Abstract
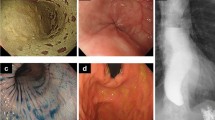
A case of achalasia coexistent with sigmoid megacolon in a 38-year-old man with known epilepsy is described. The patient was referred to the Ryukyu University Hospital with a 4-year history of dysphagia and heartburn and a 1-year history of abnormal bowel movement. On admission, upper gastrointestinal (GI) series demonstrated a dilated, tortuous thoracic esophagus with a flask-type configuration. Barium enema studies showed a dilated sigmoid colon from the rectosigmoid junction to the descending colon. Myotomy (modified Jekler-Lhotka's procedure) for achalasia and simple sigmoidectomy for sigmoid megacolon were carried out. The biopsied wall of the narrowed esophageal segment at operation showed decreased numbers of ganglion cells in Auerbach's plexus and atrophy of the muscle fibers. The resected dilated sigmoid colon revealed degeneration and markedly decreased numbers of ganglion cells in Auerbach's and Meissner's plexuses. The patient's postoperative course was uneventful and he has been doing well since surgery.
The present case is very interesting and to our knowledge, such a case is rare in the literature. We believe that the abnormalities of the ganglion cells may be due to the same etiologic factor as the sigmoid megacolon. The association of the two pathologic processes is discussed, together with a brief review of the literature.
Similar content being viewed by others
References
Okamoto E, Iwasaki T, Kakutani T, et al. Selective destruction of myenteric plexus: Its relation to Hirshsprung's disease, achalasia of the esophages and hypertrophic pyloric stenosis. J Pediatr Surg 1967;2:444–454.
Ehrenpreis T. Pseudo-Hirschsprung's disease: Seminar on pseudo-Hirschsprung's disease and related disorders. Arch Dis Child 1966;41:143–144.
Ehrenpreis T. Some newer aspects of Hirschsprung's disease and allied disorders. J Pediatr Surg 1966;1:329–337.
Ariel I, Hershlag A, Lernau O, et al. Hypoganglionosis of the myenteric plexus with normal Meissner's plexus: A new variant of colonic ganglion cell disorders. J Pediatr Surg 1985;20:90–92.
Okamoto S, Ohno H, Sakai Y, et al. A case of achalasia with megacolon. Jpn J Gastroenterol 1989;86:916–920.
Kawasugi K, Sugamata N, Ohkuni A, et al. An autopsy case of achalasia with megacolon and spinocerebellar degeneration. Gastroenterol Endosc 1982;24:986.
Touloukian RJ, Duncan R. Aequired aganglionic megacolon in a premature infant: Report of a case. J Pediatr Surg 1975; 12:675–680.
Towne BH, Stocker JT, Thompson HE, et al. Acquired aganglionosis. J Pediatr Surg 1979;14:688–690.
Ponka JL, Grodsinsky C, Brush BE, et al. Megacolon in teenage and adult patients. Dis Colon Rectum 1972;15:14–22.
MacMahon RA, Moore CC, Cussen LJ, et al. Hirschsprung-like syndromes in patients with normal ganglion cells on suction rectal biopsy. J Pediatr Surg 1981;16:835–839.
Ferreira-Santos R. Megacolon and megarectum in Chaga' disease. Proc R Soc Med 1961;16:1047–1053
Raia A. Pathogenesis and treatment of acquired megacolon. Surg Gynecol Obstet 1955;101:69–79.
Chow CW, Chan WC, Yue PC. Histochemical criteria for the diagnosis of Hirschsprung's disease in rectal suction biopsy by acetylcholinesterase activity. J Pediatr Surg 1977;12:675–680.
Lesser PB, El-Nahas AM, Luki P, et al. Adult-onset Hirschsprung's disease. JAMA 1979;8:747–748.
Ritama V, Vapaatalo HI, Neuvonen PJ. Phenothiazines and intestinal dilation. Lancet 1969:I:470.
Schuster R, Ferenci P, Schmidbauer M. et al. Intestinal neuronal degeneration in a patient with chronic idiopathic intestinal pseudoobstruction. Dig Dis Sci 1989;34:123–128.
Bruyn GA, Bots AM, Wijhe MV, et al. Chronic intestinal pseudoobstruction as a possible sequel to encephalitis. Am J Gastroenterol 1986;81:50–54.
Lennon VA, Sas DF, Busk MF, et al. Enteric neuronal autoantibodies in pseudoobstruction with small-cell lung carcinoma. Gastroenterology 1991;100:137–142.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Tokumine, F., Muto, Y., Okushima, N. et al. A rare case of achalasia coexistent with sigmoid megacolon and associated with epilepsy. J Gastroenterol 29, 637–641 (1994). https://doi.org/10.1007/BF02365448
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02365448