Abstract
Objective
Investigate the effects of mask physiotherapy on post-operative complications after thoracic surgery.
Design
A prospective, consecutive, randomized, controlled study.
Setting
Department of Thoracic and Heart Surgery at a University Hospital. The treatments were performed by experienced and specially trained physiotherapists.
Patients
97 low-risk male patients undergoing coronary artery by-pass graft surgery were evaluated. 66 patients completed the study.
Interventions
The patients were treated with routine chest physiotherapy alone or supplied with either positive expiratory pressure (PEP), or inspiratory resistance-positive expiratory pressure (IR-PEP).
Measurements and results
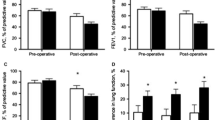
Post-operative pulmonary complications were assessed by forced vital capacity (FVC), arterial oxygen tension (PaO2), and chest X-ray examination, all measured pre-operatively and on the third and sixth post-operative day. There was an almost equal decrease and subsequent rise in spirometric and blood gas values, but patients treated with the PEP mask had a borderly significantly higher increase in PaO2 from day 3 to day 6 compared with patients treated with no mask. There was an almost equal frequency of atelectasis in the 3 treatments. The patients filled in a questionaire expressing their opinion about their treatment. Most patients liked their treatment and found it helpful but a little less so in the IR-PEP group.
Conclusion
We did not find any significant difference between the three groups; however, a tendency to decreased risk of having post-operative complications was observed in the groups having positive expiratory pressure (PEP) and inspiratory resistance-positive expiratory pressure (IR-PEP).
Similar content being viewed by others
References
Craig DB (1981) Postoperative recovery of pulmonary function. Anesth Analg 60:46–52
Wilcox P, Baile EM, Hards J, Muller NL, Dunn L, Pardy RL, Paré PD (1988) Phrenic nerve function and its relationship to atelectasis after coronary artery bypass surgery. Chest 93:693–698
Matthay MA, Wiener-Kronish JP (1989) Respiratory management after cardiac surgery. Chest 95:424–434
Berrizbeitia LD, Tessler S, Jacobowitz IJ, Kaplan P, Budzilowicz L, Cunningham JN (1989) Effect of sternotomy and coronary bypass surgery on postoperative pulmonary mechanics. Chest 96:873–876
Dammann JF, McAslan TC (1977) Optimal flow pattern for mechanical ventilation of the lungs. Crit Care Med 5:128–136
Jenkins SC, Soutar SA, Loukota JM, Johnson LC, Moxham J (1989) Physiotherapy after coronary artery surgery: are breathing exercises necessary? Thorax 44:634–639
Duncan AW, Oh TE, Hillman DR (1986) PEEP and CPAP. Anaesth Intensive Care 14:236–250
Andersen JB, Olesen KP, Eikard B, Jansen E, Quist J (1980) Periodic continuous positive airway pressure, CPAP, by mask in the treatment of atelectasis. Eur J Respir Dis 61:20–25
Ricksten S-E, Bengtsson A, Søderberg C, Thordén M, Kvist H (1986) Effects of periodic positive airway pressure by mask on postoperative pulmonary function. Chest 89:774–781
Ingwersen UM, Richter Larsen K, Thodberg Bertelsen M, Kiil Nielsen K, Laub M, Sandermann J, Bach K, Hansen H (1993) Three different mask physiotherapy regimens for prevention of post-operative pulmonary complications after heart and pulmonary surgery. Intensive Care Med 19:294–298
Tiep BL, Burns M, Kao D, Madison R, Herrera J (1986) Pursed lips breathing training using car oximetry. Chest 90:218–221
Ingwersen UM, Andersen JB (1992) Lungefysioterapi (Danish). Munksgaard, Copenhagen, pp 65–68 and pp 187–190
Braun SR, Birnbaum ML, Chopra PS (1978) Pre- and postoperative pulmonary function abnormalities in coronary artery revascularization surgery. Chest 73:316–320
Locke TJ, Griffiths TL, Mould H, Gibson GJ (1990) Ribcage mechanics after median sternotomy. Thorax 45:465–468
Jenkins SJ, Soutar SA, Forsyth A, Keates JRW, Moxham J (1989) Lung function after coronary artery surgery using the internal mammary artery and the saphenous vein. Thorax 44:209–211
Bahn CH, Holloway GA (1990) Effect of internal mammary artery mobilization on sternal blood flow. Chest 98:878–880
De Troyer A, Rosso J (1982) Reflex inhibition of the diaphragm by esophageal afferents. Neurosci Letters 30:43–46
Mortensen J, Falk M, Groth S, Jensen C (1991) The effects of postural drainage and positive espiratory pressure physiotherapy on tracheobronchial clearance in cystic fibrosis. Chest 100:1350–1357
Degn H, Haxholdt OS, Jørgensen BC, Krintel JJ, Risbo A (1986) Postoperative changes in pulmonary function. Pathological physiology, prophylaxis and treatment (Danish with English summary). Ugeskr Læger 148:2338–2341
Stranberg Å, Tokics L, Brismar B, Lundquist H, Hedenstierna G (1986) Atelectasis during anaesthesia and in the postoperative period. Acta Anaesthesiol Scand 30:154–158
Ford GT, Whitelaw WA, Rosenal TW, Cruse PJ, Guenter CA (1983) Diaphragm function after upper abdominal surgery in humans. Am Rev Respir Dis 127:431–436
Ford GT, Guenter CA (1984) Toward prevention of postoperative pulmonary complications. Am Rev Respir Dis 130:4–5
Christensen EF, Schultz P, Jensen OV, Egebo K, Engberg M, Grøn I, Juhl B (1991) Postoperative pulmonary complications and lung function in highrisk patients: a comparison of three physiotherapy regimens after upper abdominal suggery in general anesthesia. Acta Anaesthesiol Scand 35:97–104
Katz JA, Ozanne GM, Zinn SE, Fairley HB (1981) Time course and mechanisms of lung-volume increase with PEEP in acute pulmonary failure. Anesthesiology 54:9–16
Roussos C (1985) Function and fatigue of respiratory muscles. Chest 88:124s-132s
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Richter Larsen, K., Ingwersen, U., Thode, S. et al. Mask physiotherapy in patients after heart surgery: A controlled study. Intensive Care Med 21, 469–474 (1995). https://doi.org/10.1007/BF01706199
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01706199