Abstract
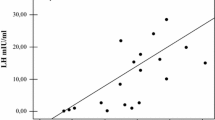
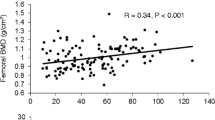
After prolonged treatment (76.4±10 and 70.1±12.3 months, respectively) (mean± SE) with testosterone enanthate (250 mg im every 3 weeks), bone mineral density (BMD) and bone metabolism were evaluated in 12 patients (aged 29.3±1.4 yr) affected by idiopathic hypogonadotropic hypogonadism (IHH), in 8 patients (29.6±2.6 yr) affected by Klinefelter’s syndrome (KS), and in 10 healthy men (30.6±1.7 yr) matched according to age and BMI. Spinal BMD in IHH was significantly lower than in controls (0.804±0.04 vs 1.080±0.01 g/cm2; p<0.001), while there was no difference in neck BMD (0.850±0.01 vs 0.948±0.02 g/cm2). Neither spinal (0.978±0.05 g/cm2) nor neck (0.892±0.03 g/cm2) BMD in KS were significantly different from controls. Six IHH and one KS subjects were osteoporotic, while 6 IHH and 2 KS subjects were osteopenic. A significant inverse correlation was found between spinal BMD and age at the treatment onset in IHH (r=−0.726, p=0.007). In IHH there were significant increases in bone formation (alkaline phosphatase=318.3±33.9 vs 205.4±20.0 IU/l; osteocalcin=13.44±1.44 vs 8.57±0.94 ng/ml; p<0.05) and in bone resorption (urinary cross-linked N-telopeptides of type I collagen= 149.1± 32.3 vs 47.07±8.4 nmol bone collagen equivalents/mmol creatinine; p<0.05) compared to controls, while such differences were not present in KS. Our results outline the importance of BMD evaluation in all hypogonadal males. Nevertheless, bone loss is a minor characteristic of KS, while it is a distinctive feature of IHH. Therefore, early diagnosis and age-related replacement therapy coupled with a specific treatment for osteoporosis could be useful in preventing future severe bone loss and associated skeletal morbidity.
Similar content being viewed by others
References
Seeman E., Melton L.J., O’Fallon W.M., Riggs B.L. Risk factors for spinal osteoporosis in men. Am. J. Med. 1983, 75: 977–983.
Jackson J.A., Kleerekoper M. Osteoporosis in men: diagnosis, pathophysiology, and prevention. Medicine 1990, 69: 137–152.
Colvard D.S., Erikson E.F., Keeting P.E., Wilson E.M., Lubahn D.B., French F.S., Riggs B.L., Spelsberg T.C. Identification of androgen receptors in normal human osteoblast-like cells. Proc. Natl. Acad. Sci. USA 1989, 86: 854–857.
Orwoll E.S., Stribrska L., Ramsey E.E., Keenan E.J. Androgen receptors in osteoblast-like cell lines. Calcif. Tissue Int. 1991, 49: 183–187.
Kasperk C.H., Wergedal J.E., Farkey J.R., Linkhart T.A., Turner R.T., Baylink D.J. Androgens directly stimulate proliferation of bone cells in vitro. Endocrinology 1989, 124: 1576–1578.
Baran D.T., Bergfeld M.A., Teitelbaum S.L., Avioli L.V. Effect of testosterone therapy on bone formation in an osteoporotic hypogonadal male. Calcif. Tissue Res. 1978, 26: 103–106.
Crilly R.G., Francis R.M., Nordin B.E.C. Steroid hormones, ageing and bone. J. Clin. Endocrinol. Metab. 1989, 10: 115–139.
Smith E.P., Boyd J., Frank G.R., Takahashi H., Cohen R.M., Specker B., Williams T.C., Lubahn D.B., Korach K.S. Estrogen resistance caused by a mutation in the estrogen- receptor gene in a man. N. Engl. J. Med. 1994, 331: 1056–1061.
Horowitz M., Wishart J.M., O’Loughlin P.D., Morris H.A., Need A.G., Nordin B.E.C. Osteoporosis and Klinefelter’s syndrome. Clin. Endocrinol. (Oxf.) 1992, 36: 113–118.
Favus M.J. Bone density reference data. In: Favus M.J. (Ed.), Primer on the metabolic bone diseases and disorders of mineral metabolism, ed 2. Raven Press, New York, 1993, p. 426.
Finkelstein J.S., Klibanski A., Neer R.M., Greenspan S.L., Rosenthal D.I., Crowley W.F. Osteoporosis in men with idiopathic hypogonadotropic hypogonadism. Ann. Intern. Med. 1987, 106: 354–361.
Canale D., Vignali E., Golia F., Martino E., Pinchera A., Marcocci C. Effects of hormonal replacement treatment on bone mineral density and metabolism in hypogonadal patients. Mol. Cell. Endocrinol. 2000, 161: 47–51.
Guo C.Y., Jones T.H., Eastell R. Treatment of isolated hypogonadotropic hypogonadism effect on bone mineral density and bone turnover. J. Clin. Endocrinol. Metab. 1997, 82: 658–665.
Wong H.W., Pun K.K., Wang C. Loss of bone mass in patients with Klinefelter’s syndrome despite sufficient testosterone replacement. Osteoporos. Int. 1993, 3: 3–7.
Cantrill J.A., Denis P., Large D.M., Neuman M., Anderson D.C. Which testosterone replacement therapy. Clin. Endocrinol. (Oxf.) 1984, 21: 97–107.
Behre H.M., Kliesch S., Leifke E., Link T.M., Nieschlag E. Long-term effect of testosterone therapy on bone mineral density in hypogonadal men. J. Clin. Endocrinol. Metab. 1997, 82: 2386–2390.
Katznelson L., Finkelstein J.S., Schoenfeld D.A., Rosenthal D.I., Anderson E.J., Klibanski A. Increase in bone density and lean body mass during testosterone administration in men with acquired hypogonadism. J. Clin. Endocrinol. Metab. 1996, 81: 4358–4365.
Scane A.C., Francis R.M. Risk factors for osteoporosis in men. Clin. Endocrinol. (Oxf.) 1993, 38: 15–16.
Finkelstein J.S., Klibanski A., Neer R.M., Doppelt S.H., Rosenthal D.I., Segre G.V., Crowley W.F. Increases in bone density during treatment of men with idiopathic hypogonadotropic hypogonadism. J. Clin. Endocrinol. Metab. 1989, 69: 776–783.
Finkelstein J.S., Klibanski A., Neer R.M. A longitudinal evaluation of bone mineral density in adult men with histories of delayed puberty. J. Clin. Endocrinol. Metab. 1996, 81: 1152–1155.
Bardin C.W., Swerdloff R.S., Santen R.J. Androgens: risks and benefits. J. Clin. Endocrinol. Metab. 1991, 73: 4–7.
Luisetto G., Mastrogiacomo I., Bonanni G., Pozzan G., Botteon S., Tizian L., Galuppo P. Bone mass and mineral metabolism in Klinefelter’s syndrome. Osteoporos. Int. 1995, 5: 455–461.
Foresta C., Ruzza G., Mioni R., Meneghello A., Baccichetti C. Testosterone and bone loss in Klinefelter’s syndrome. Horm. Metab. Res. 1983, 15: 56–57.
Choi H.R., Lim S.K., Lee M.S. Site-specific effect of testosterone on bone mineral density in male hypogonadism. J. Korean Med. Sci. 1995, 10: 431–435.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
De Rosa, M., Paesano, L., Nuzzo, V. et al. Bone mineral density and bone markers in hypogonadotropic and hypergonadotropic hypogonadal men after prolonged testosterone treatment. J Endocrinol Invest 24, 246–252 (2001). https://doi.org/10.1007/BF03343854
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03343854