literature, editorials, and abstracts. These criteria were defined in advance and applied for all steps of inclusion assessment.
Data extraction and quality assessment
One reviewer screened titles and abstracts for relevance using a predefined form. Unclear cases were discussed with a second reviewer. Disagreements were resolved by consensus. To enhance reliability of the screening process, training sessions were held in advance and agreement was assessed in a random sample, using chance-adjusted kappa statistics. Agreement between reviewers was high (Kappa 0.86). Potentially relevant studies were ordered and assessed for inclusion by full text.
Data were extracted by one reviewer on data extraction forms and checked independently by a second reviewer. We extracted data on general study information (such as study design, definition of HL), study setting (e.g., level of population recruitment), population details (e.g., age, ethnicity), outcome (e.g., definition of low HL, HL-outcome, intermediate outcome), and cost information (e.g., description of currency, cost date, discounting).
We performed a quality assessment using selected criteria of methodological standards for health-economic studies (Berkman et al. 2004; Drummond et al. 2005; NHS Centre for Reviews and Dissemination 2001; Pignone et al. 2005). We covered aspects of internal and external validity (such as description of population recruitment; description of outcome measurement for HL; or description of cost measurement; for details of quality assessment items see Appendix 2).
Analysis
We present the included studies in a tabulated form. Due to considerable methodological heterogeneity between studies, no data pooling was possible. Major obstacles to pooling were diverse measurement tools and thresholds for limited HL as well as varying cost reporting and applied assumptions; minor obstacles were differences in description of study populations. The presentation format allows for a systematic overview on study characteristics to judge similarities and differences between studies.
Results
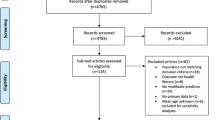
Our searches retrieved 2,340 potentially relevant studies (Fig. 1). We selected 72 studies that assessed either the prevalence of limited HL, the costs of limited HL or interventions to improve limited HL. Of those 72 studies, we excluded 22 interventional studies as they did not address the defined risk populations or did not report HL-outcomes and further 40 studies that assessed the effectiveness of interventions to improve limited HL but did not provide sufficient economic data.
The remaining ten studies were included for analysis. Of those ten studies, four reported prevalence data of limited HL in different populations (Kirsch et al. 1993; Kutner et al. 2005; OECD 2005; Rudd et al. 2004) and six studies (Friedland 1998; Howard et al. 2005; Sanders et al. 2007; Spycher 2006; Vernon et al. 2007; Weiss and Palmer 2004) assessed the costs of limited HL. No study reported cost-effectiveness data according to our inclusion criteria.
Costs of limited health literacy
We first report prevalence data that was applied in some of the included cost studies. Four studies (Kirsch et al. 1993; Kutner et al. 2005; OECD 2005; Rudd et al. 2004) provided data for the prevalence of limited HL in different populations (Table 2). The prevalence studies include data of more than 110,000 participants from nationally representative samples. Data most often represent the US population [1992 National Adult Literacy Survey, NALS (Kirsch et al. 1993); 2003 National Assessment of Adult Literacy, NAAL (Kutner et al. 2005); 2003 Adult Literacy and Life Skills Survey, ALL (OECD 2005); 2004 Health Activities Literacy Scale, HALS (Rudd et al. 2004)]. The 2003 Adult Literacy and Life Skills Survey also provides data for Norway, Italy, Canada, Bermuda, Mexico and Switzerland. Besides the US data, we have also extracted the information for the Swiss population.
Methods for the measurement of HL differed between studies and often relied on basic/functional HL, sometimes on interactive or critical HL. While the 1992 NALS measured degrees of skills in prose, document, and quantitative Literacy, the 2004 HALS project measured five health-related activities (health promotion; health protection; disease prevention; health care and maintenance; systems navigation), that represent HL in a more complex form. The HALS instrument comprises 191 health-related items extracted from previous surveys (mostly from NALS and IALS). The definitions of limited HL varied between studies, too. Some measurement scales comprise five (Kirsch et al. 1993; Rudd et al. 2004), some four categories (Kutner et al. 2005; OECD 2005) to distinguish between people with low, intermediate or adequate HL.
Overall, the proportion of people with limited HL varied between 9 and 23% for the lowest HL level and between 34 and 59% if the two lowest HL levels were taken together. Comparing studies with five and four HL categories, the lowest figures for the lowest HL category alone (1/5 or 1/4) were 19 or 9%, and for the two lowest categories together (2/5 or 2/4) 46 or 34%.
Six studies (Friedland 1998; Howard et al. 2005; Sanders et al. 2007; Spycher 2006; Vernon et al. 2007; Weiss and Palmer 2004) provided data for the costs of limited HL, some of them relying on the prevalence data above (Table 3). These studies include data of more than 54,000 participants. The cost studies most often applied data of selected US Medicaid or Medicare populations. Few individual patient data exist with HL-information and service cost data for the same person in one data set (Howard et al. 2005). Thus, some authors have modeled the costs of persons with limited HL using assumptions (Friedland 1998; Vernon et al. 2007). Spycher (2006) has combined 2004 ALL Swiss prevalence data for limited HL with US cost data (also applying several assumptions) to provide a rough calculation for the costs of limited HL for Switzerland.
The costs of limited HL are reported in two ways: Three studies (Friedland 1998; Spycher 2006; Vernon et al. 2007) report the additional health care costs due to limited HL on the system level (Table 4). According to these studies, the costs due to limited HL in the US or in Switzerland correspond to about 3–5% of the total health care spending [upper bound for the US: 10% (Vernon et al. 2007)].
Three other studies (Howard et al. 2005; Sanders et al. 2007; Weiss and Palmer 2004) assessed additional costs due to limited HL on the patient level in selected populations. The amount of additional health care expenditures with limited HL compared to a reference group with adequate HL is in a range of $143–7,798 per person per year (Fig. 2). Persons with low HL also showed a slightly increased use of inpatient and emergency room services (difference in probability: 0.05; 95%-CI: 0.00–0.10) and consumed an inefficient mix of health care services (Howard et al. 2005).
Costs of limited health literacy (HL) on the patient level. Differences in average annual health care costs per patient (for costs on the health care system level) (see Table 4). Three studies are included in this plot. For each study two different outcome items are provided. Values on the left side of the indifference line indicate lower health care costs of persons with limited HL, values on the right side of the indifference line indicate higher health care costs of persons with limited HL compared to persons with adequate HL. If provided by the primary authors, a 95%-CI is added to the point estimates of each study
Cost-effectiveness of interventions to improve limited health literacy
We retrieved no study that jointly compared costs and HL-outcomes for two alternatives according to our inclusion criteria. For example, one excluded systematic review (Norris et al. 2001) provided some information about the economic consequences to improve HL by patient self management programmes for diabetes, but only in relationship to clinical outcomes. Most primary studies with health-economic evaluations in this review failed to demonstrate effectiveness for the chosen clinical outcome, some studies only described the cost of intervention. In one study, the per-patient cost per unit improvement in glycemic control (as measured with HbA1c) was lower in the control group. No economic analyses in this review included indirect costs (productivity losses), no cost-benefit analyses were identified.
We did not retrieve studies from other sectors that assessed the cost-effectiveness of interventions to improve limited HL in specific risk groups (e.g., in workplace settings or for generation of HL-friendly environments in the community) (Kickbusch et al. 2006).
Methodological quality
In general, the methodological quality of the included studies for this review was moderate to fair. Surveys for the estimation of population representative HL levels often used sophisticated sample selection criteria. However, measurement of HL was not standardized. Cost studies also varied in their methodological quality. While five of six studies reported population characteristics and recruitment of participants sufficiently well, only one study (Sanders et al. 2007) described outcome measurement for service use in detail and only two (Howard et al. 2005; Weiss and Palmer 2004) of six studies described cost measurement in detail (e.g., quantities of resources use, currency and pricing date, discounting). None of the cost studies considered indirect costs. In addition, in all but one study (Sanders et al. 2007), health care costs of children and adolescents that may also be influenced by low HL are not included and costs may be an underestimate.
Discussion
The additional costs of limited HL may be substantial (ranges per year: on the system level: 3–5% of the total health care cost; on the patient level: $143–7,798 per person), but few studies were retrieved and the results are heterogenous. The evidence for the cost-effectiveness of interventions to improve limited HL is scarce.
To our knowledge, this is the first attempt to systematically summarize the economic impact of limited HL with a systematic review. We used a stepwise approach with implementation of an expert workshop, searches in electronic databases and inclusion of additional sources of information.
Our study has some limitations. First, the concept of HL is still under debate as well as methods for measurement of HL levels (Abel 2008; Kickbusch 2002). Therefore, we established an expert workshop in advance to discuss current methodological and conceptual problems in this area. Second, we may have missed relevant studies despite our attempts to retrieve further studies in addition to the electronic search results. Electronic retrieval of studies in the HL field is difficult. Authors sometimes do not (yet) use the term “health literacy” when they report about studies on improving knowledge or skills for daily health decisions. Third, the retrieved cost studies used solely data from the health care system. Little is known about the transferability of results to other societal areas, such as workplace settings. Finally, there is a substantial overlap between issues addressing HL and the area of health promotion/disease prevention. HL is seen as one key outcome of health promotion/disease prevention (Nutbeam 2000). Thus, in a broader sense any health promotion/disease prevention intervention covers aspects of improving HL (such as improvement of knowledge, change of attitudes and development of skills). Even though HL is sometimes seen as an enabling factor to apply health promotion messages in daily life (“empowerment”) (Nutbeam 2000), the distinction between the two areas is not always clear. Therefore, in order not to replicate existing research about the cost-effectiveness of health promotion/disease prevention interventions (Brügger et al. 2004; Rush et al. 2002), we concentrated on studies that explicitly covered issues of limited HL [i.e., HL (or its components) was conceptualized and measured in risk groups].
To our knowledge, no systematic review has so far assessed the economic impact of limited HL on the health care system- or the patient level. However, comparison data exist for the prevalence of limited HL in patient populations. One systematic review (Paasche-Orlow et al. 2005) assessed studies that examined the prevalence of limited HL specifically related to US health care or health services inquiries. The pooled weighted prevalence was 26% for low HL and 20% for marginal HL. Though that review did not provide nationally representative prevalence data, its estimates fit well with the prevalence data collected in our review.
The findings have serious implications for health policy. A considerable proportion of the assessed populations is deemed to have a HL level below the threshold considered to be adequate for increasingly difficult health-related tasks in the information society. Low HL is not only restricted to typical risk groups (such as ethnic minorities or migrants). A relevant part of inborn, native speakers is functionally illiterate with respect to health knowledge, health information retrieval, or performance of simple health-related problem solving (Rudd et al. 2004). Problems that may grow as electronic information sources (e.g., the internet or electronic decision aids) will be increasingly important for daily health decisions, as well as in the health care system (Parker et al. 2003).
Health care system reforms are urgently needed to improve communication and decision making between providers and patients. In addition, organisational development in the health care system is required to enable persons with low HL to navigate in HL-friendly environments (Rudd 2008).
Societal areas beyond the health care system may play an even bigger role in tackling low HL in the society as a whole. This applies to the educational sector (with adult educational programmes; school based interventions), workplace settings (with specifically tailored health promotion interventions) or family based programmes for ethnic minority groups.
However, little evidence is available if interventions that aim to improve HL in citizens/patients will reduce service costs or are cost-effective on a societal perspective. Two scenarios are possible: on one hand, persons who gain improved skills to retrieve updated health information might behave like uncritical “health care consumers”. Thus, they may show a greater demand for any new, apparently more effective and save, but also more expensive services. If such a trend takes place, it may be unlikely that the health care expenditures will decrease. On the other hand, interventions to improve HL might enable persons to critically check the supply on the health care market, to selectively choose services and, presumably more important, to take healthy decisions in their daily life settings (such as family, workplace, politics) (Kickbusch et al. 2006). Such changes may contribute to lower health care costs of formerly low HL populations.
Based on the findings of our review we suggest some future research issues in the HL field: (1) Standardized, validated measurement tools that take account for the complex nature of HL. (2) Measurement of HL-level distribution on the population level with such instruments. This may allow for robust prevalence data. (3) Application of methodological standards for conduct and reporting of health-economic studies in the HL field. This may reduce bias of study results. For example, the two concordant cost studies (Howard et al. 2005; Sanders et al. 2007) with lower cost estimates included a potentially less needy population compared to the discrepant study of Weiss and Palmer (2004), as different instruments to categorize HL levels were applied. Sound health-economic studies, based on robust prevalence data, are most needed to address major impediments for data pooling (such as diversity in HL measurement tools, thresholds for limited HL, reporting of costs and model assumptions). (4) Observational studies to prospectively assess the association between HL and health care costs with individual patient data in health care settings with different organisational features and normative background. For example, employing US data for modeling in European health care settings with compulsory health care insurance may be problematic (Drummond et al. 2005). Only one (Spycher 2006) out of the six retrieved cost studies took place outside the United States. This study employed US cost data for modeling in an European (Swiss) health care setting with compulsory health care insurance. (5) Interventional studies to prospectively assess the cost-effectiveness of interventions to improve limited HL. (6) Continuous conceptual research to better understand the link between health promotion/disease prevention interventions and interventions designed to improve HL.
Conclusion
The costs of limited HL for the health care system may be substantial. However, results of cost studies are heterogeneous, relate to selected groups and studies show methodological shortcomings. More research is needed to better understand the economic aspects of limited HL and the cost-effectiveness of interventions to improve HL.
References
Abel T (2008) Cultural capital and social inequality in health. J Epidemiol Commun H 62:e13
Berkman ND, Dewalt DA, Pignone MP, Sheridan SL, Lohr KN, Lux L, Sutton SF, Swinson T, Bonito AJ (2004) Literacy and health outcomes. Evid Rep Technol Assess (Summ): 1–8
Brügger U, Federspiel B, Kreuzer E, Horisberger B (2004) Ökonomische Beurteilung von Gesundheitsförderung und Prävention. Winterthur Institute of Health Economics Zurich University of Applied Sciences, Winterthur
DeWalt DA, Berkman ND, Sheridan S, Lohr KN, Pignone MP (2004) Literacy and health outcomes: a systematic review of the literature. J Gen Intern Med 19:1228–1239
Drummond M, Sculpher M, Torrance G, O’Brien B, Stoddart G (2005) Methods for the economic evaluation of health care programmes. Oxford University Press, Oxford
Friedland R (1998) Understanding health literacy: new estimates of the high costs of inadequate health literacy. In: Congress of the U.S. (ed) The price we pay for illiteracy, Washington, DC, pp 57–91
Gesundheitsförderung Schweiz (2007) Das Ergebnismodell im Überblick, vol 2007, Berne
Howard DH, Gazmararian J, Parker RM (2005) The impact of low health literacy on the medical costs of Medicare managed care enrollees. Am J Med 118:371–377
Kickbusch I (2002) Health literacy: a search for new categories. Health Promot Int 17:1–2
Kickbusch I, Wait S, Maag S (2006) Navigating health. The role of health literacy. Alliance for health and future. International Longevity Centre-UK, London
Kirsch I, Jungeblut A, Jenkins L, Kolstad A (1993) Adult literacy in America. A first look at the findings of the National Adult Literacy Survey. US Department of Education, Washington, DC
Kondilis BK, Soteriades ES, Falagas ME (2006) Health literacy research in Europe: a snapshot. Eur J Public Health 16:113
Kutner M, Greenberg E, Baer J (2005) A first look at the literacy of America’s adults in the 21st century. US National Center for Education Statistics, Washington, DC
NHS Centre for Reviews and Dissemination (2001) CRD’s guidance for those carrying out or commissioning reviews. University of York, York
Nielsen-Bohlman L, Panzer AM, Hamlin B, Kindig DA (2004) Health literacy. A prescription to end confusion. In: Institute of Medicine (ed). Institue of Medicine, Washington, DC
Norris SL, Engelgau MM, Narayan KM (2001) Effectiveness of self-management training in type 2 diabetes: a systematic review of randomized controlled trials. Diabetes Care 24:561–587
Nutbeam D (2000) Health literacy as a public health goal: a challenge for contemporary health education and communication strategies into the 21st century. Health Prom Int 15:259
OECD (2005) Learning a living. First results of the Adult Literacy and Life Skills survey. OECD, Ottawa and Paris
Paasche-Orlow MK, Parker RM, Gazmararian JA, Nielsen-Bohlman LT, Rudd RR (2005) The prevalence of limited health literacy. J Gen Intern Med 20:175–184
Parker RM, Ratzan SC, Lurie N (2003) Health literacy: a policy challenge for advancing high-quality health care. Health Aff (Millwood) 22:147–153
Pignone M, Saha S, Hoerger T, Lohr KN, Teutsch S, Mandelblatt J (2005) Challenges in systematic reviews of economic analyses. Ann Intern Med 142:1073–1079
Rudd RR (2008) The health literacy environment of hospitals and health centres. National Center for the Study of Adult Learning and Literacy, Boston, MA
Rudd RR, Moeykens BA, Colton TC (1999) Health and literacy. A review of medical and public health literature. In: Comings JGB, Smith C (eds) Annual review of adult learning and literacy. Jossey-Bass, New York
Rudd R, Kirsch I, Yamamoto K (2004) Literacy and health in America. Policy Information Report. Policy Information Center, Princeton, NJ
Rush B, Shiell A, Hawe P (2002) A census of economic evaluations of primary prevention interventions in population health. Department of Community Health Sciences and Centre for Health and Policy Studies, University of Calgary
Sanders LM, Thompson VT, Wilkinson JD (2007) Caregiver health literacy and the use of child health services. Pediatrics 119:e86–e92
Spycher S (2006) Ökonomische Aspekte der Gesundheitskompetenz. BASS, Büro für Arbeits- und Sozialpolitische Studien, Berne
Vernon J, Trujillo A, Rosenbaum S, DeBuono B (2007) Low health literacy: implications for national health policy. University of Connecticut. National Bureau of Economic Research, Storrs, CT
Weiss BD, Palmer R (2004) Relationship between health care costs and very low literacy skills in a medically needy and indigent Medicaid population. J Am Board Fam Pract 17:44–47
Acknowledgments
The authors are grateful to the participants of the expert workshop for the critical discussion of conceptual issues concerning HL and methodological support as well as to Dr. Phillip Stalder, information retrieval specialist, University of Zurich, Switzerland. This study was funded by Health Promotion Switzerland, Berne, Switzerland and Merck, Sharp & Dohme-Chibert AG, Glattbrugg-Opfikon, Switzerland. The funding sources were involved in the study design. They had no influence in the collection, analysis and interpretation of the data, and in writing of this report.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Appendix 1. Search strategy
Pubmed search strategy
#9 | Search #4 AND #5 Limits: Publication Date from 1980 |
#6 | Search #4 AND #5 |
#5 | Search Literacy [TIAB] |
#4 | Search #1 OR #3 |
#3 | Search “Meta-Analysis”[Publication Type] |
#1 | Search (“Economics”[Mesh]) OR (“economics”[Subheading]) OR (“Review”[Publication Type]) OR (“Clinical Trial”[Publication Type]) OR (“Comparative Study”[Publication Type]) OR (pre-post[TIAB]) OR (“pre-post”[TIAB]) OR (“before-after”[TIAB]) OR (before-after[TIAB]) OR (cost-effectiveness[TIAB]) OR (“cost-effectiveness”[TIAB]) OR (“cost-benefit”[TIAB]) OR (cost-benefit[TIAB]) OR (“cost of illness”[TIAB]) OR (“burden of disease”[TIAB]) |
Cochrane search strategy
ID | Search | Hits | Edit | Delete |
|---|---|---|---|---|
#1 | (Economic*):ti,ab,kw in Cochrane Reviews, Other Reviews, Clinical Trials, Technology Assessments and Economic Evaluations | 27966 | Edit | Delete |
#2 | (Review):pt or (Clinical Trial):pt or (Controlled):pt or (Comparative Study):pt or (Meta-Analysis):pt in Cochrane Reviews, Other Reviews, Clinical Trials, Technology Assessments and Economic Evaluations | 308798 | Edit | Delete |
#3 | (pre-post):ti,ab,kw or (before-after):ti,ab,kw or (cost-effectiveness):ti,ab,kw or (cost-benefit):ti,ab,kw in Cochrane Reviews, Other Reviews, Clinical Trials, Technology Assessments and Economic Evaluations | 15723 | Edit | Delete |
#4 | “cost of illness”:ti,ab,kw or “burden of disease”:ti,ab,kw in Cochrane Reviews, Other Reviews, Clinical Trials, Technology Assessments and Economic Evaluations | 2660 | Edit | Delete |
#5 | (#1 OR #2 OR #3 OR #4) | 333297 | Edit | Delete |
#6 | (Literacy):ti,ab,kw in Cochrane Reviews, Other Reviews, Clinical Trials, Technology Assessments and Economic Evaluations | 171 | Edit | Delete |
#7 | (#5 AND #6) | 132 | Edit | Delete |
#8 | (#7), from 1980 to 2008 | 132 | Edit | Delete |
Appendix 2. Applied quality items (Berkman et al. 2004; Drummond et al. 2005; NHS Centre for Reviews and Dissemination 2001; Pignone et al. 2005)
No. | Items | Comment/criteria | PREV | COST | CEFF |
|---|---|---|---|---|---|
1 ext | Population characteristics described in sufficient detail? (pop_sex_age_ethn_morb) | At least 3: sex; age; morbidities or social features (such as ethnicity; education; income) | PREV | COST | CEFF |
2 ext | Recruitment of population described in sufficient detail? (site_level) | Qual. description is sufficient; | PREV | COST | CEFF |
3 ext | Intervention described in sufficient detail? (intervention) | CEFF | |||
4 ext | Alternative described in sufficient detail? (alternative) | CEFF | |||
5 int | Randomisation procedure adequate? (gen of ran sequ; concealm of alloc) | Both have to be described for randomised studies | CEFF | ||
6 int | Completeness of follow up (follup_compl) | Completeness fulfilled: >=80% | CEFF | ||
7 int | Blinding (of outcome assessors or study analysts, may be for HL or costs) | Fulfilled if stated in the text | CEFF | ||
8 int | Outcome measurement for HL: described in sufficient detail? (out_HL-meas) | PREV | COST | CEFF | |
9 int | Outcome measurement for intermed/final: outcome described in sufficient detail? (out_cons) | COST | CEFF | ||
10 int | Costs measured correctly? (out_cost) | To be described: quantities of resource use; currency and price date; discounting | COST | CEFF | |
11 int | Outcome incremental analysis for costs and consequences? (out_cost) | CEFF | |||
12 ext | Perspective of economic evaluation stated? (CEFF_persp) | CEFF | |||
13 ext | Sensitivity analysis performed? (CEFF_sensit) | To address uncertainty of input variables | COST | CEFF | |
14 int | Analysis: adequate techniques used? | Measures of uncertainty for main results reported? (e.g. CI); accounted for confounding? (restriction; stratific.; multivar. models; ran) If econometric model used: time horizon stated? | PREV | COST | CEFF |
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License ( https://creativecommons.org/licenses/by-nc/2.0 ), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Eichler, K., Wieser, S. & Brügger, U. The costs of limited health literacy: a systematic review. Int J Public Health 54, 313–324 (2009). https://doi.org/10.1007/s00038-009-0058-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00038-009-0058-2