Abstract
Background
The optimal use of radical surgery to palliate primary rectal cancers presenting with synchronous distant metastases is poorly defined. We have reviewed stage IV rectal cancer patients to evaluate the effectiveness of radical surgery without radiation as local therapy.
Methods
Eighty stage IV patients with resectable primary rectal tumors treated with radical rectal surgery without radiotherapy were identified. Sixty-one (76%) patients received chemotherapy; response information was available for 34 patients.
Results
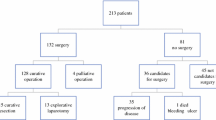
Radical resection was accomplished by low anterior resection (n=65), abdominoperineal resection (n=11), and Hartmann’s resection (n=4). Surgical complications were seen in 12 patients (15%), with 1 death and 4 reoperations. The local recurrence rate was 6% (n=5), with a median time to local recurrence of 14 months. Only one patient received pelvic radiotherapy as salvage treatment. One patient required subsequent diverting colostomy. Median survival was 25 months. On multivariate analysis, the extent of metastasis and response to chemotherapy were determinants of prolonged survival.
Conclusions
For patients who present with distant metastases and resectable primary rectal cancers, radical surgery without radiotherapy can provide durable local control with acceptable morbidity. The extent of metastatic disease and the response to chemotherapy are the major determinants of survival. Effective systemic chemotherapy should be given high priority in the treatment of stage IV rectal cancer.
Similar content being viewed by others
References
Heald RJ, Moran BJ, Ryall RDH, et al. Rectal cancer: the Basingstoke experience of total mesorectal excision, 1978–1997.Arch Surg 1998;133:894–9.
Michelassi F, Block GE, Vannucci L, et al. A 5- to 21-year follow-up and analysis of 250 patients with rectal adenocarcinoma.Ann Surg 1988;208:379–89.
Arenas RB, Fichera A, Mhoon D, Michelassi F. Total mesenteric excision in the surgical treatment of rectal cancer: a prospective study.Arch Surg 1998;133:608–11.
Jessup JM, Stewart AK, Menck HR. The National Cancer Data Base report on patterns of care for adenocarcinoma of the rectum, 1985–95.Cancer 1998;83:2408–18.
Gastrointestinal Tumor Study Group. Prolongation of the disease-free interval in surgically treated rectal carcinoma.N Engl J Med 1985;312:1465–72.
Krook JE, Moertel CG, Gunderson LL, et al. Effective surgical adjuvant therapy for high-risk rectal carcinoma.N Engl J Med 1991;324:709–15.
Wolmark N, Wieand HS, Hyams DM, et al. Randomized trial of postoperative adjuvant chemotherapy with or without radiotherapy for carcinoma of the rectum: National Surgical Adjuvant Breast and Bowel Project Protocol R-02.J Natl Cancer Inst 2000;92:388–96.
Hyams DM, Mamounas EP, Petrelli N, et al. A clinical trial to evaluate the worth of preoperative multimodality therapy in patients with operable carcinoma of the rectum: a progress report of National Surgical Breast and Bowel Project Protocol R-03.Dis Colon Rectum 1997;40:131–9.
Kapiteijn E, Marijnen CAM, Nagtegaal ID, et al. Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer.N Engl J Med 2001;345:638–46.
Kemeny N, Niedzwiecki D, Shurgot B, Oderman P. Prognostic variables in patients with hepatic metastases from colorectal cancer. Importance of medical assessment of liver involvement.Cancer 1989;63:742–7.
Kemeny N, Braun DW Jr. Prognostic factors in advanced colorectal carcinoma. Importance of lactic dehydrogenase level, performance status, and white blood cell count.Am J Med 1983;74:786–94.
Crane CH, Janjan NA, Abbruzzese JL, et al. Effective pelvic symptom control using initial chemoradiation without colostomy in metastatic rectal cancer.Int J Radiat Oncol Biol Phys 2001;49:107–16.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nash, G.M., Saltz, L.B., Kemeny, N.E. et al. Radical resection of rectal cancer primary tumor provides effective local therapy in patients with stage IV disease. Annals of Surgical Oncology 9, 954–960 (2002). https://doi.org/10.1007/BF02574512
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02574512