Abstract
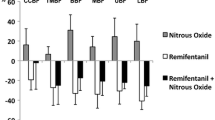
The effect of nitrous oxide (N2O) on ischaemic myocardium was investigated in the presence of beta-receptor blockade. Three anaesthetics were compared in each of six dogs: isoflurane 1.8% alone, isoflurane 1.4% with 50% N2O, and isoflurane 1.8% with 50% N2O. Heart rate (HR), systolic aortic blood pressure (SBP), and left atrial pressure (LAP) were held constant during the three treatments. The left anterior descending coronary artery (LAD) was cannulated and perfused with an autoperfusion circuit. Systolic segment length was measured with a sonomicrometer in the LAD and circumflex regions. Regional myocardial blood flow was measured using radioactive microspheres. Propranolol was administered intravenously and then measurements were made during imposition of a stenosis on the perfusion circuit sufficient to decrease systolic shortening by 30%. The substitution of 50% N2O for 0.4% isoflurane had no effect on systolic shortening or transmural myocardial blood flow in the ischaemic or normal region. When N2O was added to 1.8% isoflurane, systolic shortening decreased by 34.6% in the ischaemic and 57.3% in the normally perfused region, while transmural myocardial blood flow distribution did not change significantly. The decrease in shortening was therefore not due to increased ischaemia. These results were similar to those of a previous experiment which was identical except that beta-blockade was absent. It is concluded that beta-receptor blockade does not markedly alter the response of normal or ischaemic myocardium to N2O.
Résumé
L’ejfet du protoxyde d’azote (N2O) sur le myocarde ischémique a été investigué en présence d’un bloc des récepteurs beta. Six chiens ont été étudiés et trois anesthesiques out été comparés chez chacun: l’isoflurane 1.8% seul, l’isoflurane 1.4% avec N2O 50%, et iisoflurane 1.8% avec N2O 50%. Le rythme cardiaque (HR), la tension arterielle systolique aortique (SBP), et la tension de l’oreillette gauche (LAP) ont été maintenus constants durant les trois traitements. L’artère coronaire antérieure descendante gauche (LAD) a été cannulée etperfusée à l’aide d’un circuit à autoperfusion. La longueur du segment systolique a été mesurée a l’aide d’un sonomicromètre pour la LAD et les régions de la circonflexe. Le débit sanguin myocardique régional a été mesuré à l’aide de microsphères radioactives. Suite à l’administration intraveineuse de propranolol, des mesures ont été prises pendant la création d’une sténose, au niveau du circuit de perfusion, suffisante pour diminuer le raccourcissement systolique de 30%. La substitution du N2O 50% par de l’isoflurane 0.4% n’a eu aucun effet sur le raccourcissement systolique ou le débit sanguin myocardique transmural dans les régions ischémiques ou normales. Lorsque le N2O était ajouté a l’isoflurane 1.8%, le raccourcissement systolique diminuait de 34.6% dans les régions ischémiques et de 57.3% dans les régions normalement perfusées, tandis que la distribution du debit sanguin myocardique transmural n’a pas changé de façon significative. La diminution du raccourcissement n’était done pas due à une augmentation de l’ischémie. Ces résultats étaient semblables à ceux d’une expérience précédente, qui était identique à l’exception de l’absence de bloc beta. Nous concluons que le bloc des récepteurs beta n’altère pas de façon marquée la réponse du myocarde normal ou ischémique au N2O.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Nathan HJ. Nitrous oxide worsens myocardial ischemia in isoflurane anesthetized dogs. Anesthesiology 1988; 68: 407–15.
Nathan HJ. Control of hemodynamics prevents worsening of myocardial ischemia when nitrous oxide is administered to isoflurane-anesthetized dogs. Anesthesiology 1989; 71: 686–94.
Dolan WM, Stevens WC, Eger EI et al. The cardiovascular and respiratory effects of isoflurane nitrous oxide anesthesia. Can Anaesth Soc J 1974; 21: 557–68.
Smith NT, Eger EI, Stoelting RK, Whayne TF, Cullen D, Kadis IB. The cardiovascular and sympathomimetic responses to the addition of nitrous oxide to halothane in man. Anesthesiology 1970; 32: 410–21.
Stoelting RK, Reis RR, Longnecker DE. Hemodynamic responses to nitrous oxide halothane and halothane in patients with valvular heart disease. Anesthesiology 1972; 37: 430–5.
Robotham JL, Stuart RS, Doherty K, Borkon AM, Baumgartner W. Mitral and aortic blood flows during spontaneous respiration in dogs. Anesthesiology 1988; 69: 516–26.
Heymann MA, Payne BD, Hoffman JIE, Rudolph AM. Blood flow measurement with radionuclidc labeled particles. Prog Cardiovasc Dis 1977; 20: 55–79.
Theroux P, Franklin D, Ross J Jr,Kemper WS. Regional myocardial function during acute coronary artery occlusion and its modification by pharmacologic agents in the dog. Circ Res 1974; 35: 896–908.
Dolezel S, Gerova MB, Hartmannova B, Dostal M, Janeckova H, Vasku J. Cardiac adrenergic innervation after instrumentation of the coronary artery in the dog. Am J Physiol 1984; 246: H459–65.
Roth DM, White FC, Mathieu-Costello O et al. Effects of left circumflex amcroid constrictor placement on adrenergic innervation of myocardium. Am J Physiol 1987; 253: H1425–34.
Wilkowski DA, Sill JC, Bonta W, Owen R, Bove AA. Nitrous oxide constricts cpicardial coronary arteries without effect on coronary arteriolcs. Anesthesiology 1987; 66: 659–65.
Brown BG, Lee AB, Bolson EL, Dodge HT. Reflex constriction of significant coronary stenosis as a mechanism contributing to ischemic left ventricular dysfunction during isometric exercise. Circulation 1984; 70: 18–24.
Dottori O, Haggendal E, Linder E, Nordstrom G, Seeman T. The hemodynamic effect of nitrous oxide anesthesia on myocardial blood flow in dogs. Acta Anaesthisiol Scand 1976; 20: 421–8.
Thorburn J, Smith G, Vance JP, Brown DM. Effect of nitrous oxide on the cardiovascular system and coronary circulation of the dog. Br J Anaesth 1979; 51: 937–42.
Cahalan MK, Prakash O, Rulf ENR et al. Addition of nitrous oxide to fentanyl anesthesia does not induce myocardial ischemia in patients with ischemic heart disease. Anesthesiology 1987; 67: 925–9.
Slavik JR, LaMantia KR, Kopriva CJ, Prokop E, Ezekowitz MD, Barash PG. Docs nitrous oxide cause regional wall motion abnormalities in patients with coronary artery disease? Anesth Analg 1988; 67: 695–700.
Mitchell MM, Prakash O, Rulf EN, van Daele ME, Cahalan MK, Roelandt JR. Nitrous oxide does not induce myocardial ischemia in patients with ischemic heart disease and poor ventricular function. Anesthesiology 1989; 71: 526–34.
Author information
Authors and Affiliations
Additional information
Supported by an operating grant from the Heart and Stroke Foundation of Ontario and a Career Scientist Award from the Ontario Ministry of Health.
Rights and permissions
About this article
Cite this article
Nathan, H.J. Nitrous oxide does not worsen myocardial ischaemia following beta-receptor blockade in isoflurane anaesthetized dogs. Can J Anaesth 38, 640–647 (1991). https://doi.org/10.1007/BF03008202
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03008202