Abstract
Purpose
To assess the analgesic and side effects of the continuous epidural infusion of 0.2% ropivacaine combined with morphine compared to both drugs alone.
Methods
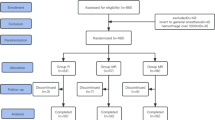
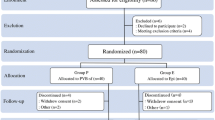
In this study, both observers and patients were blinded to patient group assignment. Sixty patients scheduled to undergo lower abdominal surgery were enrolled. Patients were randomized to one of three postoperative treatment groups: 1) combination group (a combination of 0.2% ropivacaine and 0.003% morphine); 2) morphine group (0.003% morphine); or 3) ropivacaine group (0.2% ropivacaine). Postoperatively, all solutions were administered epidurally at a rate of 6 mL·hr-1 for 24 hr. Patients were given iv flurbiprofen as a supplemental analgesic on demand.
Results
The combination group showed lower visual analogue scale scores than those of patients receiving either drug alone, both at rest and on coughing. The combination group showed a slight motor block at two hours after the continuous epidural infusion, while the ropivacaine and morphine groups did not show any motor block. The incidence of itching was significantly increased in the morphine and combination groups, compared to the ropivacaine group. There was no significant difference between the numbers of patients with nausea in the three groups. No hypotension or respiratory complications were observed in the three groups.
Conclusion
The combination of epidural 0.2% ropivacaine and 0.003% morphine has more effective analgesic effects than either of the drugs alone for postoperative pain relief after lower abdominal surgery.
Résumé
Objectif
Comparer l’effet analgésique et les effets secondaires d’une perfusion péridurale continue de ropivacaïne à 0,2 % combinée à la morphine à ceux des deux médicaments employés seuls.
Méthode
Dans notre étude, la répartition des sujets s’est faite à l’insu des observateurs et des patients. Nous avons recruté 60 patients devant subir une intervention abdominale basse. Ils ont été répartis en trois groupes: 1) combinaison médicamenteuse (ropivacaïne à 0,2% et morphine à 0,003 %); 2) morphine (morphine à 0,003 %); 3) ropivacaïne (ropivacaïne à 0,2 %). Après l’opération, toutes les solutions ont été administrées par voie péridurale au débit de 6 mL·h-1 pendant 24 h. Les patients ont reçu du flurbiprofène iv comme analgésique complémentaire sur demande.
Résultats
Avec la combinaison de médicaments, comparée à chacun employé seul, on a noté des scores plus bas à l’échelle visuelle analogique et ce, au repos et pendant la toux. La combinaison de médicaments a produit un léger blocage moteur deux heures après la perfusion péridurale continue, mais la ropivacaïne et la morphine n’en ont pas provoqué. L’incidence de prurit a été significativement accrue avec la morphine et la combinaison médicamenteuse, comparées à la ropivacaïne. Il n’y a pas eu de différence intergroupe significative pour l’incidence des nausées. Dans les trois groupes, aucun cas d’hypotension ou de complications respiratoires n’a été observé.
Conclusion
La combinaison de ropivacaïne à 0,2 % et de morphine à 0,003 % a des effets analgésiques plus efficaces que l’un ou l’autre médicament seul pour le soulagement des douleurs après une opération abdominale basse.
Article PDF
Similar content being viewed by others
References
Feldman HS, Arthur GR, Pitkanen M, Hurley R, Doucette AM, Covino BG. Treatment of acute systemic toxicity after the rapid intravenous injection of ropivacaine and bupivacaine in the conscious dog. Anesth Analg 1991; 73: 373–84.
Reiz S, Haggmark S, Johansson G, Nath S. Cardiotoxicity of ropivacaine-a new amide local anaesthetic agent. Acta Anaesthesiol Scand 1989; 33: 93–8.
Scott DB, Lee A, Fagan D, Bowler GM, Bloomfield P, Lundh R. Acute toxicity of ropivacaine compared with that of bupivacaine. Anesth Analg 1989; 69: 563–9.
Bader AM, Datta S, Flanagan H, Covino BG. Comparison of bupivacaine- and ropivacaine-induced conduction blockade in the isolated rabbit vagus nerve. Anesth Analg 1989; 68: 724–7.
Scott DA, Chamely DM, Mooney PH, Deam RK, Mark AH, Hagglof B. Epidural ropivacaine infsion for postoperative analgesia after major lower abdominal surgery-a dose finding study. Anesth Analg 1995; 81: 982–6.
Etches RC, Writer WD, Ansley D, et al. Continuous epidural ropivacaine 0.2% for analgesia after lower abdominal surgery. Anesth Analg 1997; 84: 784–90.
Berti M, Casati A, Fanelli G, et al. 0.2% ropivacaine with or without fentanyl for patient-controlled epidural analgesia after major abdominal surgery: a double-blind study. J Clin Anesth 2000; 12: 292–7.
Scott DA, Blake D, Buckland M, et al. A comparison of epidural ropivacaine infusion alone and in combination with 1, 2, and 4 µg/mL fentanyl for seventy-two hours of postoperative analgesia after major abdominal surgery. Anesth Analg 1999; 88: 857–64.
Finucane BT, Ganapathy S, Carli F, et al. Prolonged epidural infusions of ropivacaine (2 mg/mL) after colonic surgery: the impact of adding fentanyl. Anesth Analg 2001; 92: 1276–85.
Niv D, Rudick V, Chayen MS, David MP. Variations in the effect of epidural morphine in gynecological and obstetric patients. Acta Obstet Gynecol Scand 1983; 62: 455–9.
Niv D, Rudick V, Golan A, Chayen MS. Augmentation of bupivacaine analgesia in labor by epidural morphine. Obstet Gynecol 1986; 67: 206–9.
Watcha MF, White PF. Postoperative nausea and vomiting. Its etiology, treatment, and prevention. Anesthesiology 1992; 77: 162–84.
Dahl JB, Rosenberg J, Hansen BL, Hjortso NC, Kehlet H. Differential analgesic effects of low-dose epidural morphine and morphine-bupivacaine at rest and during mobilization after major abdominal surgery. Anesth Analg 1992; 74: 362–5.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Niiyama, Y., Kawamata, T., Shimizu, H. et al. The addition of epidural morphine to ropivacaine improves epidural analgesia after lower abdominal surgery. Can J Anaesth 52, 181–185 (2005). https://doi.org/10.1007/BF03027726
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03027726