Abstract
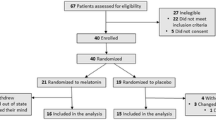
Background and aims: The aim of the study was to evaluate the effect of melatonin administration on sleep and behavioral disorders in the elderly and the facilitation of the discontinuation of regular hypnotic drugs. Methods: This was a prospective, randomized, double-blind, placebo-controlled, crossover trial in a community-living population. Participants were 22 older adults (7 men, 15 women over 65) with a history of sleep disorder complaints. Fourteen of these subjects were receiving hypnotic drug therapy. Participants received 2 months of melatonin (5 mg/day) and 2 months of placebo. Sleep disorders were evaluated with the Northside Hospital Sleep Medicine Institute (NHSMI) test, discarding secondary insomnia and evaluating sleep quality. Behavioral disorders were evaluated with the Yesavage Geriatric Depression Scale (GDS) and Goldberg Anxiety Scale (GAS). Patients discontinuing hypnotic drugs were also recorded. Results: Melatonin treatment for two months significantly improved sleep quality scores measured by the NHSMI test (1.78± 0.40) when compared with both basal (3.72± 0.45; p=0.001) and placebo (3.44± 0.56; p=0.025) groups. Depression measured by GDS and anxiety measured by GAS also improved significantly after melatonin administration (p=0.043 and p=0.009, respectively). Nine out of 14 subjects receiving hypnotic drugs were able to discontinue this treatment during melatonin but not placebo administration; one discontinued hypnotic drugs during both melatonin and placebo administration, and four were unable to discontinue hypnotic therapy. Conclusions: The results of this study suggest that melatonin administration significantly improves sleep and behavioral disorders in the elderly and facilitates discontinuation of therapy with conventional hypnotic drugs.
Similar content being viewed by others
References
Ancoli-Israel S, Cooke JR. Prevalence and comorbidity of insomnia and effect on functioning in elderly populations. J Am Geriatr Soc 2005; 53: S264–71.
Buysse DJ. Insomnia, depression and aging. Assessing sleep and mood interactions in older adults. Geriatrics 2004; 59: 47–51.
Taylor DJ, Lichstein KL, Durrence HH et al. Epidemiology of insomnia, depression, and anxiety. Sleep 2005; 28: 1457–64.
Ried LD, Johnson RE, Gettman DA. Benzodiazepine exposure and functional status in older people. J Am Geriatr Soc 1998; 46: 71–6.
Rajput V, Bromley SM. Chronic insomnia: a practical review. Am Fam Physician 1999; 60: 1431–8.
McCall WV. Diagnosis and management of insomnia in older people. J Am Geriatr Soc 2005; 53: S272–7.
Yoon IY, Kripke DF, Elliott JA et al. Age-related changes of circadian rhythms and sleep-wake cycles. J Am Geriatr Soc 2003; 51: 1085–91.
Monk TH. Aging human arcadian rhythms: conventional wisdom may not always be right. J Biol Rhythms 2005; 20: 366–74.
Lavie P. Melatonin: role in gating nocturnal rise in sleep propensity. J Biol Rhythms 1997; 12: 657–65.
Cajochen C, Krauchi K, Wirz-Justice A. Role of melatonin in the regulation of human circadian rhythms and sleep. J Neuroendocrinol 2003; 15: 432–7.
Dollins AB, Zhdanova IV, Wurtman RJ et al. Effect of inducing nocturnal serum melatonin concentrations in daytime on sleep, mood, body temperature, and performance. Proc Natl Acad Sci USA 1994; 91: 1824–8.
Arendt J, Skene DJ. Melatonin as a chronobiotic. Sleep Med Rev 2005; 9: 25–39.
Garfinkel D, Laudon M, Nof D et al. Improvement of sleep quality in elderly people by controlled-release melatonin. Lancet 1995; 346: 541–4.
Garfinkel D, Laudon M, Zisapel N. Improvement of sleep quality by controlled-release melatonin in benzodiazepine-treated elderly insomniacs. Arch Gerontol Geriatr 1997; 24: 223–31.
Hughes RJ, Sack RL, Lewy AJ. The role of melatonin and circadian phase in age-related sleep-maintenance insomnia: assessment in a clinical trial of melatonin replacement. Sleep 1998; 21: 52–68.
Zhdanova IV, Wurtman RJ, Regan MM et al. Melatonin treatment for age-related insomnia. J Clin Endocrinol Metab 2001; 86: 4727–30.
Leger D, Laudon M, Zisapel N. Nocturnal 6-sulfatoxymelatonin excretion in insomnia and its relation to the response to melatonin replacement therapy. Am J Med 2004; 116: 91–5.
Sack RL, Lewy AJ, Erb DL et al. Human melatonin production decreases with age. J Pineal Res 1986; 3: 379–88.
Benot S, Goberna R, Reiter RJ et al. Physiological levels of melatonin contribute to the antioxidant capacity of human serum. J Pineal Res 1999; 27: 59–64.
Garfinkel D, Zisapel N, Wainstein J et al. Facilitation of benzodiazepine discontinuation by melatonin: a new clinical approach. Arch Intern Med 1999; 159: 2456–60.
Siegrist C, Benedetti C, Orlando A et al. Lack of changes in serum prolactin, FSH, TSH, and estradiol after melatonin treatment in doses that improve sleep and reduce benzodiazepine consumption in sleep-disturbed, middle-aged, and elderly patients. J Pineal Res 2001; 30: 34–42.
Brzezinski A, Vangel MG, Wurtmann RJ et al. Effects of exogenous melatonin on sleep: a meta-analysis. Sleep Med Rev 2005; 9: 41–50.
Buscemi N, Vandermeer B, Hooton N et al. The efficacy and safety of exogenous melatonin for primary sleep disorders: A metaanalysis. J Gen Intern Med 2005; 20: 1151–8.
The Northside Hospital Sleep Medicine Institute Test. Available at http://www.nshsleep.com/test.cfm. Accessed February 20, 2006.
Yesavage JA, Brink TL, Rose TL et al. Development and validation of a geriatric depression screening scale: a preliminary report. J Psychiatr Res 1982–83; 17: 37–49.
Goldberg D, Bridges K, Duncan-Jones P et al. Detecting anxiety and depression in general medical settings. BMJ 1988; 297: 897–9.
Gorfine T, Assaf Y, Goshen-Gottstein Y et al. Sleep-anticipating effects of melatonin in the human brain. Neuroimage 2006; 31: 410–8.
Haimov I, Lavie P, Laudon M et al. Melatonin replacement therapy of elderly insomniacs. Sleep 1995; 18: 598–603.
Jean-Louis G, von Gizycki H, Zizi F. Melatonin effects on sleep, mood, and cognition in elderly with mild cognitive impairment. J Pineal Res 1998; 25: 177–83.
Leppamaki S, Partonen T, Vakkuri O et al. Effect of controlledrelease melatonin on sleep quality, mood, and quality of life in subjects with seasonal or weather-associated changes in mood and behaviour. Eur Neuropsychopharmacol 2003; 13: 137–45.
Almeida Montes LG, Ontiveros Uribe MP, Cortes Sotres J et al. Treatment of primary insomnia with melatonin: a double-blind, placebo-controlled, crossover study. J Psychiatry Neurosci 2003; 28: 191–6.
Dolberg OT, Hirschmann S, Grunhaus L. Melatonin for the treatment of sleep disturbances in major depressive disorder. Am J Psychiatry 1998; 155: 1119–21.
Buscemi N, Vandermeer B, Hooton N et al. Efficacy and safety of exogenous melatonin for secondary sleep disorders and sleep disorders accompanying sleep restriction: meta-analysis. BMJ 2006; 332: 385–93.
Cardinali DP, Gvozdenovich E, Kaplan MR et al. A double blind-placebo controlled study on melatonin efficacy to reduce anxiolytic benzodiazepine use in the elderly. Neuroendocrinol Lett 2002; 23: 55–60.
Frels C, Williams P, Narayanan S et al. Iatrogenic causes of falls in hospitalised elderly patients: a case-control study. Postgrad Med J 2002; 78: 487–9.
Landi F, Onder G, Cesari M et al. Psychotropic medications and risk for falls among community-dwelling frail older people: an observational study. J Gerontol A Biol Sci Med Sci 2005; 60: 622–6.
Dalton EJ, Rotondi D, Levitan RD et al. Use of slow-release melatonin in treatment-resistant depression. J Psychiatry Neurosci 2000; 25: 48–52.
Seabra ML, Bignotto M, Pinto LR Jr et al. Randomized, double-blind clinical trial, controlled with placebo, of the toxicology of chronic melatonin treatment. J Pineal Res 2000; 29: 193–200.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Garzón, C., Guerrero, J.M., Aramburu, O. et al. Effect of melatonin administration on sleep, behavioral disorders and hypnotic drug discontinuation in the elderly: a randomized, double-blind, placebo-controlled study. Aging Clin Exp Res 21, 38–42 (2009). https://doi.org/10.1007/BF03324897
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03324897