Abstract
Purpose
Ischemic brainstem stroke resulting from occlusion of the basilar artery during cervical spine surgery in a previously asymptomatic patient is a rare event. We report the development of a large ischemic brainstem stroke, resulting from occlusion of the basilar artery during anterior cervical discectomy, in a patient without previous neurological deficit, or signs of vertebrobasilar insufficiency.
Clinical features
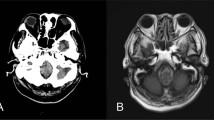
A 55-yr-old, diabetic and hypertensive male who developed a cervical spine infection, underwent surgery for anterior discectomy at C5-C6. During the 2.5-hr long procedure the patient was lying supine with his neck hyperextended. Except for a temporary reduction in systolic blood pressure, the intraoperative course was uneventful. At the end of surgery the patient remained unconscious with flaccid paralysis in all extremities, fixed pinpoint pupils, low respiratory rate, and no response to painful stimuli. Naloxone administration did not improve the clinical picture, while brain computed tomography showed a large brainstem and cerebellar stroke, implicating basilar artery occlusion. The patient died five days later from stroke complications. Intraoperative surgical manipulation with a severely inflamed vertebral system, as well as prolonged neck hyperextension occluding the blood flow of vertebrobasilar arteries might have contributed to fatal brainstem stroke in this patient.
Conclusion
Neck surgery carries a potential risk for posterior circulation stroke, and this report heightens awareness of this rare, but serious complication.
Résumé
Objectif
Un accident ischémique du tronc cérébral, résultat de ľocclusion de ľartère basilaire pendant une opération de la colonne cervicale chez un patient auparavant asymptomatique, est un événement rare. Nous présentons le cas ďun important accident ischémique du tronc cérébral causé par ľocclusion de ľartère basilaire pendant une discectomie cervicale antérieure chez un patient sans déficit neurologique ou signes ďinsuffisance vertébro-basilaire connus.
Éléments cliniques
Un homme de 55 ans, diabétique et hypertendu, ayant une infection de la colonne cervicale, a subi une discectomie antérieure en C5-C6. Pendant ľopération de 2,5 h, le patient était en décubitus dorsal avec le cou en hyperextension. Ľopération s’est déroulée sans incident, sauf une réduction temporaire de la tension artérielle systolique. À la fin de ľopération, le patient est demeuré inconscient et présentait une paralysie flasque aux extrémités, des micropupilles fixes, une fréquence respiratoire faible et aucune réaction aux stimuli douloureux. Ľadministration de naloxone n’a pas corrigé la situation et la tomodensitométrie du cerveau a montré un accident vasculaire important du tronc cérébral et du cervelet consécutif à ľocclusion de ľartère basilaire. Le patient est décédé cinq jour plus tard des complications de ľaccident vasculaire. Les manipulations chirurgicales peropératoires ďun système vertébral sévèrement enflammé et ľhyperextension prolongée du cou, bloquant le débit sanguin des artères vertébrobasilaires, ont pu contribuer à ľaccident vasculaire fatal du tronc cérébral.
Conclusion
Ľopération du cou comporte un risque potentiel ďaccident circulatoire postérieur et notre article présente cette complication rare, mais grave.
Article PDF
Similar content being viewed by others
References
Forrest JB, Cahalan MK, Rehder K, et al. Multicenter study of general anesthesia. II. Results. Anesthesiology 1990; 72: 262–8.
Larsen SF, Zaric D, Boysen G. Postoperative cerebrovascular accidents in general surgery. Acta Anaesthesiol Scand 1988; 32: 698–701.
Turnipseed WD, Berkoff HA, Belzer FO. Postoperative stroke in cardiac and peripheral vascular disease. Ann Surg 1980; 192: 365–8.
Landercasper J, Merz BJ, Cogbill TH, et al. Perioperative stroke risk in 173 consecutive patients with a past history of stroke. Arch Surg 1990; 125: 986–9.
Harris EJ Jr, Moneta GL, Yeager RA, Taylor LM Jr, Porter JM. Neurologic deficits following noncarotid vascular surgery. Am J Surg 1992; 163: 537–40.
Limburg M, Wijdicks EF, Li H. Ischemic stroke after surgical procedures. Clinical features, neuroimaging, and risk factors. Neurology 1998; 50: 895–901.
Wong GY, Warner DO, Schroeder DR, et al. Risk of sur gery and anesthesia for ischemic stroke. Anesthesiology 2000; 92: 425–32.
Hart R, Hindman B. Mechanisms of perioperative cerebral infarction. Stroke 1982; 13: 766–73.
Parikh S, Cohen JR. Perioperative stroke after general surgical procedures. N Y State J Med 1993; 93: 162–5
Lee TH, Hsu WC, Chen CJ, Chen ST. Etiologic study of young ischemic stroke in Taiwan. Stroke 2002; 33: 1950–5.
Jeng JS, Chung MY, Yip PK, Hwang BS, Chang YC. Extracranial carotid atherosclerosis and vascular risk factors in different types of ischemic stroke in Taiwan. Stroke 1994; 25: 1989–93.
Blacker DJ, Flemming KD, Wijdicks EF. Risk of ischemic stroke in patients with symptomatic vertebrobasilar stenosis undergoing surgical procedures. Stroke 2003; 34: 2659–63.
Evans BA, Wijdicks EF. High-grade carotid stenosis detected before general surgery: is endarterectomy indicated? Neurology 2001; 57: 1328–30.
Hosoya T, Adachi M, Yamaguchi K, Haku T, Kayama T, Kato T. Clinical and neuroradiological features of intracranial vertebrobasilar artery dissection. Stroke 1999; 30: 1083–90.
Tettenborn B, Caplan LR, Sloan MA, et al. Postoperative brainstem and cerebellar infarcts. Neurology 1993; 43: 471–7.
Nwokolo N, Bateman DE. Stroke after a visit to the hairdresser. Lancet 1997; 350: 866.
Nosan DK, Gomez CR, Maves MD. Perioperative strok in patients undergoing head and neck surgery. Ann Otol Rhinol Laryngol 1993; 102: 717–23.
Sherman DG, Hart RG, Easton JD. Abrupt change in head position and cerebral infarction. Stroke 1981; 12 2–6.
Weintraub MI, Khoury A. Critical neck position as an independent risk factor for posterior circulation stroke. A magnetic resonance angiographic analysis. J Neuroimaging 1995; 5: 16–22.
Weintraub MI, Khoury A. Cerebral hemodynamic changes induced by simulated tracheal intubation: a possible role in perioperative stroke? Magnetic resonance angiography and flow analysis in 160 cases. Stroke 1998; 29: 1644–9.
Chaturvedi S, Lukovits TG, Chen W, Gorelick PB. Ischemia in the territory of a hypoplastic vertebrobasilar system. Neurology 1999; 52: 980–3.
George B, Laurian C. Impairment of vertebral artery flow caused by extrinsic lesions. Neurosurgery 1989; 24: 206–14.
Citow JS, Macdonald RL. Posterior decompression of the vertebral artery narrowed by cervical osteophyte: case report. Surg Neurol 1999; 51: 495–8; discussion 498-9.
Sullivan HG, Harbison JW, Vines FS, Becker D. Embolic posterior cerebral artery occlusion secondary to spondylitic vertebral artery compression. Case report. J Neurosurg 1975; 43: 618–22.
Wright NM, Lauryssen C. Vertebral artery injury in C1-2 transarticular screw fixation: results of a survey of the AANS/CNS section on disorders of the spine and peripheral nerves. American Association of Neurological Surgeons/Congress of Neurological Surgeons. J Neurosurg 1998; 88: 634–40.
Tumialan LM, Wippold FJ 2nd, Morgan RA. Tortuous vertebral artery injury complicating anterior cervical spinal fusion in a symptomatic rheumatoid cervical spine. Spine 2004; 29: E343–8.
Manaouil C, Graser M, Delcour J, et al. Postoperative bilateral vertebral artery dissection: a case report. J Clin Forensic Med 2003; 10: 81–4.
Curylo LJ, Mason HC, Bohlman HH, Yoo JU. Tortuous course of the vertebral artery and anterior cervical decompression. A cadaveric and clinical case study. Spine 2000; 25: 2860–4.
Pollard ME, Little PW. Changes in carotid artery blood flow during anterior cervical spine surgery. Spine 2002; 27: 152–5.
Kernan WN, Viscoli CM, Inzucchi SE, et al. Prevalence of abnormal glucose tolerance following a transient ischemic attack or ischemic stroke. Arch Intern Med 2005; 165: 227–33.
Tanne D, Koren-Morag N, Goldbourt U. Fasting plasma glucose and risk of incident ischemic stroke or transient ischemic attacks. A prospective cohort study. Stroke 2004; 35: 2351–5.
Baird TA, Parsons MW, Phanh T,et al. Persistent poststroke hyperglycemia is independently associated with infarct expansion and worse clinical outcome. Stroke 2003; 34: 2208–14.
Wass CT, Lanier WL. Glucose modulation of ischemic brain injury: review and clinical recommendations. Mayo Clin Proc 1996; 71: 801–12.
Grundy BL, Jannetta PJ, Procopio PT, Lina A, Boston JR, Doyle E. Intraoperative monitoring of brain-stem auditory evoked potentials. J Neurosurg 1982; 57: 674–81.
Lam AM, Keane JF, Manninen PH. Monitoring of brainstem auditory evoked potentials during basilar artery occlusion in man. Br J Anaesth 1985; 57: 924–8.
Wijdicks EF, Rabinstein AA. Absolutely no hope? Some ambiguity of futility of care in devastating acute stroke. Crit Care Med 2004; 32: 2332–42.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tsai, YF., Doufas, A.G., Huang, CS. et al. Postoperative coma in a patient with complete basilar syndrome after anterior cervical discectomy. Can J Anesth 53, 202–207 (2006). https://doi.org/10.1007/BF03021828
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03021828