Abstract
Purpose
To determine whether inclusion of a neutrophil-specific filter into the extracorporeal circuit during open heart valve surgery alters postoperative outcomes.
Methods
Convenience sampling of 24 patients undergoing elective open heart valve surgery between July 1993 and June 1994. Patients were randomized to a neutrophil-specific filter (n= 11) or to a standard blood filter (n= 13) during cardiopulmonary bypass.
Results
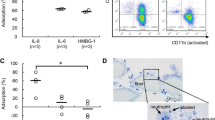
Neutrophil-specific filter diminished (P < 0.02) the expression of CD 18, a neutrophil surface adhesion molecule, at 1 (84.5 ± 4.2 vs 94.8 ± 3.8%). 4 (80.0 ± 4.2 vs 95.1 ± 3.9%) and 24 hr (75.2 ± 4.2 vs 98.2 ±3.9%) post-operatively compared with standard filter. Total white blood cell count, neutrophil count, and proinflammatory cytokmes (IL-6, IL-8) were similar between groups at all times. Measured outcomes including: PaO2, cardiac index, ejection fraction, haemodynamic variables, use of motropes, spirometry (FEV FVC). and hospitalization duration were similar between groups.
Conclusions
Inclusion of the neutrophil filter during open heart valve surgery selectively depletes activated neutrophils. There were no other detectable differences between the two groups and the use of a neutrophilspecific filter in routine clinical practice for patients undergoing open heart valve surgery is not supported.
Résumé
Objectif
Déterminer si l’ajout au circuit extracorporel d’un filtre spécifique aux neutrophiles pendant une chirurgie valvulaire modifiait les résultats de l’intervention
Méthodes
Un échantillonnage de 24 patients subissant une intervention valvulaire à coeur ouvert entre juillet 1993 et juin 1994. Les patients ont été répartis aléatoirement à un circuit extracorporel incluant un filtre spécifique aux neutrophiles (n= 11) ou un filtre standard (n= 13).
Résultats
Le filtre spécifique aux neutrophiles a diminué l’expression de CD 18. une molécule adhésive de sur face, une heure (84.5 ± 4.2 vs 98.8 ± 3.8%), quatre heures (80 ± 4,2 vs 95.1 ± 3,9%) et 24 heures (75.2 ± 4,2 vs 98.2 ± 3.9%) après l’opération comparativement au filtre standard. Le décompte total des globules blancs, des neutrophiles et des cytokines pro-inflammatoires (IL-6. IL8) étaient à tous les moments identiques entre les groupes. Les mesures de résultats incluant la PaO2, l’index cardiaque, la fraction d’éjection, les données hémodynamiques, l’utilisation d’inotropes, la spirométne (VEMS, CVF) et la durée du séjour hospitalier étaient identiques entre les groupes.
Conclusion
L’ajout d’un filtre spécifique aux neutrophiles pendant la chirurgie à coeur ouvert épuise sélectivement les neutrophiles activés. Aucune autre différence n’est discernable entre les groupes. L’utilisation courante de filtres spécifiques aux neutrophiles en clinique chez des patients soumis à une chirurgie valvulaire à coeur ouvert n’est pas justifiée.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Abbreviations
- CABG:
-
coronary artery bypass graft
- CPB:
-
cardiopulmonary bypass
- IL-6:
-
interleukin 6
- IL-8:
-
interleukin 8
- PSA :
-
systemic arterial pressure
- PRA :
-
right atrial pressure
- PPA :
-
pulmonary artery pressure
- PCWP :
-
pulmonary capillary wedge pressure
- CI:
-
cardiac index
- WBC:
-
white blood cell count
- IL-6SR:
-
interleukin 6 soluble receptor
- FAS:
-
fractional shortening
- EF:
-
ejection fraction
- A-aDO2 :
-
aveolar to arterial difference for oxygen
- Qs/Qt:
-
intrapulmonary shunt
References
Kirklin JK, Blackstone EH, Kirklin JW. Cardiopulmonary bypass: studies on its damaging effects. Blood Purif 1987; 5: 168–78.
Westaby S. Organ dysfunction after cardiopulmonary bypass. A systemic inflammatory reaction initiated by the extracorporeal circuit. Intensive Care Med 1987; 13: 89–95.
Downing SW, Edmunds LH Jr. Release of vasoactive substances during cardiopulmonary bypass. Ann Thorac Surg 1992; 54: 1236–43.
Finkel MS, Hoffman RA, Shen L, Oddis CV, Simmons RL, Hattler BG. Interleukin-6 (IL-6) as a mediator of stunned myocardium. Am J Cardiol 1993; 71: 1231–2.
Finn A, Naik S, Klein N, Levinsky RJ, Strobel S, Elliott M. Interleukin-8 release and neutrophil degranulation after pediatric cardiopulmonary bypass. J Thorac Cardiovasc Surg 1993; 105: 234–41.
Ratliff NB, Young WG Jr, Hackel DB, Mikat E, Wilson JW. Pulmonary injury secondary to extracorporeal circulation. An ultrastructural study. J Thorac Cardiovasc Surg 1973; 65: 425–32.
Genco CM, Connolly RJ, Peterson MB, et al. Granulocyte sequestration and early failure in the autoperfused heart-lung preparation. Ann Thorac Surg 1992; 53: 217–26.
Myers ML, Webb C, Moffat M, McIver D, Del Maestro R. Activated neutrophils impair rabbit heart recovery after hypothermic global ischemia. Ann Thorac Surg 1992; 53: 247–52.
Litt MR, Jeremy RW, Weisman HF, Winkelstein JA, Becker LC. Neutrophil depletion limited to reperfusion reduces myocardial infarct size after 90 minutes of ischemia. Evidence for neutrophil-mediated reperfusion injury. Circulation 1989; 80: 1816–27.
Johnson D, Thomson D, Mycyk T, Burbridge B, Mayers I. Depletion of neutrophils by filter during aortocoronary bypass surgery transiently improves postoperative cardiorespiratory status. Chest 1995; 107: 1253–9.
Mazer CD, Byrick RJ, Sibbald WJ, et al. Postoperative utilization of critical care services by cardiac surgery: a multicentre study in the Canadian healthcare system. Crit Care Med 1993; 21: 851–9.
Tuman KJ, McCarthy RJ, March RJ, Najafi H, Ivankovich AD. Morbidity and duration of ICU stay after cardiac surgery. A model for preoperative risk assessment. Chest 1992; 102: 36–44.
Proudfit WL. Grading angina pectoris: comment on the Canadian System (Editorial). Can J Cardiol 1986; 2: 62–3.
Teichholz LE, Kreulen T, Herman MV, Gorlin R. Problems in echocardiographic volume determinations: echocardiographic-angiographic correlations in the presence or absence of asynergy. Am J Cardiol 1976; 37: 7–11.
Johnson D, Thomson D, Hurst T, et al. Neutrophilmediated acute lung injury after extracorporeal perfusion. J Thorac Cardiovasc Surg 1994; 107: 1193–202.
Palanzo DA, Manley NJ, Montesano RM, Yeisley GL, Gordon D. Clinical evaluation of the LeukoGuard (LG-6) arterial line filter for routine open-heart surgery. Perfusion 1993; 8: 489–96.
Gu YJ, deVries AJ, Boonstra PW, van Oeveren W. Leukocyte depletion results in improved lung function and reduced inflammatory response after cardiac surgery. J Thorac Cardiovasc Surg 1996; 112: 494–500.
Rinder CS, Rinder HM, Smith BR, et al. Blockade of C5a and C5b-9 generation inhibits leukocyte and platelet activation during extracorporeal circulation. J Clin Invest 1995; 96: 1564–72.
Chenoweth DE, Cooper SW, Hugli TE, et al. Complement activation during cardiopulmonary bypass. N Eng J Med 1981; 304: 497–503.
Schmid-Schonbein GW. Capillary plugging by granulocytes and the no-reflovv phenomenon in the microcirculation. Federation Proceedings 1987; 46: 2397–401.
Bando K, Pillai R, Cameron DE, et al. Leukocyte depletion ameliorates free radical-mediated lung injury after cardiopulmonary bypass. J Thorac Cardiovasc Surg 1990; 99: 873–7.
Davies GG, Wells DG, Mabee TM, Sadler R, Melling NJ. Platelet-leukocyte plasmapheresis attenuates the deleterious effects of cardiopulmonary bypass. Ann Thorac Surg 1992; 53: 274–7.
Breda MA, Drinkwater DC, Laks H, et al. Prevention of reperfusion injury in the neonatal heart with leukocyte-depleted blood. J Thorac Cardiovasc Surg 1989; 97: 654–65.
Bryne JG, Appleyard RF, Lee CC, et al. Controlled reperfusion of the regionally ischémic myocardium with leukocyte-depleted blood reduces stunning, the no-reflow phenomenon, and infarct size. J Thorac Cardiovasc Surg 1992; 103: 66–72.
MacNee W, Selby C. Neutrophil traffic in the lungs: role of haemodynamics, cell adhesion, and deformability. Thorax 1993; 48: 79–88.
Arnaout MA. Structure and function of the leukocyte adhesion molecules CD11/CD18. Blood 1990; 75: 1037–50.
Mileksi WJ, Winn RK, Vedder NB, Pohlman TH, Harlan JM, Rice CL. Inhibition of CD 18-dependent neutrophil adherence reduces organ injury after hemorrhagic shock in primates. Surgery 1990; 108: 206–12.
Mulligan MS, Polley MJ, Bayer RJ, Nunn MF, Paulson JC, Ward PA. Neutrophil-dependent acute lung injury. Requirement for P-selectin (GMP-140). J Clin Invest 1992; 90: 1600–7.
Dreyer WJ, Michael LH, Millman EE, Berens KL. Neutrophil activation and adhesion molecule expression in a canine model of open heart surgery with cardiopulmonary bypass. Cardiovasc Res 1995; 29: 775–81.
Wilson I, Gillinov AM, Curtis WE, et al. Inhibition of neutrophil adherence improves postischemic ventricular performance of the neonatal heart. Circulation. 1993; 88 Part II: 372–9.
Buttrum SM, Drost EM, MacNee W, et al. Rheological response of neutrophils to different types of stimulation. J Appl Physiol 1994;77: 1801–10.
Müllberg J, Schooltink H, Stoyan T, et al. The soluble interleukin-6 receptor is generated by shedding. Eur J Immunol 1993; 23: 473–80.
Johnson D, Kelm C, To T, et al. Postoperative physical therapy after coronary artery bypass surgery. Am J Respir Crit Care Med 1995; 152: 953–8.
Gorcsan J III, Diana P, Lee J, Katz WE, Hattler BG. Reversible diastolic dysfunction after successful coronary artery bypass surgery. Assessment by transesophageal Doppler echocardiography. Chest 1994; 106: 1364–9.
Tuman KJ, McCarthy RJ, Spiess BD, DaValle M, Dabir R, Ivankovich AD. Does choice of anesthetic agent significantly affect outcome after coronary artery surgery? Anesthesiology 1989; 70: 189–98.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hurst, T., Johnson, D., Cujcc, B. et al. Depletion of activated neutrophils by a filter during cardiac valve surgery. Can J Anaesth 44, 131–139 (1997). https://doi.org/10.1007/BF03013000
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03013000