Abstract
Objective
To compare the global health status, frequency of somatic and psychological problems, and alcohol use in adulthood among women hospitalized in adolescence for severe anorexia nervosa (AN), with a matched control sample from the general population.
Method
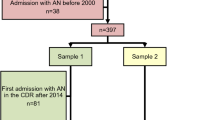
Women (n = 86) who had been hospitalized for AN 9.31 ± 1.82 years previously were compared with 258 controls matched for gender, age, and socio-professional category. Data were retrieved from a French survey on health and social insurance coverage, and was mainly collected by self-report, except for the assessment of current eating disorders for those previously hospitalized for AN (assessed with the MINI).
Results
The women who had been hospitalized for AN reported significantly poorer current health status compared to controls (OR 2.9, 95% CI 1.5–5.79). According to the MINI, 13 women previously hospitalized with severe AN still presented an eating disorder (ED). Women with past AN reported more frequent acute throat infections (OR 4.9, 95% CI 1.81–13.51), gastralgia (OR 3.6, 95% CI 1.9–6.83), gastro-oesophageal reflux (OR 5.279, 95%CI 2.11–13.22), excess blood cholesterol or triglyceride levels (OR 2.55, 95% CI 1.03–6.33), anxiety (OR 8.7, 95% CI 3.48–21.8) and depression (OR 5.02 (2.8–9.01). These differences remained significant and of the same order of magnitude in sensitivity analyses among subjects with previous AN but without current ED, except for perceived health status and excess cholesterol and triglyceride levels.
Discussion
Women who had been hospitalized for severe AN reported more symptoms 10 years after treatment, implies psychological and somatic follow-up in the long term.
Level of evidence
Level III, case–control analytic study.

Similar content being viewed by others
References
Steinhausen H-C (2009) Outcome of eating disorders. Child Adolesc Psychiatr Clin N Am 18:225–242. https://doi.org/10.1016/j.chc.2008.07.013
Mitchell JE, Crow S (2006) Medical complications of anorexia nervosa and bulimia nervosa. Curr Opin Psychiatry 19:438–443. https://doi.org/10.1097/01.yco.0000228768.79097.3e
NICE guidelines (2017) Eating disorders: recognition and treatment
American Psychiatric Association (2006) Treatment of patients with eating disorders, third edition. American Psychiatric Association. Am J Psychiatry 163:4–54
HAS (2011) Anorexia Nervosa: Management. Clinical Practice Guidelines. HAS, Saint-Denis
Vestergaard P, Emborg C, Støving RK et al (2002) Fractures in patients with anorexia nervosa, bulimia nervosa, and other eating disorders—a nationwide register study. Int J Eat Disord 32:301–308. https://doi.org/10.1002/eat.10101
Andersen AE, Ryan GL (2009) Eating disorders in the obstetric and gynecologic patient population. Obstet Gynecol 114:1353–1367. https://doi.org/10.1097/AOG.0b013e3181c070f9
Ante Z, Luu TM, Healy-Profitós J et al (2020) Pregnancy outcomes in women with anorexia nervosa. Int J Eat Disord. https://doi.org/10.1002/eat.23251
Forney KJ, Buchman-Schmitt JM, Keel PK, Frank GKW (2016) The medical complications associated with purging. Int J Eat Disord 49:249–259. https://doi.org/10.1002/eat.22504
Stheneur C, Bergeron S, Lapeyraque A-L (2014) Renal complications in anorexia nervosa. Eat Weight Disord 19:455–460. https://doi.org/10.1007/s40519-014-0138-z
Romanos GE, Javed F, Romanos EB, Williams RC (2012) Oro-facial manifestations in patients with eating disorders. Appetite 59:499–504. https://doi.org/10.1016/j.appet.2012.06.016
Katzman DK (2005) Medical complications in adolescents with anorexia nervosa: a review of the literature. Int J Eat Disord 37(Suppl):S52–59. https://doi.org/10.1002/eat.20118(discussion S87–89)
Smith C, Feldman SS, Nasserbakht A, Steiner H (1993) Psychological characteristics and DSM-III-R diagnoses at 6-year follow-up of adolescent anorexia nervosa. J Am Acad Child Adolesc Psychiatry 32:1237–1245. https://doi.org/10.1097/00004583-199311000-00018
Herpertz-Dahlmann B, Müller B, Herpertz S et al (2001) Prospective 10-year follow-up in adolescent anorexia nervosa-course, outcome, psychiatric comorbidity, and psychosocial adaptation. J Child Psychol Psychiatry 42:603–612
Godart NT, Flament MF, Perdereau F, Jeammet P (2002) Comorbidity between eating disorders and anxiety disorders: a review. Int J Eat Disord 32:253–270. https://doi.org/10.1002/eat.10096
Lange CRA, Ekedahl Fjertorp H, Holmer R et al (2019) Long-term follow-up study of low-weight avoidant restrictive food intake disorder compared with childhood-onset anorexia nervosa: psychiatric and occupational outcome in 56 patients. Int J Eat Disord 52:435–438. https://doi.org/10.1002/eat.23038
Andrés-Pepiñá S, Plana MT, Flamarique I et al (2020) Long-term outcome and psychiatric comorbidity of adolescent-onset anorexia nervosa. Clin Child Psychol Psychiatry 25:33–44. https://doi.org/10.1177/1359104519827629
Deter HC, Herzog W (1994) Anorexia nervosa in a long-term perspective: results of the Heidelberg–Mannheim Study. Psychosom Med 56:20–27
Wentz E, Gillberg IC, Gillberg C, Råstam M (2000) Ten-year follow-up of adolescent-onset anorexia nervosa: physical health and neurodevelopment. Dev Med Child Neurol 42:328–333. https://doi.org/10.1111/j.1469-8749.2000.tb00098.x
Dobrescu SR, Dinkler L, Gillberg C et al (2020) Anorexia nervosa: 30-year outcome. Br J Psychiatry 216:97–104. https://doi.org/10.1192/bjp.2019.113
Prince M, Patel V, Saxena S et al (2007) No health without mental health. Lancet 370:859–877. https://doi.org/10.1016/S0140-6736(07)61238-0
Erdur L, Kallenbach-Dermutz B, Lehmann V et al (2012) Somatic comorbidity in anorexia nervosa: first results of a 21-year follow-up study on female inpatients. Biopsychosoc Med 6:4. https://doi.org/10.1186/1751-0759-6-4
Stheneur C, Ali A, Tric L et al (2017) Impact of somatic severity on long-term mortality in anorexia nervosa. Eat Weight Disord 22:285–289. https://doi.org/10.1007/s40519-016-0346-9
Roux H, Blanchet C, Stheneur C et al (2013) Somatic outcome among patients hospitalised for anorexia nervosa in adolescence: disorders reported and links with global outcome. Eat Weight Disord 18:175–182. https://doi.org/10.1007/s40519-013-0030-2
Godart N, Atger F, Perdereau F et al (2004) Treatment of adolescent patients with eating disorders: description of a psychodynamic approach in clinical practice. Eat Weight Disord 9:224–227
Godart N, Wallier J, Hubert T et al (2009) Determining factors for target weights in an anorexia nervosa inpatient program for adolescents and young adults: study on the links between theory-based hypotheses and the realities of clinical practice. Eat Weight Disord 14:e176–183
Allonier C, Dourgnon P, Rochereau T (2008) Enquête sur la santé et la protection sociale. IRDES
American Psychiatric Association (1994) Diagnostic and statistical manual of mental disorders (DSM-IV), 4th edn. American Psychiatric Association, Arlington
Hubert T, Pioggiosi P, Huas C et al (2013) Drop-out from adolescent and young adult inpatient treatment for anorexia nervosa. Psychiatry Res 209:632–637. https://doi.org/10.1016/j.psychres.2013.03.034
Wentz E, Gillberg IC, Anckarsäter H et al (2009) Reproduction and offspring status 18 years after teenage-onset anorexia nervosa—a controlled community-based study. Int J Eat Disord 42:483–491. https://doi.org/10.1002/eat.20664
Rizk M, Kern L, Lalanne C et al (2019) High-intensity exercise is associated with a better nutritional status in anorexia nervosa. Eur Eat Disorders Rev 27:391–400. https://doi.org/10.1002/erv.2661
Billeci L, Brunori E, Scardigli S et al (2018) Excessive physical activity in young girls with restrictive-type anorexia nervosa: its role on cardiac structure and performance. Eat Weight Disord 23:653–663. https://doi.org/10.1007/s40519-017-0447-0
Fisher M, Golden NH, Katzman DK et al (1995) Eating disorders in adolescents: a background paper. J Adolesc Health 16:420–437. https://doi.org/10.1016/1054-139X(95)00069-5
Fairburn CG, Harrison PJ (2003) Eating disorders. Lancet 361:407–416. https://doi.org/10.1016/S0140-6736(03)12378-1
Shaheen NJ, Richter JE (2009) Barrett’s oesophagus. Lancet 373:850–861. https://doi.org/10.1016/S0140-6736(09)60487-6
Halmi KA, Eckert E, Marchi P et al (1991) Comorbidity of psychiatric diagnoses in anorexia nervosa. Arch Gen Psychiatry 48:712–718
Foulon C, Guelfi JD, Kipman A et al (2007) Switching to the bingeing/purging subtype of anorexia nervosa is frequently associated with suicidal attempts. Eur Psychiatry 22:513–519. https://doi.org/10.1016/j.eurpsy.2007.03.004
Arcelus J, Mitchell AJ, Wales J, Nielsen S (2011) Mortality rates in patients with anorexia nervosa and other eating disorders. A meta-analysis of 36 studies. Arch Gen Psychiatry 68:724–731. https://doi.org/10.1001/archgenpsychiatry.2011.74
Prabhakaran R, Misra M, Miller KK et al (2008) Determinants of height in adolescent girls with anorexia nervosa. Pediatrics 121:e1517–1523. https://doi.org/10.1542/peds.2007-2820
Wentz E, Mellström D, Gillberg C et al (2003) Bone density 11 years after anorexia nervosa onset in a controlled study of 39 cases. Int J Eat Disord 34:314–318. https://doi.org/10.1002/eat.10192
Linna MS, Raevuori A, Haukka J et al (2013) Reproductive health outcomes in eating disorders. Int J Eat Disord 46:826–833. https://doi.org/10.1002/eat.22179
Gueguen J, Godart N, Chambry J et al (2012) Severe anorexia nervosa in men: comparison with severe AN in women and analysis of mortality. Int J Eat Disord 45:537–545. https://doi.org/10.1002/eat.20987
Strobel C, Quadflieg N, Voderholzer U et al (2018) Short- and long-term outcome of males treated for anorexia nervosa: a review of the literature. Eat Weight Disord 23:541–552. https://doi.org/10.1007/s40519-018-0538-6
Voderholzer U, Hessler JB, Naab S et al (2019) Are there differences between men and women in outcome of intensive inpatient treatment for anorexia nervosa? An analysis of routine data. Eur Eat Disord Rev 27:59–66. https://doi.org/10.1002/erv.2624
Acknowledgements
Mrs Jo Ann Cahn.
Funding
Fondation Wyeth.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
“All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.” This research was authorized in 2007 by the Ile-de-France III Ethics Committee (No Am359-1-2353) and complied with the terms of the Helsinki declaration, and accepted by the CNIL no 253/29-05-06. Patients and parents (during the admission for AN) provided informed written consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chapelon, E., Barry, C., Hubert, T. et al. Health in adulthood after severe anorexia nervosa in adolescence: a study of exposed and unexposed women. Eat Weight Disord 26, 1389–1397 (2021). https://doi.org/10.1007/s40519-020-00940-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-020-00940-5