Abstract
Purpose: To describe the relative effects of graded central nervous system (CNS) depression, using increasing propofol infusion rates, on neurovegetative brainstem-mediated circulatory control mechanisms and higher cortical activity in healthy humans.
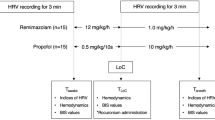
Methods: Propofol was administered using an infusion scheme designed to achieve three target blood concentrations in ten healthy volunteers. Blood propofol concentrations and sedation scores were determined at baseline, during the three propofol infusion levels, and 30 min into the recovery period. Electroencephalographic (EEG) power was measured in three frequency bands to quantify cortical activity, and autonomic heart rate control was quantified using spontaneous baroreflex assessment and power spectral analysis of pulse interval.
Results: Sedation scores dosely paralleled propofol blood concentrations (0, 0.53±0.34, 1.24±0.21, 3.11±0.80, and 0.96±0.42 µg·mL−1 at baseline, three infusion levels and recovery respectively), and all subjects were unconscious at the deepest level. Indices of autonomic heart rate control were decreased only at the deepest levels of CNS depression, while EEG effects were apparent at all propofol infusion rates. These EEG effects were frequency specific, with power in the beta band being affected at light levels of sedation, and alpha and delta power altered at deeper levels.
Conclusions: The results of this study support a relative preservation of neurovegetative circulatory control mechanisms during the early stages of CNS depression using gradually increasing rates of infusion of propofol. Indices of arculatory control did not reliably reflect depth of sedation.
Résumé
Objectif: Décrire les effets relatifs d’une dépression graduée du système nerveux central (SNC) sur les mécanismes d’origine centrale du contrôle neurovégétatif de la circulation, et l’activité corticale supérieure chez des humains sains, en utilisant des perfusions de propofol à vitesses croissantes.
Méthode: Le propofol a été administré, chez dix volontaires en santé, selon un schéma de perfusion conçu pour atteindre trois concentrations sanguines cibles. Les concentrations sanguines de propofol et les scores de sédation ont été déterminés au départ, pendant les trois régimes de perfusion de propofol et à 30 min pendant la récupération. La puissance électroencéphalographique (EEG) a été mesurée selon trois bandes fréquentielles pour quantifier l’activité corticale, et le contrôle autonome de la fréquence cardiaque a été mesuré à l’aide d’une évaluation bar oréflexe spontanée et de l’analyse spectrale de la puissance de l’intervalle pulsé.
Résultats: Les scores de sédation ont présenté un étroit parallélisme avec les concentrations sanguines de propofol (0; 0,53±0,34, 1,24±0,21; 3,11±0,80, et 0,96±0,42 µg·mL−1 au début, pendant les trois perfusions et la récupération, respectivement), et tous les sujets ont connu un profond sommeil. Les indices de contrôle autonome de la fréquence cardiaque ont diminué seulement au moment de la plus profonde dépression du SNC, tandis que les effets EEG ont été apparents pour toutes les vitesses de perfusion du propofol. Ces effets EEG différaient selon les fréquences, la puissance de la bande bêta étant affectée à de bas niveaux de sédation et les bandes alpha et delta étant modifiées à des niveaux plus profonds.
Conclusion: Les résultats de l’étude entretiennent une relative préservation des mécanismes de contrôle neurovégétatif de la circulation pendant les premiers stades de la dépression du SNC quand on utilise des vitesses de perfusion de propofol qui augmentent graduellement. Les indices de contrôle circulatoire ne reflètent pas fidèlement la profondeur de la sédation.
Article PDF
Similar content being viewed by others
References
Franks NP, Lieb WR Molecular and cellular mechanisms of general anaesthesia. Nature 1994; 367: 607–14.
Kearse LA Jr,Rosow C, Zaslavsky A, Connors P, Dershwitz M, Denman W. Bispectral analysis of the electroencephalogram predicts conscious processing of information during propofol sedation and hypnosis. Anesthesiology 1998; 88: 25–34.
Sneyd JR, Samra SK, Davidson B, Kishimoto T, Kadoya C, Domino EF. Electrophysiologic effects of propofol sedation. Anesth Analg 1994; 79: 1151–8.
Rocchiccioli C, Saad MAA, Elghozi J-L. Attenuation of the baroreceptor reflex by propofol anesthesia in the rat. J Cardiovasc Pharmacol 1989; 14: 631–5.
Cullen PM, Turtle M, Prys-Roberts C, Way WL, Dye J. Effect of propofol anesthesia on baroreflex activity in humans. Anesth Analg 1987; 66: 1115–20.
Kamijo Y, Goto H, Nakazawa K, Benson KT, Arakawa K. Arterial baroreflex attenuation during and after continuous propofol infusion. Can J Anaesth 1992; 39: 987–91.
Sellgren J, Ejnell H, Elam M, Pontén J, Wallin BG Sympathetic muscle nerve activity, peripheral blood flows, and baroreceptor reflexes in humans during propofol anesthesia and surgery. Anesthesiology 1994; 80: 534–44.
Robinson BJ, Ebert TJ, O’Brien TJ, Colinco MD, Muzi M. Mechanisms whereby propofol mediates peripheral vasodilation in humans. Sympathoinhibition or direct vascular relaxation? Anesthesiology 1997; 86: 64–72.
Krassioukov AV, Gelb AW, Weaver LC Action of propofol on central sympathetic mechanisms controlling blood pressure. Can J Anaesth 1993; 40: 761–9.
Imholz BPM, Settels JJ, van der Meiracker AH, Wesseling KH, Wieling W. Non-invasive continuous finger blood pressure measurement during orthostatic stress compared to intra-arterial pressure. Cardiovasc Res 1990; 24: 214–21.
Parati G, Casadei R, Groppelli A, Di Rienzo M, Mancia G Comparison of finger and intra-arterial blood pressure monitoring at rest and during laboratory testing. Hypertension 1989; 13: 647–55.
White M, Kenny GNC Intravenous propofol anaesthesia using a computerised infusion system. Anaesthesia 1990; 45: 204–9.
Skipsey IG, Colvin JR, MacKenzie N, Kenny GNC Sedation with propofol during surgery under local blockade. Assessment of a target-controlled infusion system. Anaesthesia 1993; 48: 210–3.
White PF. Propofol: pharmacokinetics and pharmacodynamics. Sem Anesth 1988; VII: 4–20.
Altmayer P, Büch U, Büch HP, Larsen R Rapid and sensitive pre-column extraction high-performance liquid chromatographic assay for propofol in biological fluids. J Chromatogr 1993; 612: 326–30.
Chernik DA, Gillings D, Laine H, et al. Validity and reliability of the Observer’s Assessment of Alertness/Sedation Scale: study with intravenous midazolam. J Clin Psychopharmacol 1990; 10: 244–51.
Bertinieri G, di Rienzo M, Cavallazzi A, Ferrari AU, Pedotti A, Mancia G A new approach to analysis of the arterial baroreflex. J Hypertension 1985; 3: S79-S81.
Blaber AP, Yamamoto Y, Hughson RL. Methodology of spontaneous baroreflex relationship assessed by surrogate data analysis. Am J Physiol 1995; 268: 1682–7.
Parlow JL, Viale J-P, Annat G, Hughson RL, Quintin L. Spontaneous cardiac baroreflex activity in humans. Comparison with drug-induced responses. Hypertension 1995; 25: 1058–68.
Yamamoto Y, Hughson RL. Coarse-graining spectral analysis: new method for studying heart rate variability. J Appl Physiol 1991; 71: 1143–50.
Smith I, Monk TG, White PF, Ding Y Propofol infusion during regional anesthesia: sedative, amnestic, and anxiolytic properties. Anesth Analg 1994; 79: 313–9.
Smith I, White PF, Nathanson M, Gouldson R Propofol. An update on its clinical use. Anesthesiology 1994; 81: 1005–43.
Dagnone AJ, Parlow JL. Effects of inhaled albuterol and ipratropium bromide on autonomic control of the cardiovascular system. Chest 1997; 111: 1514–8.
Dimier-David L, Billon N, Costagliola D, Jaillon P, Funck-Brentano C Reproducibility of non-invasive measurement and of short-term variability of blood pressure and heart rate in healthy volunteers. Br J Clin Pharmacol 1994; 38: 109–15.
Iellamo F, Legramante JM, Raimondi G, Castrucci F, Massaro M, Peruzzi G Evaluation of reproducibility of spontaneous baroreflex sensitivity at rest and during laboratory tests. J Hypertension 1996; 4: 1099–104.
Parlow JL, Bégou G, Sagnard P, et al. Cardiac baroreflex during the postoperative period in patients with hypertensive. Effect of clonidine. Anesthesiology 1999; 90: 681–92.
Akselrod S, Gordon D, Ubel FA, Shannon DC, Berger AC, Cohen RJ. Power spectrum analysis of heart rate fluctuation: a quantitative probe of beat-to-beat cardiovascular control. Science 1981; 213: 220–3.
Latson TW, McCarroll SM, Mirhej MS, Hyndman VA, Whitten CW, Lipton JM Effects of three anesthetic induction techniques on heart rate variability. J Clin Anesth 1992; 4: 265–76.
Pomeranz B, Macauley RJB, Caudill MA, et al. Assessment of autonomic function in humans by heart rate spectral analysis. Am J Physiol 1985; 248: H151-H153.
Ebert TJ, Muzi M, Berens R, Goff D, Kampine JP. Sympathetic responses to induction of anesthesia in humans with propofol or etomidate. Anesthesiology 1992; 76: 725–33.
Galletly DC, Corfiatis T, Westenberg AM, Robinson BJ. Heart rate periodicities during induction of propofol-nitrous oxide-isoflurane anaesthesia. Br J Anaesth 1992; 68: 360–4.
Howell SJ, Wanigasekera V, Young JD, Gavaghan D, Sear JW, Garrard CS. Effects of propofol and thiopentone, and benzodiazepine premedication on heart rate variability measured by spectral analysis. Br J Anaesth 1995; 74: 168–73.
Wang DY, Pomfrett CJD, Healy TEJ. Respiratory sinus arrhythmia: a new, objective sedation score. Br J Anaesth 1993; 71: 354–8.
Robinson BJ, Buyck HCE, Galletly DC Effect of propofol on heart rate, arterial pressure and digital plethysmograph variability. Br J Anaesth 1994; 73: 167–73.
Novak V, Novak P, De Champlain J, Le Blanc AR, Martin R, Nadeau R. Influence of respiration on heart rate and blood pressure fluctuations. J Appl Physiol 1993; 74: 617–26.
Rampil IJ. A primer for EEG signal processing in anesthesia. Anesthesiology 1998; 89: 980–1002.
Kearse LA Jr,Manberg P, DeBros F, Chamoun N, Sinai V. Bispectral analysis of the electroencephalogram during induction of anesthesia may predict hemodynamic responses to laryngoscopy and intubation. Electroencephalogr Clin Neurophysiol 1994; 90: 194–200.
Veselis RA, Reinsel RA, Wronski M, Marino P, Tong WP, Bedford RF. EEG and memory effects of low-dose infusions of propofol. Br J Anaesth 1992; 69: 246–54.
Seifert HA, Blouin RT, Conard PF, Gross JB. Sedative doses of propofol increase beta activity of the processed electroencephalogram. Anesth Analg 1993; 76: 976–8.
Veselis RA. The EEG as a monitor of sedation: encouraging progress. J Clin Anesth 1996; 8: S81-S87.
Author information
Authors and Affiliations
Corresponding author
Additional information
Financial support: Propofol blood concentrations funded by Zeneca Pharma Ltd.
Rights and permissions
About this article
Cite this article
Lafreniere, G., Milne, B., Brunet, D.G. et al. Autonomic circulatory and cerebrocortical responses during increasing depth of propofol sedation/hypnosis in humans. Can J Anaesth 47, 441–448 (2000). https://doi.org/10.1007/BF03018974
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03018974