Summary
Introduction
Pioglitazone (from the group of thiazolidinediones) is now available in Italy for oral combination therapy for type 2 diabetes, after monotherapy with metformin or sulfonylurea has failed to control hyperglycaemia. Clinical trials have proved it can significantly improve HbA1c levels and lipid profiles.
Objective
Since treatment with pioglitazone, though effective, costs more than standard medications, an analysis was conducted to test its cost-effectiveness. Comparators were metformin and sulfonylurea.
Methods
Long term clinical data are not available about pioglitazone effectiveness, so a published Markov model was used to simulate the occurrence of severe complications and the life expectancy in a cohort of type 2 diabetic patients from the beginning of treatment until death. Baseline characteristics were UKPDS overweight patients’, but sensitivity analysis was performed on data from the CODE-2 Italian sub-study too. Local Italian unit costs for treatment and complications were used. The perspective was the National Health Service’s.
Results
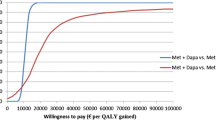
The model outcomes show that combination therapy with pioglitazone improves life expectancy more than any other treatment combination. After discounting costs and life expectancy at 5%, the incremental cost per life year gained (CLYG) of pioglitazone (PIO) 30 mg + metformin (MET) versus sulfonylurea (SU) + MET was € 41,859. The CLYG of PIO 30 mg + SU was € 20,981 versus MET + SU. The CLYG of PIO 15 mg + SU versus MET + SU was € 49,013.
Conclusions
The present study found that pioglitazone improves life expectancy and reduces complications at a cost that is fairly acceptable in terms of established cost-effectiveness thresholds. Pioglitazone represents an opportunity for the health care budget in Italy and should be one of the preferred options in the treatment of type 2 diabetes patients for the approved indications.
Similar content being viewed by others
Bibliografia
WHO. Diabetes mellitus. Fact Sheet N. 138, WHO information, 2002
Lucioni C, Garancini MP, Massi-Benedetti M, et al. The costs of type 2 diabetes mellitus in Italy. A CODE-2 Sub-Study. Treat Endocrinol 2003; 2(2): 121–33
UKPDS Group. Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet, 1998, 352(9131): 854–65
Stratton IM, Adler AI, Neil H, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ 2000; 321(7258): 405–12
UKPDS Group. UKPDS 24: a 6-year, randomized, controlled trial comparing sulfonylurea, insulin, and metformin therapy in patients with newly diagnosed type 2 diabetes that could not be controlled with diet therapy. Ann Intern Med 1998; 128(3): 165–75
Einhorn D, Rendell M, Rosenzweig J, et al. Pioglitazone hydrochloride in combination with metformin in the treatment of type 2 diabetes mellitus: a randomized, placebo-controlled study. The Pioglitazone 027 Study Group. Clin Ther 2000; 22(12): 1395–409
Kipnes MS, Krosnick A, Rendell MS, et al. Pioglitazone hydrochloride in combination with sulfonylurea therapy improves glycemic control in patients with type 2 diabetes mellitus: a randomized, placebo controlled study. Am J Med 2001; 111(1): 10–7
Shaffer S, Rubin CJ, Zhu E. The effect of pioglitazone on the lipid profile in patients with type 2 diabetes. Diabetes 2000; 49 (Suppl. 1): A125
Coyle D, Lee KM, O’Brien BJ. The role of models within economic analysis. Focus on Type 2 Diabetes Mellitus. PharmacoEconomics 2002; 20 (Suppl. 1): 11–9
Palmer AJ, Weiss C, Brandt A, et al. Cost-effectiveness of intensive therapy for type 1 diabetes changes depending on risk factors and level of existing complications. Med Decis Making 1999; 17(4): 528
Palmer AJ, Sendi PP, Spinas GA. Applying some UK Prospective Diabetes Study results to Switzerland: the cost-effectiveness of intensive glycaemic control with metformin versus conventional control in overweight patients with type-2 diabetes. Schweiz Med Wochenschr 2000; 130(27–28): 1034–40
Hunt L. Pioglitazone the answer to managing type 2 DM in Europe? Pharmacoeconomics and Outcomes News 2001; 343: 7–9
Coyle D, Palmer AJ, Tam R. Economic evaluation of pioglitazone hydrochloride in the management of type 2 diabetes mellitus in Canada. PharmacoEconomics 2002; 20 (Suppl. 1): 31–42
Henriksson F. Applications of economic models in healthcare: the introduction of pioglitazone in Sweden. PharmacoEconomics 2002; 20 (Suppl. 1): 43–53
Anderson KM, Odell PM, Wilson PW, et al. Cardiovascular disease risk profiles. Am Heart J 1991; 121 (1 Pt 2): 293–8
Wolf PA, D’Agostino RB, Belanger AJ, et al. Probability of stroke: a risk profile from the Framingham Study. Stroke 1991; 22(3): 312–8
Lewis EJ, Hunsicker LG, Bain RP, et al. The effect of angiotensin-converting-enzyme inhibition on diabetic nephropathy. N Engl J Med 1993; 329(20): 1456–62
Klein R, Klein BE, Moss SE, et al. The Wisconsin Epidemiologic Study of Diabetic Retinopathy. XV The long-term incidence of macular edema. Ophthalmology 1995; 102(1): 7–16
Assmann G, Schulte H, von Eckardstein A. Hypertriglyceridemia and elevated lipoprotein(a) are risk factors for major coronary events in middle-aged men. Am J Cardiol 1996; 77(14): 1179–94
Moss SE, Klein R, Klein BE. Long-term incidence of lower-extremity amputations in a diabetic population. Arch Fam Med 1996; 5(7): 391–8
Assmann G, Schulte H, Cullen P. New and classical risk factors. The Munster heart study (PROCAM). Eur J Med Res 1997; 2(6): 237–42
Molyneaux LM, Constantino MI, Mc Gill M, et al. Better glycaemic control and risk reduction of diabetic complications in Type 2 diabetes: comparison with the DCCT. Diabetes Res Clin Pract 1998; 42(2): 77–83
UKPDS Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet 1998; 352(9131): 837–53
UKPDS Group. Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes (UKPDS 38). BMJ 1998; 317(7160): 703–13
Palmer AJ, Neeser K, Paschen B, et al. Economic implications of the Total Ischaemic Burden Bisoprolol Study (TIBBS) follow-up. Journal of Medical Economics 1998; 1: 263–80
UKPDS Group. Efficacy of atenolol and captopril in reducing risk of macrovascular and microvascular complications in type 2 diabetes (UKPDS 39). BMJ 1998; 317(7160): 713–20
UKPDS Group. A randomized trial of efficacy of early addition of metformin in sulfonylurea-treated type 2 diabetes (UKPDS 28). Diabetes Care 1998; 21(1): 87–92
Matthews DR, Cull CA, Stratton IM, et al. Sulphonylurea failure in non-insulin-dependent diabetic patients over six years (UKPDS 26). Diabet Med 1998; 15(4): 297–303
Turner RC, Millns H, Neil HA, et al. Risk factors for coronary artery disease in non-insulin-dependent diabetes mellitus (UKPDS 23). BMJ 1998; 316(7134): 823–8
Turner RC, Cull CA, Frighi V, et al. Glycemic control with diet, sulphonylurea, metformin, or insulin in patients with type 2 diabetes mellitus: progressive requirement for multiple therapies (UKPDS 49). JAMA 1999; 281(21): 2005–12
Heart Outcomes Prevention Evaluation (HOPE) Study Investigators. Effects of ramipril on cardiovascular and microvascular outcomes in people with diabetes mellitus: results of the HOPE study and MICRO.HOPE substudy. Lancet 2000; 355(9200): 253–9
Kshirsagar AV, Joy MS, Hogan SL, et al. Effect of ACE inhibitors in diabetic and nondiabetic chronic renal disease: a systematic overview of randomized placebo-controlled trials. Am J Kidney Dis 2000; 35(4): 695–707
Stevens RJ, Kothari V, Adler AI, et al. The UKPDS risk engine: a model for the risk of coronary heart disease in Type II diabetes (UKPDS 56). Clin Sci (London) 2001; 101(6): 671–9
Ministero della Sanità. Aggiornamento delle tariffe delle prestazioni di assistenza ospedaliera di cui al Decreto Ministeriale 14 dicembre 1994. Decreto Ministeriale 12 marzo 1997. Suppl. ord. alla G.U. n. 209, 8 settembre 1997
Ministero della Sanità. Prestazioni di assistenza specialistica ambulatoriale erogabili nell’ambito del Servizio Sanitario Nazionale e relative tariffe. Decreto Ministeriale 22 luglio 1996. Suppl. ord. alla G.U. n. 216, 14 settembre 1996
Legge 18/1980 (Indennità di accompagnamento agli invalidi civili totalmente inabili), pubblicata su G.U. n. 44, 14 febbraio 1980
Porta M, Rizzitello A, Tomalino M, et al. Comparison of the cost-effectiveness of three approaches to screening for and treating sight-threatening diabetic retinopathy. Diabetes & Metabolism 1999; 25: 44–53
Lucioni C, Mazzi S, Serra G. L’autocontrollo del livello glicemico nei pazienti con diabete di tipo 2: i risultati dello studio CODE-2. Il Diabete, ottobre 1999
Cantagallo A. Costo-efficacia di un programma di prevenzione con dieta a basso contenuto proteico nella nefropatia diabetica. Mecosan 1999: 29: 9–17
Informatore Farmaceutico, marzo 2003 (aggiornamento). Milano; OEMF, 2003
Musacchio N, Lo Monaco G, Rocca A, et al. Razionalizzazione dell’erogazione dei presidi per diabetici in un distretto sociosanitario della Regione Lombardia. Giornale Italiano di Diabetologia 1998; 18: 157–60
IMS. Il mercato farmaceutico. Milano: IMS Health, 2002
Tengs TO, Adams ME, Pliskin JS, et al. Five-hundred life-saving interventions and their cost-effectiveness. Risk Anal 1995; 15(3): 369–90
Gold MR (ed.), Siegel JE, Russel L, et al. Cost-effectiveness in Health and Medicine. New York; Oxford University Press, 1996
Goldman L, Garber AM, Grover SA, Hlatky MA. 27th Bethesda Conference: matching the intensity of risk factor management with the hazard for coronary heart disease events. Task Force 6. Cost effectiveness of assessment and management of risk factors. J Am Coll Cardiol 1996; 27(5): 1020–30
National Institute of Clinical Excellence. NICE Present Evidence to Health Select Committee. London; NICE, 2002
Messori A, Santarlasci B, Trippoli S, et al. Controvalore economico del farmaco e beneficio clinico: stato dell’arte della metodologia e applicazione di un algoritmo farmacoeconomico. PharmacoEconomics — Italian Research Articles 2003; 5(2): 53–67
Author information
Authors and Affiliations
Corresponding author
Additional information
I peer reviewers, per questo articolo, sono stati coordinati da Livio Garattini.
Rights and permissions
About this article
Cite this article
Lucioni, C., Mazzi, S. & Neeser, K. Analisi di costo-efficacia della terapia combinata con pioglitazone nel trattamento del diabete mellito di tipo 2 in Italia. Pharmacoeconomics-Ital-Res-Articles 6, 81–93 (2004). https://doi.org/10.1007/BF03320626
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03320626