Conclusions
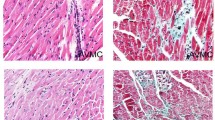
Infection of adolescent CD-1 mice with CVB3 activates NK cells. These activated NK cells can lyse infected fibroblasts in vitro and their transfer into mice prior to inoculation with CVB3 can reduce virus titers in heart tissues. If mice are depleted of NK cells prior to and throughout a CVB3 infection, myocarditic lesions show a comparatively greater pathology in the form of severe dystrophic calcification than in infected mice with an intact NK cell system. Also NK cell-depleted mice have significantly higher virus titers in heart tissues. These data suggest a role for NK cells in the infected mouse, i. e., that they reduce virus titers through lysis of infected cells and thereby reduce the severity of myocarditis. In keeping with such a defensive role is the finding of NK cells among the first inflammatory cells forming the nascent CVB3-induced focal myocarditic lesion. Paradoxically, NK cells remain in the mature lesion up to 10 days p.i. and may thus contribute to pathology. Further studies on whether these long-term residents release cytotoxic factors which continue to damage myocytes in absence of significant virus titers in heart tissues must be performed. These studies are now feasible because of the recent development of monoclonal antibodies against NK cytotoxic factor [30]. Finally, diet can adversely effect generation of activated NK cells in CVB3-inoculated mice and this finding may have significance for health-conscious human beings.
Similar content being viewed by others
References
Baron S, Dianzani F, Stanton J (1982) The interferon system: a review to 1982. Tex Rep Biol Med 41: 1
Bonavida B, Wright SC (1986) Role of natural killer cytotoxic factors in the mechanism of target-cell killing by natural killer cells. J Clin Immunol 6: 1
Biron CA, Welsh RM (1982) Activation and role of natural killer cells in virus infections. Med Microbiol 170: 155
Biron CA, Welsh RM (1982) Blastogenesis of natural killer cells during viral infection in vivo. J Immunol 129: 2788
Casali, P, Trinchieri G (1984) Natural killer cells in viral infections. In: Notkins AL, Oldstone MAB (eds) Concepts in viral pathogenesis. Springer, New York Berlin Heidelberg, pp 11–19
Dianzani F, Capbianchi MR, Matteucci D, Bendinelli M (1988) The role of interferon in picornavirus infections. In: Bendinelli M, Friedman H (eds) Coxsackieviruses A general update. Plenum Press, New York, p 65–80
Dyerberg J (1986) Linolenate-derivated polyunsaturated fatty acids and prevention of athrosclerosis. Nutr Rev 44: 125
Fernandes G, Gauntt CJ, Sandburg L, Freidrich W, Meydani SN (1987) Effect of high fish intake on vitamin E levels, NK activity and susceptibility to viral-induced myocarditis in lupus-prone mice. Arthritis Rheum 30: S 123
Gauntt CJ (1987) Cellular and humoral immune responses in coxsackieviruses myocarditis. In: Kawai C, Abelmann WH, Matsumori A (eds) Cardiomyopathy update 1. Pathogenesis of myocarditis and cardiomyopathy. Recent experimental and clinical studies. University of Tokyo Press, Tokyo, p 49–61
Gauntt CJ, Paque RE, Trousdale MD, Gudvangen RJ, Barr DT, Lipotich GJ, Nealon TJ, Duffey PS (1983) Temperature-sensitive mutant of coxsackievirus B3 (CVB3) establishes resistance in neonatal mice which protects them during adolescence against CVB3-induced myocarditis. Infect Immun 39: 851
Gauntt CJ, Arizpe HM, Kung JT, Ogilvie KK, Cheriyan UO (1985) Antimyocarditic activity of the guanine derivative BIOLF-70 in a coxsackievirus B3 murine model. Antimicrob Agents Chemother 27: 184
Gauntt CJ, Godeny EK, Lutton CW (1988) Host factors regulating viral clearance. Pathol Immunopathol Res 7: 251
Godeny EK, Gauntt CJ (1986) Involvement of natural killer cells in coxsackievirus B3-induced murine myocarditis. J Immunol 137: 1695
Godeny EK, Gauntt CJ (1987) Murine natural killer cells limit coxsackievirus B3 replication. J Immunol 139: 913
Godeny EK, Gauntt CJ (1987) In situ immune autoradiographic identification of cells in heart tissues of mice with coxsackievirus B3-induced myocarditis. Am J Pathol 129: 267
Godeny EK, Gauntt CJ (1987) Interferon and natural killer cell activity in coxsackie virus B3-induced murine myocarditis. Eur Heart J [Suppl J] 8: 433
Godeny EK, Cassling RS, Gauntt CJ (1987) Studies on the mechanism(s) of resistance to coxsackie virus B3 (CVB3)-induced myocarditis at adolescence in mice vaccinated at birth with a temperature-sensitive mutant of CVB3. Eur Heart J [Suppl J] 8: 403
Godeny EK, Arizpe HM, Gauntt CJ (1988) Characterization of the antibody response in vaccinated mice protected against coxsackievirus B3-induced myocarditis. Viral Immunol 1: 305
Goodnight SH, Harris WS, Connor WE, Illingworth JR (1982) Polyunsaturated fatty acids hyperlipidemia and thrombosis. Arteriosclerosis 2: 87
Huber SA, Job LP (1981) Cellular immune mechanisms in coxsackievirus group B, type 3 induced myocarditis in BALB/c mice. In: Spitzer JJ (ed) Myocardial injury. Plenum Press, New York, pp 491–508
Huber SA, Job LP, Woodruff JF (1981) Sex-related differences in the pattern of coxsackievirus B3-induced immune spleen cell cytotoxicity against virus-infected myofibers. Infect Immun 32: 68
Kurane I, Binn LN, Bancroft WH, Ennis FA (1985) Human lymphocyte responses to hepatitis A virus-infected cells: interferon production and lysis of infected cells. J Immunol 135: 2140
Levy RC, Rifkind B, Dennis B, Ernest N (1979) Nutrition, lipids and coronary heart disease. Raven Press, New York, pp 247–364
Lutton CW, Gauntt CJ (1985) Ameliorating effect of IFN-β and anti-IFN-β on coxsackievirus B3-induced myocarditis in mice. J Interferon Res 5: 137
Lutton CW, Gauntt CJ (1986) Coxsackievirus B3 infection alters plasma membrane of neonatal skin fibroblasts. J Virol 60: 294
Lutton CW, Gudvangen RJ, Nealon TJ, Paque RE, Gauntt CJ (1985) Cellular immune responses in mice challenged with an amyocarditic variant of coxsackievirus B3. J Med Virol 17: 345
McManus BM, Cassling RS, Gauntt CJ (1987) Immunologic basis of myocardial injury. Cardiovasc Clin 18: 163
Meydani SN, Yogeeswaran G (1987) No effect of fish oil on natural killer cell activity and prostaglandin E2 synthesis in young and old mice. In: Lands WEM (ed) Proceedings of the American Oil Chemistry Society on polyunsaturated fatty acids and eicosanoids. American Oil Chemistry Society, Champaign, IL, USA, pp 438–441
Ortaldo JR, Herberman RB (1984) Heterogeneity of natural killer cells. Annu Rev Immunol 2: 359
Ortaldo JR, Winkler-Pickett R, Morgan AC, Woodhouse C, Kantor R, Reynolds CW (1987) Analysis of rat natural killer cytotoxic factor (NKCF) produced by rat NK cell lines and the production of a murine monoclonal antibody that neutralizes NKCF. J Immunol 139: 3159
Preble OT, Friedman RM (1983) Biology of disease. Interferon-induced alterations in cells: relevance to viral and nonviral diseases. Lab Invest 49: 4
Rager-Zisman B, Bloom BR (1982) Natural killer cells in resistance to virus-infected cells. Springer Semin Immunopathol 4: 397
Roder JC, Pross HF (1982) The biology of the human natural killer cell. J Clin Immunol 2: 249
Sinclair HM (1980) Drugs affecting lipid metabolism. Elsevier/North Holland Biomedical Press, Amsterdam, p 363–378
Sonnenfeld G, Merigan TC (1979) The role of interferon in viral infections. Springer Semin Immunopathol 2: 311
Stamler J (1983) Nutrition related risk factors for the athrosclerotic diseases: present status. Prog Biochem Pharmacol 19: 245
Stewart WE (1979) The interferon system. Springer, New York Berlin Heidelberg, pp 233–255
Trinchieri G, Perussia B (1982) Interferons and natural killer cells: interacting systems of nonspecific host defense. In: Herberman RB NK cells and other natural effector cells. Academic Press, New York, p 369–374
Welsh RM (1984) Natural killer cells and interferon. CRC Crit Rev Immunol 5: 55
Welsh RM, Biron CA, Bukowski JF, McIntyre KW, Yang H (1984) Role of natural killer cells in virus infections of mice. Surv Synth Pathol Res 3: 409
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Gauntt, C.J., Godeny, E.K., Lutton, C.W. et al. Role of natural killer cells in experimental murine myocarditis. Springer Semin Immunopathol 11, 51–59 (1989). https://doi.org/10.1007/BF00197084
Issue Date:
DOI: https://doi.org/10.1007/BF00197084