Abstract
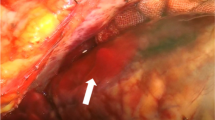
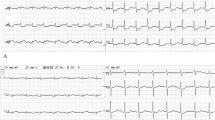
A 76-year-old woman was referred to our hospital because of postinfarction ventricular septal perforation (VSP). VSP occurred twelve days after acute myocardial infarction and resulted in interventricular shunt with Qp/Qs of 4.8. Because she suffered from pulmonary edema and oligouria, she underwent emergent surgical treatment after application of the intraaortic balloon pump. The infarction involved whole of right ventricle and the inferoposterior wall of left ventricle, and the location of the perforation was infero-septum with the size of 10 × 6 mm. A bovine pericardial patch was tailored in a triangular shape of approximately 7 × 7 × 5 cm. The base of the patch was sutured to the fibrous annulus of the mitral valve and medial margin of the patch was sewn to healthy septal endocardium. And the lateral side of the patch was sutured to the posterior wall of the left ventricle. Because of difficulty in weaning of the cardiopulmonary bypass, a percutaneous cardiopulmonary support system (PCPS) was inserted via femoral artery and vein with a flow support of 2.0 L/min. After 4 days support of PCPS, improvement of right ventricular function was detected by echocardiogram and PCPS was removed. While PCPS support, low dose heparin to maintain ACT level around 150 seconds was continuously administered. Any complication including bleeding and thrombosis was not remarkable. The patient was discharged on the 53th postoperative day, and is now doing well.
Similar content being viewed by others
References
David TE: Surgical treatment of postinfarction ventricular septal rupture. Australas J Cardiac Thorac Surg 1: 7–10, 1992
Komeda M, Fremes SE, David TE: Surgical repair of postinfarction ventricular septal defect Circulation 82(Suppl): IV 243–247, 1990
David TE, Dale L, Sun Z: Postinfaction ventricular septal rupture. Repair by endocardial patch with infarct exclusion. J Thorac Cardiovasc Surg 110: 1315–1322, 1995
Moore CA, Nygaard TW, Kaiser DL, Cooper AA, Gibson RS: Postinfarction ventricular septal rupture. The importance of location of infarction and right ventricular function in determining survival. Circulation 74: 45–55, 1986
Cummings RG, Reimer KA, Califf R, Hackel D, Boswick J, Lowe JE: Quantitative analysis of right and left ventricular infarction in the presence of postinfarction ventricular septal defect. Circulation 77: 33–42, 1988
Dagget WM, Guyton RA, Mundth ED, Buckly MJ, McEnany MT, Gold HK, Leinbach RC, Austen WC: Surgery for post-myocardial infarct ventricular septal defect. Ann Surg 186: 260–271, 1977
Dagget WM: Surgical technique for early repair of posterior ventricular septal rupture. J Thorac Cardiovase Surg 84: 306–312, 1982
Deville C, Fontan F, Chevalier JM, et al: Surgery for postinfarction ventricular septal defect, Risk factors for hospital death and long-term results. Eur J Cardiothorac Surg 5: 167–75, 1991
Skillington PD, Davies RH, Luff AJ, Williams JD, Dawkins KD, Conway N, Lanb RK, Shore DF, Monro JL, Ross JK: Surgical treatment for infarct-related ventricular septal defects. Improved early results combined with analysis of late functional status. J Thorac Cardiovasc Surg 99: 798–808, 1990
Cummings RG, Califf R, Jones RN, Reimer KA, Kong YH, Lowe JE: Correlates of survival in patients with postinfarction ventricular defect. Ann Thorac Surg 47: 824–830, 1989
Zehnder M, Kasper W, Kauder E, Schönthaler M, Geibel A, Olshewski M, Just H: Right ventricular infarction as an independent predictor of prognosis after acute inferior myocardial infarction. N Engl J Med 328: 981–988, 1993
Low dose systemic heparinization. 23: 612–617, 1994
45: 1159–1164, 1997
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Yamaguchi, A., Adachi, H., Tsuboi, J. et al. Surgical treatment with infarction exclusion technique and postoperative percutaneous cardiopulmonary support for a patient with ventricular septal perforation —A case report—. Jpn J Thorac Caridovasc Surg 46, 307–311 (1998). https://doi.org/10.1007/BF03217747
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03217747