Summary
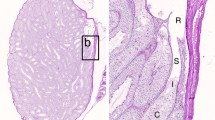
We provide evidence that testicular concretions form exclusively in association with seminiferous cords. Testicular material obtained from 6 patients with various disorders of spermatogenesis was studied by means of light-and electron microscopy. Seminiferous cords in the testes examined form so-called hypoplastic zones. They contain immature Sertoli cells and are surrounded by an unusually thick basal lamina and one or two layers of myofibroblasts. They display extensive coiling and form ring-like structures. Concretions are located at the periphery or in the center of the cords and consist of a hyaline material with an occasional granular core. They are enveloped by Sertoli cells or myofibroblasts. Data presented indicate that concretions may develop within the above-mentioned ring-like structures or in deep indentations of the surrounding connective tissue. Computer-assisted 3-D reconstructions of a seminiferous cord based on 24 serial semithin sections revealec that the majority of concretions communicate with the interstitial tissue through a broad opening comparable to a “meso”. On the basis of our observations we could demonstrate that concretions are accumulations of basal lamina that occasionally contain remnants of degenerated myofibroblasts. They form outside the cords and belong to the connective tissue compartment. As the components of the basal lamina are thought to be produced by the interaction of Sertoli cells and myofibroblasts we tentatively assume that the development of concretions reflects a disturbance in this complex interaction. We suggest that the presence of concretions refers to a developmental disorder and may be pathognomonic for the occurrence of defective seminiferous cords.
Similar content being viewed by others
References
Azzopardi JG, Mostofi FK, Theiss EA (1961) Lesions of testes observed in certain patients with widespread choriocarcinoma and related tumours. Am J Pathol 38:207–225
Barsky SH, Hannah JB (1987) Extracellular hyaline bodies are basement membrane accumulations. J Clin Pathol 87:455–460
Bieger RC, Passarge E, McAdams AJ (1965) Testicular intratubular bodies. J Clin Endocrinol 25:1340–1346
Blumensaat C (1929) Über einen neuen Befund in Knabenhoden. Virchows Arch [A] 273:51–61
Bunge RG, Bradbury JT (1961) Intratubular bodies in the human testis. J Urol 85:306–310
Halley JBW (1963a) Germ cell loss in prepuberal cryptorchid testes. J Urol 90:211–214
Halley JBW (1963b) The growth of Sertoli cell tumors: a possible index of differential gonadotrophic activity in the male. J Urol 90:220–229
Hedinger Chr, Plattner D (1961) Dysgenetische, sogenannte hypoplastische Zonen in retinierten und beidseits normal deszendierten Hoden. Pathol Microbiol 24:227–233
Hedinger Chr, Huber R, Weber E (1967) Frequency of so-called hypoplastic or dysgenetic zones in scrotal and otherwise normal human testes. Virchows Arch [A] 342:165–168
Holstein AF, Roosen-Runge EC, Schirren C (1988) Illustrated pathology of human spermatogenesis. Grosse Verlag, Berlin
Hornstein B von, Hedinger Chr (1965) Spharische intratubuläre Körperchen im präpuberalen Hoden und Nebenhoden. Virchows Arch [A] 339:83–99
Huber R, Weber E, Hedinger Chr (1968a) Struktur intratubulärer Körperchen (sog. Ringtubuli) des kindlichen Hodens. Virchows Arch [A] 344:40–46
Huber R, Weber E, Hedinger Chr (1968b) Zur mikroskopischen Anatomie der sog. hypoplastischen Zonen des normal descendierten Hodens. Virchows Arch [A] 344:47–53
Kleinteich B, Leman A, Schickedanz H (1975) Beitrag zu den intratubulären Körperchen des Hodens bei Kindern. Z Mikrosk Anat Forsch 89:975–982
Kreibig W (1929) Über Konkremente in unterentwickelten Hoden. Wien Klin Wochenschr 14:436–437
Kretser DM de (1968) The fine structure of the immature human testis in hypogonadotropic hypogonadism. Virchows Arch [B] 1:283–296
Laczko J, Levai G (1975) A simple differential staining method for semi-thin sections of ossifying cartilage and bone tissue embedded in epoxy resin. Mikroskopie 31:1–4
Lecène P, Chevassu M (1907) L'adénome vrai dans le testicule ectopique. Rev Chir (Paris) 35:234–244
Oiye T (1928) Über anscheinend noch nicht beschriebene Steinchen in den menschlichen Hoden. Beitr Pathol Anat 80:479–495
Plattner D (1962) Hypoplastische und keimepithelfreie Zonen in beidseits deszendierten Hoden als Zeichen einer partiellen Dysgenesie. Virchows Arch [A] 335:598–616
Reynolds ES (1963) The use of lead citrate at high pH as an electron-opaque stain in electron microscopy. J Cell Biol 17:208–212
Schantz A, Milsten R (1976) Testicular microlithiasis with sterility. Fertil Steril 27:801–805
Scheibli P (1968) Häufigkeit von sogenannten Ringtubuli mit intratubulären Körperchen in normal descendierten und fehlgelagerten Knabenhoden. Virchows Arch [A] 344:249–256
Schulze C (1984) Sertoli cells and Leydig cells in man. Adv Anat Embryol Cell Biol 88:1–104
Skinner MK, Tung PS, Fritz IB (1985) Cooperativity between Sertoli cells and testicular peritubular cells in the production and deposition of extracellular components. J Cell Biol 100:1941–1947
Smith BD, Leeson CR, Bunge RG, Anderson WR (1967) Microscopic appearance of the gonads in postpuberal testicular feminization. Invest Urol 5:73–86
Sohval AR (1954) Testicular dysgenesis as an etiologic factor in cryptorchidism. J Urol 72:693–701
Sohval AR (1956) Testicular dygenesis in relation to neoplasm of the testicle. J Urol 75:285–291
Strasmann T, Halata Z (1989) Applications for 3-D image processing in functional anatomy-reconstruction of the cubital joint region and spatial distribution of mechanoreceptors surrounding this joint in Monodelphis domestica, a laboratory marsupial. Eur J Cell Biol 48 [Suppl], 25:107–110
Török L, Mauss J, Borsch G (1974) Beitrag zu den sogenannten hypoplastischen Zonen und den Ringtubuli der menschlichen Hoden. Andrologia 6:203–209
Vegni-Talluri M, Bigliardi E, Vanni MG, Tota G (1980) Testicular microliths: their origin and structure. J Urol 124:105–107
Weinberg AG, Currarino G, Stone IC (1973) Testicular microlithiasis. Arch Pathol 95:312–314
Author information
Authors and Affiliations
Additional information
Supported by Deutsche Forschungsgemeinschaft (Ho 388/6-1) and Verein zur Förderung der Forschung auf dem Gebiet der Fortpflanzung e.V; Hamburg
Rights and permissions
About this article
Cite this article
Schulze, C., Schütte, B. Concretions in the human testis are derived from the basal lamina of seminiferous cords. Cell Tissue Res 260, 1–12 (1990). https://doi.org/10.1007/BF00297484
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00297484