Abstract
Objective:
Before a patient can be connected to a mechanical ventilator, the controls of the apparatus need to be set up appropriately. Today, this is done by the intensive care professional. With the advent of closed loop controlled mechanical ventilation, methods will be needed to select appropriate startup settings automatically. The objective of our study was to test such a computerized method which could eventually be used as a start-up procedure (first 5–10 minutes of ventilation) for closed-loop controlled ventilation.
Design:
Prospective Study.
Settings:
ICU's in two adult and one children's hospital.
Patients:
25 critically ill adult patients (age≥15 y) and 17 critically ill children selected at random were studied.
Interventions:
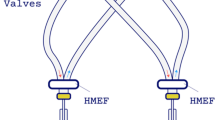
To simulate ‘initial connection’, the patients were disconnected from their ventilator and transiently connected to a modified Hamilton AMADEUS ventilator for maximally one minute. During that time they were ventilated with a fixed and standardized breath pattern (Test Breaths) based on pressure controlled synchronized intermittent mandatory ventilation (PCSIMV).
Measurements and main results:
Measurements of airway flow, airway pressure and instantaneous CO2 concentration using a mainstream CO2 analyzer were made at the mouth during application of the Test-Breaths. Test-Breaths were analyzed in terms of tidal volume, expiratory time constant and series dead space. Using this data an initial ventilation pattern consisting of respiratory frequency and tidal volume was calculated. This ventilation pattern was compared to the one measured prior to the onset of the study using a two-tailed paired t-test. Additionally, it was compared to a conventional method for setting up ventilators. The computer-proposed ventilation pattern did not differ significantly from the actual pattern (p>0.05), while the conventional method did. However the scatter was large and in 6 cases deviations in the minute ventilation of more than 50% were observed.
Conclusions:
The analysis of standardized Test Breaths allows automatic determination of an initial ventilation pattern for intubated ICU patients. While this pattern does not seem to be superior to the one chosen by the conventional method, it is derived fully automatically and without need for manual patient data entry such as weight or height. This makes the method potentially useful as a startup procedure for closed-loop controlled ventilation.
Article PDF
Similar content being viewed by others
References
Kacmarek RM, Venegas J. Mechanical Ventilatory Rates and Tidal Volumes. Respiratory Care 1987; 32: 466.
Frumin MJ. Clinical use of a physiological respirator producing N2O amnesia/analgesia. Anesthesiology 1957; 18: 290–9.
Frumin MJ, Bergman NA, Holaday DA. Carbon dioxide and oxygen blood levels with a carbon dioxide controlled artificial respirator. Anesthesiology 1959; 20: 313–20.
Mitamura Y, Mikami T, Sugawara H, Yoshimoto C. An optimally controlled respirator. IEEE Trans Biomed Engineering 1971; BMEI 18(5): 300–7.
Mitamura Y, Mikami T, Yamamoto K. A dual control system for assisting respiration. Med. Biol. Engineering 1975; 846–53.
Coles JR, Brown WA, Lampard DG. Computer control of respiration and anesthesia. Med Biol Engineering 1973; 262–7.
Ohlson KB, Westenskow DR, Jordan WS. A microprocessor based feedback controller for mechanical ventilation. Ann Biomed Engineering 1982; 10: 35–48.
Chapman FW, Newell JC, Roy RJ. A feedback controller for ventilatory therapy. Ann Biomed Engineering 1985; 13: 359–72.
East TD, Adriano KP, Pace NL. Computer-controlled optimization of positive end-expiratory pressure. Crit Care Med 1986; 14(9): 792–7.
Ritchie RG, Ernst EA, Pate BL, Pearson JD, Sheppard LC. Closed-loop control of an anesthesia delivery system: development and animal testing. IEEE Trans Biomed Engineering 1987; BME-34(6): 437–43.
East TD, Westenskow DR, Pace NL, Nelson LD. A microcomputer-based differential lung ventilation system. IEEE Trans Biomed Engineering 1982; 11: 736–40.
Coon RL, Zuperku EJ, Kampine JP. Systemic Arterial blood pH servocontrol of mechanical ventilation. Anesthesiology 1978; 201–4.
Brunner JX. Pulmonary function indices in critical care patients. First ed. Berlin: Springer, 1988.
Brunner JX, Wolff G. Reliable estimation of series dead space in ventilated patients. Clin Physiol 1985; 5 (Suppl 3): 65–8.
Otis AB, Fenn WO, Rahn H. Mechanics of breathing in man. J Appl Physiol 1950; 2: 592–607.
Mead J. Control of respiratory frequency. J Appl Physiol 1960; 15(3): 325–36.
Bland JM, Altman DG. Statistical Methods for assessing agreement between two methods of clinical measurement. Lancet 1986; 1: 307–10.
Marini JJ, Crooke PS, Truwit JD. Determinants and limits of pressure-preset ventilation: a mathematical model of pressure control. J Appl Physiol 1989; 67(3): 1081–92.
Radford EP, Jr. Ventilation standards for use in artifical respiration. N Engl J Med 1954; 251: 877–83.
Niemer, Nemes. Datenbuch Intensivmedizin. Gustav Fischer Verlag: Stuttgart, New York 1979; p. 5.
Giovannini I, Boldrini G, Castagneto M, Sganga G, Nanni G, Pittiruti M et al. Respiratory quotient and patterns of substrate utilization in human sepsis and trauma. JPEN 1983; 7: 226–30.
Hickling KG, Henderson SJ, Jackson R. Low mortality associated with low pressure limited ventilation with permissive hypercapnia in severe adult respiratory distress syndrome. Intensive Care Med 1990; 16: 372–7.
Iotti G, Braschi A, Brunner JX, Smits T, SalaGallini G, Rodi G et al. Evaluation non invasive et continue de la constante de temps expiratoire en ventilation artificielle (VA). Abstract, Réan Soins Intens Méd Urg 1992, 1(1): 129.
Hart MC, Orzalesi MM, Cook CD. Relation between anatomic respiratory dead space and body size and lung volume. J Appl Physiol 1963; 18(3): 519–22.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Laubscher, T.P., Frutiger, A., Fanconi, S. et al. Automatic selection of tidal volume, respiratory frequency and minute ventilation in intubated ICU patients as startup procedure for closed-loop controlled ventilation. J Clin Monit Comput 11, 19–30 (1994). https://doi.org/10.1007/BF01132840
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01132840