Summary
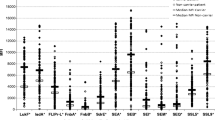
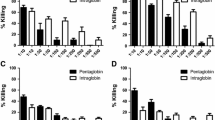
Chronic colonization withStaphylococcus aureus is found in 40–50% of the sputum producing patients with cystic fibrosis treated at Stockholm's Cystic Fibrosis Center, Huddinge University Hospital. 30–40% of these patients had increased ELISA IgG antibody titres against teichoic acid and against alpha-toxin. About half of the number of patients showed increased antibody titres to either antigen during infection. Increased antibody titres against staphylococcal antigenes were only found in ≤10% of patients not chronically colonized with S. aureus (no different from the normal population). The serum titres of antistaphylococcal antibodies were significantly higher in the chronically colonized patients (p<0.001). Patients who were also chronically harbouringPseudomonas aeruginosa had the highest titres of both antibodies. The titres increased with clinical signs of infection and were normalized by antimicrobial chemotherapy. To conclude, the use of ELISA IgG antibodies may prove suitable for routine evaluation of the need for, and control of the efficacy of antistaphylococcal chemotherapy in cystic fibrosis.
Zusammenfassung
Bei 40 bis 50% der Sputum produzierenden Patienten mit zystischer Fibrose, die am Stockholmer Zystische Fibrose Zentrum der Universitätsklinik Huddinge behandelt werden, findet sich eine chronische Kolonisation mitStaphylococcus aureus. 30 bis 40% dieser Patienten zeigten einen Anstieg der mit ELISA bestimmten IgG-Antikörper gegen Teichonsäure und alpha-Toxin. Im Laufe der Infektion traten bei etwa der Hälfte der Patienten Antikörpertiteranstiege gegen eines der Antigene auf. Bei nicht chronisch mitS. aureus kolonisierten Patienten fanden sich in ≤10% der Fälle erhöhte Antikörpertiter gegen Staphylokokkenantigene (kein Unterschied zur Normalbevölkerung). Bei chronisch kolonisierten Patienten waren die Titer an Serumantikörpern gegen Staphylokokkenantigene außerdem signifikant höher (p<0,001). Patienten, die zusätzlich chronisch mitPseudomonas aeruginosa besiedelt waren, wiesen die höchsten Antikörpertiter gegen die beiden Antigene auf. Wenn klinische Infektionszeichen auftraten, stiegen die Titer an, sie normalisierten sich mit der Antibiotikatherapie. Die Bestimmung der IgG-Antikörper mittels ELISA eignet sich möglicherweise für die Routinebestimmung der Notwendigkeit einer anti-Staphylokokken-Therapie bei zystischer Fibrose und für die Bewertung ihrer Wirksamkeit.
Similar content being viewed by others
References
Batten, J. C., Matthew, D. J. The respiratory system. In:Hodson, M., Norman, A. P., Batten, J. C. (eds.): Cystic Fibrosis, Bailliere Tindall, London (1983), pp. 105–131.
Kulcycki, L. L., Murphy, T. M., Bellanti, J. A. Pseudomonas colonization in cystic fibrosis. A study of 160 patients. JAMA 240 (1978) 30–34.
Marks, M. I. The pathogenesis and treatment of pulmonary infections in patients with cystic fibrosis. J. Pediatr. 98 (1981) 173–179.
Szaff, M., Høiby, N. Antibiotic treatment ofStaphylococcus aureus infection in cystic fibrosis. Acta Paediatr., Scand. 71 (1982) 821–826.
Høiby, N. Microbiology of lung infections in cystic fibrosis patients. Acta Paediatr., Scand. (Suppl. 301) (1982) 33–54.
Lawson, D. Simple parameters in the assessment of progress. In: Proceedings of the Seventh International Cystic Fibrosis Congress. Imp. Jouve, Paris 1976, pp. 510–517.
Ericsson Hollsing, A. Serological markers of pulmonary infection in patient with cystic fibrosis. Thesis. Karolinska Institutet, Stockholm 1987, pp. 34–35.
Knothe, H., Dette, G. A. Thein-vitro activity of ceftazidime against clinically important pathogens. J. Antimicrob. Chemother. 8 (Suppl. B) (1981) 33–41.
Hoogkamp-Korstanje, J. A. A. Comparativein vitro activity of five quinolone derivates and five other antimicrobial agents used in oral therapy. Eur. J. Clin. Microbiol. 3 (1984) 333–338.
Ericsson, A., Granström, M., Möllby, R., Strandvik, B. Antibodies of staphylococcal teichoic acid and alpha-toxin in cystic fibrosis. Acta Paediatr., Scand. 75 (1986) 139–144.
Ericsson Hollsing, A., Granström, M., Strandvik, B. Prospective study of serum staphylococcal antibodies in cystic fibrosis. Arch. Dis. Child. 62 (1987) 905–911.
Strandvik, B. Antibiotic therapy of pulmonary infections in cystic fibrosis. Dosage schedules and duration of treatment. Chest 94 (1988) 146S-149S.
Granström, M., Julander, I. G., Hedström, S. Å., Möllby, R. Enzyme-linked immunosorbent assay for antibodies against teichoic acid in patients with staphylococcal infections. J. Clin. Microbiol. 17 (1983) 640–646.
Julander, I. G., Granström, M., Hedström, S. Å, Möllby, R. The role of antibodies against α-toxin and teichoic acid in the diagnosis of staphylococcal infections. Infection 11 (1983) 77–83.
Verbrugh, H. A., Peters, R., Goessens, W. H. F., Michel, M. F. Distinguishing complicated from uncomplicated bacteremia caused byStaphylococcus aureus: The value of “new” and “old” serological tests. J. Infect. Dis. 153 (1986) 109–115.
Granström, M., Julander, I. G., Möllby, R. Serological diagnosis of deepStaphylococcus aureus infections by enzyme-linked immunosorbent assay (ELISA) for staphylococcal hemolysins and teichoic acid. Scand. J. Infect. Dis. (Suppl. 41) (1983) 132–139.
Granström, M., Ericsson, A., Strandvik, B., Wretlind, B., Pavlovskis, O. R., Berka, R., Vasil, M. L. Relation between antibody response toPseudomonas aeruginosa exoproteins and colonization/infection in patients with cystic fibrosis. Acta Paediatr., Scand. 73 (1984) 772–777.
Ericsson Hollsing, A., Granström, M., Vasil, M. L., Wretlind, B., Strandvik, B. Prospective study of serum antibodies toPseudomonas aeruginosa exoproteins in cystic fibrosis. J. Clin. Microbiol. 25 (1987) 1868–1874.
Ericsson Hollsing, A., Lantz, B., Bergström, K., Malmborg, A.-S., Stranvik, B. Granulocyte elastase α1-antiproteinase complex in cystic fibrosis: sensitive plasma assay for monitoring pulmonary infections. J. Pediatr. 111 (1987) 206–211.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Strandvik, B., Hollsing, A., Möllby, R. et al. Antistaphylococcal antibodies in cystic fibrosis. Infection 18, 170–172 (1990). https://doi.org/10.1007/BF01642107
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01642107