Abstract
Objective
To determine the relation of malnutrition and underlying diagnosis to the length of stay in the Intensive Care Unit (ICU) and to mortality after lung transplantation (LTX).
Design
Retrospective ICU chart review.
Setting
Cardiothoracic ICU in a University hospital.
Patients
Fifty-one consecutive patients who suffered from end-stage lung disease from. April 1992 to January 1994.
Interventions
None.
Measurements and results
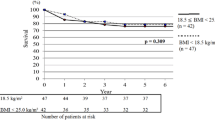
The median time spent in the ICU was 5 days (range, 2–123 days). Patients with an underlying diagnosis of obstructive lung disease had significantly shorter ICU stays (median 4 days; range, 2–28 days) than those with restrictive lung disease (median 7 days; range, 2–123 days) (p=0.005) or pulmonary hypertension (median 10 days; range, 2–38 days) (p=0.041). Significant differences in ICU duration were observed between patients after double lung transplantation (median 10 days; range, 2–123 days) and those after single lung transplantation (median 4 days; range, 2–36 days) (p=0.004). No statistically significant difference in ICU duration was found between patients with different nutritional statuses. In those patients who could not be discharged from the ICU before the 5th day, a body mass index (BMI) below the 25th percentile was a statistically significant risk factor for ICU mortality (p<0.05).
Conclusions
We conclude that the type of transplant procedure and the underlying diagnosis are important predictive indicators of ICU duration. A poor nutritional status (BMI below the 25th percentile) is a risk factor for ICU mortality in cases of patients who stay for 5 days or longer in the ICU.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Mullen JL (1981) Consequences of malnutrition in the surgical patient. Surg Clin North Am 61: 465–487
Gorse GJ, Messner RL, Stephens ND (1989) Association of malnutrition with nosocomial infection. Infect Control Hosp Epidemiol 10: 194–203
Nwiloh J, Freeman H, McCord C (1989) Malnutrition: an important determinant of fatal outcome in surgically treated pulmonary suppurative disease. J Natl Med Assoc 81: 525–529
Hunter AMB, Carey MA, Larsh HW (1981) The nutritional status of patients with chronic obstructive pulmonary disease. Am Rev Respir Dis 124: 376–381
Openbrier DR, Irwin MM, Rogers RM, Gottlieb GP, Dauber JH, Van Thiel DH, Pennock BE (1983) Nutritional status and lung function in patients with ephysema and chronic bronchitis. Chest 83: 17–22
Cronk CE, Roche AF (1982) Race-and sex-specific reference data for triceps and subscapular skinfolds and weight/stature. Am J Clin Nutr 35: 347–354
Klepetko W, Grimm M, Laufer G, Wollenek G, Hiesmayr M, Wisser W, Oturanlar D, End A, Wolner E (1992) One and one-half year experience with unilateral and bilateral lung transplantation. J Card Surg 7: 126–133
Davis RD, Trulock EP, Manley J, Pasque MK, Sundaresan S, Cooper JD, Patterson GA (1994) Differences in early results after single-lung transplantation. Ann Thorac Surg 58: 1327–1335
El Gamel A, Kakadellis J, Egan J, Deiraniya A, Rahman A, Campbell C, Yonan N (1996) Single lung transplantation for emphysema: predictors of native lung hyperinflation (Abstract). J Heart Lung Transplant 15: S42
Montoya A, Mawulawde K, Houck J, Sullivan H, Lonchyna V, Blakeman B, Hinkamp T, Garrity E, Pifarre R (1994) Survival and functional outcome after single and bilateral lung transplantation. Surgery 116: 712–718
Detterbeck FC, Egan TM, Mill MR (1995) Lung transplantation after previous thoracic surgical procedures. Ann Thorac Surg 60: 139–143
Triantafillou AN, Pasque MK, Huddleston CB, Pond CG, Cerza RF, Forstot RM, Cooper JD, Patterson GA, Lappas DG (1994) Predictors, frequency, and indications for cardiopulmonary bypass during lung transplantation in adults. Ann Thorac Surg 57: 1248–1251
Novick RJ, Menkis AH, McKenzie FN (1992) New trends in lung preservation: a collective review. J Heart Lung Transplant 11: 377–392
Pikul J, Sharpe MD, Lowndes R, Ghent CN (1994) Degree of preoperative malnutrition is predictive of postoperative morbidity and mortality in liver transplant recipients. Transplantation 57: 469–472
Sharples L, Hathaway T, Dennis C, Caine N, Higenbottam T, Wallwork J (1993) Prognosis of patients with cystic fibrosis awaiting heart and lung transplantation. J Heart Lung Transplant 12: 669–674
Wilmore DW (1991) Catabolic illness. Strategies for enhancing recovery. N Engl J Med 325: 695–702
Chandra RK (1983) Nutrition, immunity, and infection: present knowledge and future directions. Lancet 1: 688–691
Windsor JA, Knight GS, Hill GL (1988) Wound healing response in surgical patients: recent food intake is more important than nutritional status. Br J Surg 75: 135–137
Windsor JA, Hill GL (1988) Grip strength: a measure of the proportion of protein loss in surgical patients. Br J Surg 75: 880–882
Kelly SM, Rosa A, Field S, Coughlin M, Shizgal HM, Macklem PT (1984) Inspiratory muscle strength and body composition in patients receiving total parenteral nutrition therapy. Am Rev Respir Dis 130: 33–37
Kaye MP (1992) The registry of the International Society for Heart and Lung Transplantation: ninth official report-1992. J Heart Lung Transplant 11: 599–606
Chaparro C, Maurer JR, Chamberlain D, De Hoyos A, Winton T, Westney G, Kesten S (1994) Cause of death in lung transplant recipients. J Heart Lung Transplant 13: 758–766
Zenati M, Dowling RD, Dummer JS, Paradis IL, Arena VC, Armitage JM, Kormos RL, Hardesty RL, Griffith BP (1990) Influence of the donor lung on development of early infections in lung transplant recipients. J Heart Transplant 9: 502–509
Otaki M (1994) Surgical treatment of patients with cardiac cachexia. An analysis of factors affecting operative mortality. Chest 105: 1347–1351
Van den Berghe G, Zegher F, Vanhaecke J, Verleden G, Lauwers P (1994) Growth hormone as a rescue treatment after heart-lung or double-lung transplantation. Endocrinol Metab 1: 187–190
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Plöchl, W., Pezawas, L., Hiesmayr, M. et al. Nutritional status, ICU duration and ICU mortality in lung transplant recipients. Intensive Care Med 22, 1179–1185 (1996). https://doi.org/10.1007/BF01709333
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01709333