Summary
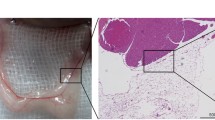
Hypercalcemia causes acute pancreatitis in humans, a phenomenon reproduced experimentally in cats and guinea pigs. Because the rat is the most frequently used animal for the study of experimental pancreatitis, the present studies were performed to evaluate the effects of hypercalcemia in the rat In in vitro studies, pancreatic lobules were prepared from fasted Wistar rats (200–250 g) and incubated in HEPES bicarbonate-buffered medium (pH 7.4) containing 0, 0.6, 1.2, 2.5, 5, and 10 mM CaCL2 with or without carbachol l0-6M. Amylase was measured in the medium after 30 min to 3 h, and expressed as percent of total amylase. In in vivo studies, fasted male Wistar rats (300-400 g) received calcium (CaCl2; 0.6 mmol/kgh) into the tail vein for 12 h. Control animals received NaCl 0.9% infusion. Histologic slides (H&E-stained) were evaluated in a blinded fashion. Pancreatic lobules showed a higher basal amylase output when incubated in higher calcium medium. The largest, significant difference (2.6-fold) was between 0.6 and 5 mM medium CaCl2 (p < 0.05). Carbachol-stimulated amylase release was again higher with increasing medium calcium with the most pronounced difference (1.3-fold) between 0.6 and 2.5 mM CaCl2, (p < 0.05). In vivo calcium-treated animals showed accumulation of zymogen granules in the cytoplasm, cytoplasmic vacuolization, focal acinar cell depolarization, acinar necrosis, and edema. Calcium causes amylase release from rat pancreatic lobules in vitro. Higher medium calcium levels both significantly increase amylase release from unstimulated and carbachol stimulated lobules. Twelve-hour in vivo calcium infusion leads to accumulation of zymogen granules in acinar cells and acinar injury. These findings are consistent with pancreatitis evolving from calciuminduced hypersecretion to a secretion block lesion in the rat.
Similar content being viewed by others
References
Fernandez-del Castillo C, Harringer W, Warshaw AL, Vlahakes GJ, Koski G, Zaslavsky AM, Rattner DW. Risk factors for pancreatic cellular injury after cardiopulmonary bypass.N Engl J Med 1991; 325: 382–387.
Frick TW, Fryd DS, Sutherland DER, Goodale RL, Simmons RL, Najarian JS. Hypercalcemia associated withpancreatitis and hyperamylasemia in renal transplant recipients. Data from the Minnesota randomized trial of cyclosporine versus antilymphoblast azathioprine.Am J Surg 1987; 154:487–489.
Frick TW, Speiser DE, Bimmler D, Largiader F. Druginduced acute pancreatitis; further criticism.Dig Dis 1993;11: 112–132.
Goebell H, Steffen Ch, Balzer G. Stimulation of pancreatic secretion of enzymes by acute hypercalcemia in man.Eur J Clin Invest 1973; 3: 98–104.
Tiscornia O, Palasciano G, Dzieniszewski J, Verine H, Sarles H. Analysis of the mechanism of action of calciuminduced exocrine pancreatic secretory changes in the dog.Am J Gastroenterol 1975; 63: 293–298.
Layer P, Hotz J, Eysselein VE, Jansen JBMT, Goebell H. Effects of acute hypercalcemia on exocrine pancreatic secretion in the cat.Gastroenterology 1985; 88: 1168–1174.
Frick TW, Hailemariam S, Heitz PU, Largiader F, Goodale RL. Acute hypercalcemia induces acinar cell necrosis and intraductal precipitates in the pancreas of cat and guinea pig.Gastroenterology 1990; 98: 1675–1681.
Layer P, Hotz J, Cherian L, Goebell H. In vitro stimulation of pancreatic enzyme discharge by elevated extracellular calcium concentrations.Gut 1987; 28: 1215–1220.
Scheele GA, Haymovits A. Cholinergic and peptidestimulated discharge of secretory protein in guinea pig pancreatic lobules. Role of intracellular and extracellular calcium.J Biol Chem 1979; 254: 10,346–10,353.
Ziegler R, Minne H, Zwicker M, Hotz J. Unresponsiveness of exocrine rat pancreas to calcemic challenges.rRes Exp Med 1974; 162:347–350.
Scheele GA, Palade GE. Studies on the guinea pig pancreas parallel discharge of exocrine enzyme activities.J Biol Chem 1975; 250: 2660–2670.
Pappritz G, Bräuer U. Zur Technik der Schwanzvenen Dauerinfusion an der nicht immobilisierten Ratte.Drug Res 1977; 27: 864–865.
Layer P, Hotz J, Goebell H. Stimulatory effect of hypercalcemia on pancreatic secretion is prevented by pretreatment with cholecysto kinin and cholinergic agonists.Pancreas 1986; 6: 478–482.
Tsunoda Y, Stuenkel EL, Williams JA. Characterization of sustained [Ca2+]i increase in pancreatic acinar cells and its relation to amylase secretion.Am J Physiol 1990; 259: G792-G801.
Krims PE, Pandol SJ. Free cytosolic calcium and secretagogue-stimulated initial pancreatic exocrine secretion.Pancreas 1988; 3: 383–390.
Scheele GA, Palade GE. Studies on the guinea pig pancreas: parallel discharge of exocrine enzyme activities.J Biol Chem 1975; 250: 2660–2670.
Pandol SJ, Schoeffield MS, Fimmel CJ, Muallem S. The agonist-sensitive calcium pool in the pancreatic acinar cell.J Biol Chem 1987; 262: 16,963–16,968.
Lampel M, Kern HF. Acute interstitial pancreatitis in the rat induced by excessive doses of a pancreatic secretagogue.Virchows Arch A 1977; 373: 97–117.
Watanabe O, Baccino FM, Steer ML, Meldolesi J. Supramaximal caerulein stimulation and ultrastmcture of rat pancreatic acinar cell: early morphological changes during development of experimental pancreatitis.Am J Physiol 1984; 246: G457–467.
Scheele G, Adler G, Kern HF. Exocytosis occurs at the lateral plasma membrane of the pancreatic acinar cell during supramaximal secretagogue stimulation.Gastroenterology 1987; 92: 345–353.
Frick TW, Spycher MA, Heitz PU, Okagaki T, Goodale RL. Ultrastmcture of the guinea pig pancreas in acute hypercalcemia.Pancreas 1992; 7: 287–294.
Frick TW, Spycher MA, Heitz PU, Largiadèr F, Goodale RL. Hypercalcemia and pancreatic ultrastmcture in cats.Eur J Surg 1992; 158: 289–294.
Adler G, Rohr G, Kern HF. Alteration of membrane fusion as a cause of acute pancreatitis in the rat.Dig Dis Sci 1982; 27:993–1002.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Frick, T.W., Wiegand, D., Bimmler, D. et al. A rat model to study hypercalcemia-induced acute pancreatitis. Int J Pancreatol 15, 91–96 (1994). https://doi.org/10.1007/BF02924658
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02924658