Summary
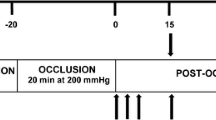
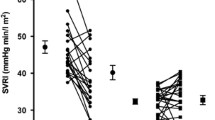
Increased peripheral vascular tone in patients with chronic heart failure (CHF) is an important factor which contributes to increased cardiac afterload and reduced exercise capacity, and consequent further deterioration in CHF. The role of endogenous nitric oxide (NO) in the regulation of basal vascular tone in CHF is controversial. This study has investigated (1) whether basal NO bioavailability is reduced in the peripheral vasculature of patients with nonischemic CHF in the absence of confounding factors influencing endothelial function, and (2) if a difference is found, what clinical characteristics are related to the decreased NO-dependent vasodilation. Basal forearm blood flow (FBF) of 12 patients with CHF and 14 healthy volunteers was measured before and after administration ofN G-monomethyl-l-arginine (l-NMMA) by venous occlusion plethysmography. Afterl-NMMA administration, basal FBF in both healthy subjects and patients with CHF decreased significantly, with the decrease in CHF patients being less than that in healthy volunteers (−0.7 ± 0.2 vs −1.5 ± 0.2ml/min per 100ml tissue,P < 0.01). When both groups were considered together, basal FBF was closely related to the decrease in FBF afterl-NMMA administration (r = −0.83.P < 0.001). When CHF patients were divided into two groups according to NYHA class, thel-NMMA-induced decrease in FBF in moderate CHF (NYHA III;n = 7) was significantly less than that in mild CHF (NYHA II;n = 5) (−0.36 ± 0.13 vs −1.16 ± 0.72ml/min per 100ml tissue,P < 0.05). In conclusion, basal bioavailability of NO in the peripheral vascular bed in nonischemic CHF is impaired, with an increase in basal vascular tone and with progression of this disorder. This suggests that impaired basal NO bioactivity may make an important contribution to the elevated peripheral vascular tone and expression of symptoms seen in CHF.
Similar content being viewed by others
References
Zelis R, Flaim SF (1982) Alterations in vasomotor tone in congestive heart failure. Prog Cardiovasc Dis 24:437–459
Kubo SH, Rector TS, Bank AJ, Williams RE, Heifetz SM (1991) Endothelium-dependent vasodilation is attenuated in patients with heart failure. Circulation 84:1589–1596
Drexler H, Hayoz D, Munzel T, Hornig B, Just H, Brunner HR, Zelis R (1992) Endothelial function in chronic congestive heart failure. Am J Cardiol 69:1596–1601
Katz SD, Biasucci L, Sabba C, Strom JA, Jondeau G, Galvao M, Solomon S, Nikolic SD, Forman R, LeJemtel TH (1992) Impaired endothelium-mediated vasodilation in the peripheral vasculature of patients with congestive heart failure. J Am Coll Cardiol 19:918–925
Imaizumi T, Hirooka Y, Takeshita A (1992) Decreased skeletal muscle vasodilation in patients with congestive heart failure. Jpn Circ J 56:500–503
Hirooka Y, Imaizumi T, Harada S, Masaki H, Momohara M, Tagawa T, Takeshita A (1992) Endothelium-dependent forearm vasodilation to acetylcholine but not to substance P is impaired in patients with heart failure. J Cardiovasc Pharmacol 20:S221-S225
Nakamura M, Arakawa N, Yoshida H, Makita S, Hiramori K (1994) Vasodilatory effects of C-type natriuretic peptide on forearm resistance vessels are distinct from those of atrial natriuretic peptide in chronic heart failure. Circulation 90:1210–1214
Koller A, Sun D, Huang A, Kaley G (1994) Corelease of nitric oxide and prostaglandins mediates flow-dependent dilation of rat gracilis muscle arterioles. Am J Physiol 267:H326-H332
Kuchan MJ, Frangos JA (1994) Role of calcium and calmodulin in flow-induced nitric oxide production in endothelial cells. Am J Physiol 266:C628-C6236
Rudic RD, Shesely EG, Maeda N, Smithies O, Segal SS, Sessa WC (1998) Direct evidence for the importance of endothelium-derived nitric oxide in vascular remodeling. J Clin Invest 101:731–736
Katz SD, Krum H, Khan T, Knecht M (1996) Exerciseinduced vasodilation in forearm circulation of normal subjects and patients with congestive heart failure: role of endothelium-derived nitric oxide. J Am Coll Cardiol 28:585–590
Kubo SH, Rector TS, Bank AJ, Raij L, Kraemer MD, Tadros P, Beardslee M, Garr MD (1994) Lack of contribution of nitric oxide to basal vasomotor tone in heart failure. Am J Cardiol 74:1133–1136
Ferrari R, Bachetti T, Confortini R, Opasich C, Febo O, Corti A, Cassani G, Visioli O (1995) Tumor necrosis factor soluble receptors in patients with various degrees of congestive heart failure. Circulation 92:1479–1486
Levine B, Kalman J, Mayer L, Fillit HM, Packer M (1990) Elevated circulating levels of tumor necrosis factor in severe chronic heart failure. N Engl J Med 323:236–241
Aoki N, Siegfried M, Lefer AM (1998) Anti-EDRF effect of tumor necrosis factor in isolated, perfused cat carotid arteries. Am J Physiol 256:H1509-H1512
Usui M, Matsuoka H, Miyazaki H, Ueda S, Okuda S, Imaizumi T (1998) Increased endogenous nitric oxide synthase inhibitor in patients with congestive heart failure. Life Sci 26:2425–2430
Belch JJ, Bridges AB, Scott N, Chopra M (1991) Oxygen free radicals and congestive heart failure. Br Heart J 65:245–248
Nakamura M, Yoshida H, Arakawa N, Mizunuma Y, Makita S, Hiramori K (1996) Endothelium-dependent vasodilatation is not selectively impaired in patients with chronic heart failure secondary to valvular heart disease and congenital heart disease. Eur Heart J 17:1875–1881
Creager MA, Quigg RJ, Ren CJ, Roddy MA, Colucci WS (1991) Limb vascular responsiveness to beta-adrenergic receptor stimulation in patients with congestive heart failure. Circulation 83:1873–1879
Katz SD, Rao R, Berman JW, Schwarz M, Demopoulos L, Bijou R, LeJemtel TH (1994) Pathophysiological correlates of increased serum tumor necrosis factor in patients with congestive heart failure. Relation to nitric oxidedependent vasodilation in the forearm circulation. Circulation 90:12–16
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Yoshida, H., Nakamura, M., Akatsu, T. et al. Effects of nitric oxide inhibition on basal forearm blood flow in patients with nonischemic chronic heart failure. Heart Vessels 13, 142–146 (1998). https://doi.org/10.1007/BF01747831
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01747831