Abstract
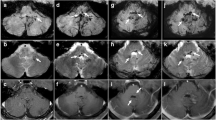
A 7-year-old boy developed mutism after surgery for cerebellar medulloblastoma. Postoperative magnetic resonance imaging (MRI) whowed atrophy of the cerebellar vermis and both cerebellar hemispheres, predominantly on the right side. Single photon emission computed tomography (SPECT) with technetium-99m-ethyl cysteinate dimer (Tc-99m ECD) revealed decreased cerebral blood flow (CBF) in the bilateral thalami, bilateral medial frontal lobes, and left temporal lobe in addition to the cerebellar vermis and both cerebellar hemispheres when mutism was manifest, indicating the existence of bilateral crossed cerebello-cerebral diaschisis (BCCCD). Circulatory disturbance in both cerebellar hemispheres secondary to tumor resection probably caused BCCCD in both cerebral hemispheres, predominantly in the left, via the dentatothalamocortical pathway (DTCP). With recovery of his mutism, CBF increased in the right thalamus, bilateral medial frontal lobes and left temporal lobe. Thus BCCCD was improved, with only a slight decrease in CBF still persisting in the left thalamus. The mechanism of mutism may have involved damage to the cerebellar vermis (the site of incision at operation), the left dentate nucleus (heavily infiltrated by the tumor) and the right dentate nucleus of the cerebellum (affected by circulatory disturbance secondary to acute postoperative edema). The SPECT findings suggested that mutism was associated with BCCCD-induced cerebral circulatory and metabolic hypofunction in the supplementary motor area mediated via the DTCP.
Similar content being viewed by others
References
Benson DF.Aphasia, Alexia, and Agraphia. New York: Churchill Livingstone, 1979: 163–164.
Martins IP, Ferro JM. Recovery of Acquired aphasia in children.Aphasiology 1992; 6: 431–438.
David AS, Bone I. Mutism following left hemisphere infarction.J Neurol Neurosurg Psychiatry 1984; 47: 1342–1344.
Arseni C, Botez MI. Speech disturbances caused by tumors of supplementary motor area.Acta Psychiatr Neurol Scand 1986; 36: 279–299.
Peled R, Harnes B, Borovich B, Sharf B. Speech arrest and supplementary motor area seizures.Neurology 1984; 34: 110–111.
Rostomily RC, Berger MS, Ojemann GA, Lettich E. Postoperative deficits and functional recovery following removal of tumors involving the dominant hemisphere supplementary motor area.J Neurosurg 1991; 75: 62–68.
Watson RT, Fleet WS, Gonzalez-Rothi L, Heilman KM. Apraxia and the supplementary motor area.Arch Neurol 1986; 43: 787–792.
Krayenbühl H, Wyss OAM, Yasargil MG. Bilateral thalamotomy and pallidotomy as treatment for bilateral parkinsonism.J Neurosurg 1961; 18: 429–444.
Levin HS, Madison CF, Bailey CB, Meyers CA, Eisenberg HM, Guinto FC. Mutism after closed head injury.Arch Neurol 1983; 40: 601–606.
Sakai H, Sekino H, Nakamura N. Three cases of “cerebellar mutism.”Shinkeinaika 1980; 12: 302–304.
Dailey AT, Mckhann II GM, Berger MS. The pathophysiology of oral pharyngeal apraxia and mutism following posterior fossa tumor resection in children.J Neurosurg 1995; 83: 467–475.
Pollack IF, Polinko P, Albright AL, Towbin R, Fitz C. Mutism and pseudobulbar symptoms after resection of posterior fossa tumors in children: Incidence and pathophysiology.Neurosurgery 1995; 37:885–893.
Kawanishi A, Hirahara K, Shimozuru T, Makiuchi T, Kawasaki T, Kawahara T, et al. Ependymoma in the fourth ventricle; a report of four cases and a discussion of cerebellar mutism.Neurvous System in Children 1994; 9: 379–384.
Endo K, Yoshii Y, Tsuboi K, Saito A, Aoki K, Nose T. Transient cerebellar mutism after removal of a posterior fossa tumor in two cases.No shinkei Geka 1995; 23: 509–513.
Ichinose M, Abe M, Hirotsu T, Tabuchi K. Sequential SPECT analysis of cerebellar mutism after removal of medulloblastoma: a case report.Jpn J Neurosurg (Tokyo) 1997; 6: 493–497.
Crutchfield JS, Sawaya R, Meyers CA, Moore BD III. Postoperative mutism in neurosurgery: Report of two cases.J Neurosurg 1994; 81: 115–121.
Erşahin Y, Mutluer S, Çaĝli S, Duman Y. Cerebellar mutism: report of seven cases and review of the literature.Neurosurgery 1996; 38: 60–66.
Germanó A, Baldari S, Caruso G, Caffo M, Montemagno G, Cardia E, et al. Reversible cerebral perfusion alterations in children with transient mutism after posterior fossa surgery.Child’s Nerv Syst 1998; 14: 114–119.
Suma T, Makiyama Y, Nishimoto H. A case of cerebellar mutism after medulloblastoma surgery.Nervous System in Children 1996; 21: 247–251.
Broich K, Hartomann A, Biersack HJ, Horn R. Crossed cerebello-cerebral diaschisis in a patient with cerebellar infarction.Neurosci Lett 1987; 83: 7–12.
Rousseaux M, Steinling M. Remote regional cerebral blood flow consequences of focused infarcts of the medulla, pons and cerebellum.J Nucl Med 1999; 40: 721–729.
Hausen HS, Lachmann EA, Nagler W. Cerebral diaschisis following cerebellar hemorrhage.Arch Phys Med Rehabil 1997; 78: 546–549.
Penfield W, Welch K. The supplementary motor area of the cerebral cortex. A clincal and experimental study.Arch Neurol Psychiatry 1951; 66: 289–317.
Larsen B, Skinhoj E, Lassen NA. Variations in regional cortical blood flow in the right and left hemispheres during automatic speech.Brain 1978; 101: 193–209.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Sagiuchi, T., Ishii, K., Aoki, Y. et al. Bilateral crossed cerebello-cerebral diaschisis and mutism after surgery for cerebellar medulloblastoma. Ann Nucl Med 15, 157–160 (2001). https://doi.org/10.1007/BF02988609
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02988609