Abstract
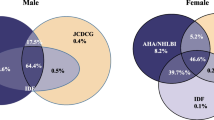
Objective: To assess the prevalence of the metabolic syndrome (MS) and relative associations with vascular disease in an older Chinese population using the US National Cholesterol Education Program: Adult Treatment Panel (NCEP: ATP III) and International Diabetes Federation (IDF) definitions. Design: Cross-sectional study. Subjects: A total of 3035 men and 7291 women aged 50 to 85 yr recruited from Guangzhou, China. Measurements: All participants received a full medical check-up including measurement of blood pressure, obesity indices, fasting total, LDL-, HDL-cholesterol, triglycerides (TG) and glucose levels. Demographic information and self-reported history of physician-diagnosed coronary heart disease (CHD), stroke and myocardial infarction (MI) were collected through standardized interview. Results: The estimates under the two definitions differed substantially, with the age standardized prevalence of MS 15.57% using the NCEP: ATP III definition and 25.81% using the IDF definition. Among all participants, 80.23% were similarly classified using both definitions. The association between self-reported CHD, stroke and MI and the MS defined by the IDF definition was stronger than that by the NCEP: ATP III. Conclusions: The IDF compared to the ATP III definition shows a stronger association with the MS and associated vascular disease in Chinese. The prevalence of the MS is alarmingly high in this older Chinese population. Comprehensive strategies are needed for prevention and treatment of the MS to reduce the increased societal burden of cardiovascular disease in China.
Similar content being viewed by others
References
Isomaa B, Almgren P, Tuomi T, et al. Cardiovascular morbidity and mortality associated with the metabolic syndrome. Diabetes Care 2001, 24: 683–9.
Trevisan M, Liu J, Bahsas FB, Menotti A. Syndrome X and mortality: a population-based study. Risk Factor and Life Expectancy Research Group. Am J Epidemiol 1998, 148: 958–66.
Wilson PW, Kannel WB, Silbershatz H, D’Agostino RB. Clustering of metabolic factors and coronary heart disease. Arch Intern Med 1999, 159: 1104–9.
Roberts WC. The metabolic syndrome. Am J Cardiol 2004, 93: 274.
Thomas GN, Ho SY, Janus ED, et al. The US National Cholesterol Education Programme Adult Treatment Panel III (NCEP ATP III) prevalence of the metabolic syndrome in a Chinese population. Diabetes Res Clin Pract 2005, 67: 251–7.
Gu D, Reynolds K, Wu X, et al. Prevalence of the metabolic syndrome and overweight among adults in China. Lancet 2005, 365: 1398–405.
Li ZY, Xu GB, Xia TA. Prevalence rate of metabolic syndrome and dyslipidemia in a large professional population in Beijing. Atherosclerosis 2006, 184: 188–92.
Executive Summary of The Third Report of The National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, And Treatment of High Blood Cholesterol In Adults (Adult Treatment Panel III). JAMA 2001, 285: 2486–97.
Alberti KG, Zimmet P, Shaw J. The metabolic syndrome—a new worldwide definition. Lancet 2005, 366: 1059–62.
Ang LW, Ma S, Cutter J, et al. The metabolic syndrome in Chinese, Malays and Asian Indians. Factor analysis of data from the 1998 Singapore National Health Survey. Diabetes Res Clin Pract 2005, 67: 53–62.
Heng D, Ma S, Lee JJ, et al. Modification of the NCEP ATP III definitions of the metabolic syndrome for use in Asians identifies individuals at risk of ischemic heart disease. Atherosclerosis 2005.
Tan CE, Ma S, Wai D, Chew SK, Tai ES. Can we apply the National Cholesterol Education Program Adult Treatment Panel definition of the metabolic syndrome to Asians? Diabetes Care 2004, 27: 1182–6.
Lee ZS, Critchley JA, Ko GT, et al. Obesity and cardiovascular risk factors in Hong Kong Chinese. Obes Rev 2002, 3: 173–82.
Thomas GN, Ho SY, Lam KS, et al. Impact of obesity and body fat distribution on cardiovascular risk factors in Hong Kong Chinese. Obes Res 2004, 12: 1805–13.
Deurenberg-Yap M, Chew SK, Deurenberg P. Elevated body fat percentage and cardiovascular risks at low body mass index levels among Singaporean Chinese, Malays and Indians. Obes Rev 2002, 3: 209–15.
Li G, Chen X, Jang Y, et al. Obesity, coronary heart disease risk factors and diabetes in Chinese: an approach to the criteria of obesity in the Chinese population. Obes Rev 2002, 3: 167–72.
He M, Tan KC, Li ET, Kung AW. Body fat determination by dual energy X-ray absorptiometry and its relation to body mass index and waist circumference in Hong Kong Chinese. Int J Obes Relat Metab Disord 2001, 25: 748–52.
International Diabetes Federation. The IDF consensus worldwide definition of the metabolic syndrome. April 14, 2005: http://www.idf.org (accessed September, 2005).
Population Census Office of Guang Dong Province. Tabulation on the 2000 Population census of Guang Dong province. Beijing. China Statistics Press. 2002, 156–65.
Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics 1977, 33: 159–74.
Ministry of Health People’s Republic of China. Summary of the 2005 health annals. http://www.moh.gov.cn/ (accessed October, 2005).
Deurenberg P, Yap M, van Staveren WA. Body mass index and percent body fat: a meta analysis among different ethnic groups. Int J Obes Relat Metab Disord 1998, 22: 1164–71.
Chang CJ, Wu CH, Chang CS, et al. Low body mass index but high percent body fat in Taiwanese subjects: implications of obesity cutoffs. Int J Obes Relat Metab Disord 2003, 27: 253–9.
Pan WH, Flegal KM, Chang HY, et al. Body mass index and obesity-related metabolic disorders in Taiwanese and US whites and blacks: implications for definitions of overweight and obesity for Asians. Am J Clin Nutr 2004, 79: 31–9.
Little RJA, Rubin DB. Statistical analysis with missing data. New York: John Wiley and Sons. 1986.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lao, X.Q., Thomas, G.N., Jiang, C.Q. et al. Association of the metabolic syndrome with vascular disease in an older Chinese population: Guangzhou Biobank Cohort Study. J Endocrinol Invest 29, 989–996 (2006). https://doi.org/10.1007/BF03349212
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03349212