Abstract
Purpose
The GlideScope® videolaryngoscope usually provides excellent glottic visualization, but directing an endotracheal tube (ETT) through the vocal cords is sometimes difficult. The goal of the study was to determine which of two ETT angles (60°vs 90°) and cambers (forwardvs reverse) was better, as determined by time to intubation (TTI).
Methods
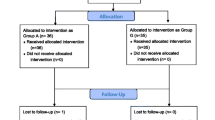
Tw o hundred patients requiring orotracheal intubation for elective surgery were randomly allocated to one of four groups: A) 90° angle, forward camber; B) 90° angle, reverse camber; C) 60° angle, forward camber; D) 60° angle, reverse camber. Time to intubation was assessed by a blinded observer. Operators were blinded until the point of intubation. A visual analogue scale (VAS) assessed the ease of intubation. The number of intubation attempts, number of failures, glottic grades, and use of external laryngeal manipulation were recorded.
Results
The angle of the ETT had an impact on TTI but camber did not. The 90° angle demonstrated a 13% faster TTI than the 60° angle (47.1 ± 21.2 secvs 54.4 ± 28.2 sec,P = 0.042), and it resulted in easier intubation (VAS 16.4 ± 14.2 mmvs 27.3 ± 23.5 mm,P = 0.0001). The overall incidence of a grade 1 or 2 Cormack-Lehane glottic view was 99%.
Conclusions
In a heterogeneous group of operators and patients intubated with the GlideScope®, a 90° ETT angle provided the best result and should be the initial configuration. The camber of the ETT does not affect the time to intubation.
Résumé
Objectif
Le vidéo-laryngoscope GlideScope® offre en général une excellente visualisation glottique; toutefois, il est parfois difficile d’orienter la sonde endotrachéale (SET) entre les cordes vocales. Le but de cette étude était de déterminer lequel de deux angles de SET (60° vs 90°) et quelle cambrure (avant vs arrière) étaient les meilleurs, déterminés selon le temps requis pour l’intubation (TRI).
Méthodes
Deux cents patients nécessitant une intubation oro-trachéale pour une chirurgie réglée ont été répartis en quatre groupes de façon aléatoire: a) angulation de 90°, cambrure avant; b) angulation de 90°, cambrure arrière; c) angulation de 60°, cambrure avant; d) angulation de 60°, cambrure arrière. Le temps requis pour l’intubation était estimé par un observateur ignorant le groupe d’allocation. Les opérateurs ont été tenus ignorants du groupe d’allocation jusqu’à l’intubation. Une échelle visuelle analogique (VAS) permettait d’estimer la facilité d’intubation. Le nombre de tentatives d’intubation, d’échecs, les grades glottiques ainsi que l’utilisation de manipulation laryngée externe étaient notés.
Résultats
L’angulation de la SET a eu un impact sur le TRI mais pas la cambrure. Avec une angulation de 90°, le TRI était de 13% plus rapide qu’avec une angulation de 60° (47,1 ± 21,2 sec vs 54,4 ± 28,2 sec, P = 0,042), et l’ intubation était plus facile (VAS 16,4 ± 14,2 mm vs 27,3 ± 23,5 mm, P = 0,0001). L’incidence globale d’une visualisation glottique Cormack-Lehane de grade I ou 2 a été de 99 %.
Conclusions
Dans un groupe hétérogène d’opérateurs et de patients intubés avec le GlideScope®, une angulation de la SET de 90° offre le meilleur résultat et devrait être la configuration initiale. La cambrure de la SET n’affecte pas le temps requis pour l’intubation.
Article PDF
Similar content being viewed by others
References
Cooper RM, Pacey JA, Bishop MJ, McCluskey SA. Early clinical experience with a new videolaryngoscope (GlideScope) in 728 patients. Can J Anesth 2005; 52: 191–8.
Doyle DJ. The GlideScope video laryngoscope. Anaesthesia 2005; 60: 414–5.
Cuchillo JV, Rodriguez MA. Considerations aimed at facilitating the use of the new GlideScope videolaryn- goscope (Letter). Can J Anesth 2005; 52: 661.
The GlideScope® Video Intubation System - Operator & Service Manual. Burnaby, BC, Canada: Saturn Biomedical Systems Inc.; 2003.
Bader SO, Heitz JW, Audu PB. Tracheal intubation with the GlideScope® videolaryngoscope, using a “J” shaped endotracheal tube (Letter). Can J Anesth 2006; 53: 634–5.
Cooper RM. Considerations aimed at facilitating the use of the new GlideScope videolaryngoscope (Letter, reply). Can J Anesth 2005; 52: 661–2.
Mallampati SR, Gatt SP, Gugino LD, et al. A clinical sign to predict difficult tracheal intubation: a prospective study. Can Anaesth Soc J 1985; 32: 429–34.
Cormack RS, Lehane J. Difficult tracheal intubation in obstetrics. Anaesthesia 1984; 39: 1105–11.
Lim TJ, Lim Y, Liu EH. Evaluation of ease of intubation with the GlideScope or Macintosh laryngoscope by anaesthetists in simulated easy and difficult laryn- goscopy. Anaesthesia 2005; 60: 180–3.
Turkstra TP, Craen RA, Pelz DM, Gelb AW. Cervical spine motion: a fluoroscopic comparison during intubation with lighted stylet, GlideScope, and Macintosh laryngoscope. Anesth Analg 2005; 101: 910–5.
Hardman JG, Wills JS, Aitkenhead AR. Factors deter- mining the onset and course of hypoxemia during apnea: an investigation using physiological modelling. Anesth Analg 2000; 90: 619–24.
Falco-Molmeneu E, Ramirez-Montero F, Carregui-Tuson R, Santamaria-Arribas N, Gallen-Jaime T, Vila-Sanchez M. The modified Eschmann guide to facilitate tracheal intubation using the GlideScope® (Letter). Can J Anesth 2006; 53: 633–4.
Sun DA, Warriner CB, Parsons DG, Klein R, Umedaly HS, Moult M. The GlideScope® Video Laryngoscope: randomized clinical trial in 200 patients. Br J Anaesth 2005; 94: 381–4.
Rai MR, Dering A, Verghese C. The Glidescope system: a clinical assessment of performance. Anaesthesia 2005; 60: 60–4.
Halligan M, Charters P. A clinical evaluation of the Bonfils Intubation Fibrescope. Anaesthesia 2003; 58: 1087–91.
Holden JD. Hawthorne effects and research into professional practice. J Eval Clin Pract 2001; 7: 65–70.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure statement: This study was internally funded. None of the authors have any conflicts to report
Rights and permissions
About this article
Cite this article
Jones, P.M., Turkstra, T.P., Armstrong, K.P. et al. Effect of stylet angulation and endotracheal tube camber on time to intubation with the GlideScope®. Can J Anesth 54, 21–27 (2007). https://doi.org/10.1007/BF03021895
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03021895