Abstract
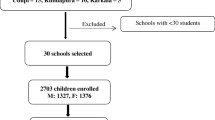
Background: One decade after universal salt iodization in Iran, goiter prevalence, urinary iodine concentration (UIC) and thyroperoxidase antibody (TPOAb) values were assessed among schoolchildren in Gorgan, Iran. Methods: From 2003–2004, 500 girls and 900 boys aged 7–11 yr were evaluated for goiter by palpation. UIC was measured in 183 randomly-selected goitrous children. Serum TSH, T4, and TPOAb were measured in 53 goitrous and 30 non-goitrous children with adequate UIC. Results: Goiter was detected in 370 (26.4%) children. Goiter was present in 31 % of girls and 17% of boys age 9 (p<0.012); 37% of girls and 20% of boys age 10 (p<0.003); and 52% of girls and 19% of boys age 11 (p<0.0001). Median (range) UIC for all goitrous children sampled was 190 (20–600) μg/I; 220 (30–590) in boys and 170 (20–600) in girls (p=0.001). Eight point seven percent of goitrous children and 22% of goitrous girls aged 10–11 had UIC<100 μg/I, while 47% of the goitrous children had UIC≥200 μg/ I. TPOAb was present in 52.8% of goitrous children and 10% of non-goitrous children (p=0.0001 ). TPOAb was present in 53.9% of 10–11 and 22.7% of 7–9 yr old goitrous and non-goitrous children (p=0.003) with adequate UIC. Median (range) TSH was 2.9 (0.3–10.9) mIU/I in TPO-positive and 1.8 (0.5–4.1) in TPO-negative children (p=0.001). Conclusions: Gorgan, Iran, is an iodine-sufficient area and almost half of schoolchildren have more than adequate UIC. TPOAb is associated with endemic goiter. Despite sufficient UIC overall, some school-aged girls remain at risk of iodine deficiency.
Similar content being viewed by others
References
Hetzel BS. Iodine deficiency disorders (IDD) and their eradication. Lancet 1983, 2: 1126–9.
Delange F. Iodine deficiency as a cause of brain damage. Postgrad Med J 2001, 77: 217–20.
Hetzel BS. Eliminating iodine deficiency disorders-the role of the International Council in the global partnership. Bull World Health Organ 2002, 80: 410–3.
WHO, UNICEF, and ICCIDD. Progress towards the elimination of iodine deficiency disorders (IDD). Geneva: WHO publ. WHO/NHD/99.4.1999,1-33.
Connolly RJ, Vidor G I, Stewart JC. Increase in thyrotoxicosis in endemic goitre area after iodation of bread. Lancet 1970, 1: 500–2.
Todd CH, Allain T, Gomo ZA, Hasler JA, Ndiweni M, Oken E. Increase in thyrotoxicosis associated with iodine supplements in Zimbabwe. Lancet 1995, 346: 1563–4.
Bourdoux PP, Ermans AM, Mukalay wa mukalay A, Filetti S, Vigneri R. Iodine-induced thyrotoxicosis in Kivu, Zaire. Lancet 1996, 347: 552–3.
Harach HR, Escalante DA, Day ES. Thyroid cancer and thyroiditis in Salta, Argentina: a 40-yr study in relation to iodine prophylaxis. Endocr Pathol 2002, 13: 175–81.
Braverman LE. Adequate iodine intake — the good far outweighs the bad. Eur J Endocrinol 1998, 139: 14–5.
Delange F. Risks and benefits of iodine supplementation. Lancet 1998, 351: 923–4.
Emami A, Shahbazi H, Sabzevari M, et al. Goiter in Iran. Am J Clin Nutr 1969, 22: 1584–8.
Azizi F, Sheikholeslam R, Hedayati M, et al. Sustainable control of iodine deficiency in Iran: beneficial results of the implementation of the mandatory law on salt iodization. J Endocrinol Invest 2002, 25: 409–13.
Regional meeting for the promotion of iodized salt in the Eastern Mediterranean, Middle East and North African Region, Dubai, United Arab Emirates, 10–21 April 2000.
Heydarian P, Azizi F. Thyroid dysfunction and autoantibodies 10 years after implementation of universal salt iodization: Tehran Thyroid Study. Iran J Endocrinol Metab 2003, 4: 229–41 [in Persian].
WHO/UNICEF/ICCIDD. Assessment of the iodine deficiency disorders and monitoring their elimination. A guide for programme managers, 2nd ed. Geneva: WHO publ. WHO/NHD/01.1; 2001,1-107.
Dunn JT, Crutchfield HE, Gutekunst R, Dunn AD. Methods for measuring iodine in urine. Wagenigen, The Netherlands: ICCIDD; 1993, 1–71.
Follis RH Jr. Patterns of urinary iodine excretion in goitrous and nongoitrous areas. Am J Clin Nutr 1964, 14: 253–68.
Sandell EB, Kolthoff IM. Micro-determination of iodine by a catalytic method. Mikrochemica Acta 1937, 1: 9–25.
Delange F, Hetzel B.The iodine deficiency disorders. In: De-Groot L, Hennemann G eds. Thyroid Disease Manager. http://www.thyroidmanager.org. Revision 16 September 2004.
Delange F. Iodine deficiency. In: Braverman LE, Utiger RD eds. Werner and Ingbar’s The Thyroid: A fundamental and clinical text. 8th ed. Philadelphia: Lippincott Williams and Wilkins. 2000, 295–316.
Fisher DA. Physiological variations in thyroid hormones: physiological and pathophysiological considerations. Clin Chem 1996, 42: 135–9.
Needlman RD. Growth and development. In: Behrman RE, Kliegman RM, Jenson HB eds. Nelson Textbook of Pediatrics. 17th ed. Philadelphia: Saunders 2004, 23–66.
Hollowell JG, Hannon WH. Teratogen update: iodine deficiency, a community teratogen. Teratology 1997, 55: 389–405.
Fenzi GF, Giani C, Ceccarelli P, et al. Role of autoimmune and familial factors in goiter prevalence: Studies performed in a moderately endemic area. J Endocrinol Invest 1986, 9: 161–4.
Svinaryov M, Aranovich V. Iodine deficiency disorders in the Saratov province in Russia. J Endocrinol Invest 2003, 26: 16–9.
Delange F, de Benoist B, Burgi H, ICCIDD Working Group. International Council for Control of Iodine Deficiency Disorders. Determining median urinary iodine concentration that indicates adequate iodine intake at population level. Bull World Health Organ 2002, 80: 633–6.
Marwaha RK, Tandon N, Gupta N, Karak AK, Verma K, Kochupillai N. Residual goitre in the postiodization phase: iodine status, thiocyanate exposure and autoimmunity. Clin Endocrinol (Oxf) 2003, 59: 672–81.
Peterson S, Sanga A, Eklof H, et al. Classification of thyroid size by palpation and ultrasonography in field surveys. Lancet 2000, 355: 106–10.
Perez C, Scrimshaw S, Munoz A. Technique of endemic goiter surveys. In: Endemic goiter. Geneva: WHO 1960, 369–83.
DeMayer EM, Lowenstein FW, Thilly CH. The control of endemic goitre. Geneva: WHO 1979.
Vitti P, Martino E, Aghini-Lombardi F, et al. Thyroid volume measurement by ultrasound in children as a tool for the assessment of mild iodine deficiency. J Clin Endocrinol Metab 1994, 79: 600–3.
WHO/UNICEF/ICCIDD. Indicators for assessing iodine deficiency disorders and their control through salt iodization. WHO/NUT/94.6.Geneva: WHO 1994.
WHO/ICCIDD. Recommended normative values for thyroid volume in children aged 6–15 years. Bull WHO 1997, 75: 95–7.
Delange F. Iodine deficiency in Europe anno 2002. Thyroid International 2002, 5: 1–20.
Wiersinga WM, Podoba J, Srbecky M, van Vessem M, van Beeren HC, Platvoet-Ter Schiphorst MC. A survey of iodine intake and thyroid volume in Dutch schoolchildren: reference values in an iodine-sufficient area and the effect of puberty. EurJ Endocrinol 2001, 144: 595–603.
Als C, Keller A, Minder C, Haldimann M, Gerber H. Ageand gender-dependent urinary iodine concentrations in an area-covering population sample from the Bernese region in Switzerland. Eur J Endocrinol 2000, 143: 629–37.
Fleury Y, Van Melle G, Woringer V, Gaillard RC, Portmann L. Sex-dependent variations and timing of thyroid growth during puberty. J Clin Endocrinol Metab 2001, 86: 750–4.
Clark PA, Rogol AD. Growth hormones and sex steroids interactions in puberty. Endocrinol Metab Clin North Am 1996, 25: 665–81.
Kreipe RE, Kodjo CM. Adolescent medicine. In: Behrman RE, Kliegman RM, eds. Nelson Essentials of Pediatrics, 4th ed. Philadelphia: W.B. Saunders Company 2002, 251–95.
Dunn JT. Iodine should be routinely added to complementary foods. J Nutr 2003, 133: 3008–10S.
Als C, Helbling A, Peter K, Haldimann M, Zimmerli B, Gerber H. Urinary iodine concentration follows a circadian rhythm: a study with 3023 spot urine samples in adults and children. J Clin Endocrinol Metab 2000, 85: 1367–9.
Weetman AP. Is endemic goiter an autoimmune disease? J Clin Endocrinol Metab 1994, 78: 1017–9.
Roth C, Scortea M, Stubbe P, et al. Autoimmune thyreoiditis in childhood—epidemiology, clinical and laboratory findings in 61 patients. Exp Clin Endocrinol Diabetes 1997, 105(Suppl 4): 66–9.
Markou KB, Georgopoulos NA, Makri M, et al. Improvement of iodine deficiency after iodine supplementation in schoolchildren of Azerbaijan was accompanied by hypo and hyperthyrotropinemia and increased titre of thyroid autoantibodies. J Endocrinol Invest 2003; 26: 43–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bazrafshan, H.R., Mohammadian, S., Ordookhani, A. et al. Prevalence of goiter among schoolchildren from Gorgan, Iran, a decade after national iodine supplementation: Association with age, gender, and thyroperoxidase antibodies. J Endocrinol Invest 28, 727–733 (2005). https://doi.org/10.1007/BF03347556
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03347556