Abstract
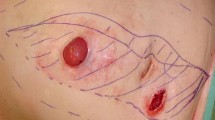
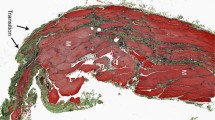
Animal studies and clinical experience in adults suggest that the Gore-Tex patch, because of its strength and lack of reactivity, is superior to other synthetic materials as a fascial replacement. We report our experience with Gore-Tex for the repair of neonatal abdominal wall defects when direct fascial closure was not possible. Between January 1985 and July 1992, 84 patients underwent repair of an omphalocele or gastroschisis. Ten of these were repaired with a Gore-Tex patch. Follow-up averaged 2.2 years (range 13–63 months). Data collected were graft life (time from insertion to removal), patch-related complications such as exteriorization (exposure of the patch due to dehiscence of the overlying skin), presence or absence of local and/or systemic infection, and patch separation (separation of the sutured edge of the patch from the fascia). The ease of removal as well as the appearance of the wound after patch removal was documented. Patch-related complications were divided into early (≤30 days postoperatively), and late (> 30 days). All ten patients required graft removal because of patch-related complications. The median time to removal was 90 days (range 20–540). There were a total of 12 complications in the ten patients. Three had early complications; three had exteriorized patches and two had concomitant local infections. Seven patients had late complications. Exteriorization was less common in this group, occurring in two cases. Local infections occurred in five of seven patients. Patch removal was necessary to clear the infection in all cases. No patient developed systemic sepsis or enteric fistulae. The patch was removed easily and there were no bowel-to-patch adhesions. Fascial closure was successfully accomplished in all patients regardless of the size of the initial defect. In no case did removal of the patch and secondary closure of the abdominal wall result in a ventral hernia. This study demonstrates that: (1) Gore-Tex patch closure of neonatal abdominal wall defects is associated in all cases with either early or late exteriorization and/or infection; (2) removal is easy and complication-free because it does not incorporate into the tissue and is relatively non-reactive; and (3) following removal of the patch it is possible to successfully close the abdominal wall defect. We conclude that Gore-Tex is a useful synthetic material for closure of neonatal abdominal wall defects, but should be considered a temporary bridge to subsequent fascial closure.
Similar content being viewed by others
References
Bauer JJ, Salky BA, Gelernt IM, Kreel I (1987) Repair of large abdominal wall defects with expanded polytetrafluoroethylene (PTFE). Ann Surg 206: 765–769
Brown GL, Richardson JD, Malangoni MA, Tobin GR, Ackerman D, Polk HC (1985) Comparison of prosthetic materials for abdominal wall reconstruction in the presence of contamination and infection. Ann Surg 201: 705–711
Burkel WE, Khan RH (1982) Biocompatibility of prosthetic grafts. In: Stanley JC (ed) Biologic and synthetic vascular prostheses. Grune and Stratton, New York, pp 221–247
Dayton MT, Buchele BA, Shirazi SS, Hunt LB (1986) Use of an absorbable mesh to repair contaminated abdominal-wall defects. Arch Surg 121: 954–960
Hamer-Hodges DW, Scott NB (1985) Replacement of an abdominal wall defect using expanded PTFE sheet (Gore-Tex). J R Coll Surg Edinb 30: 65–67
Kaufman Z, Engelberg M, Zager M (1981) Fecal fistula: a late complication of Marlex mesh repair. Dis Colon Rectum 24: 543–544
Lamb JP, Vitale T, Kaminski DL (1983) Comparative evaluation of synthetic meshes used for abdominal wall replacement. Surgery 93: 643–648
Larson GM, Harrower HW (1978) Plastic mesh repair of incisional hernias. Am J Surg 135: 559–563
Marmon LM, Vinocur CD, Standiford SB, Wagner CW, Dunn JM, Weintraub WM (1985) Evaluation of absorbable polyglycolic acid mesh as a wound support. J Pediatr Surg 20: 737–742
Massulo C, Pocchiari M, Macchi G et al. (1989) Transmission of Creutzfeld-Jakob disease by dural cadaveric graft. J Neurosurg 71: 954–955
Meddings RN, Carachi R, Gorhams S, Frend DA (1993) A new bioprosthesis in large abdominal wall defects. J Pediatr Surg 28: 660–663
Murphy JL, Freeman JB, Dionne PG (1989) Comparison of Marlex and Gore-Tex to repair abdominal wall defects in the rat. Can J Surg 32: 244–247
Rosenman JE, Pearce WH, Kempczinski RF (1985) Bacterial adherence to vascular grafts after in vitro bacteremia. J Surg Res 38: 648–655
Schmitt DD, Bandyk DF, Pequet AJ, Towne JB (1986) Bacterial adherence to vascular prostheses. A determinant of graft infectivity. J Vasc Surg 3: 732–740
Smith S, Gault N, Nowe MI, Lloyd DA (1989) Dura vs. Gore-Tex as an abdominal wall prosthesis in an open and closed infected model. J Pediatr Surg 24: 519–521
Stone HH, Fabian TC, Turkelson ML, Jurkiewicz MF (1981) Management of acute full-thickness losses of the abdominal wall. Ann Surg 193: 612–618
Stringel G (1993) Large gastroschisis: primary repair with Gore-Tex patch. J Pediatr Surg 28: 653–655
Tyrell J, Silberman H, Chandrasoma P, Niland J, Shull J (1989) Absorbable versus permanent mesh in abdominal operations. Surg Gynecol Obstet 168: 227–232
Voyles CR, Richardson JD, Bland KI, Tobin GR, Flint LM, Polk HC Jr (1981) Emergency abdominal wall reconstruction with polypropylene mesh. Short-term benefits versus long-term complications. Ann Surg 194: 219–223
Willison HJ, Gale AN, McLaughlin JE (1991) Creutzfeld-Jakob disease following cadaveric dura mater graft. J Neurol Neurosurg Psychiatry 54: 940
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Willis, P.M., Albanese, C.T., Rowe, M.I. et al. Long-term results following repair of neonatal abdominal wall defects with Gore-Tex. Pediatr Surg Int 10, 93–96 (1995). https://doi.org/10.1007/BF00171163
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00171163