Abstract
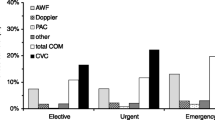
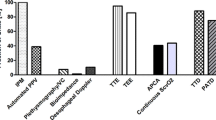
As part of a nationwide evaluation of intensive care, we examined patient- and hospital-related factors which could influence the patterns of utilization of arterial cannulae and central venous and pulmonary artery catheters. We also studied the possible impact of these interventions on the short-term outcome among 14951 consecutive ICU admissions to 25 intensive care units (75% of all ICU beds) in Finland. There was considerable variation between individual units in the use of these devices even if the differences in severity of illness were taken into account. Arterial cannulation was used in 71.2%, PA catheterization in 10.6% and CVP monitoring in 49.3% of cases in teaching ICUs, excluding cardiac surgery, and in 38.5%, 2.6% and 33.1% of cases in nonteaching ICUs respectively. The factors predicting the use of invasive monitoring included extensive surgery causing a risk of cardiovascular instability, needs for mechanical ventilation, infusion of vasoactive drugs and complicated fluid therapy. Cardiovascular problems among non-operative patients increased the odds for PA catheterization but reduced them for arterial and CV cannulation. No clear-cut benefit could be found in the form of hospital mortality reduction from invasive haemodynamic monitoring, used as described in this study.
Similar content being viewed by others
References
Gore JM, Goldberg RJ, Spodick DH, Alpert JS, Dalen JE (1987) A community-wide assessment of the use of pulmonary artery catheters in patients with acute myocardial infarction. Chest 92:721–727
Mangano DT (1980) Monitoring pulmonary arterial pressure in ccronary artery disease. Anesthesiology 53:364–370
Connors Jr AF, McCaffree DR, Gray BA (1983) Evaluation of right-heart catheterization in the critically ill patient without acute myocardial infarction. N Engl J Med 308:263
Eisenberg PR, Jaffe AS, Schuster DP (1984) Clinical evaluation compared to pulmonary artery catheterization in the hemodynamic assessment of critically ill patients. Crit Care Med 12:549–553
Tuchschmidt J, Sharma OP (1987) Impact of hemodynamic monitoring in a medical intensive care unit. Crit Care Med 15:840–843
Damen J, Bolton D (1986) A prospective analysis of 1400 pulmonary artery catheterizations in patients undergoing cardiac surgery. Acta Anasthesiol Scand 30:386–392
Band JD, Maki DG (1979) Infections caused by arterial catheters used for hemodynamic monitoring. Am J Med 67:735–741
Bedford RF, Wollman H (1973) Complications of percutaneous radial-artery cannulation. An objective prospective study in man. Anesthesiology 38:228–236
Davis FM, Stewart JM (1980) Radial artery cannulation. A prospective study in patients undergoing cardiothoracic surgery. Br J Anaesth 52:41–47
Gill JE, Cairns JA (1988) Prospective study of pulmonary artery balloon floatation catheter insertions. Intensive CAre Med 3:121–128
Matthay MA, Chatterjee K (1988) Bedside catheterization of the pulmonary artery: risks compared with benefits. Ann Intern Med 109:826–834
Shah KB, Rao TLK, Laughlin S, El-Etr AA (1984) A review of pulmonary artery catheterization in 6245 patients. Anesthesiology 61:271–275
Rull JRV, Aguirre LJ, de la Puerta E, Millan ME, Maldonado LP, Clausell CP (1984) Thrombocytopenia induced by pulmonary artery flotation catheters. A prospective study. Intensive Care Med 10:29–31
Lowenstein E, Teplick R (1980) To (PA) catheterize or not to (PA) catheterize — that is the question. Anesthesiology 53:361–363
Robin ED (1985) The cult of the Swan-Ganz catheter. Overuse and abuse of pulmonary flow catheters. Ann Intern Med 103:445–449
Spodick DH (1989) Analysis of flow-directed pulmonary artery catheterization. JAMA 261:1946–1947
Sibbald WJ, Sprung CL (1988) The pulmonary artery catheter. The debate continues. Chest 94:899–901
Singer M, Bennett ED (1989) Invasive hemodynamic monitoring in the United Kingdom. Enough or too little? Chest 95:623–626
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1986) An evaluation of outcome from intensive care in major medical centers. Ann Intern Med 104:410–418
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) Apache II: a severity of disease classification system. Crit Care Med 13:818–829
Cullen DJ, Keene R, Waternaux C, Peterson H (1984) Objective quantitative measurement of severity of illness in critically ill patients. Crit Care Med 12:155–160
The French multicenter group for ICU research. The inserm unit 169 of statistical and epidemiological studies (1989) Factors related to outcome in intensive care: French multicenter study. Crit Care Med 17:305
Rauhala V, Kari A, Nikki P, Iisalo E, Kaukinen L, Saarela E (1989) The outcome of intensive care in teaching and non-teaching hospitals (abstract) Proc 5th World Congr Intentive Crit CAre Med. Excerpta Medica 1990:1297
Pearson KS, Gomez MN, Moyers JR, Carter JG, Tinker JH (1989) A cost/benefit analysis of randomized invasive monitoring for patients undergoing cardiac surgery. Anesth Analg 69:336–341
Iberti TJ, Fisher CJ (1983) A prospective study on the use of the pulmonary artery catheter in a medical intensive care unit — its effect on diagnosis and therapy. Crit Care Med 11:238
Tuman KJ, McCarthy RJ, Spiess BD, DaValle M, Hompland SJ, Dabir R, Ivankovich AD (1989) Effect of pulmonary artery catheterization on outcome in patients undergoing coronary artery surgery. Anesthesiology 70:199–206
Fedullo AJ, Swinburne AJ, Wahl GW, Bixby KR (1988) Apache II score and mortality in respiratory failure due to cardiogenic pulmonary edema. Crit Care Med 16:1218
Hopefl AW, Taaffe CL, Herrmann WM (1989) Failure of Apache II alone as a predictor of mortality in patients receiving total parenteral nutrition. Crit Care Med 17:414–417
Author information
Authors and Affiliations
Consortia
Rights and permissions
About this article
Cite this article
Saarela, E., Kari, A., Nikki, P. et al. Current practice regarding invasive monitoring in intensive care units in Finland. Intensive Care Med 17, 264–271 (1991). https://doi.org/10.1007/BF01713935
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01713935