Abstract
Background
Prevalence of peripheral arterial disease increases with age and is related to increased morbidity and mortality. The clinical diagnosis includes the measurement of ankle–brachial index (ABI).
Aims
To check the prevalence of abnormal ABI, and the value of physical examination of arterial system in detection of ABI < 0.9.
Methods
We performed subgroup analysis of patients included in the PolSenior survey. We measured ABI, performed physical examination of arterial system, assessed laboratory and questionnaire factors related to atherosclerosis. Participants were divided according to ABI strata of < 0.9, 0.9–1.4 and > 1.4. Clinical score of abnormalities on physical examination was proposed. Using logistic regression, we obtained areas under the curve (AUC).
Results
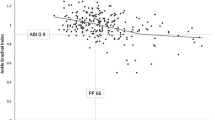
The mean age of 844 participants (53.3% men) was 74.7 (10.6) years. ABI < 0.9 was found in 20.3% participants and it was linked to history of myocardial infarction, hypertension and renal failure. In the entire group, 72.4% of subjects declared, that they were able to walk a distance of 200 m without interruption. Higher clinical score was associated with lower ABI. Full physical examination (AUC = 0.67) followed by examination of lower extremities (AUC = 0.65) showed strongest diagnostic value for PAD based on ABI. Neither ABI nor clinical examination was a good predictor of the inability to walk 200 meters without difficulties.
Discussion/conclusions
Full clinical examination, only moderately, adds to detection of PAD. The ability to walk 200 m is not a good measure of PAD in older subjects.

Similar content being viewed by others
References
Fowkes F, Rudan D, Rudan I, et al (2013) Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: a systematic review and analysis. Lancet 382:1329–1340
Ostchega Y, Paulose-Ram R, Dillon C et al (2007) Prevalence of peripheral arterial disease and risk factors in persons aged 60 and older: data from the National Health and Nutrition Examination Survey 1999–2004. J Am Geriatr Soc 55:583–589
Meijer W, Hoes A, Rutgers D et al (1998) Peripheral arterial disease in the elderly. The Rotterdam Study. Arterioscler Thromb Vasc Biol 18:185–192
Diehm C, Schuster A, Allenberg J et al (2004) High prevalence of peripheral arterial disease and co-morbidity in 6880 primary care patients: cross-sectional study. Atherosclerosis 172:95–105
DeBakey M, Lawrie G, Glaeser D (1985) Patterns of atherosclerosis and their surgical significance. Ann Surg 201:115–131
DeBakey M, Glaeser D (2000) Patterns of atherosclerosis: effect of risk factors on recurrence and survival-analysis of 11,890 cases with more than 25-year follow-up. Am J Cardiol 85:1045–1053
Cui R, Yamagishi K, Imano H, IHC investigators et al (2014) Relationship between the ankle-brachial index and the risk of coronary heart disease and stroke: the circulatory risk in communities study. J Atheroscler Thromb 21:1283–1289
Fowkes F, Murray G, Butcher I et al (2008) Ankle brachial index combined with Framingham Risk Score to predict cardiovascular events and mortality: a meta-analysis. JAMA 300:197–208
Meijer W, Grobbee D, Hunink M Hofman A, Hoes A (2000) Determinants of peripheral arterial disease in the elderly. The Rotterdam Study. Arch Intern Med 160:2934–2938
Alzamora M, Forés R, Baena-Díez J et al (2010) The peripheral arterial disease study (PERART/ARTPER): prevalence and risk factors in the general population. BMC Public Health. https://doi.org/10.1186/1471-2458-10-38
Velescu A, Clara A, Peñafiel J et al (2016) Peripheral arterial disease incidence and associated risk factors in a Mediterranean population-based cohort. The REGICOR Study. Eur J Vasc Endovasc Surg 51:696–705
Hiramoto J, Katz R, Weisman S, Conte M (2014) Gender-specific risk factors for peripheral artery disease in a voluntary screening population. J Am Heart Assoc. https://doi.org/10.1161/JAHA.113.000651
Sigvant B, Wiberg-Hedman K, Bergqvist D et al (2007) A population-based study of peripheral arterial disease prevalence with special focus on critical limb ischemia and sex differences. J Vasc Surg 45:1185–1191
Van Kuijk J, Flu W, Poldermans D (2011) Risk factors and peripheral arterial disease; a plea for objective measurements. Atherosclerosis 214:37–38
Ramos R, Quesada M, Solanas P et al (2009) Prevalence of symptomatic and asymptomatic peripheral arterial disease and the value of the ankle-brachial index to stratify cardiovascular risk. Eur J Vasc Endovasc Surg 38:305–311
Londero L, Lindholt J, Thomsen M et al (2016) Pulse palpation is an effective method for population-based screening to exclude peripheral arterial disease. J Vasc Surg 63:1305–1310
McDermott M (2015) Lower extremity manifestations of peripheral artery disease: the pathophysiologic and functional implications of leg ischemia. Circ Res 116:1540–1550
Khan N, Rahim S, Anand S et al (2006) Does the clinical examination predict lower extremity peripheral arterial disease? JAMA 295:536–546
Crawford F, Welch K, Andras A et al (2016) Ankle brachial index for the diagnosis of lower limb peripheral arterial disease. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD010680.pub2
Diehm C, Lange S, Darius H et al (2006) Association of low ankle brachial index with high mortality in primary care. Eur Heart J 27:1743–1749
Hirsch A, Criqui M, Treat-Jacobson D et al (2001) Peripheral arterial disease detection, awareness, and treatment in primary care. JAMA 286:1317–1324
Xu D, Zou L, Xing Y et al (2013) Diagnostic value of ankle-brachial index in peripheral arterial disease: a meta-analysis. Can J Cardiol 29:492–498
Kazmers A, Koski M, Groehn H et al (1996) Assessment of noninvasive lower extremity arterial testing versus pulse exam. Am Surg 62:315–319
Armstrong D, Tobin C, Matangi M (2010) The accuracy of the physical examination for the detection of lower extremity peripheral arterial disease. Can J Cardiol 26:e346–e350
Cournot M, Boccalon H, Cambou J et al (2007) Accuracy of the screening physical examination to identify subclinical atherosclerosis and peripheral arterial disease in asymptomatic subjects. J Vasc Surg 46:1215–1221
Collins T, Suarez-Almazor M, Peterson N (2006) An absent pulse is not sensitive for the early detection of peripheral arterial disease. Fam Med 38:38–42
Kaufmann C, Jacomella V, Kovacicova L et al (2013) Predictive value of auscultation of femoropopliteal arteries. Swiss Med Wkly. https://doi.org/10.4414/smw.2013.13761
Bledowski P, Mossakowska M, Chudek J et al (2011) Medical, psychological and socioeconomic aspects of aging in Poland: assumptions and objectives of the PolSenior project. Exp Gerontol 46:1003–1009
Tendera M, Aboyans V, Bartelink ML et al (2011) ESC Guidelines on the diagnosis and treatment of peripheral artery diseases: document covering atherosclerotic disease of extracranial carotid and vertebral, mesenteric, renal, upper and lower extremity arteries: the Task Force on the Diagnosis and Treatm. Eur Heart J 32:2851–2906
Aboyans V, Ricco J, Bartelink M et al (2018) 2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS): Document covering atherosclerotic disease of extracranial carotid and vertebral, mesenteric, renal, upper and lower extremity arteriesEndorsed by: the European Stroke Organization (ESO)The Task Force for the Diagnosis and Treatment of Peripheral Arterial Diseases of the European Society of Cardiology (ESC) and of the European Society for Vascular Surgery (ESVS). Eur Heart J 39:763–816
Criqui M, Fronek A, Klauber M et al (1985) The sensitivity, specificity, and predictive value of traditional clinical evaluation of peripheral arterial disease: results from noninvasive testing in a defined population. Circulation 71:516–522
Sigvant B, Wiberg-Hedman K, Bergqvist D et al (2009) Risk factor profiles and use of cardiovascular drug prevention in women and men with peripheral arterial disease. Eur J Cardiovasc Prev Rehabil 16:39–46
Funding
Project was supported by the national grant from the Polish Ministry of Science and Higher Education (Grant no. PBZ-MEiN-9/2/2006).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Statement of human and animal rights
The study was approved by the Bioethics Committee of the Medical University of Silesia in Katowice (Nb: KNW-6501-38/I//08).
Informed consent
Each participant gave written, informed consent to participate in the study.
Additional information
Joint senior authorship: Anna Skalska and Jerzy Gąsowski.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Królczyk, J., Piotrowicz, K., Chudek, J. et al. Clinical examination of peripheral arterial disease and ankle–brachial index in a nationwide cohort of older subjects: practical implications. Aging Clin Exp Res 31, 1443–1449 (2019). https://doi.org/10.1007/s40520-018-1095-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-018-1095-6