Summary
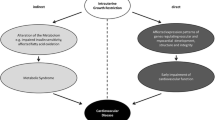
In recent years, a relation has been shown between low birth weight and a higher risk of diseases in adult life, particularly hypertension, cardiovascular diseases and type 2 diabetes. Causal factor could be intrauterine growth retardation, which interferes with the development and function of organs (called programming).
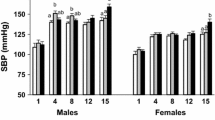
Human and animal studies show that programming of the kidney leads to a reduced number of nephrons. In order to compensate, there is hyperfiltration in remnant nephrons, leading to glomerular and systemic hypertension and glomerulosclerosis, with renal failure as endpoint. Oligonephronia makes the kidneys more vulnerable: in case of accessory renal disease, prognosis seems to deteriorate with low birth weight.
The renin-angiotensin system (ras) appears to play an important role based on its influence on renal hemodynamics, which is altered when associated with low birth weight. Animal studies suggest the ras as means for pharmacological manipulation of the low birth weight consequences. However, more data is needed before coming to clinical implications.
Samenvatting
De laatste jaren is er bewijs geleverd voor een relatie tussen een laag geboortegewicht en een toegenomen risico op aandoeningen op latere leeftijd, zoals hypertensie, hart- en vaatziekten en diabetes mellitus type II. Oorzakelijk dient gedacht te worden aan intra-uteriene groeivertraging, hetgeen interfereert met de aanleg en functie van organen (herprogrammering genoemd).
Uit onderzoek bij de mens en diverse proefdiermodellen blijkt herprogrammering van de nier voor een afgenomen hoeveelheid nefronen te zorgen. Ter compensatie treedt er in de aanwezige nefronen hyperfiltratie op, leidend tot glomerulaire en systemische hypertensie en glomerulosclerose, met als eindpunt nierinsufficiëntie. Door het verminderde aantal nefronen zijn de nieren kwetsbaarder; in het geval van bijkomende renale aandoeningen lijkt de prognose slechter te zijn bij een laag geboortegewicht.
De rol van het renine-angiotensine-systeem (ras) is belangrijk gezien de invloed ervan op de renale hemodynamiek, die veranderd is bij een laag geboortegewicht. Uit proefdieronderzoek lijkt het ras een aangrijpingspunt te bieden voor medicamenteuze manipulatie van de gevolgen van een laag geboortegewicht. Aanvullende gegevens zijn echter noodzakelijk om tot klinische implicaties te komen.
Similar content being viewed by others
Literatuur
Barker DJ, Osmond C. Infant mortality, childhood nutrition, and ischaemic heart disease in England and Wales. Lancet 1986;1:1077-81.
Law CM, Swiet M de, Osmond C, et al. Initiation of hypertension in utero and its amplification throughout life. BMJ 1993; 306:24-7.
Hales CN, Barker DJ, Clark PM, et al. Fetal and infant growth and impaired glucose tolerance at age 64. BMJ 1991; 303:1019-22.
Barker DJ. Fetal origins of coronary heart disease. BMJ 1995;311:171-4.
Barker DJ, Gluckman PD, Godfrey KM, et al. Fetal nutrition and cardiovascular disease in adult life. Lancet 1993;341:938-41.
Kramer MS. Invited commentary: association between restricted fetal growth and adult chronic disease: is it causal? Is it important? Am J Epidemiol 2000;152:605-8.
IJzerman RG, Stehouwer CD, Boomsma DI. Evidence for genetic factors explaining the birth weight-blood pressure relation : analysis in twins. Hypertension 2000;36:1008-12.
Merlet-Benichou C, Vilar J, Lelievre-Pegorier M, et al. Fetal nephron mass: its control and deficit. Adv Nephrol Necker Hosp 1997;26:19-45.
Brenner BM, Lawler EV, Mackenzie HS. The hyperfiltration theory: a paradigm shift in nephrology. Kidney Int 1996;49: 1774-7.
Hostetter TH, Olson JL, Rennke HG, et al. Hyperfiltration in remnant nephrons: a potentially adverse response to renal ablation. Am J Physiol 1981;241:F85-F93.
Garrett PJ, Bass PS, Sandeman DD. Barker, Brenner, and babies – early environment and renal disease in adulthood. J Pathol 1994;173:299-300.
Hinchliffe SA, Lynch MR, Sargent PH, et al. The effect of intrauterine growth retardation on the development of renal nephrons. Br J Obstet Gynaecol 1992;99:296-301.
Merlet-Benichou C, Gilbert T, Vilar J, et al. Nephron number: variability is the rule. Causes and consequences. Lab Invest 1999;79:515-27.
Konje JC, Bell SC, Morton JJ, et al. Human fetal kidney morphometry during gestation and the relationship between weight, kidney morphometry and plasma active renin concentration at birth. Clin Sci (Colch ) 1996;91:169-75.
Spencer J, Wang Z, Hoy W. Low birth weight and reduced renal volume in aboriginal children. Am J Kidney Dis 2001; 37:915-20.
Woods LL, Ingelfinger JR, Nyengaard JR, Rasch R. Maternal protein restriction suppresses the newborn renin-angiotensin system and programs adult hypertension in rats. Pediatr Res 2001;49:460-7.
Jones SE, Bilous RW, Flyvbjerg A, Marshall SM. Intra-uterine environment influences glomerular number and the acute renal adaptation to experimental diabetes. Diabetologia 2001;44:721-8.
Vanpee M, Blennow M, Linne T, et al. Renal function in very low birth weight infants: normal maturity reached during early childhood. J Pediatr 1992;121:784-8.
Vasarhelyi B, Dobos M, Reusz GS, et al. Normal kidney function and elevated natriuresis in young men born with low birth weight. Pediatr Nephrol 2000;15:96-100.
Kistner A, Celsi G, Vanpee M, Jacobson SH. Increased blood pressure but normal renal function in adult women born preterm. Pediatr Nephrol 2000;15:215-20.
Monge M, Garcia-Nieto VM, Domenech E, et al. Study of renal metabolic disturbances related to renal lithiasis at school age in very-low-birth-weight children. Nephron 1998;79:269-73.
Regina S, Lucas R, Miraglia SM, et al. Intrauterine food restriction as a determinant of nephrosclerosis. Am J Kidney Dis 2001;37:467-76.
Baudoin P, Provoost AP, Molenaar JC. Renal function up to 50 years after unilateral nephrectomy in childhood. Am J Kidney Dis 1993;21:603-11.
Wikstad I, Celsi G, Larsson L, et al. Kidney function in adults born with unilateral renal agenesis or nephrectomized in childhood. Pediatr Nephrol 1988;2:177-82.
Howie AJ. Age and effects of reduced renal mass. J Pathol 1995;176:321.
Provoost AP. Lange-termijnvervolgonderzoek van mensen met een solitaire nier. Ned Tijdschr Geneeskd 1995;139:214-9.
Woods LL. Neonatal uninephrectomy causes hypertension in adult rats. Am J Physiol 1999;276:R974-8.
Gurnani A, Nenov V, Taal MW, et al. Congenital nephron deficit (first hit) predicts increased renal injury in uninephrectomized rats (second hit). American Society of Nephrology Renal Week 2000;A3268.
Zidar N, Avgustin CM, Kenda RB, Ferluga D. Unfavorable course of minimal change nephrotic syndrome in children with intrauterine growth retardation. Kidney Int 1998;54:1320-3.
Sheu JN, Chen JH. Minimal change nephrotic syndrome in children with intrauterine growth retardation. Am J Kidney Dis 2001;37:909-14.
Zidar N, Cavic MA, Kenda RB, et al. Effect of intrauterine growth retardation on the clinical course and prognosis of IgA glomerulonephritis in children. Nephron 1998;79:28-32.
Nelson RG, Morgenstern H, Bennett PH. Birth weight and renal disease in Pima Indians with type 2 diabetes mellitus. Am J Epidemiol 1998;148:650-6.
Rossing P, Tarnow L, Nielsen FS, et al. Low birth weight. A risk factor for development of diabetic nephropathy? Diabetes 1995;44:1405-7.
Wintour EM. The renin-angiotensin system and the development of the kidney. Trends Endocrinol Metab 1997;8:199-207.
Manning J, Vehaskari VM. Low birth weight-associated adult hypertension in the rat. Pediatr Nephrol 2001;16:417-22.
Vehaskari VM, Aviles DH, Manning J. Prenatal programming of adult hypertension in the rat. Kidney Int 2001;59:238-45.
Langley-Evans SC, Sherman RC, Welham SJ, et al. Intrauterine programming of hypertension: the role of the renin-angiotensin system. Biochem Soc Trans 1999;27:88-93.
Kingdom JC, Hayes M, McQueen J, et al. Intrauterine growth restriction is associated with persistent juxtamedullary expression of renin in the fetal kidney. Kidney Int 1999;55:424-9.
Nakaya H, Sasamura H, Hayashi M, Saruta T. Temporary treatment of prepubescent rats with angiotensin inhibitors suppresses the development of hypertensive nephrosclerosis. J Am Soc Nephrol 2001;12:659-66.
Author information
Authors and Affiliations
Corresponding author
Additional information
M.F. Schreuder, agiko.
Correspondentieadres: M.F. Schreuder, vu medisch centrum, afdeling Kindergeneeskunde, Postbus 7057, 1007 MB Amsterdam.
Dr. M. Fodor, onderzoeker.
Dr. J.A.E. van Wijk, kinderarts-nefroloog.
Prof.dr. H.A. Delemarre-van de Waal, kinderarts-endocrinoloog. Onderzoeksinstituut Endocrinologie, Voortplanting en Metabolisme, afdeling Kindergeneeskunde, vu medisch centrum, Amsterdam.
Rights and permissions
About this article
Cite this article
Schreuder, M.F., Fodor, M., van Wijk, J.A.E. et al. Laag geboortegewicht: consequenties voor de nier?. KIND 70, 49–53 (2002). https://doi.org/10.1007/BF03061371
Issue Date:
DOI: https://doi.org/10.1007/BF03061371