Abstract
Objective
To design and evaluate a simple and rapid method to predict body hydration status in critically ill patients.
Design
Prospective, consecutive sample.
Setting
Medical intensive care unit of a university hospital.
Patients
31 consecutive patients.
Methods
All patients were classified daily for hydration status by the attending physician based on clinical impression, weight changes and laboratory measurements. The hydration status was scored as ‘dehydrated’, ‘euvolemic’ or ‘edematous’. The total body impedance was measured daily by a tetrapolar impedance technique.
Results
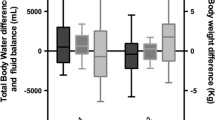
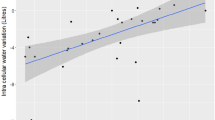
Resistances >700Ω were found in dehydrated subjects and resistances of <400 Ω in edematous patients. Weight gain was observed in dehydrated and weight loss in edematous patients. A discriminant analysis was used to create a predictive model for hydration using the daily impedance and weight measurements. If a cutoff point of 60% for the predicted classification was used to categorize the patient's hydration as dehydrated, euvolemic and edematous, no false positive predictions were observed for the dehydrated or the edematous state.
Conclusion
Impedance measurements are in close agreement with the clinical impression of hydration of critically ill patients. Future investigations must elucidate the clinical importance.
Similar content being viewed by others
References
Roos AN, Westendorp RGJ, Frölich M, Meinders AE (1993) Weight changes in critically ill patients evaluated by fluid balances and impedance measurements. Crit Care Med 21:871–877
Hoffer FC, Meador CK, Simpson DC (1969) Correlation of whole-body impedance with total body water volume. J Appl Physiol 27:531–534
Zillikens MC, Conway JM (1991) Estimation of total body water by bioelectrical impedance analysis in blacks. Am J Human Biol 3:25–32
Heitmann BL (1990) Prediction of body water and fat in adult Danes from measurement of electrical impedance, a validation study. Int J Obes 14:789–802
Kushner RF, Schoeller DA (1986) Estimation of total body water by bioelectrical impedance analysis. Am J Clin Nutr 44:417–424
Böhm D, Odaischi M, Beyerlein C, Overbeck W (1990) Total body water: changes during dialysis estimated by bioimpedance analysis. Infusionstherapie 17:75–78
De Lorenzo A, Barra PF, Sasso GF, Battistini NC, Deurenberg P (1991) Body impedance measurements during dialysis. Eur J Clin Nutr 45:321–325
Scanferla F, Landini S, Fracasso A, Morachiello P, Righetto F, Toffoletto (1990) On-line bioelectric impedance during haemodialysis: monitoring of body fluids and cell membrane status. Nephrol Dial Transplant 5:167–170
Zarowitz BJ, Pilla AM (1989) Bioelectrical impedance in clinical practice. DICP 23:548–555
Kawai C, Tomiyama T, Ueki H (1992) Phase angle derived from bioelectrical impedance analysis and postoperative fluid balance. Clin Nutr 11:99
Siervogel RM, Woynarowska B, Chumlea WC, Guo SM, Roche AF (1987) Bioelectric impedance measures of body composition: their relationship with level of blood pressure in young adults. Hum Biol 59:245–255
Chumlea WC, Baumgartner RN (1990) Bioelectrical impedance methods for the estimation of body composition. Can J Sport Sci 15:172–179
Nyboer J (1991) Workable volume and flow concepts of bio-segments by electrical impedance plethysmography. Nutrition 7:396–408
Pullicino E, Coward WA, Stubbs RJ, Elia M (1990) Bedside and field methods for assessing body composition: comparison with deuterium dilution technique. Eur J Clin Nutr 44:753–762
Lukaski HC, Bolonchuk WW (1988) Estimation of body fluid volumes using tetrapolar bioelectrical impedance measurements. Aviat Space Environ Med 59:1163–1169
Fredrix EW, Saris WH, Soeters PB, Wouters EF, Kester AD, von Meyenfeldt MF, Westerterp KR (1990) Estimation of body composition by bioelectrical impedance in cancer patients. Eur J Clin Nutr 44:749–752
Shike PW (1991) Statistical methods in laboratory medicine. Butterworth-Heinemann, Oxford
Zillikens MC, van den Berg JW, Wilson JH, Swart GR (1992) Whole-body and segmental bioelectrical-impedance analysis in patients with cirrhosis of the liver: changes after treatment of ascites. Am J Clin Nutr 55:621–625
Kushner RF, Schoeller DA, Fjeld CR, Danford L (1992) Is the impedance index (ht2/R) significant in predicting total body water. Am J Clin Nutr 56:835–839
Gleichauf CN, Roe DA (1989) The menstrual cycle's effect on the reliability of bioimpedance measurements for assessing body composition. Am J clin Nutr 50:903–907
Gray DS (1988) Changes in bioelectrical impedance during fasting. Am J Clin Nutr 48:1184–1187
Schroeder D, Christie PM, Hill GL (1990) Bioelectrical impedance analysis for body composition: clinical evaluation in general surgical patients. JPEN 14:129–133
Chioléro RL, Gay LJ, Cotting J, Gurtner C, Schutz Y (1992) Assessment of changes in body water by bioimpedance in acutely ill surgical patients. Intensive Care Med 18:322–326
Novak I, Davies PSW, Elliott MJ (1992) Noninvasive estimation of total body water in critically ill children after cardiac operations. J Thorac Cardiovasc Surg 104:585–589
Meguid MM, Lukaski HC, Tripp MD, Rosenburg JM, Parker FB (1992) Rapid bedside method to assess changes in postoperative fluid status with bioelectrical impedance analysis. Surgery 112: 502–508
De Lorenzo A, Barra PF, Sasso GF, battistini NC, Deurenberg P (1991) Body impedance measurements during dialysis. Eur J Clin Nutr 45:321–325
Jebb SA, Elia M (1991) Assessment of changes in total body water in patients undergoing renal dialysis using bioelectrical impedance analysis. Clin Nutr 10:81–84
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Roos, A.N., Westendorp, R.G.J., Brand, R. et al. Predictive value of tetrapolar body impedance measurements for hydration status in critically ill patients. Intensive Care Med 21, 125–131 (1995). https://doi.org/10.1007/BF01726535
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01726535