Abstract
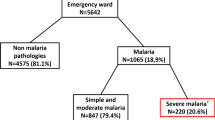
Objective:A cross-sectional hospital based study was carried out to investigate clinical features and outcome of cerebral malaria in a rural area.Methods: All children fulfilling inclusion criteria, were enrolled and were entered on specially designed proforma. Their peripheral smear (PS) were studied based on which the diagnosis was classified as definite cereral malaria (DCM) and probable cerebral malaria (PCM).Result: There were 2991 admissions in pediatric ward, of which 1394 (46.6%) were for fever. Of 781 (56.6%) cases with fever no cause was identified. Of the 56 cases positive for malarial parasite on PS 4.3% werePlasmodium vivax (PV) and 2.8%Plasmodium falciparum (PF). Fifteen patients fulfilled the criteria for study of which 7 were DCM and 8 belonged to PCM group. Twelve (80%) were in school-going age group and M : F ratio was 2 :1. All patients presented with fever, and CNS involvement, 66.6% had convulsion, 7 developed coma, anaemia was seen in 60%, but only 20% required blod transfusion. Splenomegaly and hepatomegaly was seen in 53.3% and 47% cases respectively. Two patients died, one each in DCM and PCM. Cerebral malaria is a serious complication of severe falciparum malaria and is seen in approximately 32% of PF positive cases.Conclusion; PCM is an entity which should be kept in mind when treating fever without definite focus in rural areas, because timely and specific therapy is lifesaving.
Similar content being viewed by others
References
National Malaria Eradication Programme. Operation manual for malaria action programme New Delhi. Director General of ’ Health Services, Ministry of Health and Family Welfare, 1995.
Ringwald P. Resistant malaria in children.Indian Pediatr 2001; 38:9–14.
Greenwood BM, Bradly AK, Greenwood AM. Mortality and morbidity in children from malaria in rural area of Gambia, West Africa.Trans R Soc Trap Med Hyg 1987; 81:178–186.
Molyneux ME, Taylor TE, Wirima JJ, Borgstein A. Clinical features and prognostic indicator in Pediatric cerebral malaria. Study of 131 comatosed Malwin children.Q J Med 1989; 265: 441–459.
Chaudary DS. Species of Malarial parasite.Indian Pediatr 1985; 52: 257–260.
Kulkarni AV, Kasturi L, Amin A, Mashankar V. Therapy and drug resistance in malaria.Indian J Pediatr 2000; 67: 33–35.
Faliseva C. Early diagnosis and clinical picture of malaria.WHO Bull 1974; 50:159–163.
Brown JK, Minnus RA. Disorders of central nervous system. In Campbell AGM, Mclntosh N, eds.Forfer and Arneil’s Text Book of Pediatrics; 5th edn. London, Churchill Livingstone, 1998; 704–705.
Woodrow CJ, Riberio I, Krishna S. Recent development in the management of malaria.Indian J Pediatr 1998; 65: 103–109.
Brewester DR, Kwiatkewski D, Wnite NJ. Neurological sequlae of cerbral malaria in children.Lancet 1990; 335: 1039–1043.
Philps RE, Slolman T. Cerebral Malaria in children.Lancet 1990; 336: 1355–1360.
Chander V, Mehta SR, Sharma PD, Sarkar PK, Sharma R. Falciparum Malaria.Indian J Pediatr 1989; 56: 365–369.
Beg S, Samal GC, Deep N, Patra WC, Nayal M, Mehar LK. Complicatied falciparum malaria.Indian Pediatr 1994; 31: 821–825.
Thapa BR, Marwaha RK, Kumar L, Mehta S. Cerebral Malaria in children, therapeutic consideration.Indian f Pediatr 1988; 25:61–65.
Ahmed SH, Menis R, Kidwai T, Khan TA, Khan HM, Sahal T. Cerebral malaria in children.Indian J Pediatr 1986; 53:409–413.
Akpade G, Sykes RM, Abidocum PO. Convulsion with malaria Febrile or indicative of cerebral involvement.J Trop Pediatr 1993; 39:350–355.
Toro G, Roman G. Cerebral Malaria — A disseminated vasculomyelinopathy.Arch Nerol 1978; 35:271–275.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kamble, M.B., Raut, P.P. & Hussain, Z.F. Cerebral malaria in rural India. Indian J Pediatr 69, 659–661 (2002). https://doi.org/10.1007/BF02722697
Issue Date:
DOI: https://doi.org/10.1007/BF02722697