Abstract
Purpose
This study reports clinicopathological features and outcome of thymic tumors. Twenty-seven patients with invasive thymoma and 6 patients with thymic carcinoma who had received radiotherapy either primary or postoperatively were analyzed retrospectively.
Patients and Methods
All 33 patients were irradiated with a mean dose of 50 Gy after complete resection (16 patients), partial resection (9 patients) or biopsy (8 patients). Staging was done according to the Masaoka classification; there were 12 Stage II, 12 Stage III and 9 Stage IV patients.
Results
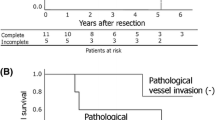
In patients with invasive thymoma Stage II to IV (median follow-up 54.4 months) Kaplan-Meier estimates of overall survival (OS), disease-specific (DSS) and disease-free survival (DFS) at 5 years were 63.7% (95% confidence interval [CI], 42 to 84%), 88.3% (CI, 75 to 100%) and 77.4% (CI, 58 to 95%), respectively. Among the prognostic factors tested, such as age, myasthenia gravis, completeness of surgery and histologic subclassification, total radiation dose, and Masaoka Stage, the latter was the only significant predictor of improved survival (p = 0.04). Considering local control, radiation dose was a significant prognostic factor (p = 0.0006). In patients with thymic carcinoma (median follow-up 43.4 months) 5-year DSS, and DFS were 22.2% (CI, 0 to 60%) and 16.7% (CI, 0 to 46%), respectively. Thymoma as compared to thymic carcinoma had a statistically significant better DSS (p = 0.007) and DFS (p = 0.0007).
Conclusion
Postoperative radiotherapy with sufficient doses plays an important role as adjuvant treatment in complete or incomplete resected invasive Stage II to III thymoma. In unresectable thymoma Stage III to IV as well as in thymic carcinoma a multimodality approach should be considered to improve survival.
Zusammenfassung
Ziel
Bericht über 27 Patienten mit invasivem Thymom und sechs Patienten mit Thymuskarzinom nach primärer oder postoperativer Strahlentherapie unter besonderer Berücksichtigung der pathohistologischen Befunde und klinischen Ergebnisse.
Patienten und Methoden
Alle 33 Patienten wurden nach kompletter Resektion (n = 16), Teilresektion (n = 9) oder Biopsie (n = 8) mit einer mittleren Dosis von 50 Gy (30 bis 60 Gy) bestrahlt. Die Stadieneinteilung nach Masaoka (Tabelle 1) ergab jeweils zwolf Patienten in Stadium II und III sowie neun Patienten im Stadium IV (Tabelle 2).
Ergebnisse
Patienten mit einem invasivem Thymom Masaoka-Stadium II bis IV (mediane Nachsorgezeit 54,4 Monate) hatten ein Fünf-Jahres-Gesamüberleben, krankheitsspezifisches und krankheitsfreies Überleben von 63,7% (95%Konfidenzintervall [KI] 42 bis 84%), 88,3% (KI 75 bis 100%) sowie 77,4% (KI 58 bis 95%). Bei den untersuchten prognostischen Faktoren, wie Alter, Myasthenia gravis, chirurgische Radikalität, histologische Subgruppe, Bestrahlungsdosis und Masaoka-Stadium, hatte nur letzteres einen stätistisch signifikanten Einfluß auf das Überleben (p = 0.04). (Tabelle 8). Bei alleiniger Berücksichtigung der lokalen Kontrolle war die Bestrahlungsdosis ein stätistisch signifikanter prognostischer Parameter (p = 0,0006) (Tabelle 7). Patienten mit Thymuskarzinom (mediane Nachsorgezeit 43,3 Monate) hatten ein krankheitsspezifisches und krankheitsfreies Fünf-Jahres-Überleben von 22,2% (KI 0 bis 60%) sowie 16,7% (KI 0 bis 46%). Patienten mit Thymomen hatten im Vergleich zu Patienten mit Thymuskarzinomen sowohl ein statistisch signifikant besseres krankheitsspezifisches (p = 0,007) als auch krankheitsfreies Überleben (p = 0,0007) (Abbildung 1).
Schlußfolgerung
Postoperative Strahlentherapie mit adäquater Dosis spielt eine wichtige Rolle als adjuvante Therapie bei inkomplett und komplett resezierten invasiven Thymomen Stadium II bis III. Bei primär inoperablen Thymomen und bei Thymuskarzinom sollte ein multimodales Vorgehen in Erwägung gezogen werden, urn die Überlebensraten zu verbessern.
Similar content being viewed by others
References
Akaogi E, Ohara K, Mitsui K, et al. Preoperative radiotherapy and surgery for advanced thymoma with invasion to the great vessels. J Surg Oncol 1996;63:17–22.
Bernatz PE, Harrison EG, Glagett OT. Thymoma. A clinicopathologic study. J Thorac Cardiovasc Surg 1961;42:424–44.
Blumberg D, Port JL, Weksler B, et al. Thymoma: A multivariate analysis of factors predicting survival. Ann Thorac Surg 1995;60:908–14.
Blumberg D, Burt ME, Bains MS, et al. Thymic carcinoma: Current staging does not predict prognosis. J Thorac Cardiovasc Surg 1998;15:303–9.
Ciernik IF, Meier U, Lütolf UM. Prognostic factors and outcome of incompletely resected invasive thymoma following radiation therapy. J Clin Oncol 1994;12:1484–90.
Cowen D, Richaud P, Mornex F, et al. Thymoma: Results of a multicentric retrospective series of 149 non-metastatic irradiated patients and review of the literature. Radiother Oncol 1995;34:9–16.
Curran WJ, Kornstein MJ, Brooks JJ, et al. Invasive thymoma: The role of mediastinal irradiation following complete or incomplete surgical resection, J Clin Oncol 1988;6:1722–7.
Haniuda M, Miyazawa M, Yoshida K, et al. Is postoperative radiotherapy for thymoma effective? Ann Surg 1996;224:219–24.
Hsu CH, Yeh KH, Cheng AL. Thymic carcinoma with autoimmune syndrome: Successful treatment with weekly infusional high dose 5 flurouracil and leucoverin. Anticancer Res 1997;17:1331–4.
Kirchner T, Schalke B, Buchwald J, et al. Well-differentiated thymic carcinoma. An organo-typical low-grade carcinoma with relationship to cortical thymoma. Am J Surg Pathol 1992;16:1153–69.
Lattes R. Thymoma and other tumors of the thymus. An analysis of 107 cases. Cancer 1962;15:1224–60.
Latz D, Schraube P, Oppitz U, et al. Invasive thymoma: Treatment with postoperative radiation therapy. Radiology 1997;204:859–64.
Levine GDS, Rosai J. Thymic hyperplasia and neoplasia: A review of current concepts. Hum Pathol 1978;9:495–515.
Lewis JE, Wick MR, Scheithauer BW, et al. Thymoma. Cancer1987;60: 2727–43.
Loehrer PJ, Chen M, Kim KM, et al. Cisplatin, doxorubicin, and cyclophosamide plus thoracic radiation therapy for limited-stage unresectable thymoma: An intergroup trial. J Clin Oncol 1997;15:3093–9.
Macchiarini P, Chella A, Ducci F, et al. Neoadjuvant chemotherapy, surgery, and postoperative radiation therapy for invasive thymoma. Cancer 1991;68:706–13.
Maggi G, Casadio C, Cavallo A, et al, Thymoma: Results of 241 operated cases. Ann Thorac Surg 1991;51:152–6.
Masaoka A, Monden Y, Nakahara K, et al. Follow-up study of thymomas with special reference to their clinical stages. Cancer 1981;48:2485–92.
Mornex F, Resbeut M, Richaud P, et al. Radiotherapy and chemotherapy for invasive thymomas: A multicentric retrospective review of 90 cases. Int J Radiat Oncol Biol Phys 1995;32:651–9.
Park HS, Shin DM, Lee JS, et al. Thymoma. A retrospective study of 87 cases. Cancer 1994;73:2491–8.
Pollack A, Komaki R, Cox JD, et al. Thymoma: Treatment and prognosis. Int J Radiat Oncol Biol Phys 1992;23:1037–43.
Ribet M, Voisin C, Provot FR, et al. Lymphoepithelial thymomas. A retrospective study of 88 resections. Eur J Cardiothorac Surg 1988;2:261–4.
Thymoma-Classification. In: Rosai P, ed. Ackerman’s surgical pathology, Vol 1, 8th edn. St. Louis, Miss.: Mosby, 1996:449–56.
Schneider PM, Fellbaum C, Fink U, et al. Prognostic importance of histomorphologic subclassification for epithelial thymic tumors. Ann Surg Oncol 1997;4:45–56.
Shin DM, Walsh GL, Komaki R, et al. A multidisciplinary approach to therapy for unresectable malignant thymoma. Ann Intern Med 1998; 129:100–4.
Uematsu M, Yoshida H, Kondo M, et al. Entire hemithorax irradiation following complete resection in patients with stage II–III invasive thymoma. Int J Radiat Oncol Biol Phys 1996;35:357–60.
Urgesi A, Monetti U, Rossi G. Role of radiation therapy in locally advanced thymoma. Radiother Oncol 1990;19:273–80.
Venuta F, Rendina E, Pescarmona E, et al. Multimodality treatment of thymoma: A prospective study. Ann Thorac Surg 1997;64:1585–92.
Wagner W, Böttcher HD, Roessner A, et al. Zum gegenwärtigen Stand der Thymomtherapie. Strahlenther Onkol 1987;163:17–22.
Wang LS, Huang MH, Lin TS, et al. Malignant thymoma. Cancer 1992; 70:443–50.
Weide L, Ulbright T, Loehrer P, et al. Thymic carcinoma. Cancer 1993;71: 1219–23.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mayer, R., Beham-Schmid, C., Groell, R. et al. Radiotherapy for invasive thymoma and thymic carcinoma. Strahlentherapie und Onkologie 175, 271–278 (1999). https://doi.org/10.1007/BF02743578
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02743578