Abstract
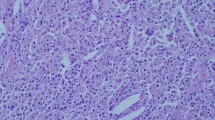
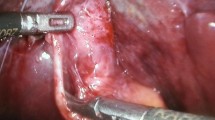
Xanthogranulomatous cholecystitis (XGC) is a rare inflammatory disease of the gallbladder. In severe cases, inflammation extends to adjacent structures, and XGC is sometimes confused with a malignant neoplasm. We recently diagnosed XGC as the preoperative cause of Mirizzi syndrome in a patient based on the clinical course. The patient was admitted because of obstructive jaundice, with gallbladder carcinoma as the suspected cause. The gallbladder was swollen with gallstones and the serum level of carbohydrate antigen 19-9 (CA19-9) was 3070 U/ml at admission. A percutaneous transhepatic cholangiodrainage (PTCD) was done, and the common hepatic duct as well as the right and left hepatic ducts were found to be obstructed. Later, the CA19-9 level and swelling of the gallbladder decreased and the obstruction of the bile ducts disappeared. A cholecystectomy was performed and the intraoperative pathohistological diagnosis of chronic cholecystitis was made from frozen sections. The pathohistological diagnosis of XGC was made from paraffin-embedded sections. Mirizzi syndrome such as that seen in our patient is a rare complication of XGC. XGC occassionally causes extensive inflammation; thus, performing a conventional cholecystectomy can be unsafe. However, in our opinion, a total, not subtotal, cholecystectomy should be done whenever possible because the incidence of gallbladder carcinoma accompanied with XGC is higher than that with ordinary cholecystitis or gallstones.
Similar content being viewed by others
References
Roberts KM, Parsons MA (1987) Xanthogranulomatous cholecystitis: clinicopathological study of 13 cases. J Clin Pathol 40:412–417
Reyes CV, Jablokow VR, Reid R (1981) Xanthogranulomatous cholecystitis: report of seven cases. Am Surg 47:322–325
Takahashi K, Oka K, Hakozaki H, Kojima M (1976) Ceroid-like histiocytic granuloma of gallbladder: a previously undescribed lesion. Acta Pathol Jpn 26:25–46
Edlund Y, Olsson O (1961) Acute cholecystitis: its aetiology and course, with special reference to the timing of cholecystectomy. Acta Chir Scand 120:479–494
Kitagawa S, Nakagawa M, Yamada T, Mori Y, Simizu H, Rin S, Kurumaya H (1990) Clinicopathological study of xanthogranulomatous cholecystitis (in Japanese with English abstract). Nippon Geka Gakkai Zasshi (J Jpn Surg Soc) 91:1001–1010
Iwasaki M, Noguchi T, Yamagiwa K (1994) Xanthogranulomatous cholecystitis with abnormally high level of CA19-9 differentiated from gallbladder carcinoma by imagings: report of a case (in Japanese with English abstract). Nippon Rinsho Gekai Gakkai Zasshi (J Jpn Soc Clin Surg) 55:2098–2102
Hanada K, Nakata H, Nakayama T, Tsukamoto Y, Terashima H, Kuroda Y, Okuma R (1987) Radiologic findings in xanthogranulomatous cholecystitis. Am J Roentgenol 148:727–730
Benbow EW (1990) Xanthogranulomatous cholecystitis. Br J Surg 77:255–256
Del Villano BC, Brennan S, Brock P, Bucher C, Liu V, McClure M, Rake B, Space S, Westrik B, Schoemaker H, Zurawski VR Jr (1983) Radioimmunometric assay for a monoclonal antibody-defined tumor marker, CA 19-9. Clin Chem 29:549–552
Mutoh I, Otowa T (1992) A case of cholecystolithiasis with abnormally high values of CA19-9 in the blood (in Japanese with English abstract). Nippon Rinsho Gekai Gakkai Zasshi (J Jpn Soc Clin Surg) 53:2763–2766
Ohkawa A, Kamegashira M, Akamatsu H, Yoshitatsu M (1993) A case of markedly elevated serum CA19-9 with choledocholithiasis (in Japanese with English abstract). Nippon Shokaki Geka Gakkai Zasshi (Jpn J Gastroenterol Surg) 26:1085–1089
Albert MB, Steinberg WM, Henry JP (1988) Elevated serum levels of tumor marker CA19-9 in acute cholangitis. Dig Dis Sci 33:1223–1225
Curet MJ, Rosendale DE, Congilosi S (1994) Mirizzi syndrome in a native American population. Am J Surg 168:616–621
Nobesawa S, Aoi T, Matsumoto A, Aoki F, Yamasaki K, Shikano S, Katayanagi T, Shinmi N (1992) An operated case of Mirizzi syndrome presenting with stenosis extending to the intrahepatic ducts (in Japanese with English abstract). Nippon Rinsho Gekai Gakkai Zasshi (J Jpn Soc Clin Surg) 53:2481–2485
Musher DR, Madayag MA, Tobias H (1976) Carcinoma of the gallbladder: a diagnosis aided by endoscopic retrograde and percutaneous hepatic cholangiography. Am J Gastroenterol 66:79–83
Howard TJ, Bennion RS, Thompson JE Jr (1991) Xanthogranulomatous cholecystitis: a chronic inflammatory pseudotumor of the gallbladder. Am Surg 57:821–824
Nagami H, Tamura K, Sumi S, Sasaki S, Kin S, Yano S, Seshimo T, Nio Y, Nagaoka S (1995) Case report of xanthogranulomatous cholecystitis accompanied by Mirizzi syndrome. J Hep Bil Pancr Surg 2:95–98
Kanegae S, Fukazawa N, Yamashiro S, Yoshihara K, Koizumi S, Miyazaki K, Hisatsugu T, Fukui T (1995) A case of xanthogranulomatous cholecystitis presenting with Mirizzi syndrome (in Japanese with English title). Naika 75:343–346
Goodman ZD, Ishak KG (1981) Xanthogranulomatous cholecystitis. Am J Surg Pathol 5:653–659
Benbow EW, Taylor PM (1988) Simultaneous xanthogranulomatous cholecystitis and primary adenocarcinoma of gallbladder. Histopathology 12:672–675
Roberts KM, Parsons MA (1988) Simultaneous xanthogranulomatous cholecystitis and primary adenocarcinoma of the gallbladder. Histopathology 13:708
Benbow EW (1989) Xanthogranulomatous cholecystitis associated with carcinoma of the gallbladder. Postgrad Med J 65:528–531
Ueda S, Urata T, Morishita A, Sonobe N, Takamoto M, Tanaka S, Nakao K, Yamada Y, Kasahara Y, Kuyama T, Hajiro K (1988) Seven cases of Mirizzi syndrome (in Japanese). Nippon Shokaki Geka Gakkai Zasshi (Jpn J Gastroenterol Surg) 21:909–912
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Lee, K.C., Yamazaki, O., Horii, K. et al. Mirizzi syndrome caused by xanthogranulomatous cholecystitis: Report of a case. Surg Today 27, 757–761 (1997). https://doi.org/10.1007/BF02384992
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02384992