Abstract
Background
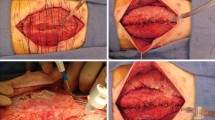
Standard therapy for abdominal compartment syndrome (ACS) is laparotomy and temporary abdominal wall closure with significant morbidity. The component separation technique allows for difficult abdominal closure. We studied a modified extraperitoneal endoscopic separation of parts technique on an animal model of ACS.
Methods
Twelve anesthetized pigs were instrumented for measurement of central venous pressure, arterial pressure, pulmonary artery pressure, pulmonary capillary wedge pressure, cardiac output, and intraabdominal pressure (IAP). ACS to 25 mmHg was created by infusing saline into an intraabdominally placed bag. Animals were divided in two equal groups. Pigs in group A underwent minimally invasive resection of the nerves supplying the rectus muscles bilaterally. Pigs in group B underwent minimally invasive modified component separation technique bilaterally. Change in IAP and other physiological parameters were recorded.
Results
(Group A) IAP increased significantly from 7.3 mmHg±3.8 to 25.2 mmHg±1.5 with infusion of saline. Following nerve transection on the right side there was a nonsignificant decrease in IAP from 25.2 mmHg±1.5 to 22.3 mmHg±1.4 and following nerve transection on the left side there was a further decrease in IAP to 20.3 mmHg±1.9. (Group B) IAP increased significantly from 3.8 mmHg±0.4 to 24.7 mmHg±0.5 with infusion of saline. Following separation of parts on the right side there was a significant decrease in IAP from 24.7 mmHg±0.5 to 15.0 mmHg±1.7 and there was a further decrease in IAP to 11.3 mmHg±1.4 following separation of parts on the left side. The only significant change in the physiological parameters measured was observed in CVP in both groups.
Conclusion
We present a porcine model of extraperitoneal endoscopic release of abdominal wall components as a treatment option for ACS.
Similar content being viewed by others
References
Bloomfield G, Saggi B, Blocher C, Sugerman H (1999) Physiologic effects of externally applied continuous negative abdominal pressure for intra-abdominal hypertension. J Trauma 46: 1009–1014; discussion 1014–1006
Bradley SE, Mudge GH, Blake WD, Alphonse P (1955) The effect of increased intra-abdominal pressure on the renal excretion of water and electrolytes in normal human subjects and in patients with diabetes insipidus. Acta Clin Belg 10:209–223.
Burch JM, Moore EE, Moore FA, Franciose R (1996) The abdominal compartment syndrome. Surg Clin North Am 76: 833–842
Corcos AC, Sherman HF (2001) Percutaneous treatment of secondary abdominal compartment syndrome. J Trauma 51: 1062–1064
Cullen DJ, Coyle JP, Teplick R, Long MC (1989) Cardiovascular, pulmonary, and renal effects of massively increased intra-abdominal pressure in critically ill patients. Crit Care Med 17: 118–121
Diebel LN, Dulchavsky SA, Brown WJ (1997) Splanchnic ischemia and bacterial translocation in the abdominal compartment syndrome. J Trauma 43: 852–855
Diebel LN, Wilson RF, Dulchavsky SA, Saxe J (1992) Effect of increased intra-abdominal pressure on hepatic arterial, portal venous, and hepatic microcirculatory blood flow. J Trauma 33: 279–282 discussion 282–273
Eddy V, Nunn C, Morris JA Jr (1997) Abdominal compartment syndrome. The Nashville experience. Surg Clin North Am 77: 801–812
Harman PK, Kron IL, McLachlan HD, Freedlender AE, Nolan SP (1982) Elevated intra-abdominal pressure and renal function. Ann Surg 196: 594–597
Ivatury RR, Porter JM, Simon RJ, Islam S, John R, Stahl WM (1998) Intra-abdominal hypertension after life-threatening penetrating abdominal trauma: prophylaxis, incidence, and clinical relevance to gastric mucosal pH and abdominal compartment syndrome. Trauma 44: 1016–1021; discussion 1021–1013
Latenser BA, Kowal-Vern A, Kimball D, Chakrin A, Dujovny N (2002) A pilot study comparing percutaneous decompression with decompressive laparotomy for acute abdominal compartment syndrome in thermal injury. J Burn Care Rehabil 23: 190–195
Maxwell RA, Fabian TC, Croce MA, Davis KA (1999) Secondary abdominal compartment syndrome: an underappreciated manifestation of severe hemorrhagic shock. J Trauma 47: 995–999
O'Mara MS, Papasavas PK, Newton ED, Caushaj PF (2004) Modified separation of parts as an intervention for intra-abdominal hypertension and the abdominal compartment syndrome in a swine model. Plast Reconstr Surg (in press)
Ramirez OM, Ruas E, Dellon AL (1990) “Components separation” method for closure of abdominal-wall defects: an anatomic and clinical study. Plast Reconstr Surg 86: 519–526
Richardson JD, Trinkle JK (1976) Hemodynamic and respiratory alterations with increased intra-abdominal pressure. J Surg Res 20: 401–404
Ridings PC, Bloomfield GL, Blocher CR, Sugerman HJ (1995) Cardiopulmonary effects of raised intra-abdominal pressure before and after intravascular volume expansion. J Trauma 39: 1071–1075
Saggi BH, Sugerman HJ, Ivatury RR, Bloomfield GL (1998) Abdominal compartment syndrome. J Trauma 45: 597–609
Voss M, Pinheiro J, Reynolds J, Greene R, Dewhirst M, Vaslef SN, Clary E, Eubanks WS (2003) Endoscopic components separation for abdominal compartment syndrome. Am J Surg 186: 158–163
Author information
Authors and Affiliations
Additional information
Online publication: 13 October 2004
Rights and permissions
About this article
Cite this article
Barnes, G.S., Papasavas, P.K., O'Mara, M.S. et al. Modified extraperitoneal endoscopic separation of parts for abdominal compartment syndrome. Surg Endosc 18, 1636–1639 (2004). https://doi.org/10.1007/BF02637135
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02637135