Abstract
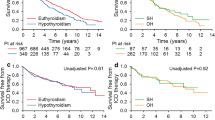
Background: Amiodarone protects patients with left ventricular systolic dysfunction (LVSD) against serious arrhythmias, but it also has numerous side effects on non-cardiac organs, such as the thyroid. Indeed, amiodarone may inhibit the peripheral conversion of T4 into T3. Pathologically reduced serum levels of T3 — the so-called “low T3 syndrome” (LOWT3) — increase mortality in patients with LVSD and not on amiodarone. Aim: The aim of the study was to examine the relationship between thyroid hormone status, amiodarone therapy, and outcome in a population with LVSD. Material/subjects and methods: A total of 2344 patients with LVSD and free of overt hyper- and hypothyroidism were enrolled. The population was divided into 4 groups: group 1 (LOWT3 and amiodarone therapy, no.=126), group 2 (isolated amiodarone therapy, no.=74), group 3 (isolated LOWT3, no.=682), group 4 (controls, no.=1462). Results: Kaplan-Meier curves showed, after a mean follow-up of 31 months, increased total and cardiac mortality in groups 1 (30% and 20%, respectively), 2 (23%, 11%), and 3 (22%, 12%) compared to group 4 (total mortality log-rank 82.8, pa<0.0001; cardiac mortality log-rank 63.1, p<0.0001). At Cox analysis, adjusted for several clinical variables, survival was reduced in groups 1 and 3 compared to group 4. Group 2 had a similar mortality to group 4, although the number of patients was too limited to accurately assess the effect of amiodarone on long-term prognosis. Conclusions: LOWT3 exerts an adverse impact on prognosis in LVSD, which is not influenced by concomitant amiodarone therapy.
Similar content being viewed by others
References
Klein I, Ojamaa K. Thyroid hormone and the cardiovascular system. N Engl J Med 2001, 344: 501–9.
Ochs N, Auer R, Bauer DC, et al. Meta-analysis: subclinical thyroid dysfunction and the risk for coronary heart disease and mortality. Ann Intern Med 2008, 148: 832–45.
Rodondi N, Bauer DC, Cappola AR, et al. Subclinical thyroid dysfunction, cardiac function, and the risk of heart failure. The Cardiovascular Health study. J Am Coll Cardiol 2008, 52: 1152–9.
Pingitore A, Landi P, Taddei MC, Ripoli A, L’Abbate A, Iervasi G. Triiodothyronine levels for risk stratification of patients with chronic heart failure. Am J Med 2005, 118: 132–6.
Dickstein K, Cohen-Solal A, Filippatos G, et al. ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2008: the Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2008 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association of the ESC (HFA) and endorsed by the European Society of Intensive Care Medicine (ESICM). Eur Heart J 2008, 29: 2388–442.
Coceani M, Mariotti R. Is amiodarone safe in heart failure? BMJ 2006, 332: 317–8.
Bardy GH, Lee KL, Mark DB, et al; Sudden Cardiac Death in Heart Failure Trial (SCD-HeFT) Investigators. Amiodarone or an implantable cardioverter-defibrillator for congestive heart failure. N Engl J Med 2005, 352: 225–37.
Lechat P, Hulot JS, Escolano S, et al. Heart rate and cardiac rhythm relationships with bisoprolol benefit in chronic heart failure in CIBIS II Trial. Circulation 2001, 103: 1428–33.
Torp-Pedersen C, Metra M, Spark P, et al; COMET Investigators. The safety of amiodarone in patients with heart failure. J Card Fail 2007, 13: 340–5.
Thomas KL, Al-Khatib SM, Lokhnygina Y, et al. Amiodarone use after acute myocardial infarction complicated by heart failure and/or left ventricular dysfunction may be associated with excess mortality. Am Heart J 2008, 155: 87–93.
Connolly SJ. Evidence-based analysis of amiodarone efficacy and safety. Circulation 1999, 100: 2025–34.
Auricchio A, Nisam S, Klein HU. Perspectives: does amiodarone increase non-sudden deaths? If so, why? J Interv Card Electrophysiol 2000, 4: 569–74.
Lang RM, Bierig M, Devereux RB, et al; Chamber Quantification Writing Group; American Society of Echocardiography’s Guidelines and Standards Committee; European Association of Echocardiography. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr 2005, 18: 1440–63.
Utiger RD. Altered thyroid function in nonthyroidal illness and surgery. To treat or not to treat? N Engl J Med 1995, 333: 1562–3.
Iervasi G, Pingitore A, Landi P, et al. Low-T3 syndrome: a strong prognostic predictor of death in patients with heart disease. Circulation 2003, 107: 708–13.
Danzi S, Klein I. Alterations in thyroid hormones that accompany cardiovascular disease. Clinical Thyroidology 2009, 21: 3–5.
Køber L, Torp-Pedersen C, McMurray JJ, et al; Dronedarone Study Group. Increased mortality after dronedarone therapy for severe heart failure. N Engl J Med 2008, 358: 2678–87.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Coceani, M., Molinaro, S., Scalese, M. et al. Thyroid hormone, amiodarone therapy, and prognosis in left ventricular systolic dysfunction. J Endocrinol Invest 34, e144–e148 (2011). https://doi.org/10.1007/BF03346723
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03346723