Abstract
Purpose
To determine the effect of epidural anesthesia (EP) on oxygenation of the chronically ischemic limb in patients undergoing aorto-femoral bypass grafting and to assess whether it produces an alteration of lipid peroxidation and antioxidant status following revascularization.
Methods
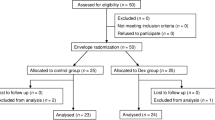
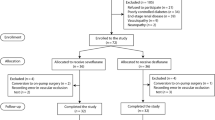
In this prospective, randomized, single-blinded study 40 ASA II or III patients undergoing elective aorto-femoral bypass grafting were allocated to receive general anesthesia (group GA,n = 20), or epidural + GA (group EP,n = 20) during surgery. Femoral venous blood-gas status, activities of the protecting antioxidant enzymes superoxide dismutase (SOD), glutathione peroxidase (GSH-px), glutathione reductase (GSH-rd), glutathione (GSH) and thiobarbituric acid-reactive substances (TBARS) as a marker of lipid peroxidation were determined in blood samples taken from the femoral vein at different intervals before and after revascularization.
Results
Before the induction of anesthesia in group EP, femoral venous PO2 [mean (standard deviation), 95% confidence interval] increased after achieving an adequate level of blockade by EP extending to the dermatomal level of T6-8 [29.32 (4.6), 26.34–32.30 to 36.29 (4.6), 33.37–39.22 mmHg,P < 0.05]. Femoral venous PO2 was similar in both groups thereafter. In the GA group a significant increase in erythrocyte TBARS was observed immediately after restoration of blood flow when compared with baseline values [221.32 (102), 148.35-294-29 to 337.26 (123) 248.99-425.53 nmol·g−1 hemoglobin,P < 0.01] but not at any other moment. In the EP group TBARS did not increase throughout the study. Within group comparisons revealed no significant differences in GSH, GSH-px, GSH-rd and SOD.
Conclusion
In patients with atherosclerotic aorto-iliac occlusive disease EP may possibly attenuate lipid peroxidation following revascularization but has no effect on antioxidant enzyme activities.
Résumé
Objectif
Déterminer l’effet de l’anesthésie péridurale (AP) sur l’oxygénation du membre soumis à l’ischémie chez les patients qui subissent un pontage aorto-fémoral et évaluer si elle produit une altération de la peroxydation lipidique et de l’état antioxydant à la suite de la revascularisation.
Méthode
Une étude prospective, randomisée et à simple insu a été menée auprès de 40 patients d’état physique ASA II ou III qui devaient subir un pontage aorto-fémoral sous anesthésie générale (groupe AG, n = 20) ou anesthésie péridurale + AG (groupe AP, n = 20). La gazométrie du sang veineux fémoral, les activités des enzymes protecteurs antioxydants superoxyde dismutase (SOD), glutathion peroxydase (GSH-px), glutathion réductase (GSH-rd), glutathion (GSH) et les substances réactives à l’acide thiobarbiturique (SRATB), comme marqueur de la peroxydation lipidique, ont été mesurés dans les échantillons sanguins prélevés de la veine fémorale à différents intervalles avant et après la revascularisation.
Résultats
Avant l’induction de l’AP, la PO2 veineuse fémorale [moyenne (écart type), intervalle de confiance de 95%] s’est élevée après le blocage péridural adéquat s’étendant au niveau du dermatome T6-8 [29,32 (4,6) 26,34-32,30 à 36,29 (4,6) 33,37-39,22 mmHg, P< 0,05]. La PO2 veineuse fémorale a été similaire dans les deux groupes par la suite. Dans le groupe AG, une hausse significative d’érythrocyte SRATB, en comparaison avec les valeurs de base, a été notée immédiatement et seulement après la restauration du débit sanguin [221,32 (102) 148,35-294-29 à 337,26 (123) 248,99-425,53 nmol·g−1 hémoglobine, P < 0,01]. Dans le groupe AP, les SRATB n’ont pas augmenté pendant l’étude. Aucune différence intragroupe significative de GSH, GSH-px, GSH-rd et SOD n’a été notée.
Conclusion
Chez les patients atteints d’occlusion aorto-iliaque, l’AP peut atténuer la peroxydation lipidique à la suite de la revascularisation, mais n’a pas d’effet sur les activités antioxydantes des enzymes.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Tuman KJ, Ivankovich AD. Pro: Regional anesthesia is better than general anesthesia for lower extremity revascularization. J Cardiothorac Vasc Anesth 1994; 8: 114–7.
Bode RH Jr, Lewis KP. Con: Regional anesthesia is not better than general anesthesia for lower extremity revascularization. J Cardiothorac Vasc Anesth 1994; 8: 118–21.
Tuman KJ, McCarthy RJ, March RJ, DeLaria GA, Patel RV, Ivankovich AD. Effects of epidural anesthesia and analgesia on coagulation and outcome after major vascular surgery. Anesth Analg 1991; 73: 696–704.
Bode RH Jr, Lewis KP, Zarich SW, et al. Cardiac outcome after peripheral vascular surgery. Comparison of general and regional anesthesia. Anesthesiology 1996; 184: 3–13.
Grace PA. Ischaemia-reperfusion injury. Br J Surg 1994; 81: 637–47.
Reilly PM, Schiller HJ, Bulkley GB. Pharmacologic approach to tissue injury mediated by free radicals and other reactive oxygen metabolites. Am J Surg 1991; 161: 488–503.
Baron JF, Bertrand M, Barre E, et al. Combined epidural and general anesthesia versus general anesthesia for abdominal aortic surgery. Anesthesiology 1991; 75:611–8.
Johnston WE, Balestrieri FJ, Plonk G, D’Souza V, Howard G. The influence of periaortic collateral vessels on the intraoperative hemodynamic effects of acute aortic occlusion in patients with aorto-occlusive disease or abdominal aortic aneurysm. Anesthesiology 1987; 66: 386–9.
Buege JA, Aust SD. Microsomal lipid peroxidation. Methods Enzymol 1978; 52: 302–10.
Sun Y, Oberley LW, Li Y. A simple method for clinical assay of superoxide dismutase. Clin Chem 1988; 34: 497–500.
Beutler E, Duran O, Kelly BM. Improved method for the determination of blood glutathione. J Lab Clin Med 1967; 61: 882–8.
Paglia DE, Valentine WN. Studies on the quantitative and qualitative characterization of erythrocyte glutathione peroxidase. J Lab Clin Med 1967; 70: 158–69.
Carlberg I, Mannervik B. Purification and characterization of the flavoenzyme glutathione reductase from rat liver. J Biol Chem 1975; 250: 5475–80.
Beyersdorf F, Unger A, Wildhirt A, et al. Studies of reperfusion injury in skeletal muscle: preserved cellular viability after extended periods of warm ischemia. J Cardiovasc Surg 1991; 32: 664–76.
Slater TF. Free-radical mechanisms in tissue injury. Biochem J 1984; 222: 1–15.
Cunningham AJ, O’Toole DP, McDonald N, Keeling F, Bouchier-Hayes D. The influence of collateral vascularisation on haemodynamic performance during abdominal aortic surgery. Can J Anaesth 1989; 36: 44–50.
Soong CV, Young IS, Blair PH, et al. Lipid peroxidation as a cause of lower limb swelling following femoropopliteal bypass grafting. Eur J Vasc Surg 1993; 7: 540–5.
Trewick AL, El-Hassan K, Round JM, Adiseshiah M. Xanthine oxidase in critically ischemic and claudicant limbs: profile of activity during early reperfusion. Br J Surg 1996; 83: 798–802.
Persson NH, Bergqvist D, Fex G, Marklund SL, Nilsson B, Takolander R. Lipid peroxidation and activity of antioxidant enzymes in muscle of the lower leg before and after arterial reconstruction. Eur J Vasc Surg 1989; 3: 399–403.
Neglen P, Jabs CM, Eklof B. Plasma metabolic disturbances and reperfusion injury following partial limb ischaemia in man. Eur J Vasc Surg 1989; 3: 165–72.
Wang WZ, Anderson G, Firrell JC, Tsai TM. Ischemic preconditioning versus intermittent reperfusion to improve blood flow to a vascular isolated skeletal muscle flap of rats. J Trauma 1998; 45: 953–9.
Korthuis RJ, Smith JK, Carden DL. Hypoxic reperfusion attenuates postischemic microvascular injury. Am J Physiol 1989; 256: H315–9.
Walker PM, Lindsay TF, Labbe R, Mickle DA, Romaschin AD. Salvage of skeletal muscle with free radical scavengers. J Vasc Surg 1987; 5: 68–75.
Perry MA, Wadhwa SS. Gradual reintroduction of oxygen reduces reperfusion injury in cat stomach. Am J Physiol 1988; 254: G366–72.
Rubin BB, Romaschin A, Walker PM, Gute DC, Korthuis R. Mechanisms of postischemic injury in skeletal muscle: intervention strategies. J Appl Physiol 1996; 80: 369–87.
Ihnken K, Beyersdorf F, Winkelmann B, Unkelbach U. Reperfusion syndrome in skeletal muscle after prolonged incomplete ischemia: reduction by controlled limb reperfusion. Transplant Proc 1995; 27: 2806–8.
Piriou V, Chiari P, Lhuillier F, et al. Pharmacological preconditioning: comparison of desflurane, sevoflurane, isoflurane and halothane in rabbit myocardium. Br J Anaesth 2002; 89: 486–91.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yüceyar, L., Erolçay, H., Konukoglu, D. et al. Epidural anesthesia may attenuate lipid peroxidation during aorto-femoral surgery. Can J Anesth 51, 465–471 (2004). https://doi.org/10.1007/BF03018309
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03018309