Abstract
Background
Second lung primaries occur at a rate of up to 3% per patient-year after curative resection for non-small-cell lung carcinoma. Postresection patients are often poor candidates for further curative surgery because of their diminished pulmonary reserve. The aim of this study was to evaluate the role of fluorescence bronchoscopy by using the Xillix® LIFE-Lung Fluorescence Endoscopy SystemTM to identify second lung primaries in patients who have had a previous curative resection of a non-small-cell lung cancer.
Methods
Patients who had no evidence of disease status after resection of a non-small-cell lung cancer were identified from a prospectively collected data base and entered onto a fluorescence bronchoscopy surveillance protocol. All suspicious areas, as well as several areas of apparently normal mucosa, were sampled for biopsy. A single pathologist reviewed all biopsy specimens, with 10% of biopsies re-reviewed, for quality control, by a second pulmonary pathologist.
Results
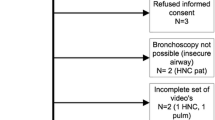
A total of 31 surveillance fluorescence bronchoscopies were performed on 25 patients after conventional bronchoscopy. Four intraepithelial neoplasias or invasive carcinomas were identified in 3 (12%) of 25 patients screened. The addition of the LIFE examination to conventional bronchoscopy increased the sensitivity of screening from 25.0% to 75.0%, which yielded a relative sensitivity of 300% with a negative predictive value of .97.
Conclusions
Use of postresection surveillance with fluorescence bronchoscopy identified intraepithelial or invasive lesions in 12% of non-small-cell lung cancer patients, and the system was three times more sensitive than conventional bronchoscopy to identify these early mucosal lesions. Fluorescence bronchoscopic surveillance of this high-risk, postresection population will help better define the true rate of occurrence and the natural history of second primaries and may assist in monitoring their response to newer, noninvasive treatment methods, such as photodynamic therapy or chemopreventive agents, in future trials.
Similar content being viewed by others
References
Johnson BE. Second lung cancers in patients after treatment for an initial lung cancer.J Natl Cancer Inst (1998);90:1335–45
Auerbach O, Stout AP, Hammond C, Garfunkel L. Changes in bronchial epithelium in relation to cigarette smoking and in relation to lung cancer.N Engl J Med (1961);265:253–67.
Woohner LB, Fontana RS, Cortese DA, et al. Roentgenographically occult lung cancer: pathologic findings and frequency of multicentricity during a 10-year period.Mayo Clin Proc (1984);59:453–66.
Lam S, Kennedy T, Unger M, et al. Localization of bronchial intraepithelial neoplastic lesions by fluorescence bronchoscopy.Chest (1998);113:696–702.
Lam S, Palcic B. Fluorescence detection. In: Roth JA, Cox JD, Hong WK, eds.Lung Cancer. Boston: Blackwell Scientific, 1991: 325–38.
Thomas P, Rubinstein L, The Lung Cancer Study Group. Cancer recurrence after resection: T1N0 non-small cell lung cancer.Ann Thorac Surg 1990;49:242–7.
Cortese DA, Pairolero PC, Bergstralh EJ, et al. Roentgenographically occult lung cancer: a ten year experience.J Thorac Cardiovasc Surg (1983);86:373–80.
Lam S, Becker HD. Future diagnostic procedures.Chest Surg Clin N Am (1996);6:363–80.
Tockman MS, Gupta PK, Pressman NJ, Mulshine JL. Considerations in bringing a cancer biomarker to clinical application.Cancer Res (1992);52:2711S-8S.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Weigel, T.L., Yousem, S., Dacic, S. et al. Fluorescence bronchoscopic surveillance after curative surgical resection for non-small-cell lung cancer. Annals of Surgical Oncology 7, 176–180 (2000). https://doi.org/10.1007/BF02523650
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02523650