Abstract
Purpose
To evaluate the usefulness of intravenous patient-controlled analgesia (PCA) fentanyl for labour analgesia, its effectiveness for maternal pain and safety for the fetus and newborn.
Methods
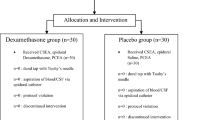
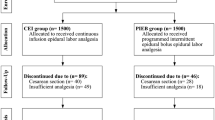
Twenty primigravidas were randomised to receive intravenous PCA fentanyl or epidural analgesia for labour pain. Maternal pain, heart rate and arterial oxyhaemoglobin saturation (SpO2) were monitored. Fetal and neonatal monitoring included cardiotocogram (CTG), APGAR, neurological scoring and static-charge-sensitive bed (SCSB) recording for 12 hr postnatally with ECG and SpO2. Fentanyl concentrations and pH of umbilical artery and vein were analysed.
Results
Initially, epidural analgesia was more effective (P = 0.01 ), and three patients in the fentanyl group were given epidural due to unsatisfactory pain relief. Overall satisfaction for analgesia did not differ between the groups. Maternal side-effects were more frequent in the fentanyl group (dizziness and tiredness most often,P = 0.0001). Severe side-effects were not reported. In CTG there were no differences between groups. All the newborns were healthy, APGAR and pH were normal. Naloxone was not used. Neurological scoring was similar in both groups. In 12 hr monitoring heart rate, breathing frequency and movement time were similar in both groups, but SpO2 was lower in the fentanyl group (P < 0.001 ). Umbilical cord fentanyl concentrations were low or beyond the detection limit.
Conclusion
Intravenous fentanyl can be used for labour analgesia with the doses reported here as an alternative to epidural analgesia. However, the fetus and neonate must be appropriately monitored. Naloxone and oxygen should be available if neonatal distress occurs.
Résumé
Objectif
Évaluer l’importance de l’analgésie intraveineuse auto-contrôlée (PCA) au fentanyl en analgésie obstétncale en tenant compte de son efficacité et de la sécurité foeto-maternelle.
Méthodes
Vingt pnmipares ont été assignées aléatoirement à recevoir soit du fentanyl intraveineux en PCA soit une analgésie épidurale dans le but de soulager la douleur de l’accouchement. La douleur maternelle, la fréquence cardiaque et la saturation arténelle (SpO2) ont été notées. Le monitorage foetal et néonatal incluait la cardiotocographie (CTG), le score d’APGAR, l’évaluation neurologique et l’enregistrement au lit sensible à la statique (SCSB) pendant 12 h après la naissance avec l’ÉCG ET la SpO2. La concentration de fentanyl et le pH de l’artère et de la veine ombilicales étaient mesurés.
Résultats
Initialement, l’analgésie épidurale s’est avérée plus efficace (P = 0,01 ) et trois patientes du groupe fentanyl ont dû accepter une analgésie épidurale à cause du manque de soulagement. La satisfaction globale en rapport avec l’analgésie n’a pas différé entre les groupes. Des effets maternels secondaires sans gravité sont survenus plus souvent dans le groupe fentanyl (surtout des étourdissements et de la fatigue,P = 0,0001 ). Le CTG n’a pas révélé de différences intergroupes. Tous les enfants sont nés en bon état avec des scores d’APGAR et des pH normaux. On n’a pas administré de naloxone. Lévaluation neurologique était identique dans les deux groupes. Après 12 h de monitorage de la fréquence cardiaque, la fréquence respiratoire et le temps de mouvement étaient identiques dans les deux groupes mais la SpO2 était plus basse dans le groupe fentanyl (P < 0,001 ). Les concentrations ombilicales de fentanyl étaient faibles ou impossible à déceler.
Conclusion
Pour l’analgésie de l’accouchement, on peut substituer le fentanyl intraveineux selon les doses utilisées à l’analgésie épidurale. Cependant, le foetus et le nouveau-né doivent être surveillés de près. Il faut avoir du naloxone ou de l’oxygène à portée de main pour traiter la détresse néonatale potentielle.
Article PDF
Similar content being viewed by others
References
Lieberman E, Lang JM, Frigoletto F Jr, Richardson DK, Ringer SA, Cohen A. Epidural analgesia, intrapartum fever, and neonatal sepsis evaluation. Pediatrics 1997; 99: 415–9.
Rawal N, Allvin R. Management of obstetric pain in Europe — a 17-nation survey. Congress Abstract. Annual Congress of European Society of Anesthesiologists, London, 1996.
Ranta P, Jouppila P, Spalding M, Kangas-Saarela T, Hollmén A, Jouppila R. Parturients’ assessment of water blocks, pethidine, nitrous oxide, paracervical and epidural blocks in labour. International Journal of Obstetric Anesthesia 1994; 3: 193–8.
Kariniemi V, Ämmälä P. Effects of intramuscular pethidine on fetal heart rate variability during labour. Br J Obstet Gynecol 1981; 88: 718–20.
Rosen MG, Scibetta JJ, Hochberg CJ. Human fetal electroencephalogram. III: pattern changes in presence of fetal heart rate alterations and after use of maternal medications. Obstet Gynecol 1970; 36: 132–40.
Boddy K, Dawes GS. Fetal breathing. Br Med Bull 1975; 31: 3–7.
Shnider SM, Moya F. Effects of meperidine on the newborn infant. Am J Obstet Gynecol 1964; 89: 1009–15.
Taylor ES, von Fumetti HH, Essig LL, Goodman SN, Walker LC. The effects of demerol and trichloroethylene on arterial oxygen saturation in the newborn. Am J Obstet Gynecol 1955; 69: 348–51.
Roberts H, Kane KM, Percival N, Snow P, Please NW. Effects of some analgesic drugs used in childbirth with special reference to variation in respiratory minute volume of the newborn. Lancet 1957; 1: 128.
Koch G, Wandel H. The effect of pethidine on the postnatal adjustment of respiration and acid base balance. Acta Obstet Gynecol Scand 1968; 47: 27–37.
Burnard ED, Cross KW. Rectal temperature in the newborn after birth asphyxia. BMJ 1958; 2: 1197–9.
Brackbill Y, Kane J, Manniello RL, Abramson D. Obstetric meperidine usage and assessment of neonatal status. Anesthesiology 1974; 40: 116–20.
Olofsson Ch, Ekblom A, Ekman-Ordeberg G, Hjelm A, Irestedt L. Lack of analgesic effect of systemicaliy administered morphine or pethidine on labour pain. Br J Obstet Gynecol 1996; 103: 968–72.
McClain DA, Hug CC Jr. Intravenous fentanyl kinetics. Clin Pharmacol Ther 1980; 28: 106–14.
Kuhnert BR, Linn PL, Kuhnert PM. Obstetric medication and neonatal behavior. Current controversies. Clin Perinatol 1985; 12: 423–40.
Koehntop DE, Rodman JH, Brundage DM, Hegland MG, Buckley JJ. Pharmacokinetics of fentanyl in neonates. Anesth Analg 1986; 65: 227–32.
Yaster M. The dose response of fentanyl in neonatal anesthesia. Anesthesiology 1987; 66: 433–5.
Jarvis AP, Arancibia CU. A case of difficult neonatal ventilation (Letter). Anesth Analg 1987; 66: 196.
Craft JB Jr, Coaldrake LA, Bolan JC, et al. Placental passage and uterine effects of fentanyl. Anesth Analg 1983; 62: 894–8.
Rayburn W, Rathke A, Leuschen MP, Chleborad J, Weidner W. Fentanyl citrate analgesia during labor. Am J Obstet Gynecol 1989; 161: 202–6.
Rayburn WF, Smith CV, Parriot JE, Woods RE. Randomized comparison of meperidine and fentanyl during labor. Obstet Gynecol 1989; 74: 604–6.
Kleiman SJ, Wiesel S, Tessler MJ. Patient-controlled analgesia (PCA) using fentanyl in a parturient with a platelet function abnormality. Can J Anaesth 1991; 38: 489–91.
Rosaeg OP, Kitts JB, Koren G, Byford LJ. Maternal and fetal effects of intravenous patientcontrolled fentanyl analgesia during labour in a thrombocytopenic parturient. Can J Anaesth 1992; 39: 277–81.
Graves DA, Foster TS, Batenhorst RL, Bennett RL, Baumann TJ. Patient-controlled analgesia. Ann Intern Med 1983; 99: 360–6.
Kanto J, Erkkola R, Mansikka M, Äärimaa L. Segmental epidural analgesia — a modern method for safe and effective management of labor pains. Biological Research Pregnancy 1983; 4: 172–6.
Dawes GS, Moulden M, Redman CWG. System 8000: computerized antenatal FHR analysis. J Perinat Med 1991; 19: 47–51.
Amiel-Tison C, Barrier G, Shnider SM, Levinson G, Hughes SC, Stefani SJ. A new neurologic and adaptive capacity scoring system for evaluating obstetric medications in full-term newborns. Anesthesiology 1982; 56: 340–50.
Alihanka J, Vaahtoranta K, Saarikivi J. A new method of long-term monitoring of the ballistocardiogram, heart rate, and respiration. Am J Physiol 1981; 240: 384–92.
Alihanka J. Basic principles for analysing and scoring Bio-matt (SCSB) recordings. Annales Universitatis Turkuensis 1987; 26: 1–129.
Katz R, Kelly HW. Pharmacokinetics of continuous infusions of fentanyl in critically ill children. Crit Care Med 1993; 21: 995–1000.
Erkinjuntti M, Vaahtoranta K, Alihanka J, Kero P. Use of the SCSB method for monitoring of respiration, body movements and ballistocardiogram in infants. Early Hum Dev 1984: 9: 119–26.
Erkinjuntti M, Kero P, Halonen J-P, Mikola H, Sainio K. SCSB method compared to EEG-based polygraphy in sleep state scoring of newborn infants. Acta Paediatr Scand 1990; 79: 274–9.
Kirjavainen T, Cooper D, Polo O, Sullivan CE. Respiratory and body movements as indicators of sleep stage and wakefulness in infants and young children. J Sleep Res 1996; 5: 186–94.
Kirjavainen T, Cooper D, Polo O, Sullivan CE. The static-charge-sensitive bed in the monitoring of respiration during sleep in infants and young children. Acta Paediatr 1996; 85: 1146–52.
Seppälä M, Alihanka J, Himberg J-J, Kanto J, Rajala T, Sourander L. Midazolam and flunitrazepam: pharmacokinetics and effects on night time respiration and body movements in the elderly. Int J Clin Pharmacol Ther Toxicol 1993; 31: 170–6.
Dinges DF, Davis MM, Glass P. Fetal exposure to narcotics: neonatal sleep as a measure of nervous system disturbance. Science 1980; 209: 619–21.
Pinto F, Torrioli MG, Casella G, Tempesta E, Funda`o C. Sleep in babies born to chronically heroin addicted mothers. A follow up study. Drug Alcohol Depend 1988; 21: 43–7.
Anand KJS, Hickey PR. Pain and its effects in the human neonate and fetus. N Engl J Med 1987; 21: 1321–9.
de Lima J, Lloyd-Thomas AR, Howard RF, Sumner E, Quinn TM. Infant and neonatal pain: anaesthetists’ perceptions and prescribing patterns. BMJ 1996; 313: 787.
Emde RN, Harmon RJ, Metcalf D, Kornig KL, Wagonfeld S. Stress and neonatal sleep. Psychosom Med 1971; 33: 491–7.
Freudigman KA, Thoman EB. Infant sleep during the first postnatal day: an opportunity for assessment of vulnerability. Pediatrics 1993; 92: 373–9.
Anand KJS, Sippell WG, Aynsley-Green A. Randomised trial of fentanyl anaesthesia in preterm babies undergoing surgery: effects on the stress response. Lancet 1987; 1: 243–8.
Author information
Authors and Affiliations
Additional information
Supported by funds from Instrumentarium Research Foundation, Finland and funds from Turku University Hospital, Finland.
Rights and permissions
About this article
Cite this article
Nikkola, E.M., Ekblad, U.U., Kero, P.O. et al. Intravenous fentanyl PCA during labour. Can J Anaesth 44, 1248–1255 (1997). https://doi.org/10.1007/BF03012771
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03012771