Abstract
Purpose
One hundred percent O2 is used routinely for preoxy-genation and induction of anesthesia. The higher the O2 concentration the faster is the development of atelectasis, an important cause of impaired pulmonary gas exchange during general anesthesia (GA). We evaluated the effect of ventilation with 0.4FiO2 in air, 0.4FiO2 in N2O and 100% O2 following intubation on the development of impaired gas exchange.
Methods
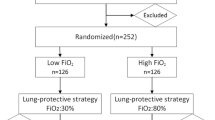
Twenty-seven patients aged 18–40 yr, undergoing elective laparoscopic cholecystectomy were administered 100% O2 for preoxygenation (three minutes) and ventilation by mask (two minutes). Following intubation these patients were randomly divided into three groups of nine each and ventilated either with 0.4FiO2 in air, 0.4FiO2 in N2O or 100% O2. Arterial blood gases were obtained before preoxygenation and 30 min following intubation for PaO2 analysis. Subsequently PaO2/FiO2 ratios were calculated. Results were analyzed with Student’s t test and one-way ANOVA. P value of ≤ 0.05 was considered significant.
Results
Ventilation of the lungs with O2 in air (FiO2 0.4) significantly improved the PaO2/FiO2 ratio from baseline, while 0.4FiO2 in N2O or 100% O2 worsened the ratio (558 ± 47vs 472 ± 28, 365 ± 34vs 472 ± 22 and 351 ± 23 vs 477 ± 28 respectively; P < 0.05).
Conclusion
Ventilation of lungs with O2 in air (FiO2 0.4) improves gas exchange in young healthy patients during GA.
Résumé
Objectif
Cent pour cent d’O2 sont utilisés habituellement pour la préoxygénation et l’induction de l’anesthésie. Plus la concentration d’O2 est élevée, plus vite peut se développer l’atélectasie, une cause importante d’anomalie des échanges gazeux pulmonaires pendant l’anesthésie générale (AG). Nous avons évalué l’effet de la ventilation avec uneFiO2 de 0,4 dans de l’air,FiO2 de 0,4 dans du N2O et 100 % d’O2 après l’intubation quand apparaissent les anomalie des échanges gazeux.
Méthode
Vingt-sept patients de 18–40 ans, devant subir une cholé-cystectomie laparoscopique non urgente ont reçu 100 % d’O2 pour la préoxygénation, pendant trois minutes, et la ventilation au masque, pendant deux minutes. Après l’intubation, ces patients ont été répartis de façon aléatoire en trois groupes de neuf et ventilés avec 0,4FiO2 dans de l’air ou 0,4FiO2 dans du N2O ou 100% d’O2. La gazométrie du sang artériel a été obtenue pendant la préoxygénation et 30 min après l’intubation pour l’analyse de la PaO2. Par la suite, les ratios PaO2/FiO2 ont été calculés. Les résultats ont été analysés selon le test t de Student et une analyse de variance à une voie. Une valeur de P ≤ 0,05 a été considérée comme significative.
Résultats
La ventilation pulmonaire avec de l’O2 dans de l’air (FiO2 de 0,4) a sensiblement amélioré le ratio PaO2/FiO2, comparativement aux données de base, tandis que 0,4FiO2 dans du N2O ou 100 % d’O2 l’ont altéré (558 ± 47vs 472 ± 28, 365 ± 34 vs 472 ± 22 et 351 ± 23 vs 477 ± 28 respectivement; P < 0,05).
Conclusion
La ventilation pulmonaire avec de l’O2 dans de l’air (FiO2 0,4) améliore les échanges gazeux chez les jeunes patients pendant l’AG.
Article PDF
Similar content being viewed by others
References
Strandberg A, Tokics L, Brismar B, Lundquist H, Hedenstierna G. Atelectasis during anaesthesia and in the postoperative period. Acta Anaesthesiol Scand 1986; 30: 154–8.
Cote CJ, Goldstein EA, Cote MA, Hoaglin DC, Ryan JF. A single-blind study of pulse oximetry in children. Anesthesiology 1988; 68: 184–8.
Moller JT, Johannessen NW, Berg H, Espersen K, Larsen LE. Hypoxaemia during anaesthesia-an observer study. Br J Anaesth 1991; 66: 437–44.
Videira RL, Neto PP, do Amaral RV, Freeman JA. Preoxygenation in children: for how long? Acta Anaesthesiol Scand 1992; 36: 109–11.
Pedersen T, Viby-Mogensen J, Ringsted C. Anaesthetic practice and postoperative pulmonary complications. Acta Anaesthesiol Scand 1992; 36: 812–8.
Hedenstierna G, Edmark L, Aherdan KK. Time to reconsider the pre-oxygenation during induction of anaesthesia. Minerva Anestesiol 2000; 66: 293–6.
Rothen HU, Sporre B, Engberg G, Wegenius G, Reber A, Hedenstierna G. Prevention of atelectasis during general anaesthesia. Lancet 1995; 345: 1387–91.
Rothen HU, Sporre B, Engberg G, Wegenius G, Hedenstierna G. Re-expansion of atelectasis during general anaesthesia: a computed tomography study. Br J Anaesth 1993; 71: 788–95.
Shambaugh GE, Harrison WG, Farrell JI. Treatment of respiratory paralysis of poliomyelitis in respiratory chamber. JAMA 1930; 94: 1371–3.
Marino PL. Hypoxia and hypercarbia.In: Zinner SR (Ed.). The ICU Book, 2nd ed. Baltimore: Williams & Wilkins, 1998: 339–54.
Hedenstierna G, Strandberg A, Brismar B, Lundquist H, Svensson L, Tokics L. Functional residual capacity, thoracoabdominal dimensions, and central blood volume during general anesthesia with muscle paralysis and mechanical ventilation. Anesthesiology 1985; 62: 247–54.
Krayer S, Rehder K, Vettermann J, Didier EP, Ritman EL. Position and motion of the human diaphragm during anesthesia-paralysis. Anesthesiology 1989; 70: 891–8.
Klineberg PL, Rehder K, Hyatt RE. Pulmonary mechanics and gas exchange in seated normal men with chest restriction. J Appl Physiol 1981; 51: 26–32.
Rothen HU, Sporre B, Engberg G, Wegenius G, Hogman M, Hedenstierna G. Influence of gas composition on recurrence of atelectasis after a reexpansion maneuver during general anesthesia. Anesthesiology 1995; 82: 832–42.
Joyce CJ, Baker AB, Kennedy RR. Gas uptake from an unventilated area of lung: computer model of absorption atelectasis. J Appl Physiol 1993; 74: 1107–16.
Webb SJ, Nunn JF. A comparison between the effect of nitrous oxide and nitrogen on arterial PO2. Anaesthesia 1967; 22: 69–81.
Tokics L, Hedenstierna G, Brismar B, Strandberg A, Lundquist H. Thoracoabdominal restriction in supine men: CT and lung function measurements. J Appl Physiol 1988; 64: 599–604.
Nunn JF, Williams IP, Jones JG, Hewlett AM, Hulands GH, Minty BD. Detection and reversal of pulmonary absorption collapse. Br J Anaesth 1978; 50: 91–100.
Baker AB, McGinn A, Joyce C. Effect on lung volumes of oxygen concentration when breathing is restricted. Br J Anaesth 1993; 70: 259–66.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Agarwal, A., Singh, P.K., Dhiraj, S. et al. Oxygen in air (FiO2 0.4) improves gas exchange in young healthy patients during general anesthesia. Can J Anesth 49, 1040–1043 (2002). https://doi.org/10.1007/BF03017898
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03017898